Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Urmanova Yu M1*, Rikhsiyeva NT1, Ivanov NV2, Vasilkova ON3, Bolshakova SV4, Ermakova MK5 and Alieva DA6
Received: February 10, 2026; Published: February 23, 2026
*Corresponding author: Urmanova YuM, Alfraganus University, Department of Internal Medicine (Republic of Uzbekistan, Tashkent, 100190, Y. Karakamysh St. 2A), Uzbekistan
DOI: 10.26717/BJSTR.2026.64.010106
The Aim of the Study: To study the clinical and hormonal characteristics of patients with giant non-functional pituitary adenomas (NFPA).
Material and Methods of Research: The research material is presented on the basis of an analysis of a pro- (151 patients) and retrospective (121 patients) study of the frequency of macro- and giant non-functional pituitary adenomas for the period 2023-2024, based on requests from three leading centers in Tashkent. Depending on the size of the pituitary adenoma, prospective (151 patients) patients were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant NFPA - 96 people who consider tumours to be giant, respectively, more30 mm and 40 mm.
Research Results: The most common were functional hyperprolactinemia (82.7% of 151 patients), secondary hypogonadism (73.5%), panhypopituitarism (50.3%), hypopituitarism (STH, LH, FSH) (76.8%), bitemporal hemianopsia (62.3%), secondary amenorrhea (33.7%), isolated GHD (44.3%), grade 1-2 obesity (25.2%), and endocrine encephalopathy (21.1%) in groups 1 and 2, respectively. Less common were disorders such as postoperative secondary osteopenia (14.5%), panhypopituitarism (13.2%), postoperative hypothyroidism (8.6%). Thus, there was a polymorphism of symptoms.
Conclusions:
1. Data analysis revealed that giant pituitary adenomas are accompanied by a wide range of clinical manifestations. The most common disorders in patients were functional hyperprolactinemia (62%/92%) and secondary hypogonadism (42%/92%). A significant proportion of patients also suffered from hypopituitarism (89%/70%) and bitemporal hemianopsia (82%/51%).
2. Panhypopituitarism (10%/73%), secondary amenorrhea (40%/30.5%), isolated growth hormone deficiency (20%/58%), endocrine encephalopathy (16%/27%) and obesity (20%/28%) were observed with different frequencies in the first and second groups. Less common, but still present, were postoperative panhypopituitarism (12%/17%), secondary osteopenia (9%/17%), and Babinski’s sign (0%/3%). Thus, the clinical picture of the disease was characterized by pronounced polymorphism.
Keywords: NFPA; Clinic; Hormones
Abbreviations: NFPA: Non-Functional Pituitary Adenomas; STH: Growth Hormone; LH: Luteinizing Hormone; FSH: Follicle-Stimulating Hormone; TSH: Thyroid-Stimulating Hormone; ACTH: Adrenocorticotropic Hormone; IHC: Immunohistochemically Studies; TPA: Transnasal Pituitary Adenomectomy; PA: Pituitary Adenoma; GHD: Growth Hormone Deficiency
Non-functional pituitary adenomas (NFPA) are benign tumors originating from adenohypophyseal cells and account for approximately one-third of all pituitary adenomas. Based on the expression of anterior pituitary hormones and pituitary-specific transcription factors, gonadotropic tumors predominate in the NFPA group, followed by corticotropic tumors. However, other, less common phenotypes can also be identified. Assessing the proliferative activity of tumor cells is a key factor in identifying “high-risk adenomas.” It should be noted that several NFPA subtypes are classified as potentially aggressive tumors, regardless of their proliferative index.cells [1]. Microadenomas, unlike macroadenomas, do not cause symptoms of compression of surrounding tissues (neurological or ophthalmological). However, as with larger tumors, they may be accompanied by elevated prolactin levels, the cause of which is still unclear. In the early stages of the disease, patients with microadenomas often experience decreased production of growth hormone (STH). As the tumor grows, persistent pituitary dysfunction occurs, manifested by decreased levels of luteinizing hormone (LH), follicle-stimulating hormone (FSH), thyroid-stimulating hormone (TSH), and adrenocorticotropic hormone (ACTH) against a background of functional hyperprolactinemia. This can lead to partial or complete hypopituitarism, impaired reproductive function, infertility, and decreased libido [2].
