Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Navjot Kaur Parmar, Nisha KJ*, Sanjeela Guru and Shyam Padmanabhan
Received: December 19, 2017; Published: January 05, 2018
Corresponding author: Dr. Nisha KJ, Dept. of Periodontics, Vydehi Institute of Dental Sciences and Research Centre, EPIP Zone, Whitefield, Bangalore, Karnataka, India
DOI: 10.26717/BJSTR.2018.02.000632
Matrixmetalloproteinases (MMPs) belong to family of proteolytic enzymes that cause degradation of extracellular matrix macromolecules, including interstitial and basement membrane collagens, fibronectin, laminin and proteoglycan core protein by secreting enzymes in latent form; which later gets activated in the pericellular environment by disruption of a Zn++ cysteine bond. There is much evidence for the role of matrix metalloproteinases in the destructive processes of periodontal disease distinguishing them as a viable target for a chemotherapeutic approach. The use of a host modulatory agent such as a matrix metalloproteinase inhibitor can assist with conventional treatment for periodontitis and, when used adjunctively, can enhance and make clinical therapeutic responses more predictable in the more susceptible patient.
Keywords: Matrixmetalloproteinases; Periodontal disease; Inflammation
Abbreviations: MMPs: Matrixmetalloproteinases; ECM: Extracellular Matrix; GCF: Gingival Crevicular Fluid; IFMA: Immunofluorometric Assay
Periodontal disease is a common, complex, inflammatory disease characterized by the destruction of tooth supporting soft and hard tissues of the periodontium, including alveolar bone and periodontal ligament. Although the inflammation is initiated by bacteria, the tissues breakdown events that lead to the clinical signs of disease result from the host inflammatory response that develops to combat the challenge presented by the subgingival biofilm. Microbial products trigger the release of pro inflammatory cytokines and host derived enzymes, the excessive and/or dysregulated production of which results in tissue breakdown. Once the immune and inflammatory processes are initiated and the complex cytokine network is established, various inflammatory molecules play a direct role in the degradation of both non mineralized and mineralized tissues of the periodontium. One such family of inflammatory molecules is the matrix metalloproteinases which are released from different cell types present in the lesion including macrophages, leukocytes and fibroblasts or other resident cells. Human MMPs also called as Matrixins, are a group of structurally related but genetically distinct endopeptidase enzymes. They are produced at low levels or not at all in restingstate adult tissues. Control of extracellular proteolysis by MMP is critically important for survival of organisms, and this is performed by interaction with various inhibitors like endogenous inhibitors, TIMPs. This review article gives an overview of the physiological functions of MMPs and its role in the pathogenesis of periodontal diseases.
Study by Woessner [1] was considered as a milestone before the discovery of first MMP, Later in that year, Jerome Gross and Charles Lapiere [2] were the first to identify an MMP using a biochemical approach. In 1966, MMP-1 was purified from tadpole tail fin and back skin. MMP-2 was identified as a higher molecular mass species (72 kDa) with gelatinolytic activity; purified from human rheumatoid synovial fibroblasts by Goldberg and colleagues whereas MMP-3 was identified as a lower molecular mass species (54 kDa) from rabbit synovial fibroblasts by the Werb laboratory in 1985 and subsequently named Stromelysin [3]. In the late 1980s, Ed Harris et al. [4] first proposed the name MMP. Subsequently, the International Union of Biochemistry and Molecular Biology designated the family with the unique name MMPs and assigned each family member with an enzyme number. To be classified as an MMP family member, the enzyme should meet the following requirements:
a) proteolysis of at least one extracellular matrix(ECM) component
b) catalysis dependent on zinc at the active site
c) activation by proteinases or organomercurials
d) inhibited by EDTA,10-phenanthroline and any one of the TIMPs
e) cDNA has sequence homology to MMP-1
Initially it was thought that the proteinase be secreted in a proform but now this no longer holds as MMP-11 and MMP-28 are intracellular activated by furin and are secreted in active forms; even the membrane-bound MMPs are not necessarily secreted [5].
a. Based on the substrate specificity MMPs are classified into the following types [6].
