Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Koumadou Konstantina1, Stefanopoulos Nikolas2, Igoumenidis Michael3, Kipourgos Georgios4, Koumadou Parthenopi5 and Tzenalis Anastasios6*
Received: April 28, 2025; Published: May 06, 2025
*Corresponding author: Anastasios Tzenalis, Associate Professor at the Nursing Department of the University of Patras, Patras City, Greece
DOI: 10.26717/BJSTR.2025.61.009643
Introduction: The appropriate management and allocation of blood in hospitals are critical factors for the functioning
of the health system and saving human lives. This study investigates the perceptions of health professionals
on the appropriate management and allocation of blood in Greek hospitals.
Methods: A prospective cross-sectional study was conducted on a sample of 439 health professionals (excluding
blood donation staff) who worked in six public hospitals in Greece, from November 2023 to February 2024.
The study was based on a quantitative approach through a questionnaire in Google Forms. The questionnaire
includes closed and open questions and consists socio-demographic data and questions on “errors or omissions”
and “causes of failure or errors” in the transfusion process.
Results: The most typical errors in blood donation were the delayed transfusion, communication errors, the lack
of relevant information for the patient, no electronic record of the clinical decision to order blood and transfusion
with inappropriate flow. The most common causes of errors were distraction due to simultaneous different
tasks, excessive workload, tired or overworked staff and work stress. According to the perceptions of healthcare
professionals, training is an important factor for proper blood management. Differences were identified in the
perceptions of healthcare professionals regarding the frequency of errors and the causes of errors during the
blood management and disposal process.
Discussion: The study showed that the blood management in hospitals is a complex process influenced by many
factors. The differentiation in the perceptions of health professionals depending on their socio-demographic
characteristics such as gender, specialty and experience, indicates the need for targeted and tailored interventions
that will enhance the safety and effectiveness of these procedures.
Keywords: Blood Management; Transfusion; Errors; Causes; Perceptions
Abbreviations: ABO: Blood Grouping System; WBIT: Wrong Blood in Tube; ICU: Intensive Care Units; SHOT: Serious Hazards οf Transfusion
Blood is an essential element for medical activities. Blood allocation has always been closely related to medical therapy, and it is recognized as a core appropriate measure for the quality of medical service. Those who do not have sufficient blood supplies are forced to postpone surgical operations or to treat only selective categories of patients or to resort to practices of not examining the blood that is being used. This entails increased harm or even death in patients. A subgroup of health professionals plays a key role in both of these steps: blood donation and blood transfusion practices. The professional behaviors of these health professionals will have a direct impact on the quality and safety of blood donation and blood transfusion. In recent years, the allocation of blood in clinical practice has attracted the attention of medical professionals and society, becoming an independent part of medical services. Blood should be administered to patients with definite indications, while, on the other hand, the blind use of blood is discouraged. Proper blood management is a critical factor for safe patient care, as ensuring adequacy, availability and timely control of blood components plays an important role in the blood supply chain [1].
