Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Sherine Abdelmissih1*, Essraa Hegazy2, Shaimaa Hussein3 and Afaf Osman1
Received: July 24, 2023; Published: September 01, 2023
*Corresponding author: Sherine Abdelmissih, Medical Pharmacology Department, Faculty of Medicine, Kasr Al-Ainy, Cairo University, Cairo, Egypt
DOI: 10.26717/BJSTR.2023.52.008281
Background: Coronavirus disease 2019 (COVID-19) due to the acute respiratory syndrome coronavirus-
2 (SARS-CoV-2) caused a global health crisis that called for re-purposing of many medications. Both
the implication of diabetes mellitus (DM) in increasing the risk of COVID-19-associated respiratory
complications, together with the claims about the involvement of acidic pH in exacerbating acute lung
injury as well as SARS-CoV-2 invasion, growth, and replication, guided our interest towards possible
efficacy of antidiabetic and anti-peptic ulcer medications in such condition. The present work aimed
to evaluate the safety and antiviral efficacy of the oral antidiabetic, metformin, and the anti-ulcer,
misoprostol, on SARS-CoV2-infected Vero-E6 cell line.
Method: SARS-CoV-2 strain was cultured on Vero-E6 cells lines, followed by the addition of various
concentrations of either metformin or misoprostol to evaluate the cell line viability, followed by selection
of concentrations to explore their antiviral activity.
Results: Concentrations that achieved 80% or more cell viability were selected to test for viral inhibitory
activity. Metformin was found to be more effective in inhibiting SARS-CoV-2 and less cytotoxic than
misoprostol. However, both drugs exhibited narrow therapeutic range, attributed to high cellular
cytotoxicity with increasing doses.
Conclusion: Our preliminary in vitro data indicated that dosing of metformin and misoprostol in COVID-19
should be done cautiously. Further in vitro studies are needed to elaborate the safety and efficacy of both
drugs in other cell cultures. In vivo experiments and observational clinical studies are also recommended
to determine the benefit-to-risk ratio for either metformin or misoprostol in COVID-19 settings.
Keywords: COVID-19; Cytotoxicity; Metformin; Misoprostol; Sars-Cov-2; Vero-E6; Viral Inhibition
Abbreviations: ACE2: Angiotensin Converting Enzyme 2; AMP: 5’-Adenosine Monophosphate; AMPK: 5’-Adenosine Monophosphate -Activated Protein Kinase; CC50: Half Maximal Cytotoxic Concentration; COVID-19: Coronavirus Disease 2019; CPE: Virus-Induced Cytopathic Effect; CRP: C-reactive Protein; CS: Corticosteroids; DM: Diabetes Mellitus; DMEM: Dulbecco’s Modified Eagle Medium; H2 Blockers: Histamine-2 Receptor Blockers; IC: Viral Inhibitory Concentration; IL-2: Interleukin-2; IL-6: Interleukin-6; MTT: 3-(4, 5dimethylthiazol -2-yl)-2, 5-diphenyltetrazolium Bromide; NFκB: Nuclear Factor Kappa-B; NRC: National Research Center; NSAIDs: Non-Steroidal Anti-Inflammatory Drugs; PGE1: Prostaglandin E1, PGE2: Rostaglandin E2, PGs Prostaglandins; PPIs: Proton Pump Inhibitors; PUD: Peptic Ulcer Disease; SARS-CoV-2: Coronavirus- 2; T2DM: Diabetes Mellitus Type2 DM; TMPRSS-2: Transmembrane Protease Serine-2; TNF-α: Tumor Necrosis Factor-Alpha
Coronavirus disease 2019 (COVID-19) is a pandemic the world has been facing since December of 2019. It has become a global leading cause of morbidity and mortality, with few effective therapeutic modalities. Outstanding efforts have been advocated to either re-purpose existing medications or develop de novo drug molecules. Angiotensin converting enzyme 2 (ACE2), assisted by the transmembrane protease serine-2 (TMPRSS-2) enzyme, was suggested to be the portal of viral entry into pulmonary as well as other cells [1]. Several risk factors predisposing to severe disease have been identified such as old age, chronic pulmonary disease, smoking, obesity, cardiovascular diseases, hypertension and diabetes mellitus (DM) [2,3]. In the setting of hospitalized patients with COVID-19, cases with DM were 2-3 folds more likely than nondiabetics to require admission to intensive care unit and the mortality rate was at least doubled in this vulnerable group [4]. Recently, COVID-19 was claimed as one of the triggers of both types (1&2) of DM [5]. Joshi and Pozzilli [6] proposed several mechanisms by which de novo DM followed COVID-19 infection, including direct pancreatic beta-cell damage by the virus [7] or its inflammatory storm [8], and indirectly through the virus-mediated defective ACE2, reducing both beta cell mass proliferation and vascularity. Also insulin resistance might contribute [9]. Metformin, a widely used anti-diabetic drug known for enhancing insulin sensitivity, is an effective, safe, and inexpensive oral euglycemic drug. Additionally, metformin can reduce the risk for cardiovascular events in patients with type2 DM (T2DM) [10]. The ability of metformin to inhibit viral replication was detected in Kaposi’s sarcoma - associated herpes virus, hepatitis B virus cell culture, dengue virus and cytomegalovirus [11].
