Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Zhalieva G.K2, Matkerimov A.T1, Subanova G.A4, Askerov A.A2*and Aaliev T.B3
Received: January 31, 2026; Published: February 11, 2026
*Corresponding author: Askerov A.A, Professor of the Department of Obstetrics and Pediatrics of Jalal-Abad State University, Kyrgyzstan
DOI: 10.26717/BJSTR.2026.64.010085
This study presents an analysis of markers for predicting preeclampsia among pregnant women in southern Kyrgyzstan. Preeclampsia predictors included burdened anamnesis of preeclampsia, systolic and diastolic blood pressure monitoring, biomarkers PlGF, sFlt-1, and the PlGF/sFlt-1 ratio.
Keywords: Preeclampsia; Major Obstetric Syndrome; Placental Invasion; Risk Factors; Biomarkers sFlt-1 and PlGF
According to the WHO, hypertension during pregnancy accounts for 9 to 25% of all maternal mortality, although precise data are difficult to determine [1,2]. Preeclampsia, while one of the clinical conditions of the “Major Obstetric Syndromes” and a leading cause of maternal and perinatal mortality, and its complications, pose a range of medical problems [3,4]. Risk factors for preeclampsia include: first pregnancy, multiple pregnancies, age (under 18 or over 35/40 years), obesity, diabetes, chronic hypertension, kidney disease, autoimmune diseases, thrombophilia, a family history of preeclampsia, and preeclampsia in a previous pregnancy. These conditions increase the likelihood of developing preeclampsia, but do not guarantee its occurrence, requiring close monitoring. The risk of developing preeclampsia during pregnancy can be increased by several factors. Understanding these risk factors allows for proactive monitoring and correction of the pregnant woman’s condition. There is still no method to reliably determine the severity of preeclampsia and predict its further course [5]. The pathophysiology of preeclampsia remains unknown. In case of blood flow disturbances in the uteroplacental-fetal complex, pregnancy complications or other “major obstetric syndromes” develop [2]. In recent years, a whole spectrum of pregnancy complications, grouped into Great Obstetric Syndromes, have been associated with placentation defects, limited remodeling, and obstructive lesions of the myometrial segments of the spiral arteries: preeclampsia, fetal growth restriction, preterm labor, premature rupture of membranes, late spontaneous abortion, and placental abruption [6,7]. To determine the clinical significance of sFlt-1/PlGF in suspected preeclampsia, a large prospective multicenter study, PROGNOSIS (Prediction of Short-Term Outcome in Pregnant Women with Suspected Preeclampsia Study), was conducted, including 1,273 patients at 24–37 weeks of gestation. gestation [1,8]. One of the goals of this study was to determine a threshold sFlt-1/PlGF value that would exclude the development of preeclampsia within the next week. Therefore, the search for highly sensitive and specific markers that can predict preeclampsia and assess its true severity in order to select optimal management tactics for such pregnant women is ongoing. Given the above, the aim of the study was to develop and validate a predictive and preventive system for managing pregnant women with risk factors for preeclampsia or ALS based on a study of its current clinical and laboratory characteristics.
A prospective cohort study of 150 pregnant women at risk for preeclampsia was conducted. Of these, 82 patients subsequently developed preeclampsia (22 with early preeclampsia, with symptom onset before 34 weeks of gestation; 60 with late preeclampsia, after 34 weeks), and 68 did not. A complete clinical, laboratory, and functional examination was performed at the first prenatal screening (10-14 weeks) and at 18-24 weeks (the time of the screening ultrasound). The most significant factors in predicting preeclampsia were assessed at these times:
1. Medical history (preconditioning risk factors – hereditary, family history, course of previous pregnancies, etc.);
2. Where Possible, assessment of uterine artery blood flow (pulsatility index, PI);
3. 24-hour blood pressure dynamics (24-hour blood pressure monitoring);
4. Antiangiogenic factor sFlt-1 and PlGF, as well as the PlGF/ sFlt-1 ratio;
Laboratory studies were conducted at the A. Tashieva Scientific Center for Maternal and Child Health, the Bonetsky Laboratory, and Aqualab. Statistical processing of the obtained data was performed using the Statistica 8 for Windows 8.0 software package and MS Excel on a personal computer using nonparametric statistical methods. Differences were considered statistically significant at a significance level of p < 0.05.