The outcome of the transfusion is influenced by the importance of implementing good practices. The criticality lies in ensuring and maintaining the quality of blood. Any negligence in the process of disposal and management of blood from blood departments to hospital clinics can have serious consequences on the outcome of the transfusion. Health organizations prioritize the safety of blood products prior to transfusion, and do not focus on the procedures associated with blood transfusion as a medical or nursing procedure [2]. This is because human error has been shown to be responsible for more than half of the losses associated with the transfusion process [3,4]. It is noteworthy that in recent years one of the most frequent causes of mortality associated with transfusions is the transfusion of ABOincompatible blood, which is directly related to the safety of the patient’s health [5-7]. It has been observed that about 50% of transfusion errors involve multiple errors in the procedure, while about 23% of errors come from failure during the final check stage rather than the patient’s bedside check, which is performed before the transfusion [8].The safety of transfusion procedures depends on a series of steps that include the decision to administer the appropriate blood, sample collection, labelling, transportation and handling, as well as pre-transfusion testing and the final administration of the blood to the patient. Any error in any of these steps can lead to the donation of the wrong blood, with serious consequences for the recipient. Regarding the stages of transfusion, at each step there are possible risks, such as errors in patient identification, blood standardization, matching and other human errors. According to the international literature, errors can occur during the identification of the patient, during the collection and laboratory analysis of the samples, in the management of blood products (from their collection to their final use), as well as during the transfusion [6,7]. Blood transfusion is a complex process that involves, in addition to blood donors and recipients, professionals of various specialties such as doctors, nurses and laboratory staff [9]. Due to the complexity of the process, the risk of errors is high. An important factor that has been identified to significantly affect the occurrence of errors during the transfusion process is the poor level of communication between the involved health professionals of different specialties. Moreover, it has been found that communication problems between clinics/departments and the blood donation department are the main causes of delayed transfusions [10]. Another key factor causing errors is inadequate training of healthcare professionals. Studies report that the lack of knowledge in the use of blood management software, in the labeling of samples, in the understanding of the differences between blood components and in the verification procedures [10] are problems that lead to avoidable errors [11].
Providing appropriate knowledge is vital to reducing errors. Other studies have identified that factors contributing to WBIT errors are protocol violations, human omissions/errors by healthcare professionals, distraction, fatigue, workplace stress, hospital safety culture, levels of teamwork and feedback and infrastructure [12-14]. To address errors that occur during the transfusion phase, countries have developed guidelines to improve blood management. Strategies usually include early and adequate preoperative risk assessment, intraoperative techniques to minimize blood loss, and targeted transfusion- guided therapy [15,16]. In Greece there are few publications about the procedures of proper management and disposal of blood from blood donation departments to hospital clinics. Therefore, it is very important to record the transfusion procedures applied in hospitals, the problems they face and to formulate proposals aimed at planning appropriate interventions.
Sample size
The study sample comprised a total of 439 health professionals who worked in public hospitals in Greece.
Study Area
The study sample consisted of doctors and nurses working in pathology, surgery, ICU and anesthesiology.
Study Population
The study population was health professionals working (excluding blood donation staff) in 6 major hospitals in Greece.
Study design
A prospective study design was employed.
Study Duration
The study was conducted from November 2023 to February 2024.
Inclusion Criteria
The method applied to select the sample was purposive sampling and specifically the snowball technique using a gatekeeper. The researcher, in consultation with the respective director of the Department, collected the emails of the executives who will be invited to participate in the research. Then, via Googleforms, the researcher would send email to the target group, which included informative note regarding the research and provided the unique link to complete the questionnaire online.
Ethical issues
The study was conducted with approval from the Ethics and Deontology Committee of six major hospitals across the country. Ηealth professionals anonymity was preserved throughout the study.
The research is cross-sectional and would include a quantitative approach. The quantitative approach was done by collecting quantitative data, choosing the questionnaire as a tool. The questionnaire would be in electronic form and was created through the free web application Google forms.A pilot study was conducted on 20 people to find out if there were any problems or difficulties. After analyzing and evaluating the data, we proceeded to distribute the questionnaire. The questionnaire includes closed and/or open type questions and will consist of 2 parts:
• Part A: Sociodemographic data of the sample
• Part B: Questions regarding “errors or omissions” and “causes of failure or errors” during the transfusion process. Cronbach’s alpha was used to measure the internal consistency reliability of the survey questionnaire [17]. Cronbach’s alpha is a measure of whether respondents answer the questions in a similar way (consistency). The value of the Cronbach’s alpha coefficient should be at least ≥0.70. The Cronbach’s alpha coefficient was 0.949, indicating very high internal consistency reliability of the questionnaire.
