Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Urmanova Yu M1*, Rikhsiyeva N T1, Pankiv V A2, Tashmanova A B3, Alieva D A4, Mirtukhtaeva M B4 and Urmanova F M5
Received: February 10, 2026; Published: February 19, 2026
*Corresponding author: Urmanova Yu M, Alfraganus University, Department of Internal Medicine (Republic of Uzbekistan, Tashkent, 100190, Y. Karakamysh St. 2A), Uzbekistan
DOI: 10.26717/BJSTR.2026.64.010101
The aim of the study is to study the neuroimaging characteristics of patients with giant inactive pituitary adenomas. Material and Methods of Research: The research material is presented on the basis of an analysis of a pro- (151 patients) and retrospective (121 patients) study of the frequency of macro- and giant non-functional pituitary adenomas (NFPA) for the period 2023-2024, based on requests from three leading centers in Tashkent. According to the size of the pituitary adenoma, prospective patients (151 patients) were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant NFPA - 96 people. The research methods included:
1. General clinical (examination of endocrine and neurological status),
2. Instrumental (perimetry in all colors, fundus, visual acuity,
3. ECG, CT/MRI of the sella turcica and adrenal glands,
4. Ultrasound of internal and genital organs, etc.),
5. Hormonal blood tests (STH, IGF-1, LH, FSH, PRL, TSH, ACTH, prolactin, testosterone, estradiol, progesterone,
cortisol
Results of the Study: Hemorrhage into the pituitary stroma occurred in 5 (9.09%)/12 (12.5%) cases, parasellar invasion – in 42 (76.4%)/78 (81.3%), suprasellar growth – in 45 (81.8%)/49 (51.0%), infrasellar expansion - 44 (80%)/57 (59.4%), expansion of the third ventricle - 32 (58.2%)/57 (59.4%) cases in groups 1 and 2, respectively. Tumor growth recurrence after TPA (transnazal pituitary adenomectomiya) occurred in 15 patients out of 150 (10%). Invasion into the brain was noted in 10/25 cases (18.2%/26.0%).
Conclusion:
1. Patients with giant pituitary adenomas showed pronounced neuroendocrine, neurological and ophthalmological
disorders. The most pronounced visual field disturbances in the form of bitemporal hemianopsia (45/49 cases) were
observed in 127 patients with endosuprasellar tumor growth.
2. Based on our analysis of pituitary MRI data from both groups of patients with NAG, we found that in patients in
Group 1, suprasellar tumor growth was predominant – 25 cases (45.4%), while in Group 2, total tumor growth was
observed – 69 cases (71.8%). In Group 2, retrosellar tumor growth was also observed – 9 cases (9.4%). Furthermore,
in 127 (84.1%) of 151 patients, tumor growth was endosuprasellar.
Keywords: NFPA; CT; MRI
Abbreviations: MRI: Magnetic Resonance Imaging; GPAs: Giant Pituitary Adenomas; TPA: Transnasal Pituitary Adenomectomy; AH: Arterial Hypertension; WHO: World Health Organization; PCOS: Polycystic Ovary Syndrome
Pituitary adenomas are classified based on their morphological characteristics, hormonal activity, and prevalence. Based on size, they are classified as microadenomas (less than 1 cm) and macroadenomas (more than 1 cm). In women, non-functional pituitary adenomas (NFPA) often present with reproductive system pathologies. A significant proportion of women with NFPA (88%) have polycystic ovary syndrome (PCOS), and 23% develop secondary hypogonadism accompanied by amenorrhea. Women with pituitary microadenomas more often consult a gynecologist, as larger tumors tend to cause predominantly neurological and ophthalmological symptoms, while reproductive system problems become less pronounced [1]. Existing classifications of arterial hypertension (AH) do not fully cover such important aspects as tumor volume, metastasis, growth pattern, and hormonal activity. This creates significant obstacles to establishing a detailed clinical diagnosis, determining optimal surgical tactics, and effectively correcting hormonal imbalances [2]. According to the 2017 World Health Organization (WHO) updated classification of endocrine tumors [2,3], pituitary adenomas are now classified based on their hormonal profile and transcription factor expression. Importantly, a significant proportion of these tumors (22–54% in various studies) present not with excessive hormone secretion but with symptoms associated with mass effect. Such cases are diagnosed as clinically NFPA [4].