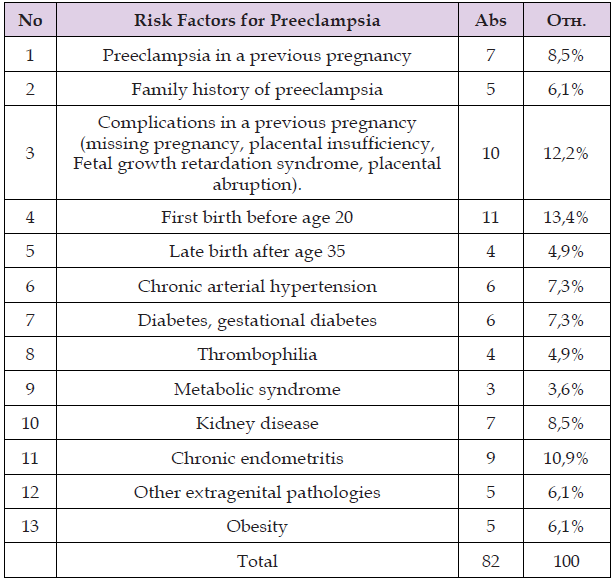
A multivariate analysis of the anamnestic data identified the most significant risk factors for preeclampsia (Table 1). As can be seen from Table 1, the following preconditioning risk factors were identified based on the anamnesis: preeclampsia in a previous pregnancy (8.5%), preeclampsia in family history (6.1%), complications of a previous pregnancy (non-viable pregnancy, placental insufficiency, Fetal growth retardation syndrome, placental abruption) (12.2%), first birth before age 20 (13.4%), late birth after age 35 (4.9%), chronic arterial hypertension (7.3%), gestational diabetes (7.3%), thrombophilia (4.9%), metabolic syndrome (3.6%), kidney disease (8.5%), chronic endometritis (10.9%), other extragenital pathologies (6.1%), obesity (6.1%). Given that chronic uteroplacental ischemia is the leading concept in the development of preeclampsia, and blood flow in the uterine arteries is an indirect marker, we conducted a Doppler assessment of the pulsatility index (PI) in these vessels in high-risk pregnant women. At 10–14 weeks of pregnancy, PI ≥95th percentile was observed in 17 women (20.7%): 5 with late preeclampsia and 12 with early preeclampsia. At 18–24 weeks of pregnancy, the same figure was observed in 18 women (21.9%): 7 with late preeclampsia and 11 with early preeclampsia. Disturbances in the circadian blood pressure biorhythm in pregnant women with preeclampsia, in particular the development of a nocturnal circadian rhythm (non-dipper type), are of scientific and practical interest. Research in recent decades has convincingly demonstrated the prognostic significance of insufficient nocturnal blood pressure reduction (Table 2).
Table 1: Risk factors for the development of preeclampsia in women in the southern regions of Kyrgyzstan.
As can be seen from Table 2, relatively high daily mean systolic blood pressure (SBP) variability (>12.7 mmHg) emerged as a significant risk factor for preeclampsia. For the prognosis and early diagnosis of preeclampsia, the characteristics of daily blood pressure fluctuations largely indicate the presence or absence of endothelial dysfunction, with varying degrees of endothelial cell damage. In the observed patients, mean daytime and mean nighttime blood pressure, as well as the magnitude of the morning blood pressure rise before the onset of clinical symptoms of preeclampsia, were within the normal range in most cases. However, by weeks 18–24, a significant increase in mean daytime and nighttime blood pressure was observed compared to the first trimester. From weeks 10–14, an increase in systolic and diastolic blood pressure variability was observed. A progressive increase in diastolic blood pressure (DBP) and the magnitude and rate of the morning BP rise, more pronounced between 18 and 24 weeks, have been noted. There is a significant increase in 24- hour and daytime hypertensive indices by 18–24 weeks, an increase in BP variability, and the magnitude and rate of the morning BP rise; nocturnal non-dipper BP dynamics are more common. The diagnosis of preeclampsia in clinical practice poses certain difficulties due to the nonspecificity of symptoms, the polymorphism of the clinical picture, and the discrepancy between the severity of clinical symptoms and the severity of multiple organ damage [3,7].
