Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Aline Vanessa Carrera-Vite1, Daniel Lopez-Hernandez2*, Leticia Brito-Aranda3, Liliana Grisel Liceaga-Perez1, Maria Clara Hernandez-Almazan4, Edgar Cruz-Aviles5, Maria Luisa Lucero Saldivar-Gonzalez6, Alberto Vazquez-Sanchez7, Xochitl Liliana Olivares-Lopez8 and Victor Hugo Noguez-Alvarez9
Received: February 07, 2026; Published: February 17, 2026
*Corresponding author: Daniel Lopez-Hernandez, Family Medicine Clinic Division del Norte, Institute of Social Security and Services for State Workers (ISSSTE), Mexico City, Mexico
DOI: 10.26717/BJSTR.2026.64.010095
Background: Primary care concentrates most prevention, diagnostic, and treatment needs across the life course, including non-communicable, communicable, oral, and preventive care conditions. Characterising the demographic and epidemiological profile of users is essential for planning integrated services in urban settings.
Methods: We conducted a population-based, cross-sectional analytical study using SIMEF records from an urban Family Medicine Clinic (ISSSTE) in the northern area of Mexico City. All outpatient consultations registered from January to December 2024 were included. Age- and sex-specific population structure and non-communicable diseases, communicable diseases, dental diseases, and preventive care conditions were analysed using descriptive and inferential statistics.
Results: A total of 11,149 subjects were included. The average age, in overall population, was 51.25 years old (SD=21.34), and the median age was 55 (Interquartile range=38-67). The population was predominantly female (61.8%) and showed a constrictive age structure, with the highest concentration between 50 and 69 years. The most prevalent non-communicable diseases were hypertension (25.5%), diabetes (20.6%), and dyslipidaemia (12.0%). Females presented higher prevalences of obesity (10.6% vs. 8.4%), hypothyroidism (9.3% vs. 2.6%), chronic venous insufficiency (6.5% vs. 4.3%), mixed anxiety–depressive disorder (6.6% vs. 3.2%), low back pain (4.7% vs. 3.4%), gastroenteritis, and colitis (4.4% vs. 3.8%), and gonarthrosis (4.0% vs. 2.3%). The most frequent communicable diseases were acute nasopharyngitis (15.2%), acute pharyngitis (8.1%), and urinary tract infection (4.7%), with significantly higher prevalences of nasopharyngitis and urinary tract infection among females. Dental caries was the most common oral condition (9.6%), followed by caries of dentine (2.7%), while chronic gingivitis was more frequent in males (2.5%). Among other conditions, administrative medical examinations predominated (24.0%), followed by general medical examinations (8.6%) and breast cancer screening (6.9%). Seasonal peaks of consultations were observed in mid and late year, mainly among women.
Conclusion: These findings support integrated, life-course, and sex-sensitive strategies for chronic disease control, infection prevention, oral health promotion, and preventive care delivery.
Keywords: Communicable Diseases; Morbidity; Non-Communicable Diseases; Primary Care
Abbreviations: WHO: World Health Organization; MADD: Mixed Anxiety and Depressive Disorder; GCUO: Gastroenteritis and Colitis of Unspecified Origin; UTI: Urinary Tract Infection; IQR: Interquartile Range; SD: Standard Deviation
Primary healthcare represents the cornerstone of health systems and constitutes the principal point of contact between populations and formal medical services (Bryant, et al. [1-5]). Likewise, the World Health Organization (WHO) has emphasised that effective primary healthcare can address up to 80% of essential health needs across the life course, particularly through prevention, early detection, and management of both communicable and non-communicable diseases (Allen, et al. [5-8]). Consequently, as demographic ageing accelerates and disease profiles evolve, primary care assumes an increasingly strategic role in responding to changing epidemiological demands. International evidence indicates that demand for primary care services is largely shaped by the morbidity profile of the populations served and is driven by a dual burden in which non-communicable chronic disease and communicable diseases coexist (Bigio, et al. [9,10]). Outpatient consultations are predominantly attributable to cardiometabolic disorders, respiratory and gastrointestinal infections, and urinary tract infections, reflecting the epidemiological transition observed in diverse populations (Global Burden of Disease [11-15]). This distribution is closely associated with demographic change characterised by declining fertility and increasing life expectancy, which expands the proportion of individuals requiring long-term management of non-communicable diseases while maintaining exposure to common infectious conditions.
In the Region of the Americas, this pattern is further differentiated by age and sex, as non-communicable diseases—particularly cardiovascular diseases and diabetes—account for most primary care visits among adults and older adults, whereas communicable diseases remain frequent causes of consultation among children and women (Stephenson, et al. [12,16-18]). Comparable utilisation profiles have been documented in the United States and Canada, where primary care services are largely devoted to the management of chronic metabolic and musculoskeletal disorders alongside common infections, with pronounced variation according to age and sex (Stephenson, et al. [12,19,20]). Collectively, these international findings are consistent with global health surveys demonstrating that population ageing and the rising prevalence of chronic disease are major drivers of increasing demand for primary healthcare services (Sun, et al. [21-23]). Similarly, in Mexico, National health surveys report high utilisation of primary care services, driven mainly by cardiometabolic diseases and their complications (Lazcano, et al. [24-26]). Alongside the predominance of non-communicable diseases, communicable diseases remain among the leading causes of outpatient consultations, highlighting the persistence of a mixed disease profile (Gamboa, et al. [27-31]).