Statistical Analysis
The data collected through the electronic questionnaires were entered into a spreadsheet excel sheet where the variables were coded and then entered into the statistical SPSS version 22 program where they were processed. The descriptive analysis of the results included absolute and relative frequencies, mean values, standard deviations, tables and graphs. The bivariate analysis included statistical techniques depending on the type of subject’s variables. The variables did not follow the normal distribution according to the results Kolmogorov- Smirnov [18] and Shapiro-Wilk tests [19]; therefore, non-parametric statistical methods [20]. The alpha level of statistical significance (α) was set at α=5% (or 0.05). For the comparison between nominal variables and quantitative or ordinal variables non-parametric Mann Whitney U test [21] was carried out where appropriate and Kruskal Wallis H test [22].
Demographics
The survey sample consisted of 439 health professionals (excluding blood donation staff) working in six major hospitals across the country. The sample comprised 62.2% women and included health professionals primarily aged 40-49 years (41.5%), with smaller representations in age groups over 50 (23.9%), 30-39 (22.3%), and 20-29 years (12.3%). Participants included nurses in surgical departments (28.9%), clinicians (28.5%), pathology nurses (24.4%), and ICU or operating room nurses (18.2%). Educationally, 55.6% were graduates of higher education institutions, and 25.7% held postgraduate degrees. Most participants had over 16 years of professional experience (42.8%), while 33.5% had 6-15 years, and 23.7% had 0-5 years. The total demographics of the sample are presented in Table 1.
Αttitudes and Knowledge
Of the respondents, 51.7% reported having attended a training course on blood management procedures. When asked about the reasons for attending, 33.7% cited “Out of personal interest,” while 27.9% selected “To do my job better.” Regarding their self-assessment of knowledge, the majority of the sample (65.8%) considered their understanding of blood management procedures to be satisfactory. Furthermore, an overwhelming 96.8% expressed interest in further education on the subject. In terms of the impact of prior training on error frequency, 88.4% of the sample believed that the education of healthcare professionals significantly contributes to reducing errors in the blood management and administration process. To a question regarding the existence of protocols for blood management and disposal, the vast majority of respondents (97.0%) confirmed the presence of such protocols within their organizations. This high percentage reflects substantial adherence to standardized practices in blood handling and disposal among the surveyed health professionals. In response to the statement, “The better the level of communication between nursing departments and blood donation, the lower the incidence of errors in blood management (please indicate whether you agree or disagree),” 63.8% of respondents indicated “Strongly agree,” 29.8% responded “Agree,” 3.6% were “Neutral,” 1.8% selected “Strongly disagree,” and 0.9% chose “Disagree.” When asked about the procedures followed for checking and collecting blood in the clinic (with the possibility of selecting more than one answer), a total of 1,637 affirmative responses were recorded. These responses were almost evenly distributed among the provided options: 26.5% selected “Confirm data,” 25.4% chose “Expiration date,” 24.1% indicated “Correct derivative,” and 23.3% selected “Review bag for damages. “Regarding the storage of blood in clinics, the majority of respondents indicated that blood is stored in the “Refrigerator” (76.1%), while the remaining 23.9% stated that blood is kept in the freezer. Respondents were asked about the frequency of various errors occurring during the blood management and disposal process. The responses are presented in terms of relative frequencies, means, and standard deviations. As shown in Table 2 below, the overall mean score for the responses was 2.13 (standard deviation = 0.62). The errors with the highest mean scores, indicating the most frequent occurrences, were as follows: performing a transfusion with a time delay, which had a mean of 3.13 (standard deviation = 1.32); delayed disposal and/or transfusion of blood, with a mean of 3.06 (standard deviation = 1.28); communication errors between nursing staff and Blood Donation Department staff, with a mean of 2.80 (standard deviation = 1.11); lack of relevant patient information, with a mean of 2.68 (standard deviation = 1.02); absence of an electronic record of the clinical decision to order a blood bag, with a mean of 2.67 (standard deviation = 1.15); and transfusion with inappropriate flow, with a mean of 2.62 (standard deviation = 1.00). The total number of responses is shown in the table below. In an effort to investigate the factors influencing the occurrence of the previously mentioned errors, the sample responses with the highest mean values, indicating the most frequent causes, were as follows: distraction due to simultaneous tasks, with a mean of 4.14 (standard deviation = 1.02); excessive workload, with a mean of 4.13 (standard deviation = 1.01); tired or overworked staff, with a mean of 4.11 (standard deviation = 1.03); and work stress, with a mean of 4.08 (standard deviation = 1.00).