b. Collagenases -MMP-1, MMP-8, MMP-13
c. Gelatinases- MMP-2, MMP-9
d. Stromelysins- MMP-3, MMP-10,MMP-11,MMP-12
e. Matrilysins- MMP-7, MMP-26
f. MT-MMPs (Membrane type) -MMP-14, MMP-15, MMP-16, MMP-17, MMP-24
g. Other MMPs- MMP-18,MMP-19,MMP-20, MMP-21,MMP- 23,MMP-27,MMP-28
MMPs are structurally similar but differ in substrate specificity. T he following features are seen in the structure [7]:
a. Signal peptide
b. Propeptide
c. Furin-cleavage site insert
d. Catalytic domain
e. Fibronectin-like repeats
f. Hinge region
g. Hemopexin domain
h. Membrane insertion extension
Modes of action of MMPs are as follows [8]:
a. MMPs may affect cell migration by changing the cells from an adhesive to non adhesive phenotype and by degrading the ECM.
b. MMPs may alter ECM microenvironment leading to cell proliferation, apoptosis, or morphogenesis.
c. MMPs may modulate the activity of biologically active molecules such as growth factors or growth factor receptors by cleaving them or releasing them from the ECM.
d. MMPs may alter the balance of protease activity by cleaving the enzymes or their inhibitors.
The activity of MMP against extracellular matrix substrates is regulated at 4 “gates” [9]:
I. Transcriptional regulation of MMP genes
II. Precursor activation
III. Differences in substrate specificity
IV. MMP inhibitors.
In periodontal diseases, MMPs play key role in the degradation of the ECM, basement membrane and protective serpins as well as in the modification of cytokine action and activation of osteoclasts. Organisms like Porphyromonas gingivalis and Aggregatibacter actinomycetemcomitans do produce collagenases for the breakdown of ECM but they do not help much in periodontal collagen degradation. One way to differentiate between mammalian and bacterial collagenases is by their different mode of collagenolysismammalian collagenase cleaves the undenatured triple helical collagen molecule at a single site resulting in characteristic 3/4 and 1/4 fragments, whereas bacterial collagenase attacks the collagen substrate at multiple sites resulting in more than 200 peptide fragments. The extracellular matrix not only consists of collagen fibrils but also their associated proteoglycans and fibronectin which must be removed first in order for the collagenase to have access to the collagen substrate. MMP-3 (stromelysin) is effective at degrading proteoglycans and fibronectin [10].
Both resident gingival and periodontal ligament fibroblasts produce collagenases that are thought to be involved in normal tissue turnover. Inflammatory cells such as neutrophils and macrophages are also responsible for production of MMPs with neutrophils being the major source of collagenase and gelatinase in inflammatory diseases such as periodontitis [11,12]. Epithelial cells can also produce elevated levels of these enzymes, which may facilitate the apical migration and lateral extension of the junctional epithelium and the subsequent loss of connective tissue attachment [13]. The evidence for the role of MMPs in periodontal destruction is strong and has been supported over many years by a number of studies; few of them are quoted in the Table 1.
Table 1: Studies related to MMPs.
