Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
D Starokadomsky1,2*, M Reshetnyk2,4 and Nd Starokadomska3
Received: October 04, 2023; Published: October 11, 2023
*Corresponding author: Dm. Starokadomsky, Chuiko Institute of Surface Chemistry, National Academy of Sciences of Ukraine, Ukraine
DOI: 10.26717/BJSTR.2023.53.008373
For the first time, at the level of a popular scientific experimental publication, a theoretical substantiation of the need to introduce preventive and self-restorative methods in dentistry was carried out, thanks to the use of compositions with nano-silica, nano-aluminum oxide and micro-sized mineral plant fillers. Methods for creating tooth powders and epoxy polymer fillings are proposed - from publicly available components, for use by non-specialists in places unsuitable for traditional prevention. All these assumptions and hypotheses were confirmed in the obtained results of observations in the wellbeing of patients by visual information (photo, x-ray image) of the treated groups of affected teeth. The experimental part was based on the results of preclinical studies and was carried out on volunteers, with the involvement of consultants from dental clinics. The findings confirm the possibility of effective prevention and self-healing of dental systems through non-operative exposure to special complexes of dental powders, pastes and rinsing systems (subject to the correct mode of dental use).
Keywords: Dental Diseases; Traditional Dentistry; Surface Preparation Problems; Self-Restoring Preventive Compositions; Self-Restoration Possibilities; Positive Effects; Highly Filled Epoxy Composites; Self-Sealing
Dental Problems Can we Help Ourselves?
Dental problems (in varying degrees of severity) have haunted people since the advent of civilizations from childhood and throughout their lives. It is rare to find a person indifferent to tooth and oral problems. Dental diseases are rarely fatal, but forced attention to them is increased in most patients. This can be explained by both psychological and physiological, as well as evolutionary reasons. Physiologically, dental diseases prevent you from properly chewing and digesting food, which leads to digestive diseases. The ancient human fear of toothache is also connected with this: even today since poor digestion shortens life, and in ancient times this meant quick death. Psychologically, bad teeth poison or eliminate the main means of relaxation and pleasure - the pleasant process of eating. But bad teeth also mean bad appearance. It is not for nothing that the health of horses, cows, and other animals is determined by their teeth - and the assessment of human health is partly done by the condition of the teeth. Over the past 100 years, a breakthrough has been made in their solution, comparable to space flights and the discovery of vaccinations. Modern dentistry has made it possible not only to pull out teeth, but also to restore them. But even this did not eliminate, but only alleviated, the anxiety and suffering caused by teeth to most people. The tooth hurt (chipped, fell out, became hypersensitive) just on the weekend or on a trip... It will be treated in the near future - no earlier than in a week... Family dentist was on vacation: There is a huge queue to see the social dentist on duty, and in private dentistry costs too much... Dentists did not want to treat a “hopeless case”, and write out referrals for removal to a surgeon... Queues, fear of “what now”, spending money... These troubles, familiar from childhood, haunt most people throughout their lives, right up to old age. Subsequently, we have to fork out money for false teeth, bridges, crowns... but they bring new problems - loss of gums, inflammation of the gums, bad bite... Is it really supposed to be like this always, and our teeth will be “a 5th column” - on which we should keep a constant guard familiar dentists and a separate wallet? Or try not to be taken into account and endure all the disorders, caries, gumboils and irritation of the teeth? In much the same way, even before the 1930s-50s, people were horrified by any cuts, bites or punctures of the skin. At every step they were then guarded by gangrene, tetanus, malaria, rabies, blood poisoning and other (long forgotten by us) diseases that passed through the blood. And until recently, in medical institutions one could see posters with recommendations to immediately go to the emergency room after initial treatment of the cut or bite site with iodine or formaldehyde. Or does anyone now, in the age of Panthenol, Iodophorm, BF-6, BrillantGreen and medical CN-acrylates, know where there is at least one emergency room for treating scratches or cuts? And now, in the 21st century, does anyone run to the ambulance after being bitten/scratched by a street cat or even a dog (not to mention mosquitoes and wasps)? This is a fait accompli - 90% of people have learned to heal skin damage that recently threatened with terrible consequences - with their own hands, with the latest and very effective cheap ointments and sprays. But dentistry and dental diseases... their method of treatment and attitude towards them are still somewhere there, in the 30s... except that the drills are not so painful and noisy, the chairs are more beautiful, the anesthesia is better, and the fillings last not a year but 5-10 years. But this is not a breakthrough, but only an improvement of traditional methods. Over half a century, medicine and medical prevention have made dramatic steps forward. If back in the 30-50s epidemics of cholera, measles, diphtheria, malaria and even typhoid and plague were considered normal, now we don’t even mention them.