Two Variable Analysis
The research team examined the potential influence of participants’ socio-demographic characteristics on their perceptions of error incidence during the blood management and disposal process. The analysis revealed that gender, years of experience, and specialty were statistically significant factors. Specifically, the Mann-Whitney U test demonstrated that gender significantly affects health professionals’ views on the occurrence of errors in the blood management and disposal process (U = 13,591.000, N_male = 166, N_female = 273, p = 0.000, two-sided test). Table 3 presents a comparison of male and female perspectives on this issue. A further analysis was conducted to investigate the relationship between the specialty of healthcare professionals and their perceptions of error incidence in the blood management and disposal process. The Kruskal-Wallis H test, applied to independent samples from four groups (Clinician, Pathology Department Nurse, Surgical Department Nurse, ICU Nurse and Operating Room Nurse), revealed that specialty significantly influenced views on error incidence during the blood management and disposal process (χ² = 41.297, df = 3, p = 0.000, two-sided test). Specifically, it was shown that the observations for the specialty “Clinician” tended to be higher than those for the specialty “Pathology Department Nurse”, which in turn were higher than those for the specialty “Surgical Department Nurse”, which in turn were higher than those for the specialty “ICU and Operating Room Nurse”. Finally, the relationship between the years of service of the participants and their perceptions of error incidence in the blood management and disposal process was examined. The Kruskal-Wallis H test, applied to three independent groups (0-5 years, 6-15 years, and 16 years or more), revealed that years of service significantly influenced views on the occurrence of errors in the blood management and disposal process (χ² = 29.272, df = 2, p = 0.000, two-sided test). The results showed that the observations for years of service “6-15 years” tended to be higher than those for years of service “0-5 years”, which in turn were higher than those for years of service “16 years and above”. A second research hypothesis examined whether demographic characteristics influence the participants’ views on the factors contributing to errors in the blood management and disposal process. The analysis confirmed that gender (Mann-Whitney U = 16,082.500, N_male = 166, N_female = 273, p = 0.000, two-sided test), professional specialty (Kruskal-Wallis χ² = 41.323, df = 3, p = 0.000, two-sided test), and years of experience (Kruskal-Wallis χ² = 23.492, df = 2, p = 0.000, two-sided test) are significant factors affecting these views. In contrast to prior findings, demographic variables such as age and educational qualifications were not found to be significant predictors of participants’ views on the frequency or causes of errors in the blood management and disposal process. A final exploratory analysis examined whether prior training of healthcare professionals influences the incidence of errors in the blood management and disposal process. The study assessed whether a statistically significant difference exists in the incidence of errors between two groups:
a. Healthcare professionals (excluding blood donation staff) who perceive that prior training influences error rates, and
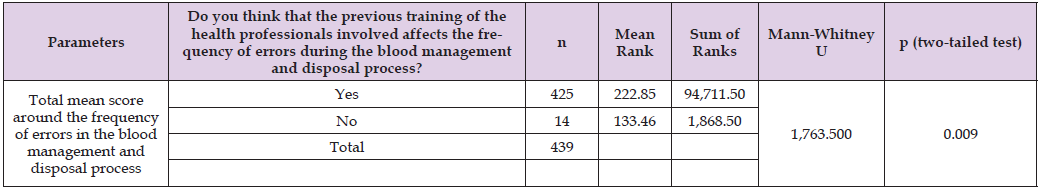
b. Healthcare professionals who do not share this perception. The Mann-Whitney U test, applied to independent samples from these groups, indicated a statistically significant difference in error incidence. Specifically, a higher incidence of errors was associated with healthcare professionals who perceived prior training as influential on error rates in blood management and disposal (U = 1,763.500, Yes = 425, No = 14, p = 0.009, two-sided test). Detailed results of this analysis are presented in Table 4.