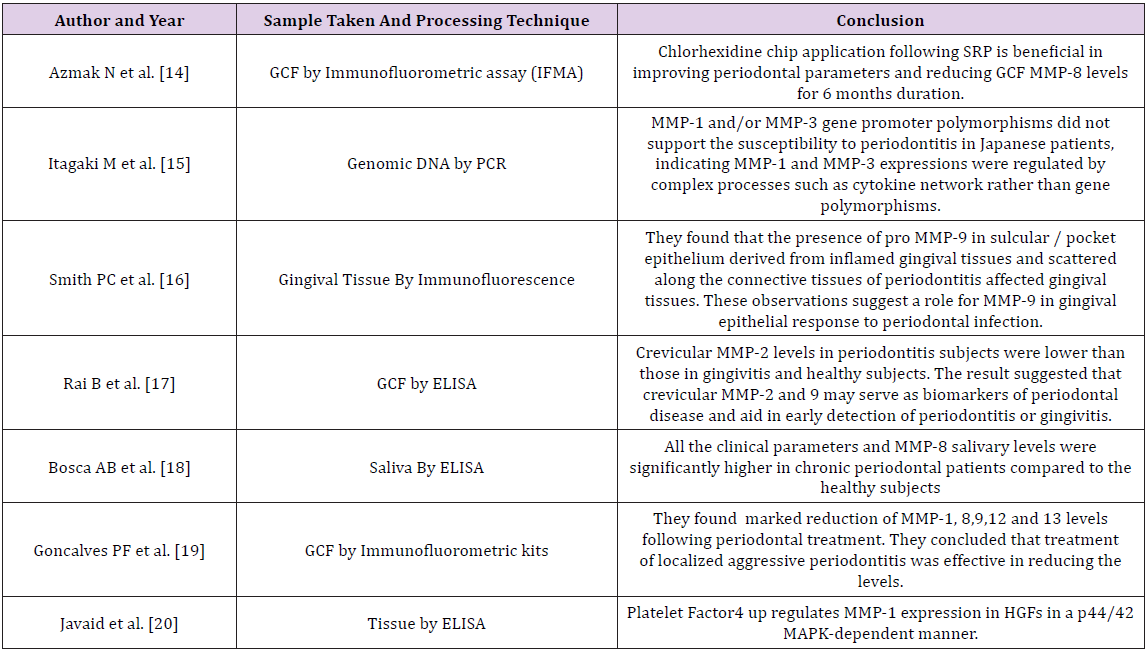
Matrix metalloproteinases can also process various bioactive non matrix substrates, such as cytokines, chemokines, growth factors and immune mediators, thereby mediating both anti and pro-inflammatory processes. Therefore, the levels of matrix metalloproteinases should not be interpreted solely as surrogate markers of tissue destruction but also as part of physiological or anti-inflammatory defense [21]. Based on these biochemical or immunological findings, the oral fluids have been a target for extensive research on diagnostic utilization of MMPs and their regulators as potential candidates in chair-side tests for monitoring periodontal and peri-implant diseases [21]. Samples collected to estimate the levels of different MMPs include- Saliva, GCF, and Tissue sample. Various proteomic techniques are being used to estimate the levels of these MMPs which are listed in Table 2.
Table 2: Proteomics techniques.
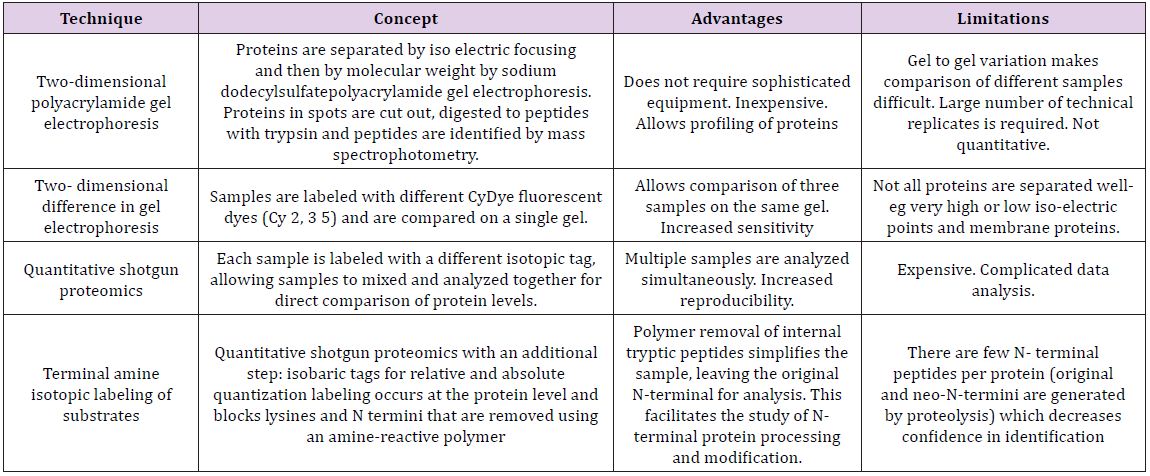
A disturbed balance between MMPs and TIMPs might contribute to the disease process in degenerative diseases. Similar patterns of MMP and TIMP expression can be found in different diseases involving matrix degradation. In some cases, the occurrence of MMPs and TIMPs in body fluids such as saliva, gingival crevicular fluid (GCF), or serum provides additional information about the progression of the disease. In healthy periodontal tissue, TIMP levels are generally higher than in inflamed periodontal tissue, in which MMP levels exceed TIMP levels. The more severe the inflammation, the higher the concentrations of active MMPs. In GCF and in gingiva from humans, MMP-1, -2, -3, and -9 are significantly increased, whereas TIMP-1 and -2 are significantly decreased. The inhibition of MMP expression or activity, or increased TIMP expression, might reduce tissue destruction in periodontitis.