Instrumental methods play a key role in diagnosing NFPA. However, a thorough medical history and clinical assessment allow for the detection of adenomas at earlier stages. German researchers, studying 517 patients, found that women with NFPA seek help on average two years after the onset of symptoms, which is twice as long as men (one year) [3]. The most common initial symptoms are oligospermia or decreased potency (57.9%), visual field defects (11.6%), and headache (11.3%). According to other sources [4], reproductive dysfunction may be observed in a significant proportion of patients with NFPA —up to 78.3%. Interestingly, in 28% of patients with an “active” tumor, endocrine disorders are not clinically evident [5-8]. In general, pituitary tumors are not traditionally associated with endocrine symptoms caused by hypersecretion of anterior pituitary hormones. Their clinical manifestations are primarily determined by the mass effect of the tumor in the sella turcica [9,10]. A retrospective study of 159 patients with a confirmed diagnosis revealed that in men aged 31-50 years, the first endocrinological manifestations of an “active” pituitary tumor manifest as sexual dysfunction (decreased libido) in 65% of cases. Moreover, in 54.7% of cases, these symptoms are mistakenly assessed as age-related changes, which leads to an incorrect diagnostic search and, consequently, a late diagnosis of the tumor at the stage of chiasmatic syndrome. All of the above formed the basis for this study.
to study the clinical and hormonal characteristics of patients with giant inactive pituitary adenomas.
The study material is presented on the basis of the analysis of a pro- (151 patients) and retrospective (121 patients) study of the frequency of macro- and giant NFPA for the period 2023-2024 based on the data of requests from three leading centers of Tashkent: the Republican Scientific and Practical Medical Center of Endocrinology of the Ministry of Health of the Republic of Uzbekistan named after Academician E.Kh. Turakulov, the Scientific Center of Neurosurgery of the Ministry of Health of the Republic of Uzbekistan and the Scientific Center of Emergency Medical Care of the Ministry of Health of the Republic of Uzbekistan (Figure 1): a total of 272 patients with macroand giant NFPA s. The study prospectively enrolled 151 patients with macro- and giant NFPA s (men and women) treated at the Neuroendocrinology Department of the Russian Scientific and Practical Medical Center of Endocrinology, Ministry of Health of the Republic of Uzbekistan named after Academician Y.Kh. Turakulov during the specified periods. Of these, 85 (56.3%) were men and 66 (43.7%) were women; they were followed continuously. The average age was 48.12 years for men and 46.15 years for women. Disease duration ranged from 2 months to 5 years. The control group consisted of 20 healthy individuals of the same sex and age.
According to the size of the pituitary adenoma, prospective patients (151 patients) were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant NFPA - 96 people.
Table 1 shows the distribution of patients by gender and age (data from a prospective study).
• Inclusion Criteria: NFPA, women, men, macro and giant NFPA.
• Exclusion Criteria: other types of pituitary adenomas, pituitary microadenomas, severe somatic diseases and endocrinopathies The research methods included:
1) General clinical (examination of endocrine and neurological status),
2) Instrumental (perimetry in all colors, fundus, visual acuity,
3) ECG, CT/MRI of the sella turcica and adrenal glands,
4) Ultrasound of internal and genital organs, etc.),
5) Hormonal blood tests (STH, IGF-1, LH, FSH, PRL, TSH, ACTH, prolactin, testosterone, estradiol, progesterone, cortisol (chemiluminescence studies of blood serum).