In this context, a detailed characterisation of the sociodemographic and epidemiological profile of individuals attending primary care services is essential for identifying prevailing health needs, understanding patterns of service utilisation, and detecting disparities by age and sex. Such analyses are fundamental for informing health system planning in settings experiencing rapid demographic ageing and epidemiological change. Accordingly, the present study aimed to characterise the sociodemographic profile of a population attending a primary care unit and to analyse the distribution of communicable and non-communicable diseases, dental morbidity, and the utilisation of screening services among individuals receiving care at the first level of healthcare in the northern area of Mexico City.
Study Design and Data Collection A population-based, cross-sectional, and analytical investigation was designed. The data included patients from the northern area of Mexico City who attended outpatient consultations at the Family Medicine Clinic Guerrero, belonging to the Institute of Social Security and Services for State Workers (ISSSTE; Instituto de Seguridad y Servicios Sociales de los Trabajadores del Estado, by its acronym in Spanish), Mexico City, Mexico. The dataset was extracted from the Medical Financial Information System (SIMEF), which systematically records outpatient consultations provided by healthcare personnel. We included medical records from January to December 2024. The complete database is consisting of 65,644 records corresponding to 11,437 persons from all age groups. The study was conducted between 1 December 2025 and 15 January 2026.
Patient Selection and Study Population
The Data Collection Procedure Included the Following Steps:
1) The information was extracted and downloaded per month (from January to December), using Excel files generated by the “SIMEF” as work tools.
2) A single database was then generated and all individual patient records were cross-referenced to ensure their accuracy.
3) A final review of the new combined database was performed to ensure the integrity and consistency of the information.
4) The single database was analyzed to select records that met the inclusion criteria.
5) Records that did not meet the inclusion criteria were excluded. 6) The cleaned and validated dataset was stored in an Excel workbook, which served as the statistical dataset for subsequent epidemiological analyses.
Inclusion Criteria:
1) Individuals with at least one consultation registered in the SIMEF system during the study period.
2) Complete clinical records, including identification variables (name, file number, sex, beneficiary type), International Classification of Diseases 10th revision (ICD-10) diagnosis code(s), and consultation dates.
Exclusion Criteria:
1) Records that were incomplete, inconsistent, or lacked essential identification or diagnostic information in the SIMEF system. 2) Duplicate records identified during data cleaning.
Finally, a census sampling method was employed, with all eligible records from the newly generated dataset. All this ensured that only patients with complete and consistent records were included in the study.
Variables and Statistical Analysis
The variables analysed comprised age (in years), sex (male and female), number of outpatient consultations, and comorbidities coded according to the ICD-10. In total, 2,719 ICD-10 codes were registered. New variables were generated to identify obesity, dyslipidaemia, diabetes, and age groups. For obesity, the following ICD-10 codes were included: E66.0 –Obesity due to excess calories; E66.1 –Drug-induced obesity; E66.2 –Extreme obesity with alveolar hypoventilation; E66.8 –Other obesity; and E66.9 –Obesity, unspecified. For dyslipidaemia, the selected codes were: E78.0 –Pure hypercholesterolaemia; E78.1 – Pure hyperglyceridaemia; E78.2 –Mixed hyperlipidaemia; E78.3 –Hyperchylomicronaemia; E78.4 –Other hyperlipidaemia; E78.5 –Hyperlipidaemia, unspecified; E78.6 –Lipoprotein deficiency; E78.8 –Other disorders of lipoprotein metabolism; and E78.9 –Disorder of lipoprotein metabolism, unspecified. Diabetes was identified using the following ICD-10 codes: E10.0–E10.9 –Type 1 diabetes mellitus, E11.0– E11.9 –Type 2 diabetes mellitus, E12.2-E12.9 –Malnutrition-related diabetes mellitus, E13.0-E13.9 –Other specified diabetes mellitus, and E14.0-E14.9 –Unspecified diabetes mellitus, encompassing type 1 and type 2 diabetes mellitus and their related complications. Age was categorised using a hierarchical epidemiological approach. The study population was first divided into four main age groups: children (0–9 years old), adolescent population (10–19 years old), mature population (20–59 years old) and elderly population (≥60 years old). Children were further classified into neonates and infants (0 years old), early childhood (1–4 years old), and childhood (5–9 years old).