We used the degree of invasion as proposed Hardy’s classification for the growth of invasive pituitary tumors according to Knoss (Figures 1 & 2). Magnetic resonance imaging (MRI) is one of the most modern, safe (not using ionizing radiation), and informative imaging techniques used to diagnose a wide range of organs and systems in the human body. In the context of examining the pituitary gland, MRI is the method of choice, allowing for a detailed assessment of its morphological structure (including the anterior, posterior, and intermediate lobes), as well as the identification and characterization of space-occupying lesions (e.g., adenomas, cysts, craniopharyngiomas). The method is also effective for identifying and determining the duration of intrafocal hemorrhages, as well as for assessing the dynamics and effectiveness of therapy (both conservative and surgical). MRI allows for the precise localization of tumor processes in the sella turcica and an assessment of their relationships with adjacent brain structures, primarily the chiasmata and optic nerves. [5] Currently, there is no assessment method based on magnetic resonance imaging (MRI) data that would allow predicting the extent of resection of giant pituitary adenomas (GPAs). Therefore, the authors proposed a new grading scale for giant pituitary adenomas (AGPA) and assessed its prognostic value in relation to the extent of GAG resection [6]. The relationship between the resection extent and the AGPA score was assessed using linear regression. The AGPA score took into account tumor extension in different planes.
The maximum total score was 9. Results. The scoring system was applied to 45 patients with AGPA who underwent surgical resection. The mean resected tumor volume (%) was 82.0 ± 16.7, and the mean total AGPA score was 4.2 ± 0.8. Pairwise correlation between the resected tumor volume and the total AGPA score showed a strong inverse relationship (r = -0.633, p < 0.001). A significant difference was found between the calculated scores of 3 and 5, as well as 4 and 5 (p < 0.001). The authors concluded that AGPA is inversely proportional to the volume of tumor to be removed, which will help surgeons to predict the possible volume of tumor resection, as well as to predict the complexity of the operation and plan optimal preoperative counseling for the patient [6,7]. All of the above formed the basis for this study. The aim of the study is to study the radiological characteristics of patients with giant NFPA.
The study material is presented on the basis of the analysis of a pro- (151 patients) and retrospective (121 patients) study of the frequency of macro- and giant inactive pituitary adenomas for the period 2023-2024 based on the data of requests from three leading centers in Tashkent: the Republican Scientific and Practical Medical Center of Endocrinology of the Ministry of Health of the Republic of Uzbekistan named after Academician E.Kh. Turakulov, the Scientific Center of Neurosurgery of the Ministry of Health of the Republic of Uzbekistan and the Scientific Center of Emergency Medical Care of the Ministry of Health of the Republic of Uzbekistan, a total of 272 patients with macro- and giant NFPA s. The study prospectively enrolled 151 patients with macro- and giant NFPA s (men and women) treated at the Neuroendocrinology Department of the Russian Scientific and Practical Medical Center of Endocrinology, Ministry of Health of the Republic of Uzbekistan named after Academician Y.Kh. Turakulov during the specified periods. Of these, 85 (56.3%) were men and 66 (43.7%) were women; they were followed continuously. The average age was 48.12 years for men and 46.15 years for women. Disease duration ranged from 2 months to 5 years. The control group consisted of 20 healthy individuals of the same sex and age. According to the size of the pituitary adenoma, prospective patients (151 patients) were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant NAG - 96 people. Table 1 shows the distribution of patients by gender and age (data from a prospective study).
Inclusion Criteria: NFPA, women, men, macro and giant NFPA.
Exclusion Criteria: other types of pituitary adenomas, pituitary microadenomas, severe somatic diseases and endocrinopathies
The research methods included:
1) General clinical (examination of endocrine and neurological
status),
2) Instrumental (perimetry in all colors, fundus, visual acuity,
3) ECG, CT/MRI of the sella turcica and adrenal glands,
4) Ultrasound of internal and genital organs, etc.),
5) Hormonal blood tests (STH, IGF-1, LH, FSH, PRL, TSH, ACTH,
prolactin, testosterone, estradiol, progesterone, cortisol (Chemiluminescence
studies of blood serum were performed in the laboratory
of the RSNPCE). In addition, the postoperative material
was subjected to histological diagnostics at the RSNPCE of the
Ministry of Health of the Republic of Uzbekistan named after academician
E.Kh. Turakulov (histology room). We have carried out
an assessment of the GAG according to the AGPA [6]. under the
new points system proposed by Enam SA, Ghazi SM, Raghib MF
in 2022 Patients in our study received the following treatments:
transnasal pituitary adenomectomy (TPA) was performed in all
151 prospective and 121 retrospective patients. Additionally, 87
patients underwent radiation therapy to prevent tumor growth.
