Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Haibo Lu1,2,3, Shibi Lu3, Wenjing Xu3, Jiang Peng3, Aiyuan Wang3, Quanyi Guo*3, Yong Luo1, Chenyang Nie1 and Sen Li1
Received: March 27, 2018; Published: April 12, 2018
*Corresponding author: Quanyi Guo, Institute of Orthopedics of Chinese PLA, Chinese PLA General Hospital, Beijing, China
DOI: 10.26717/BJSTR.2018.03.000957
Most of prothrombin initially located within allograft bone matrix is removed or destroyed by deep-freezing, freeze-drying and gamma irradiation. Prothrombin is an inactive precursor to thrombin, a key factor which can promote bone healing. Therefore, we hypothesis that topical administration of autologous prothrombin at sites of bone allografts might be helpful in promoting bone healing after bone allograft transplantation and suggest appropriate amount of venous blood be harvested to concentrate autologous prothrombin before bone allograft transplantation.
Keywords: Prothrombin; Bone Allograft; Bone Healing; Deep-Freezing; Freeze-Drying; Gamma Irradiation
Allograft bones are most commonly used materials for bone defects. Before being implanted, allograft bones are prepared by deep-freezing, freeze-drying and gamma irradiation to decrease the immunogenicity and the risk of disease transmission [1-3]. However, these methods can also get rid of or destroy most of osteoinductive proteins within the bone matrix. Therefore, these methods can compromise the bone healing of bone allografts and are related to unsatisfactory clinical outcomes. The incidence of fracture after implantation of large structural bone allografts was reported to be 5% ~ 20%, and that of non-union, 10% ~15% [2]. We hypothesise that topical administration of autologous prothrombin at sites of bone allografts might be helpful in promoting bone healing after bone allograft transplantation. Prothrombin (PT, or coagulation factor II) is the coagulation factor present in the highest concentration in blood (0.07mg/ml~0.1mg/ml) [4].
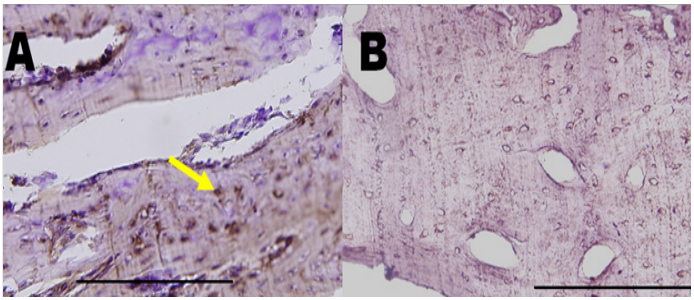
Figure 1: Most of prothrombin within the matrix of bones are removed and destroyed by freeze-drying and irradiation. A: fresh cortical bone of rat proximal femur; B: freeze-dried and irradiated cortical bone of rat proximal femur; yellow arrow, prothrombin. Immunohistochemistry stain; Bar length, 200 μm.
It is an inactive precursor to the serine protease a-thrombin, a key factor which can not only trigger the cascade of coagulation, but also promote bone healing [5-7]. Conversion of PT to thrombin occurs in the prothrombinase complex, where PT together with coagulation factor Xa and factor Va are bound to negatively charged phospholipids on cell surfaces [8]. Recently, some researchers have found that prothrombin is synthesized and proteolytically processed in bone, and is present mainly in the newly formed bone matrix of metaphyseal trabecular bones [9]. Therefore, we consider prothrombin a helpful factor which might participate bone healing. And because most of prothrombin within the matrix of bones are removed and destroyed by freeze-drying and irradiation (Figure 1), topical supplement of prothrombin initially present within bone matrix might be helpful to promote bone healing of allograft bones. We suggest before bone allograft transplantation, 50 ml~100 ml venous blood of the patient be harvested to concentrate autologous prothrombin by a safe and simple method [10]. Then the concentrated autologous prothrombin can be impregnated into bone allografts and implanted with bone allografts.