The adolescent population was subdivided into early adolescence (10–14 years old) and late adolescence (15–19 years old). The mature population was stratified into early adulthood (20–39 years old) and midlife (40–59 years old). Finally, the elderly population was disaggregated into sexagenarians (60–69 years old), septuagenarians (70–79 years old), octogenarians (80–89 years old), nonagenarians (90–99 years old), and centenarians (≥100 years old) (Lopez, et al. [32]). Categorical variables are presented as absolute frequencies and percentages, while quantitative variables are described using mean, standard deviation (SD), range, maximum value, minimum value, median, and interquartile range (IQR). A 95% confidence interval (95% CI) was reported where applicable. Comparisons of categorical variables were performed using the likelihood ratio and the Yates’ continuity correction chi-square (χ²) (LRχ² and Yχ², respectively), as appropriate. Quantitative variables were compared using U Mann-Whitney test, and Median Test between independent groups. The age distribution was analysed by the Kolmogorov–Smirnov test with Lilliefors correction. A two-tailed p-value of < 0.05 was considered statistically significant.
Ethical Considerations
The present study was conducted in compliance with the Good Clinical Practice Guidelines, national regulations, and the principles outlined in the Declaration of Helsinki for research involving human subjects. The Data was treated confidentially. To guarantee confidentiality, only the principal investigators had access to the complete dataset, including identifiable patient information (e.g., names). The patient names were replaced with unique identification numbers. The assigned number allows the data to be linked to a specific individual without revealing the individual’s identity. This approach ensured that all patient data were handled under ethical standards and maintained the highest level of confidentiality throughout the study. This anonymization was conducted before sharing the dataset for statistical analysis with some researchers. After the statistical analysis, only the processed statistical data was made available to the rest of the research team.
Characteristics of the Study Population
After excluding records corresponding to consultations not provided (n=100), the analytical dataset comprised 65,544 records representing 11,437 individuals across all age groups. Following the removal of records with inconsistencies in the sex and age variables, the final study population was defined. Finally, a total of 11,149 subjects were included. Of the total population, females constituted the main group with the highest healthcare utilisation, comprising 6,894 participants (61.8%; 95% CI: 60.8–62.8), compared with 4,255 males (38.2%; 95% CI: 37.2–39.2). To further characterise the demographic structure of the study population, a population pyramid analysis was performed to depict the age- and sex-specific distribution. This graphical representation facilitates the interpretation of population dynamics and their relationship with morbidity patterns, healthcare utilization, and age-related differences in health risk profiles. In our study population, the population pyramid reveals a clear predominance of adults and older adults, with the highest concentration observed between 50 and 69 years of age, reflecting an ageing population structure. Across nearly all age groups from mid-adulthood onwards, females outnumber males, a difference that becomes more pronounced in individuals aged 70 years and older. This sex imbalance in older age groups is indicative of higher female survival and life expectancy, a well-documented demographic phenomenon with important implications for healthcare planning, particularly in geriatric and long-term care services.
Moreover, the highest concentration of females is observed in the 60–64 years age group. In contrast, among males, the largest number of individuals is concentrated in the 65–69 years age group. This sex-specific shift in peak age distribution suggests differential survival patterns and healthcare utilization trajectories between men and women, which may have implications for the timing and type of preventive, chronic disease management, and geriatric care services required in primary healthcare settings. In contrast, children, adolescents, and young adults represent a smaller proportion of the population, resulting in a narrow base of the pyramid. This reduced representation of younger cohorts suggests lower fertility rates and demographic ageing, which may influence future population replacement dynamics and the demand for maternal, paediatric, and adolescent health services. Overall, the age- and sex-specific distribution corresponds to a constrictive (regressive) population pyramid, characterized by a narrow base and a relative expansion of middle-aged and older adult groups (Figure 1). This demographic structure reflects a population in an advanced stage of the demographic transition, with a growing burden of chronic diseases and an increasing need for integrated, age-sensitive primary healthcare strategies. The average age, in overall population, was 51.25 (Figure 2) years old (SD=21.34, range=119, minimum age=0, maximum age=119 years old, median age=55 [IQR=38-67]). The age distribution is non-normal and exhibits a bimodal pattern, with a dominant peak in middle-to-older adulthood and a secondary peak in younger ages (Figure 2).
This structure suggests the presence of distinct age-related subpopulations, likely reflecting differential healthcare utilisation patterns across the life course. This age distribution was demonstrated by the Kolmogorov–Smirnov test with Lilliefors correction (D = 0.076, p < 0.001). In addition, females exhibited a significantly higher average age (52.08 ± 20.34 years) compared with males (49.90 ± 22.82 years). However, the median age was similar in males (55 years old; IQR= 35-68) compared to female (55 years old; IQR=40-67; p= 0.937, Median Test between independent groups). The convergence of statistical testing and graphical analysis reinforces the interpretation of an ageing study population with heterogeneous age-related healthcare needs. Table 1 presents age- and sex-distribution of the study population, providing an overview of the demographic structure of the population. Most participants were concentrated in the midlife population, followed by individuals in sexagenarian, whereas young adults and children constituted a smaller segment of the study population. A higher proportion of females was observed among the EA and ML population, while males predominated in nearly all age groups. Sex-specific proportions were similar in EP. This pattern underscores the importance of integrating sex- and age-specific approaches in preventive and healthcare strategies for the management of communicable and non-communicable diseases. In 2024, a total of 66,544 outpatient consultations were recorded.