Dentistry has actually experienced a rebirth, which is associated with the emergence of new polymer materials. So, from the 60-70s. The widespread introduction of polymer cements began, and from the late 80s - photopolymers. Until now, the quality of these materials has been constantly improving. However, typical medical inertia and often political processes have gotten in the way of the progress of dentistry. In particular, mass practical dentistry remains on the foundation of the methods of the 40-50s, according to which the treatment of caries remains a nerve-, time- and money-consuming procedure - and often with side effects and complications. Medical reforms during the Soviet period led to the curtailment of mass free clinics and their replacement with paid ones - especially in the field of dentistry. At the same time, such paid private points are rare in the regions. The Chuiko Institute of Surface Chemistry was among the first institutions in the world to create its own Laboratory of Biocompatible Materials. It developed some of the first photopolymer highly filled compositions for prosthetics and filling in the USSR and the world, documented in a number of articles, patents and dissertations [1-3]. Accordingly, the Ukrainian SSR and then Ukraine became the place for the first introduction of both innovative photopolymer dental pastes (Oxomat, Stomadent, Esta, etc.) and polymerizing devices (Sakura, Polident). All of them focused on acrylic monomers and oligomers and replaced conventional filling compounds. However, in our opinion, the main direction in the development of dentistry in the future should be the prevention of dental diseases and their treatment with minimal surgical intervention. Our experience has shown that this is possible when using ordinary available epoxy resins. The prospects for self-restoration with epoxy materials were described in general terms for the first time in our first publications [1-3], and above all in this publication [4].
Self-Dentistry – Reality from Scientific Hypothesis
Dreams and even assumptions about the possibility of independently preventing, and even more so self-curing (!) caries and dental damage appeared in our childhood. But traditional dentistry\medicine, the media and public opinion strictly indicated the limits of such possibilities - “take care of your teeth, and visit the dentist every six months,” and if a hole or damage is detected, - go for an appointment as soon as possible. Most of us have had dental problems since childhood. The love of sweets, the peculiarities of the region, nutritive or vital problems… baby teeth mercilessly deteriorated, chipped, rotted and, accordingly, hurt. Doctors filled them, but the fillings fell out, or carious zones appeared around them/under them. Quite early, baby teeth fell out or were pulled out (at the first signs of destruction or discomfort from the permanent tooth supporting it), and thus, by the age of 10-12, permanent teeth took over. Now, we know that baby teeth must be protected, used to the maximum and the moment of changing teeth delayed as long as possible. Even in adolescence (and even more so in childhood) there is still no strong immunity and ability to preserve teeth. As a result, by the age of 25, permanent teeth are half damaged or even partially torn out. This was acceptable in the primitive and even Middle Ages, when people did not live longer than 40-50 years, but now we live up to 80-90 years, and problem teeth haunt us for decades, poisoning our lives. If notice the teeth of cows and horses (when can across them on country roads) They had no obvious damages, but were often “multi-layered”: areas of white shiny enamel were replaced by clay-cement areas - hard and almost insoluble analogues of our “harmful tartar”. By keeping them in acids and oxidizing agents, it was possible to partially dissolve these “cemented” areas: underneath there were ordinary carious cavities or chips. Thus, in the process of chewing dusty grass, the animals automatically “chewed” microparticles of minerals into their carious cavities, and the grass resin served as a binder - which in the mouth (i.e. at 40 degrees) was pressed and turned into a hardening putty. If ordinary herbivores have such a simple self-healing mechanism, then why shouldn’t humans adopt it? What is wrong with our civilized food that teeth do not receive proper nutrition and building materials for self-repair of microdamages? However, folk traditions have done something (although not published) in the field of detailed preventive care. For example, there are tips from long-livers like “chew pine needles and plant resin, and you won’t get sick,” or recommendations to rinse your mouth repeatedly with bactericidal decoctions. This probably does not apply to all diseases, but it is obvious that bactericides from pine resins dramatically increase the hygiene and stability of the oral cavity and nasopharynx. And the teeth probably receive damage sealing with resin, which in a constantly heated mouth will then partially harden into something similar to young amber (Figure 1).