Furthermore, 10 patients with giant NFPA s received the somatostatin
analogue Sandostatin-Lar after TPA to prevent tumor recurrence.
The obtained data were processed using Microsoft Excel
and STATISTICA_6 computer programs. The arithmetic mean
(M) was calculated,standard deviation of the arithmetic meanor
the error of the arithmetic mean of all n repetitions (m). The significance
of differences in levels between groups was assessed
using the confidence interval and Student’s t-test (p). Differences
were considered statistically significant at p<0.05.
A total of 151 patients with macro- and giant pituitary adenomas were prospectively examined. Depending on the size of the pituitary adenoma, the prospective (151 patients) patients were divided into 2 groups: Group 1 - patients with macro- NFPA - 55 people, Group 2 - patients with giant pituitary adenomas - 96 people. In our study, we relied on the classification of Kurokawa Y., (1998), who considers tumors correspondingly larger to be giant.30 mmAnd40 mm. All MRI images were carefully reviewed. Cavernous sinus invasion was diagnosed by tumors occupying more than two-thirds of the internal carotid artery lumen or by tumors of grades 3-4 according to the classifications of Knosp et al. and Edal et al., respectively. Sphenoid sinus invasion was determined by the presence of sellar bone floor erosion and/or tumor extension into the sinus (grades 1-2 according to Edal et al.). Tumors with significant suprasellar extension (grade 4 according to Edal et al.), leading to obstructive hydrocephalus due to close contact with the third ventricle and proximity to brain tissue, were also classified as invasive. Table 2 shows the distribution of patients by the nature of the sellar region formation. As can be seen from Table 2, hemorrhage into the pituitary stroma occurred in 5 (9.09%)/12 (12.5%) cases, parasellar invasion – in 42 (76.4%)/78 (81.3%), suprasellar growth – in 45 (81.8%)/49 (51.0%), infrasellar expansion - 44 (80%)/57 (59.4%), expansion of the third ventricle - 32 (58.2%)/57 (59.4%) cases in groups 1 and 2, respectively.
Note: p – significance of differences between groups 1 and 2.
Tumor growth recurrence after TPA occurred in 15 out of 150 patients (10%). Invasion into the brain was noted in 10/25 cases (18.2%/26.0%). The maximum mean tumor diameter determined at diagnosis was 44.7 ± 13.6 mm, and macroadenomas > 40 mm were present in 68% of patients. A total of 76.4%/81.3% of all tumors had evidence of parasellar invasion (22% unilateral invasion, 62% bilateral invasion). Infrasellar invasion was observed in 80%/71.9% of all cases. Suprasellar extension of any grade was observed at a frequency of 62%/69.8% of the cohort. Of these, third ventricle and/or brain parenchymal tissue (grade 4, according to Edal et al. [ 182; c.1133– 1148]) were present in 58.2%/59.4% of all cases (Table 2). Our analysis of pituitary MRI data from both groups of patients with NAG revealed that patients in Group 1 had a predominantly suprasellar tumor growth pattern—25 cases (45.4%), while in Group 2, a total tumor growth pattern was observed—69 cases (71.8%). Furthermore, retrosellar tumor growth was also observed in Group 2—nine cases (9.4%). Furthermore, in 127 (84.1%) of 151 patients, tumor growth was endosuprasellar. We have carried out an assessment of the GAG according to the AGPA [6]. according to the new scoring system proposed by Enam SA, Ghazi SM, Raghib MF in 2022, based on preoperative MRI data (Table 3) in both patient groups. As can be seen from Table 3, there was a reliable difference between the groups in terms of scores according to the system ACU, which predicts the tumor size requiring resection.