Table 3: Potential influence of participants’ socio-demographic characteristics on their perceptions of error incidence during the blood management and disposal process.
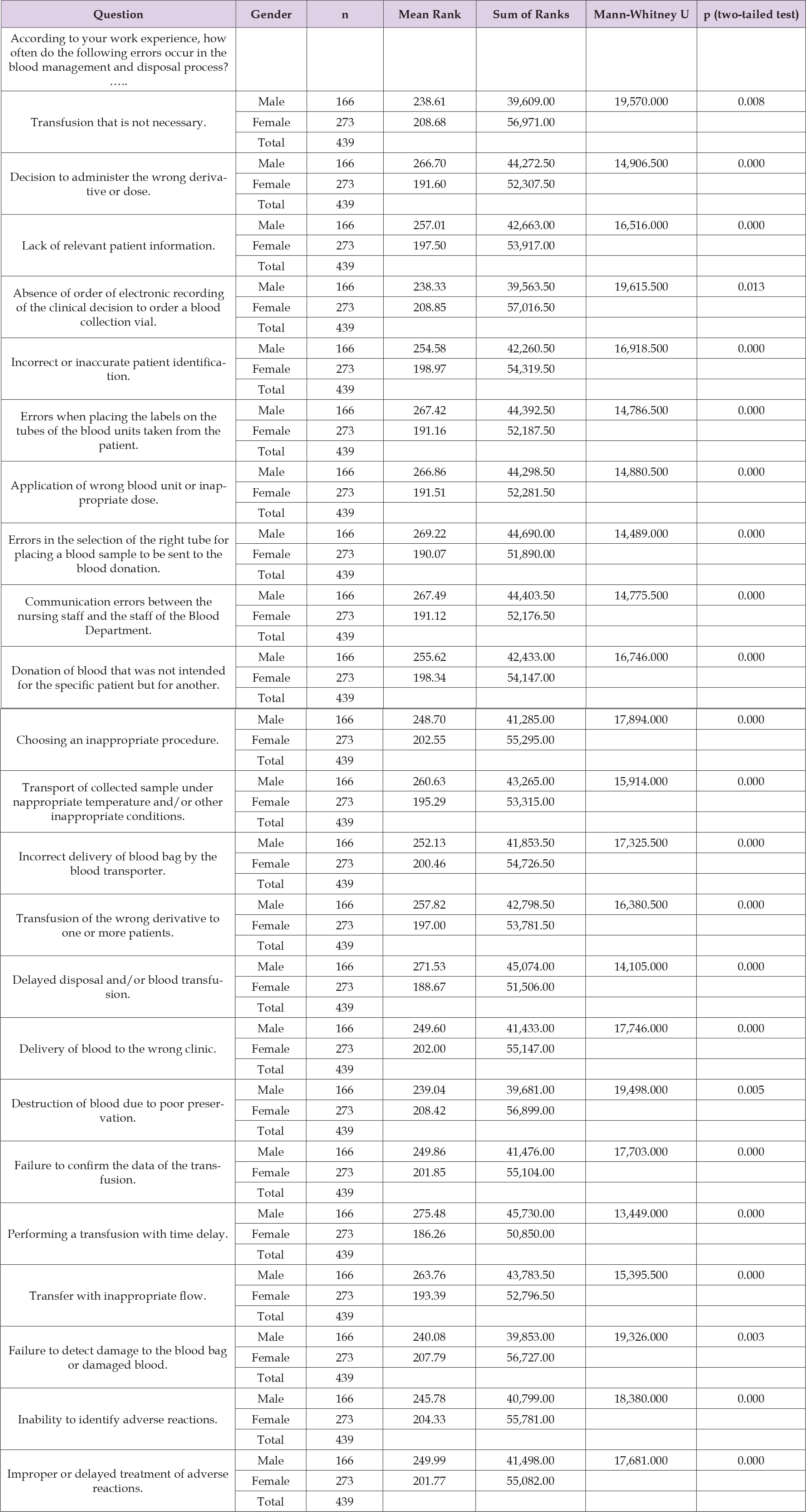
Table 4: Investigation of the relationship between the previous training of the health professionals involved (other than blood donor personnel) and the incidence of errors in the blood management and disposal process.