In addition, the postoperative material was subjected to histological diagnostics at the RSPC E MH RUz named after academician E.Kh. Turakulov (histology room). Immunohistochemically studies (IHC) were performed under a contract at the pathomorphology laboratory of IPSUM Pathology LLC. The study was performed under a contract at the IHC laboratory at the Tashkent City Oncology Clinic. Paraffin-embedded blocks with confirmed diagnoses of pituitary adenoma were used. Serial 3-μm-thick sections were deparaffinized, dehydrated, unmasked, and stained with antigens using a specialized automated Ventana Benchmark XT system (Roche, Switzerland). The study was performed with ki-67 (30-9) and P53 (Bp53-11) antibodies. Ki67. IHC assessment of sections: the proliferative activity of tumor cells in the nuclear compartment was assessed. P53. IHC assessment of sections: To verify abnormal (mutant) p53 expression, expression in more than 75% of cells in the affected area was considered. Negative expression or weak staining of the nuclear locus in up to 70% of cells was interpreted as the natural (wild) type. Patients in our study received the following treatments: transnasal pituitary adenomectomy (TPA) was performed in all 151 prospective and 121 retrospective patients. Additionally, 87 patients underwent radiation therapy to prevent tumor growth.
Furthermore, 10 patients with giant NFPA s received the somatostatin analogue Sandostatin-Lar after TPA (transnazal pituitary adenomectomiya) to prevent tumor recurrence. The obtained data were processed using Microsoft Excel and STATISTICA_6 computer programs. The arithmetic mean (M) was calculated, standard deviation of the arithmetic meanor the error of the arithmetic mean of all n repetitions (m). The significance of differences in levels between groups was assessed using the confidence interval and Student’s t-test (p). Differences were considered statistically significant at p<0.05.
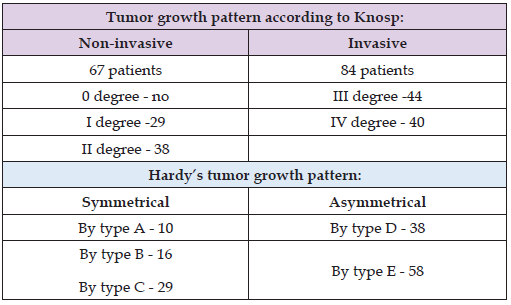
A total of 151 patients with macro- and giant pituitary adenomas were prospectively examined. Depending on the size of the pituitary adenoma, the prospective (151 patients) patients were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant pituitary adenomas - 96 people. In our study, we relied on the classification of Kurokawa Y., (1998), who considers tumors correspondingly larger to be giant.30 mmAnd40 mm. CT and MRI of the sella turcica allowed us to identify pituitary adenoma (PA) in our patients according to the radiological classification of Knoss and Hardy (Table 2): Thus, among 151 patients, tumor growth was more often invasive in nature – 84 cases (55.7%) and more often the growth pattern was asymmetrical – 96 (63.5%) cases out of 151. Next, we performed an analysis of neuroendocrine disorders in both groups (Table 3). As can be seen from Table 3, it was revealed that the most common were functional hyperprolactinemia (82.7% of 151 patients), secondary hypogonadism (73.5%), pan hypopituitarism (50.3%), hypopituitarism (STH, LH, FSH) (76.8%), bitemporal hemianopsia (62.3%), secondary amenorrhea (33.7%), isolated GHD (growth hormone deficiency) (44.3%), grade 1-2 obesity (25.2%), and endocrine encephalopathy (21.1%) in groups 1 and 2, respectively. Less common were disorders such as postoperative secondary osteopenia (14.5%), panhypopituitarism (13.2%), postoperative hypothyroidism (8.6%).
Table 2: Distribution of patients according to the topographic-anatomical classification of the side of pituitary adenoma growth according to Knospe and Hardy.
Note: DI – diabetes insipidus, GHD – growth hormone deficiency, * – significance of differences between groups 1 and 2 when p < 0.05, ** – when p < 0.001.