Experimental and Omparative Data
well reflect the difference in the approaches of traditional and our technique. The question should immediately arise (even among non-specialists) - how dare we exclude the most important stage of cleaning the surface of a damaged tooth, before filling. It should be answered like this. The stage of cleaning the surface (using a drill or other abrasive tool) leads to a strong (often leading to the loss of a nerve and even the entire tooth) cutting of living material. In this case, the relief of the tooth, bite, and the general ecosystem of the oral cavity can be noticeably disturbed. All these troubles are considered by dentists and patients as the inevitability of existing methods. Our method preserves maximum tooth structure. Abrasive-grinding cleaning before filling is replaced by repeated cleaning with a toothbrush and rinsing. The uncleaned fragments remaining on the tooth, being covered with epoxy polymer, are isolated or neutralized by the immune system - just as the skin neutralizes subcutaneous suppurations, or are partially embedded in the polymer. The last property of epoxides, the ability to use pus and carious masses as a hardener for polymerization, requires special attention in further research. Here we have an analogue of modern rust converters, when anti-corrosion treatment does not require preliminary cleaning of the corroded layer (Figures 2 & 3) (Table 1). Thus, we can talk about the discovery of a new highly demanded direction in medical materials science and dental technology - self-sealing. This will be very useful both in cases of difficult access to quality treatment, and for the treatment of special groups - for example, nomadic peoples and collectives, poor strata of the population, as well as children (milk teeth) and animals. Compared to traditional fillings (installed according to all the rules and with surface preparation), epoxy ones should be noticeably inferior in strength and durability. It is also clear from (Table 2) that epoxy materials, after exposure in water, significantly lose strength and durability. However, the first acrylic dental materials (50 years ago) were also far from ideal - they turned green, fell out, and poisoned the oral cavity. Further development of epoxy compounds will eliminate this drawback.
Table 1: The recorded effects according to the results of the first out-of-clinical restorations with epoxy composites.
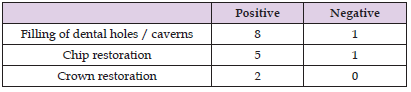
Table 2: Comparison of the strength and durability of epoxy composites in their original form and after exposure to a warm aqueous environment. *-Estimated generalized data.
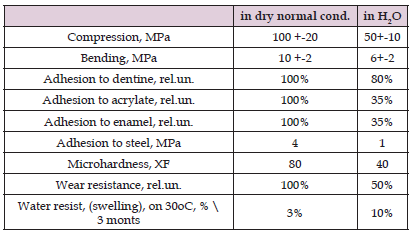
From (Table 2) can see that the service life of epoxy overlays is 10 times lower than for commercial medical fillings. This is also explained by the imperfection of the primary compositions and the lack of a broad base of research on the water resistance and resistance of the composite in the oral cavity. The quality of these compositions is also reduced due to the fact that we showed the possibilities only for ordinary, technical, commercially available polyepoxides and technical or available biocompatible fillers (gypsum, nanosilica, clay). Specially selected epoxy resins and fillers will certainly immediately increase service life, but of course they will become much more expensive and less accessible to the population. But (Table 3) show many preferences for this simple method of fast self-treatment. In many cases< patient can resolve the main dental problems without loss of finanes, nerves and time (Table 3). Our method allows you to get rid of most unnecessary visits, performing them yourself, in any conditions and without any payment for services. Finally, the absence of a surface preparation and cleaning step leaves many risks of infection and inflammation under epoxy overlays. But we do not propose to eliminate literally all problems with polyepoxides. We are talking about cases when you need:
a) First aid - for example, before the patient comes to the dentist. Removing the epoxy overlay does not require significant effort from a doctor.
b) In cases where medical assistance is impossible or unavailable
c) When doctors refuse to treat a tooth, for example by directing it to be removed, or explaining this by difficulties, neglect of the disease, etc.\
d) When a patient (for example, a child) is afraid of a doctor or does not have time for a quality appointment (for example, an employee working several jobs, a mother of many children, etc.).
e) When help is needed immediately - on the same day (for example, when part of a tooth breaks off, preventing you from eating or threatening to immediately collapse the entire tooth).
Table 3: Comparison of traditional and “self-epoxy” methods. * - according to the first tests, with a sample of 15 cases.