Different inhibitors include [22]:
a. Alpha 2- macroglobulins
b. Tissue inhibitors of metalloproteinases
c. Inhibiting antibodies
d. Synthetic inhibitors
Endogenous or natural inhibitors such as tissue inhibitors of matrix metalloproteinases and Alpha 2-macroglobulin bind in a non-covalent fashion to members of the matrix metalloproteinase family. TIMPS probably control matrix metalloproteinase activities pericellularly, whereas Alpha 2-macroglobulin functions as a regulator in body fluids. During inflammation, however, the latter high-molecular-weight protein may escape the vasculature and also function in the extracellular matrix [10]. Multiple synthetic peptides have been formulated in an attempt to synthesize more specific chelators including phosphorus containing peptides, sulfur-based inhibitors and peptidyl hydroxamic acid derivatives.
The most widely used synthetic peptides, and the ones receiving the most attention as potential pharmaceutical agents, are the hydroxamic acid derivative. Synthetic Inhibitors of MMPs fall into three pharmacologic categories [23]:
a. Collagen peptidomimetics and non peptidomimetics, Peptidomimetic MMP Inhibitors- Batimastat, Marimastat Nonpeptidic MMP Inhibitors - BAY 12–9566, AG3340, BMS- 275291, CGS-27023A
b. Tetracycline derivatives- Doxycycline, Col-3 (metastat)
c. Bisphosphonates (Figure 1).
Figure 1: Action of various inhibitors at different levels [24].
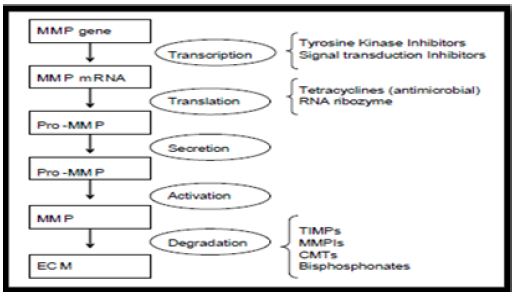
Various studies have been done to evaluate the effect of TIMPs on periodontium. Few of them are listed in Tables 3 & 4.
Table 3: Studies Pertaining to MMPs inhibitors.