Source: Prepared by the authors using the results from the SIMEF database, January-December, 2024. EA: early adulthood (20-39 years old). ML: midlife (40-59 years old). EP: elderly population (60 years old and over). N&I: neonates and infants; EC: early childhood; AP: adolescent population; EA: early adolescence; LA: late adolescence; MP: mature population. Comparisons among age group (Children, AP, MP, and EP) and sex was performed using the Likelihood Ratio chi-square (LRχ²=136.062, df=3, p<0.001). Comparisons among age group (N&I, EC, Chilhood, EA, LA, EA, ML, sexagenarians, septuagenarians, octogenarians, nonagenarians, and centenarians) and sex was performed using the Likelihood Ratio chi-square (LRχ²=142.098, df=11, p<0.001).
Females accounted for many consultations throughout the year, with 44,701 visits (67.2%), while 21,843 consultations (32.8%) corresponded to males (Figure 3). Overall, the temporal distribution of consultations reveals a stable pattern of higher service use among women, alongside seasonal fluctuations in total demand. Monthly outpatient consultation counts showed moderate variation over the year. The highest number of consultations was observed in October (6,528), followed by August (6,015) and May (5,770). The lowest monthly totals were recorded in March (4,754) and December (4,812). Across all months, consultation counts were consistently higher among women. Both females and males reached their highest outpatient consultation volumes in October, with higher counts observed among females (4,291) compared with males (2,237). The female-to-male consultation ratio remained stable across the year, averaging approximately 2:1, indicating a sustained sex-based difference in service utilisation. Table 2 presents the epidemiological profile of the ten most prevalent non-communicable diseases of the total study population, followed by a sex-based comparative analysis. In the overall population, hypertension was the most prevalent condition, followed by diabetes and dyslipidaemia. Obesity, hypothyroidism, chronic venous insufficiency, and mixed anxiety and depressive disorder (MADD) occupied intermediate positions in the prevalence ranking, whereas, low back pain, gastroenteritis, and colitis of unspecified origin, and gonarthrosis were less frequent.
Table 2: Overall epidemiological distribution and sex-based comparison of the ten most frequent non-communicable diseases in the study population.
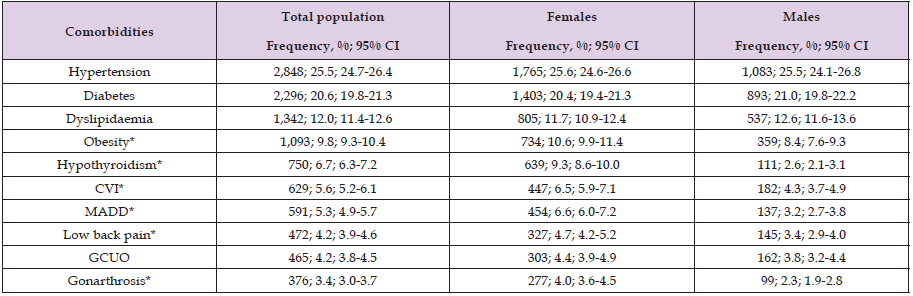
Source: Prepared by the authors using the results from the SIMEF database, January-December, 2022. CVI: chronic venous insufficiency. MADD: mixed anxiety and depressive disorder. GCUO: gastroenteritis and colitis of unspecified origin. Comparisons between sex were performed using the Yates’ continuity correction chi-square (Yχ²); degree freedom (df). *P values statistically significative. Hypertension (Yχ²=0.024, df=1, p=0.878); diabetes (Yχ²=0.613, df=1, p=0.434); dyslipidaemia (Yχ²=2.124, df=1, p=0.145); *Obesity (Yχ²=14.281, df=1, p<0.001); *hypothyroidism (Yχ²=184.949, df=1, p<0.001); *CVI (Yχ²=23.652, df=1, p<0.001); *MADD (Yχ²=58.704, df=1, p<0.001); *low back pain (Yχ²=11.247, df=1, p=0.001); GCUO (Yχ²=2.130, df=1, p=0.144); *gonarthrosis (Yχ²=22.580, df=1, p<0.001).
When stratified by sex, females exhibited a significantly higher prevalence of obesity, hypothyroidism, chronic venous insufficiency, MADD, low back pain, and gonarthrosis compared with males. Conversely, none of the evaluated conditions were significantly more prevalent in males compared with females. Finally, similar prevalences were observed for hypertension, diabetes, dyslipidaemia, and gastroenteritis and colitis of unspecified origin (GCUO), indicating a comparable burden of these conditions between sexes in our study population. Table 3 presents the overall epidemiological distribution of the five communicable diseases with the highest prevalence in the study population, followed by a sex-based comparative analysis. In the total population, acute nasopharyngitis showed the highest prevalence, followed by acute pharyngitis, and urinary tract infection (UTI). Acute upper respiratory infection (unspecified), and unspecified infectious gastroenteritis and colitis showed lower prevalence. When stratified by sex, acute nasopharyngitis and UTI had a significantly higher prevalence among females than males. In contrast, no statistically significant sex-based differences were observed for unspecified infectious gastroenteritis and colitis, AURI, and acute nasopharyngitis. Table 4 shows the distribution of the five most frequent dental conditions in the study population, stratified by sex. Overall, dental caries was the leading oral health problem, with a similar prevalence in females and males.