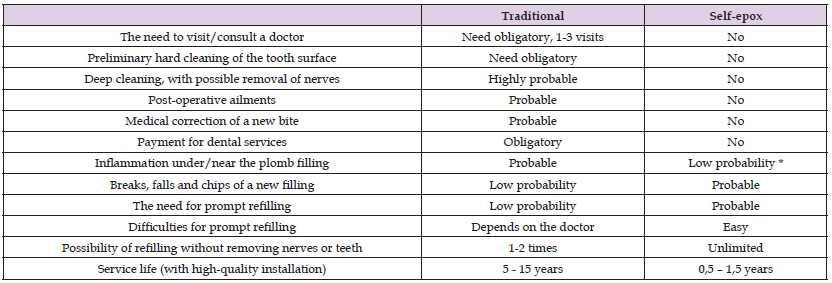
In fact, these fears about the ineffectiveness of epoxy self-treatment (to which the authors were also quite susceptible at the beginning of the work) turned out to be in vain. The remaining strength of dental epoxies is sufficient for normal chewing loads. Inflammations under fillings and onlays are not observed, and this phenomenon became the basis for the hypothesis about the utilization of purulent-microbial membranes and dental plaque by resin during its hardening into plastic. In case of peeling and loss of epoxies, it is easy to replace (even after 4-5 hours) with your own hands. In this case, the fallen off pad plays the role of a cleaning “sticky tape”, after which the adhesion of the much new poly-epoxide is higher.
Possibilities of Epoxies for Installing Auxiliary and Temporary Overlays on Weak Spots and Problematic Contact Areas. (D. Starokadomsky)
What do we do when the filling begins to behave suspiciously - food gets stuck, the bite is disturbed, wear and tear is felt and the relief is disturbed, and finally the tooth feels cold and bites? Most people sigh and move on with their lives, watching in fear as the problem expands; a minority will immediately go to the doctor. In rare cases (when the patient accidentally or himself finds a form of prevention), the problem is frozen. But in most cases, the patient still goes to dentist, fearfully anticipating the imminent operation, drilling and removal of dents. It seems that in every person’s practice there are often cases when dental care is either late or performed poorly. Dental work in a doctor’s office is an operation (albeit most often a mild one), and all the patient’s inconveniences during the operation (dependence on the doctor, anxiety, post-operative problems) are taken into account here. We are also well aware of the problems that arise even during a dental examination. For example, many doctors strive to find more holes and problems for subsequent treatment and (even sadder) strive to immediately “start treatment” before the patient comes to his senses and runs away.
At the same time, under various beautiful pretexts (“we’ll try to improve”, now we’ll just check”, etc.), a tooth or even two teeth are picked apart to the point where the patient can no longer leave without further treatment. If a simple operation fails, the doctor easily moves on to more complex procedures (sometimes without even warning) - further drilling and even removal of the nerve with long-term filling of the canals. It is clear even to a non-specialist that the tooth dies after this and soon (after 5-6 years) becomes the object of problems, further operations and removal. Only a small proportion of dentists try to fully preserve the nerve, and an even smaller proportion strive to cut into the dentin as little as possible. It is not surprising that most people on the planet do not dream of going to the dentist for either an examination or treatment. The last time (before I returned to developing dental compounds (after a pause of 10 years) I asked the dentist to simply strengthen a weaken “walking” filling. It will simply strengthen and not interfere with the depth of the tooth. He was a very friendly dentist (minimalist interventionist, largely relied on patient’s anti-caries immunity), he... still removed the old filling and cleaned the place. This led to the drilling out of most of the tooth - after which there was nothing left to put a filling on. Having placed a temporary filling, he refused further treatment, and after it quickly fell out, he said that the tooth needed to be removed. Several other dentists were even stricter (to remove this and the neighboring 8th one), and I never contacted them again. In the following year (this was in 2020), I hardly managed to restore this remnant of the half-tooth exposed by the boron (and at the same time the dilapidated 8-th neighboring one) for normal work using special powders (about which our article was [1-2]). Then, the idea arose of creating strengtheners and onlays from acrylic or epoxy materials -albeit fragile or short-lived, but publicly available and not requiring dental surgeries and doctors. And this idea has now been realized! We managed to create the world's first effective and publicly available epoxy fillings and onlays for long-term or temporary strengthening of old fillings. We can safely say that the dream of most people in the world has been realized, of being able to solve minor and even major dental problems on their own (Figures 4, 5 & 6). Epoxy overlays for fillings (that’s what we’ll call them for now: Overlays or Over-fillings) can be “stuck” not only on areas affected by caries (although this is the most important thing) or on chipped/uneven teeth - but also as a preventive measure - on weak fillings, areas of increased sensitivity or expected chips/cracks. Due to the relatively low adhesion of simple onlays to damp and poorly treated (with a simple toothbrush after eating) enamel, they can quickly fail (“fly off the tooth”). But the possibility of multiple (even endless) fast, and finance-free self-reinstallation allows you to:
a) Finally (in 3 or 4 cycles of reinstallations) install a durable overlay (over-filling);
b) Save the weak point of the tooth for full work (since in problem situations the onlay will break off and not the weak piece of the tooth);
c) Develop a new bite that is more comfortable at a given age and situation. Epoxy linings in the oral cavity are softer than tooth materials and any modern fillings.