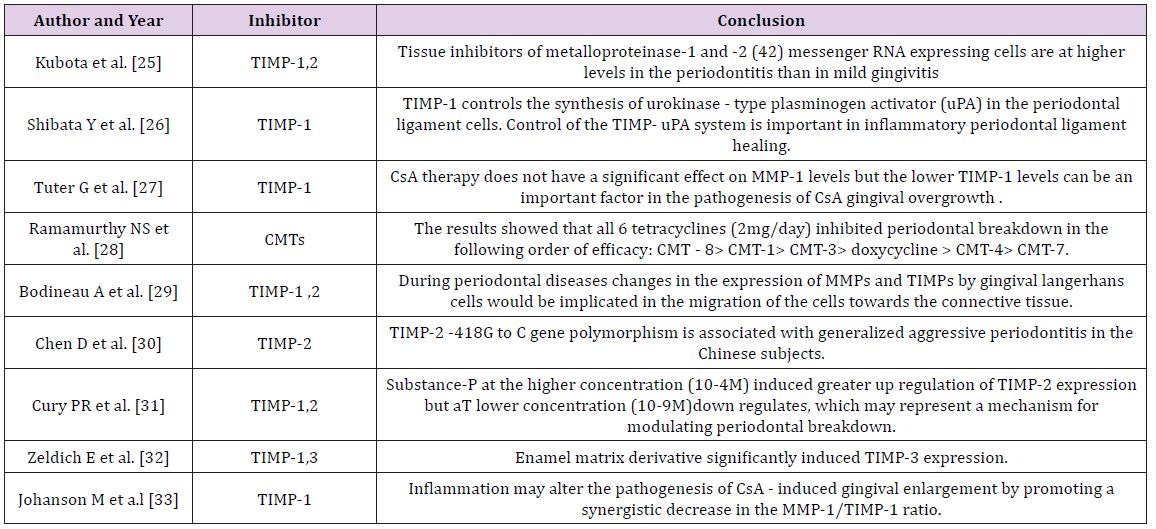
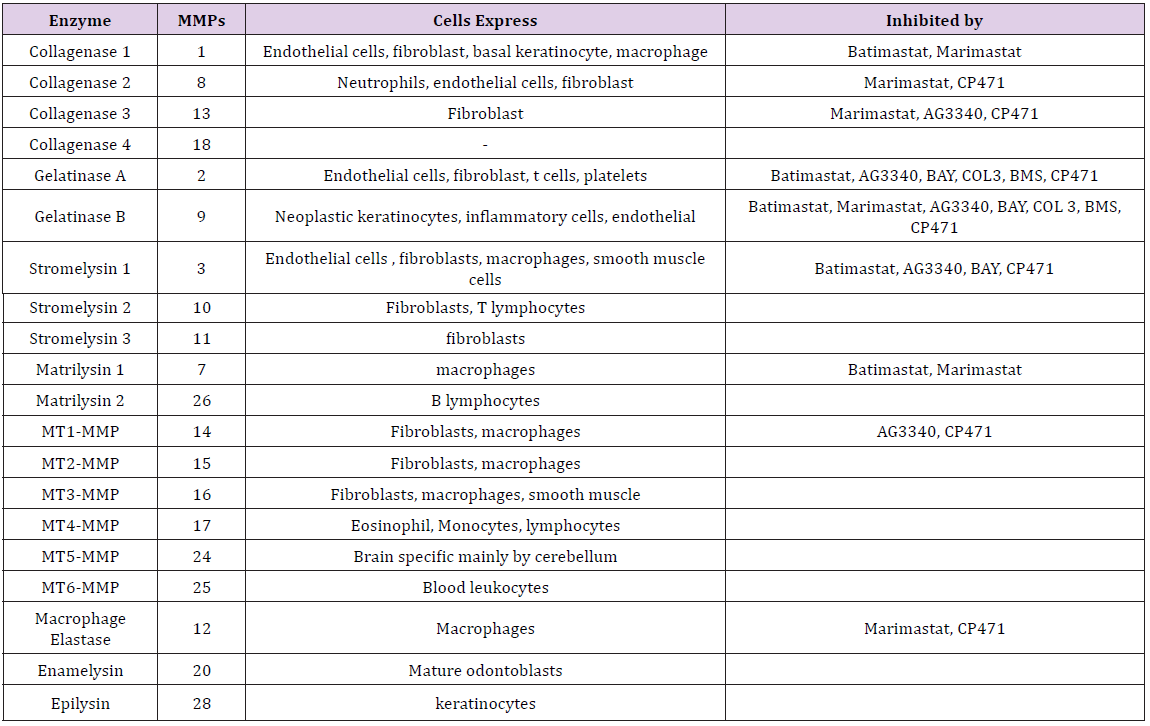
Table 4: Various MMPs and their inhibitors.
There is much evidence for the role of matrix metalloproteinases in the destructive processes of periodontal disease distinguishing them as a viable target for a chemotherapeutic approach. The use of a host modulatory agent such as a matrix metalloproteinase inhibitor can assist with conventional treatment for periodontitis and, when used adjunctively, can enhance and make clinical therapeutic responses more predictable in the more susceptible patient.