The findings of this study provide valuable insights into the knowledge, attitudes, and perceptions of healthcare professionals regarding blood management and disposal procedures, as well as the factors that influence the incidence of errors in this context.
Healthcare Professionals’ Perceptions and Education
The majority of healthcare professionals considered their knowledge of blood management to be adequate, with 51.7% having attended relevant training courses and 96.8% expressing interest in further education. These results indicate a high level of interest in continuous knowledge improvement, which is critical given the significant role that training plays in reducing errors, as also reflected by the 88.4% of respondents who believe that education significantly reduces errors. This finding aligns with previous studies that indicate training reduces the likelihood of medical errors, particularly in processes associated with the safe handling of blood.
According to Mohd Noor, et al. [23] nurses’ knowledge plays an essential role in ensuring quality and safety in blood transfusion. Another study showed that low education was a key determining factor of lack of knowledge and bad practices associated with transfusion [24].
Protocols and Communication Procedures
The study also highlighted strong adherence to blood management protocols, with 97.0% of professionals confirming the existence of such protocols in their organizations. Moreover, there was clear agreement regarding the importance of communication between departments, as 63.8% strongly agreed that improved communication reduces errors, underscoring the critical role of interdisciplinary communication. This result is supported by studies that emphasize the importance of collaborative care models and cross-departmental communication in preventing medical errors. According to the Serious Hazards of Transfusion (SHOT) study (1996-2008), an important factor that has been identified as significantly influencing errors in the transfusion process is the poor level of communication between healthcare professionals of different specialties. Moreover, communication problems between clinics/departments and the blood donation department have been found to be the main causes of delayed transfusions [25].
Factors Affecting the Incidence of Errors
Analyzing the frequency of errors, the study identified key issues, such as delayed transfusions and incomplete patient information. Factors such as distraction due to simultaneous tasks, excessive workload, and stress emerged as primary causes, findings that are consistent with the literature. This observation underscores the need to reduce workload and enhance support for healthcare professionals, elements that have been shown to mitigate error risks. Dunbar, et al. [12] conducted an international, multicenter, descriptive study to identify the factors that cause errors. The study showed that protocol violations and omissions/errors often contribute to errors
Impact of Demographic Characteristics
The two-variable analysis demonstrated that gender, specialty, and years of experience significantly affect healthcare professionals’ perceptions of error incidence. The impact of specialty is particularly indicative of the varying nature of duties and responsibilities faced by healthcare professionals in different departments, which calls for more targeted educational interventions according to specialty. Prior research has shown that experience can influence error perceptions, highlighting the need to develop programs catering to professionals with varying experience levels.
Effect of Training on Errors
Finally, the analysis revealed that professionals who consider training as a key factor in error reduction tend to have more favorable views on its necessity, reflecting the influence of knowledge and confidence on the adherence to proper procedures. This finding aligns with existing literature that links professional training with lower error rates.
This study highlights critical areas for further investigation, such as the impact of specialty-specific training and the role of the work environment in error prevention. Practically, systematic implementation of training programs tailored to healthcare professionals’ unique roles, improvement of support systems, and promotion of interdisciplinary collaboration are recommended.
No conflict of interest.