This leads to an underestimation of the severity of preeclampsia and an insufficient volume of diagnostic and therapeutic measures [8]. At the same time, preeclampsia may be overdiagnosed in clinical practice due to the nonspecificity of its symptoms and the high lability of blood pressure readings in pregnant women. Therefore, accurate diagnosis and prognosis of preeclampsia are of great importance for practical obstetrics. In the pathogenesis of preeclampsia, a key role is played by the hyperproduction of antiangiogenic factors, particularly sFlt-1, which blocks the action of placental growth factor PlGF, causing generalized endothelial dysfunction and leading to the development of clinical symptoms of preeclampsia [7]. The sFlt-1/PlGF ratio can be used to diagnose and prognosticate preeclampsia (Table 3). The sFlt-1/PlGF ratio reflects the balance between pro- and anti-angiogenic factors. This balance is disrupted in preeclampsia, and the ratio becomes high. High values, as in our study (>50.1, ranging from 43.1 to 61.3), indicate an increased risk of developing preeclampsia, which requires careful monitoring and possible hospitalization. Thus, determining the PIGF/sFlt-1 ratio is most valuable in early prediction of the risk of developing preeclampsia, especially in the second trimester. The predictive system for determining the risk of developing preeclampsia consists of the following stages:
Stage I – 10–14 Weeks of Pregnancy
1. Assessment of Clinical and Anamnestic Factors: preeclampsia in the family history (mother, sisters) or during a previous pregnancy, complicated course of a previous pregnancy, multiple pregnancies, somatic diseases.
2. Blood pressure monitoring (increased blood pressure variability, non-dipper type).
3. Biochemical markers (PIGF/sFlt-1). Stage II – 18–24 weeks of pregnancy.
Stage II – 18–24 Weeks of Pregnancy:
1. Assessment of clinical and anamnestic factors (if not performed at 10–14 weeks).
2. Doppler ultrasound (PI ≥95 percentile in the uterine arteries, early bilateral diastolic notches).
3. Blood pressure monitoring (increased blood pressure variability, magnitude and speed of morning blood pressure rise, non-dipper/night-peaker type).
4. Assessment of early clinical predictors: daily microalbuminuria, podocyturia; decreased diuresis over time; decreased platelet count over time, activation of intravascular coagulation; decreased glomerular filtration rate and/or creatinine clearance; increased creatinine and urea over time (not yet outside the reference range).
5. Biomarker determination (optimally – changes in PlGF/sFlt- 1, VEGF, NSE, or GFAP).
Predicting the risk of developing preeclampsia is most important in early pregnancy, as it enables a comprehensive multidisciplinary examination of the pregnant woman, the identification and management of any comorbidities, and the timely prevention of the most dangerous complications. The presence of one or more risk factors does not necessarily mean that preeclampsia will develop, but it does require more careful monitoring and regular visits during pregnancy. High sFlt-1/PlGF levels are associated with a significantly increased incidence of severe obstetric complications. This should be taken into account when determining obstetric management and patient management. The use of sFlt-1/PlGF allows for the differential diagnosis of preeclampsia from the exacerbation or manifestation of a number of somatic diseases that have similar clinical symptoms. The use of sFlt-1/PlGF provides economic benefits by improving patient management and reducing the incidence of severe perinatal and maternal outcomes, as well as unnecessary hospitalization. sFlt-1/PlGF is an informative marker for the diagnosis and prognosis of preeclampsia and its adverse outcomes and can be recommended for use in clinical practice.