Table 3: Overall epidemiological distribution and sex-based comparison of the five most frequent communicable diseases in the study population.
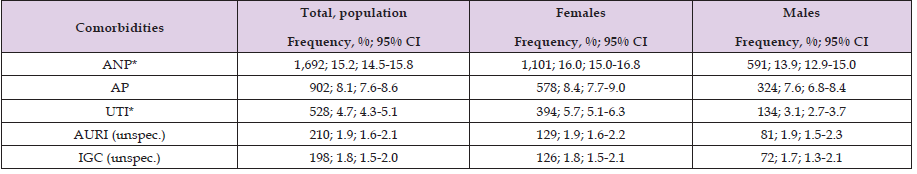
Source: Prepared by the authors using the results from the SIMEF database, January-December, 2022. ANP: acute nasopharyngitis [common cold]; AP: acute pharyngitis; UTI: urinary tract infection; AURI (unspec.): acute upper respiratory infection, unspecified; IGC (unspec.): other and unspecified gastroenteritis and colitis of infectious origin. Comparisons between sex were performed using the Yates’ continuity correction chi-square (Yχ²); degree freedom (df). *P values statistically significative. *ANP (Yχ²=8.689, df=1, p=0.003); AP (Yχ²=1.993, df=1, p=0.158); *UTI (Yχ²=37.829, df=1, p<0.001); AURI (unspec.) (Yχ²=0.003, df=1, p=0.960); and IGC (unspec.) (Yχ²=0.205, df=1, p=0.651).
Table 4: Overall epidemiological distribution and sex-based comparison of the five most frequent communicable diseases in the study population.
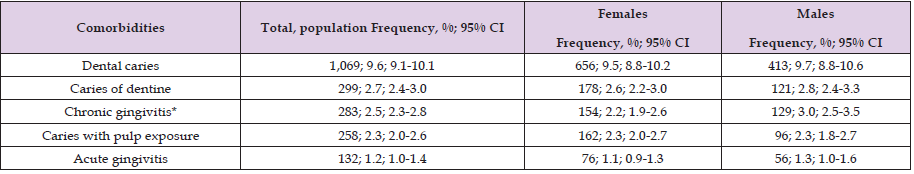
Source: Prepared by the authors using the results from the SIMEF database, January-December, 2022. Comparisons between sex were performed using the Yates’ continuity correction chi-square (Yχ²); degree freedom (df). *P values statistically significative. Dental caries (Yχ²=0.089, df=1, p=0.765); caries of dentine (Yχ²=0.594, df=1, p=0.441); *Chronic gingivitis (Yχ²=6.452, df=1, p=0.011); caries with pulp exposure (unspec.) (Yχ²=0.065, df=1, p=0.799); and acute gingivitis (Yχ²=0.852, df=1, p=0.356).
This finding confirms dental caries as the predominant preventable oral disease and a major cause of demand for dental care services. Caries of dentine ranked second in frequency, showing comparable proportions between females and males. Likewise, caries with pulp exposure accounted for fourth place, with no statistically significant differences by sex, reflecting a similar burden of advanced carious lesions in both groups. Periodontal conditions were also prominent in the morbidity profile. Chronic gingivitis affected at least 2% of the total population, with a significantly higher prevalence in males compared with females. This sex-based difference suggests disparities in oral hygiene practices and preventive care utilization, with important implications for targeted public health interventions. Acute gingivitis showed no significant variation between females and males. The presence of both acute and chronic inflammatory periodontal conditions highlights the persistence of preventable oral diseases within the study population. These dates reflect a dual burden of chronic and progressive oral pathologies that are largely preventable through primary care strategies, including health education, fluoride use, and early detection. The lack of significant sex differences in most conditions, except for chronic gingivitis, indicates a broadly similar epidemiological pattern between women and men, while underscoring underscoring the need for sex-sensitive approaches in periodontal disease prevention.
Table 5 presents the distribution and sex-based comparison of the ten most frequent health conditions related to examinations and preventive care in the study population. Overall, administrative medical examinations were the most common reason for consultation. This category showed a significantly higher proportion among females than males, indicating greater utilisation of administrative health services by this group. General medical examinations ranked second, with comparable proportions between females and males, suggesting a similar demand for routine medical assessments across sexes. Preventive breast cancer screening exhibited marked sex differences, as expected, reflecting the sex-specific nature of this preventive service. Unspecified special examinations represented no significant difference between females and males. Dental examinations were proportionally and significantly more frequent among males compared with females, suggesting sex-based differences in patterns of preventive oral healthcare utilisation. Observation for suspected disease or condition showed similar proportions in females and males. Contraceptive management represented no statistically significant difference by sex. Additionally, post-surgical convalescence also without significant sex-based variation. The predominance of administrative and general medical examinations underscores the central role of primary care services in facilitating access to employment, education, and institutional requirements.