Thus, there was a polymorphism of symptoms. Furthermore, the most pronounced neurological impairments were manifested by symptoms such as oral automatism (43.7%), endocrine encephalopathy (21.2%), ischemic stroke (1.3%), hallucinations (0.6%), inappropriate state (0.6%), Babinski’s sign (1.9%), and decreased muscle tone (2.6%), respectively. Moreover, neurological symptoms such as Babinski’s sign and decreased muscle tone were characteristic of tumor growth into the brain, and these symptoms predominated in patients with giant NFPA s. Disorders such as secondary osteopenia and endocrine encephalopathy were detected only in patients in Group 2. Thus, the most severe neuroendocrine and ophthalmological diseases were observed in patients in Group 2. Tables 4 & 5 show the mean basal plasma hormone levels by group. As can be seen from the data in Table 4, the levels of tropic hormones (LH, FSH, STH) in Group 1 were significantly reduced (p < 0.005) compared to the control group against the background of significantly increased PRL and low free testosterone (p < 0.005). The levels of free thyroxine and ACTH were within normal limits. The clinical picture of hypogonadotropic hypogonadism was characteristic of patients in Group 1. Table 5 shows the average value of plasma hormones in patients of group 2 is given.
Note: P - significance of differences compared to the control group.
Note: P - significance of differences compared to the control group.
As can be seen from Tables 4 and 5, the most significant decrease in the mean basal plasma tropic hormone levels—STH, LH, FSH, and ACTH—was observed in patients in Group 2. They were characterized by a clinical picture of hypogonadotropic hypogonadism and secondary hypocorticism. Cortisol and IGF-1 levels were significantly reduced in these patients, while ACTH and IGF-1 were within normal limits in patients in Group 1. In addition, based on the comparative characteristics of the size of the sellar tumor and the level of STH, we identified a tendency for the basal level of STH in the plasma to decrease as the size of the sella turcica formation increased. Hypogonadotropic hypogonadism is reported in half of men with NFPA preoperatively. Pituitary surgery restores normal serum total testosterone (T) concentrations in 71% of cases. The presence of low total T levels with low gonadotropin concentrations in two cases suggests central hypogonadism. If the diagnosis is in doubt, sex hormone-binding globulin and free T levels should be assessed [11]. Premenopausal women with hypogonadotropic hypogonadism often experience menstrual irregularities, amenorrhea, ovulation disorders, and infertility. Diagnosis requires a low serum estradiol level with normal gonadotropin levels. Twenty-five percent of women with hypogonadotropic hypogonadism had hypogonadism before surgery. In 15% of women with hypogonadotropic hypogonadism, hypogonadism improves after pituitary surgery [12].
Growth hormone deficiency (GHD) has been described in 79% of patients with NFPA in the early postoperative period. Recovery of growth hormone axis function has been reported within 1–2 years after surgery, and this occurs more frequently in younger patients and in patients with isolated GHD [13]. Thus, in general, the average values of pituitary tropic hormones decreased in patients of both groups, but most significantly in patients with giant pituitary adenomas. In patients with giant pituitary adenomas, the first to be observed is a decrease in the levels of STH, FSH, and LH (45%). The most pronounced neuroendocrine and ophthalmological disorders occurred in patients of the 2nd group with giant pituitary adenomas. Obvious neurological disorders in the form of Diencephalic-stem disorders (pyramidal symptoms, decreased reflexes and diffuse muscle tone) were observed in patients with a total growth variant, with retrosellar growth and with invasion into the brain.
1. Data analysis revealed that giant pituitary adenomas are accompanied by a wide range of clinical manifestations. The most common disorders in patients were functional hyperprolactinemia (62%/92%) and secondary hypogonadism (42%/92%). A significant proportion of patients also suffered from hypopituitarism (89%/70%) and bitemporal hemianopsia (82%/51%).
2. Panhypopituitarism (10%/73%), secondary amenorrhea (40%/30.5%), isolated growth hormone deficiency (20%/58%), endocrine encephalopathy (16%/27%) and obesity (20%/28%) were observed with different frequencies in the first and second groups. Less common, but still present, were postoperative panhypopituitarism (12%/17%), secondary osteopenia (9%/17%), and Babinski’s sign (0%/3%). Thus, the clinical picture of the disease was characterized by pronounced polymorphism.