This allows the teeth to self-align and grind to the desired bite even after the filling has cured, without going to the dentist. The tendency to fall off (with an unsuccessful composition and without surface preparation) can serve as an advantage - since, first of all, non-optimally established parts of the filling fall out (lateral sagging, under-adhesions with carious detachments,..) or linings that have come under traumatic loads (when biting hard fragments , impacts, etc.), and the protected tooth tissue is preserved.
Problems and Prospects of the New Method
In the practice of self-sealing, it is also important to monitor the development of defects in the new seal (split, exfoliated, worn) and in time to "grease" lost adhesion or weakened places. In home and other "self" conditions, it is easy, just choose 1-2 hours to make a new portion of the composition and 3-4 times light cleaning of the teeth with a brush, now the correction is with enhanced rinsing. Since now any correction does not require a visit or even a doctor's consultation, self-repair can be carried out several times a week - until the optimal seal is established. The process can be said to be identical in cost and risk to self-bandaging a festering wound or an insect bite. The new seal needs sealing of potentially dangerous contact points. Treatment with dental powders with a high proportion of plant resins (for example, coniferous, poplar, fruit resins) and fragments of hard plant covers (siliceous edges of grasses, pine powder, oak, sage) is suitable here. The technique of self-filling is still being formed, and its perfection requires putting up with a large percentage of primary and even secondary fillings falling out. However (taking into account the absence of the stage of cleaning the surface of the tooth with boron), even this turns out to be useful for the permanent installation of the epoxy polymer in the tooth.
Fallen and exfoliated first fillings act as surface cleaners, absorbing plaque from carious and food films and acting like tape-cleaner for clothes. The more cases of resealing, the greater the chance of durability and effectiveness of the new seal. Therefore, do not be upset if the first sealing attempt ended in failure - it gives more chances to a new demand.
Problems and Prospects of the New Method
In the practice of self-sealing, it is also important to monitor the development of defects in the new filling (chips, detachments, abrasions) and promptly “grease up” areas that have lost adhesion or weakened areas. At home and other “self” conditions, this is easy; just select 1-2 hours to prepare a new portion of the composition and lightly brush your teeth 3-4 times, now correction and with intensive rinsing. Since now any correction does not require a visit or even a consultation with a doctor, self-repair can be carried out several times a week - right up until the optimal filling is installed. The process is similar in cost and risk to self-bandaging a festering wound or insect bite. The new over-filling needs to seal potentially dangerous contact points. Here, treatment with tooth powders with a high proportion of plant resins (for example, pine, poplar, fruit) and fragments of hard plant covers (siliceous edges of grass, pine needle powder, oak, sage) is suitable. A noticeable limitation can be considered the recommendation to carefully return new over-filling to normal chewing loads. This is explained by the fact that ordinary epoxy finally hardens only after 2-3 days. This is the time to be careful. Here, however, we can note that even the best commercial fillings require careful treatment in the first days after the operation. The self-filling technique is still in its infancy, and its imperfections force us to put up with a high percentage of primary and even secondary fillings falling out. However (given the absence of the stage of cleaning the surface with a boron), even this turns out to be useful for the final installation of the epoxy polymer in the tooth. The first fillings that have fallen off and peeled off act as surface cleaners, absorbing plaque from carious and food films and acting like a scotch or clothing-cleaner. The more cases of refilling, the greater the chance for the durability and effectiveness of the new filling. Therefore, there is no need to be upset if the first filling experience ends in failure - it gives more chances to a new attempt.
1. Reasoning about the pattern of appearance of cheap affordable dental fillings and onlays for self-treatment is presented. Analogies with the advent of anti-corrosion treatment agents in technology (car service, plumbing) and new means of rapid self-disinfection in medicine (dermatology, pediatrics), are presented. It is emphasized that even imperfect self-dental compositions will significantly help humanity in solving the problems of prevention and treatment of dental diseases (especially in regions with weak or inaccessible expensive medicine).
2. Using the example of specific experimental work, the possibility of the existence of highly filled epoxy-mineral compositions capable of filling and restoring lesions and mechanical damage to teeth, independently and outside of clinical conditions, is shown.
3. The limitations and possibilities of compositions based on ordinary cheap available epoxy resins are shown. A comparison of their efficiency parameters with acrylic composites currently accepted in dental practice was carried out.
4. Based on the experimental results, the main limitations and disadvantages of these compositions are shown. Ways to overcome them are indicated.
5. These results will be very useful for people and communities who, for various reasons (remoteness from cities, business travel, poverty, workload) are temporarily or regularly left without access to quality dental services.