Table 5: Epidemiological distribution and sex-based comparison of the ten most frequent health conditions related to examinations and preventive care in the study population.
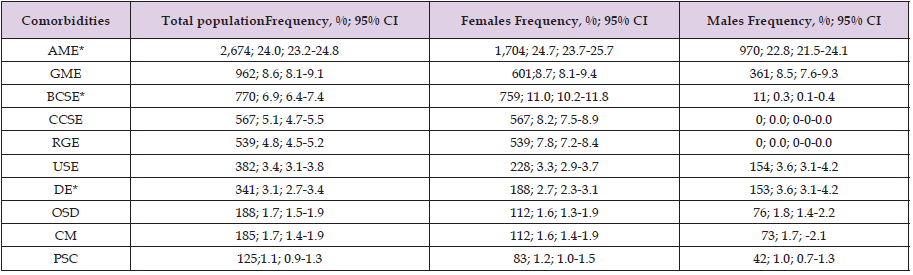
Source: Prepared by the authors using the results from the SIMEF database, January-December, 2022. AME: administrative medical examination; GME: general medical examination; BCSE: breast cancer screening examination; CCSE: cervical cancer screening examination; RGE: routine gynaecological examination; USE: unspecified special examination; DE: dental examination; OSD: observation for suspected disease or condition; CM: contraceptive management; PSC: post-surgical convalescence. Comparisons between sex were performed using the Yates’ continuity correction chi-square (Yχ²); degree freedom (df). *P values statistically significative. *AME (Yχ²=5.218, df=1, p=0.022); GME (Yχ²=0.154, df=1, p=0.695); *BCSE (Yχ²=471.331, df=1, p<0.001); CCSE Not applicate; RGE Not applicate; USE (Yχ²=0.683, df=1, p=0.409); *DE (Yχ²=6.408, df=1, p=0.011); OSD (Yχ²=0.322, df=1, p=0.570); CM (Yχ²=0.084, df=1, p=0.772); PSC (Yχ²=0.929, df=1, p=0.335).
The high frequency of cancer screening and gynaecological care among women highlights the integration of preventive services within routine healthcare utilisation, while the lower proportion of male participation in preventive consultations suggests persistent gaps in preventive health-seeking behaviour. Overall, the epidemiological pattern observed in Chapter Z conditions reflects a strong demand for preventive and regulatory healthcare services, reinforcing the importance of primary care as a gateway for both disease prevention and health system navigation.
The age structure identified in the present study provides strong evidence of an ongoing demographic and epidemiological transition towards an ageing population. Rather than exhibiting an expansive pattern dominated by younger cohorts, the population pyramid shows a progressive concentration of individuals in middle and older age groups, a hallmark of societies that have moved beyond the early stages of demographic transition (Bongaarts, et al. [33,34]). This age pattern shares several demographic characteristics with those reported in previous analyses conducted in similar settings (Lopez, et al. [28,33-35]), and is consistent with the worldwide demographic shift towards lower fertility and increased survival, which has progressively transformed population pyramids from expansive to more stationary or rectangular shapes (Bongaarts [33]). Globally, the expansion of cohorts aged ≥40 years, especially those between 50 and 69 years old and aged ≥70 years, has been associated with rising healthcare demand and a greater burden of chronic diseases (Hong, et al. [23,24,36-38]). Our findings align with this general trend, suggesting that the demographic structure observed is part of a broader epidemiological phenomenon. Nevertheless, when contrasted our data with specific world regions, we found clear differences persist.
The age structure of our study population differs from that reported for Africa (Pezzulo, et al. [39]), Europe (Eurostat, [40]), North America and Oceania (Uhlenberg, 2009; Institute of Medicine (US), 2012; Bonnet et al., 2021; Newmyer et al., 2022). Unlike African countries, where expansive pyramids predominate and are associated with a higher burden of communicable diseases and maternal and child health conditions (Pezzulo, et al. [39]), our data do not show a youthful population profile. It also contrasts with the constrictive pyramids observed in Europe (Eurostat [40]) and with the increasingly rectangular pyramids described for North America and Oceania, characterised by a greater proportion of older age groups (Uhlenberg, 2009; Institute of Medicine (US), 2012; Bonnet et al., 2021; Newmyer et al., 2022). In contrast, the structure identified in this study is comparable to that described for Latin America, which represent transitional demographic settings (Department of Economic and Social Affairs [41- 43]). This suggests that although the oldest-old segment has not yet reached the proportions seen in high-income regions, ageing-related healthcare needs are already prominent within the study population (Jin, et al. 2025). Moreover, important distinctions emerge that reflect both temporal change and contextual differences in healthcare utilisation. Compared with the national population structure, the age distribution of the study population is shifted towards older age groups, with an overrepresentation of adults aged ≥30 years and a marked concentration between 40 and 69 years.