Thus, this volume differed significantly in Group 2. Moreover, in group 1 The median preoperative tumor volume was 27 cm3 (IQR = 18.4, -35.6) and decreased to 3.5 cm3 (IQR = 1.2, -8.5) after removal. In group 2, the median preoperative tumor volume was 33 cm3 (IQR = 19.4, -38.8) and decreased to 3.6 cm3 (IQR = 1.4, -9.3) after removal. Next, we compared clinical symptoms depending on the nature of tumor growth in groups 1 and 2 of patients (Table 4). According to our data, in group 1 of patients, neuroendocrine and visual disturbances predominated in the total growth variant, while in the suprasellar and retrosellar growth their number was smaller (Table 4). As can be seen from Table 4, the comparative characteristics of patients showed thatPatients with giant pituitary adenomas exhibited pronounced neuroendocrine, neurological, and ophthalmological abnormalities. Neuroendocrine (GHR, panhypopituitarism, hypopituitarism, infertility, secondary amenorrhea) and ophthalmological (GD, amaurosis, etc.) abnormalities were characteristic of total tumor growth and suprasellar growth. Diencephalic-brainstem abnormalities (pyramidal symptoms, diffusely decreased reflexes and muscle tone) were observed in patients with total tumor growth, retrosellar growth, and invasion of the brain. Patients with giant pituitary adenomas primarily exhibited decreased levels of STH, FSH, LH, and ACTH (47%), i.e., panhypopituitarism accompanied by general cerebral and brainstem symptoms. Thus, according to our data, various variants of its total growth can serve as a neuroimaging marker of tumor aggressiveness, namely: supra-infra-laterosellar growth, supra-infrasellar tumor growth.
Table 4: Comparison of clinical symptoms depending on the nature of tumor growth in group 1 (n=55) and in group 2 (n=96) abs (%).
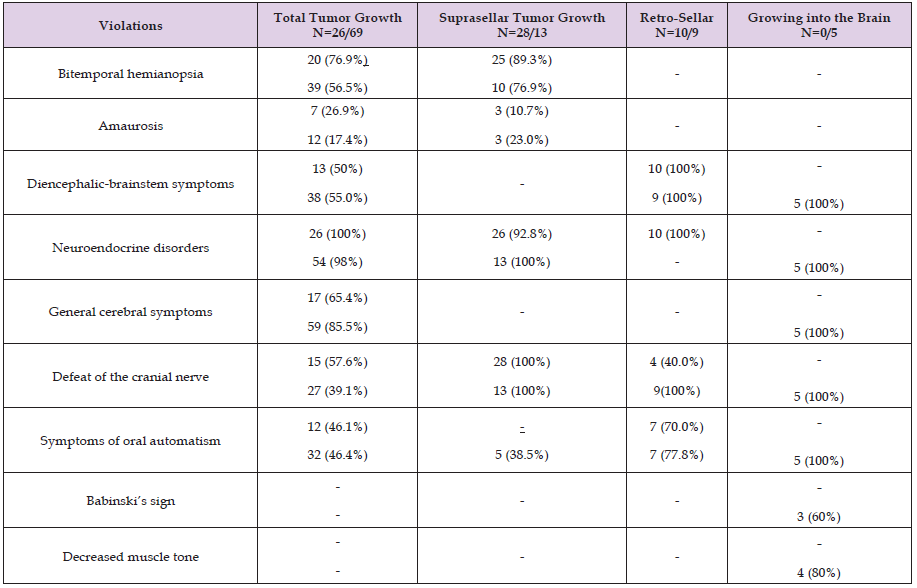
Note: CN – cranial nerves.
1) Patients with giant pituitary adenomas showed pronounced neuroendocrine, neurological and ophthalmological disorders. The most pronounced visual field disturbances in the form of bitemporal hemianopsia (45/49 cases) were observed in 127 patients with endosuprasellar tumor growth.
2) Based on our analysis of pituitary MRI data from both groups of patients with NAG, we found that in patients in Group 1, suprasellar tumor growth was predominant – 25 cases (45.4%), while in Group 2, total tumor growth was observed – 69 cases (71.8%). In Group 2, retrosellar tumor growth was also observed – 9 cases (9.4%). Furthermore, in 127 (84.1%) of 151 patients, tumor growth was endosuprasellar.