This deviation from the general population pyramid indicates a selective utilisation of health services by middle-aged and older adults, consistent with an epidemiological profile dominated by chronic non-communicable diseases and long-term care needs. Consequently, the observed structure reflects not only a demographic transition but also an epidemiological transition, in which morbidity patterns are increasingly determined by ageing-related conditions rather than by childhood or infectious diseases. This discrepancy between national and clinical pyramids is epidemiologically expected. While national demographic data reflect the composition of the entire population, clinical samples—especially those derived from primary care services—are shaped by patterns of healthcare utilisation (Melgarejo, et al. [44]). Adults and older adults are more likely to seek medical attention due to the accumulation of chronic conditions, functional limitations, and long-term exposure to behavioural and environmental risk factors. Younger individuals, although numerically substantial in the general population, tend to contribute less to outpatient consultation demand. On the other hand, the similarity between the population pyramid observed in this study and that reported in previous investigations conducted in urban primary care settings in the south and west of Mexico City (Lopez, et al. [28,44]) supports the external validity of our findings.
However, subtle shifts in age distribution suggest that demographic ageing within service-utilising populations may be progressing over time. Specifically, our findings (northern area) and some studies conducted in different regions of Mexico City (southern, and western areas) display a highly comparable demographic structure. In all cases, the pyramids are characterised by a relatively narrow base in younger age groups, a progressive widening across adult ages (approximately 30–64 years), and a marked predominance of females in the oldest age groups. This overall configuration is typical of primary care populations in large urban settings undergoing an advanced stage of demographic transition, where declining fertility and increasing life expectancy shape service utilisation profiles. Despite these broad similarities, subtle differences are evident between regions. The study conducted in the southern area of Mexico City shows a slightly higher relative concentration in middle adult age groups, particularly between 45 and 64 years (Lopez-Hernandez, et al. [28]). In contrast, the population from the western area shows a modest shift towards late middle-aged and early older adult groups, with a greater representation of individuals aged 50–69 years (Melgarejo-Estefan, et al. [44]). In our study, corresponding to the northern area of the city, the distribution appears marginally more concentrated in the 55–69- year age range, suggesting a somewhat more pronounced ageing profile of service users in this region.
Sex-specific patterns vary by region. While the western (Melgarejo- Estefan, et al. [44]) and northern populations show a clear female predominance from the seventh decade of life onwards, the southern population (Lopez-Hernandez, et al. [28]) exhibits a relative male predominance among individuals aged 70 years and above. Overall, taken together, these findings indicate that although the three populations belong to distinct geographical areas of Mexico City — south, west, and north — they share a common demographic profile, reflecting similar urban and healthcare access dynamics. The observed differences are quantitative rather than structural and are likely attributable to local demographic composition and regionalised patterns of healthcare utilisation, rather than to fundamental demographic divergence. These subtle regional variations reinforce the importance of considering population regionalisation when interpreting service- based demographic structures, even within the same metropolitan area. Additionally, this reinforces the interpretation that the morbidity patterns identified in the present study are shaped by evolving demographic realities rather than by methodological artefacts. Across the three studies, cardiometabolic disorders—particularly hypertension and diabetes—constitute the largest proportion of diagnoses (Lopez, et al. [28,44]), consistent with both the age distribution of the study populations and the pattern of health service utilisation. This pattern is consistent with national and regional evidence indicating a high burden of metabolic and cardiovascular disease in adult populations in Mexico and Latin America (Basto-Abreu, et al. [45,46]).
However, the third most prevalent non-communicable condition differs by region: dyslipidaemia ranks third in the western (Melgarejo- Estefan, et al. [44]) and northern populations. Notably, COPD, occupies third position in the southern population (Lopez-Hernandez, et al. [28]). In addition, intestinal malabsorption and dorsalgia are reported among the ten leading morbidities exclusively in the western population (Melgarejo-Estefan, et al. [44]), while unspecified colitis and gastroenteritis are observed within the ten main diagnostic categories only in the present study. Likewise, communicable diseases remain an important component of outpatient morbidity but account for a smaller share of consultations across all three settings. In all studies, acute respiratory infections, urinary tract infections, and gastrointestinal infections are the most frequent diagnoses (Lopez- Hernandez, et al. [28,44]), mirroring patterns reported in both international and Mexican primary care settings (Lopez-Hernandez, et al. [28, 44]). But, in the western population (Melgarejo-Estefan, et al. [44]), conjunctivitis was reported among the five most prevalent infectious conditions, a finding that was not observed in either the southern population or in the present study. Overall, the three studies demonstrate that communicable diseases persist as a secondary but clinically relevant component.
These findings are in line with previously published evidence from urban primary care in Mexico City (Basto-Abreu, et al. [45-47]) and from comparable primary care settings internationally (Lopez-Jaramillo, et al. [48-50]), supporting the interpretation that the morbidity patterns identified in the northern population reflect established demographic and epidemiological dynamics [51]. Beyond this epidemiological pattern, our data reveal a substantial contribution of other conditions to outpatient service demand, highlighting the multifactorial nature in primary care populations. At the same time, oral health conditions, particularly dental caries and gingival diseases, account for a relevant proportion of consultations, underscoring the persistent burden of preventable dental pathology within routine care. In addition, a considerable share of encounters corresponds to health examinations and preventive or administrative care, including general medical examinations, cancer screening procedures, and dental check-ups, reflecting the dual role of primary care services in both disease management and preventive health delivery. Taken together, these findings indicate that the pattern of observed in this study should be interpreted as the expected outcome of the underlying demographic structure of the population served, reflecting the interaction between age distribution, cumulative exposure to risk factors, and patterns of healthcare utilisation. This epidemiological and demographic pattern of healthcare service utilisation by sex- and age-group provides a robust basis for public policy design, resource allocation, and evidence-based planning of health system goals in primary care level.
A key strength of this study is the large sample size and the stratification by age and sex, which enable a robust description of demographic and morbidity patterns at the population level. Cross-sectional data are useful for estimating disease burden and identifying variation across subgroups, and the results contribute evidence relevant to the planning of sex-specific and age-oriented health interventions. On the other hand, several limitations should be considered. The cross-sectional design may result in misclassification of conditions, particularly those based on clinical diagnosis, and the high proportion of older adults may reduce the applicability of the findings to younger populations. Moreover, the morbidity profile observed highlights the need to strengthen preventive actions, including vaccination, infection surveillance, and early treatment, especially among older adults and individuals with multiple comorbidities. These findings support the prioritisation of preventive services and the allocation of healthcare resources toward groups with the greatest cardiometabolic and infectious burden.
Overall, the results show distinct epidemiological profiles across non-communicable diseases, communicable diseases, dental conditions, and preventive care services. Cardiometabolic disorders, particularly hypertension, diabetes and dyslipidaemia, constitute the main burden of morbidity, with similar prevalence in women and men, while obesity, hypothyroidism, chronic venous insufficiency, mixed anxiety and depressive disorder, low back pain and gonarthrosis were significantly more frequent among females. These patterns indicate a differentiated distribution of chronic conditions by sex rather than a uniform multimorbidity profile. Communicable diseases were dominated by acute respiratory infections and urinary tract infections, with higher prevalence among females for acute nasopharyngitis and UTI, whereas other infections showed no relevant sexbased differences. This reflects a morbidity pattern characterised by common community-acquired infections with limited sex divergence, except for conditions related to anatomical and care-seeking differences. Oral health conditions displayed a dual profile: dental caries affected both sexes similarly, while chronic gingivitis was significantly more frequent among males, suggesting sex-related disparities in periodontal health and preventive practices. Taken together, these findings demonstrate that the epidemiological profiles of this population are heterogeneous and strongly influenced by sex and type of condition. This supports the need for differentiated, age- and sex-sensitive strategies that integrate cardiometabolic risk control, infection prevention, oral health promotion, and equitable access to preventive services, in order to improve health outcomes and optimise healthcare utilisation in the adult population.
The authors would like to thank Professor Susana Ortiz Vela, Master in translation, and also express their gratitude to the Centro de Investigación y de Educación Continua S.C. for their support in translation.
Authors have declared that no competing interests exist.
All authors contributed to conceptualization (ideas, formulation, or development of research goals and objectives), formal analysis (application of statistical, mathematical, computational, or other formal techniques to analyse or synthesize study data), writing - original draft (preparation, creation, and/or presentation of the published work, specifically writing the initial draft), writing - review and editing (preparation, creation, and/or presentation of the published work by the research group, specifically critical review, commentary, or revisions, including pre- or post-publication stages), and visualization (preparation, creation, and/or presentation of the published work, specifically data visualization/presentation). Aline Vanessa Carrera-Vite, Liliana Grisel Liceaga-Perez, and López Hernández Daniel, in addition to the above, contributed to project administration (responsibility for managing and coordinating the planning and execution of the research activity), investigation (development of a research process, specifically experiments or data collection/testing), methodology (development or design of methodology, creation of models), supervision (responsibility for supervision and leadership in the planning and execution of the research activity, including external mentoring), and validation (verification, whether as part of the activity or separately, of the overall replicability/reproducibility of the results/experiments and other research outcomes).
Authors hereby declare that NO generative AI technologies such as Large Language Models (ChatGPT, COPILOT, etc.) and text-to-image generators have been used during writing or editing of manuscripts.
The study was conducted using medical records, and no informed consent was obtained. The handling of the information was approved by the ethics committee, ensuring compliance with the appropriate ethical standards.
The present study was conducted in compliance with the Good Clinical Practice Guidelines, national regulations, and the principles outlined in the Declaration of Helsinki for research involving human subjects. To guarantee confidentiality, only the principal investigators had access to the complete dataset, including identifiable patient information (e.g., names). The patient names were replaced with unique identification numbers. The assigned number allows the data to be linked to a specific individual without revealing the individual’s identity. This approach ensured that all patient data were handled under ethical standards and maintained the highest level of confidentiality throughout the study. This anonymization was conducted before sharing the dataset for statistical analysis with some researchers. After the statistical analysis, only the processed statistical data were made available to the rest of the research team.