The possible beneficial effects of metformin in patients with COVID-19 include anti-inflammatory potentiality, elevation of the cellular pH, interfering with lung fibrosis [12]. Nonetheless, metformin use in patients with COVID-19 and concomitant T2DM may carry a potential risk for lactic acidosis, aggravated by multi-organ failure. Another anticipated issue is that metformin might promote SARS-CoV-2 infection by increasing ACE2 availability in the respiratory tract [13]. On the other side, and despite being a primarily respiratory disease, gastrointestinal manifestations were also prevalent with COVID-19 [14], mostly attributed to abundance of ACE2 in visceral adipose tissue, promoting viral invasion [15]. Recently, acid pH was implicated in higher morbidity and mortality with COVID-19, by inducing ACE2 expression [16]. The nature of such acid/ACE2 association is still unidentified. Meanwhile, claims about hypoxia with subsequent acidosis, secondary to COVID-mediated pulmonary damage, could contribute [17]. Fortunately, resolving hyperacidity using a histamine receptor type-2 blocker, namely famotidine, was associated with improved clinical outcomes in hospitalized patients with COVID-19 [18], although, direct viral inhibition of famotidine was not excluded. In other studies, famotidine did not show such therapeutic privilege [19]. Conversely, cases administered proton pump inhibitors (PPIs) showed more severe COVID-19, probably related to reduced protection owing to suppressed gastrointestinal microbiota with pharmacologic manipulation of pH [20]. Interestingly, COVID-19 was suspected as a provocative factor in peptic ulcer disease (PUD) when several cases exhibited gastrointestinal symptoms after COVID-19, with or without respiratory symptoms [21,22]. Notably, PUD is also one of the common complications of T2DM [23]. It is noteworthy that the uses of non-steroidal anti-inflammatory drugs (NSAIDs) are adopted in patients with COVID-19 to relieve muscle pain, fatigue, fever, and headache [24]. Also, regimens employing corticosteroids (CS) are introduced as anti-inflammatory and anti-fibrotic modalities that may play a role in reducing pulmonary inflammation in severe pneumonia and advanced stages of COVID-19 disease [25].
Both NSAIDs and CS induce PUD, by interfering with prostaglandin (PGs) synthesis that were identified as inflammatory mediators implicated in the progression of COVID infection [26]. It is to be considered that the synthetic prostaglandin E1 (PGE1) analog, misoprostol, was, not only used in prevention and treatment of NSAIDs-induced gastroenteropathies [27], but also it demonstrated antiviral activity by suppressing the viral antigen expression in patients with viral hepatitis, thus reducing hospital stay [28], while showing an anti-inflammatory activity, as evidenced by suppressed responses to tumor necrosis factor-alpha (TNF-α), a crucial determinator of the degree of lung fibrosis in patients with COVID-19 [29]. The present study aimed to explore metformin and misoprostol as potential anti- SARS-CoV-2 medications, by employing various concentrations of metformin and misoprostol to test for cellular cytotoxicity in SARSCoV- 2-infected Vero-E6 cell line, then selecting the concentrations that achieved acceptable cellular viability of ≥80% to proceed to viral inhibitory testing.
SARS-CoV-2 strain was cultured on Vero-E6 cells lines twice, once to assess the cytotoxic activity of metformin and misoprostol by using different concentrations, and the second time, using the selected doses that exhibited acceptable cell viability, to test for their viral inhibitory activity. All experiments involving virus culture were conducted under appropriate conditions in the biosafety level-3 laboratory at Virology Unit, National Research Center (NRC), Giza, Egypt.
Virus Routine Propagation
SARS-CoV-2 strain was obtained from strain bank (hCoV-19/ Egypt/NRC-03/2020 (Accession Number on GSAID: EPI_ISL_430820) at Virology Unit, National Research Center (NRC), Giza, Egypt. SARSCoV- 2 was grown in Vero-E6 (ATCC® CRL-1586™) (Sigma-Aldrich, co) with Dulbecco’s modified Eagle medium (DMEM) supplemented with 10% fetal bovine serum (Sigma-Aldrich, co), 50 units/ml penicillin (SigmaAldrich, co), 50 μg/mL streptomycin (Sigma-Aldrich, co) at 37 °C in a humidified atmosphere with 5% CO2. Cells were regularly checked for clearance from mycoplasma contamination [30].
Drugs and Chemicals: Metformin hydrochloride powder and misoprostol hydrochloride powder (Sigma-Aldrich, co) were freshly dissolved and diluted in DMEM to obtain the needed concentrations. Penicillin-streptomycin P4333-100 mL (Sigma-Aldrich, co): solution stabilized, with 10,000 units/mL penicillin and 10 mg/mL streptomycin/ Ml. Between 0.5 and 1 mL of penicillin-streptomycin solution were added to 100 mL of cell culture media for a final concentration of 50 - 100 I.U. /mL penicillin and 50 to 100 μg/mL streptomycin.
Cell Line Assays
Treatment of Cell Line for Cytotoxicity Assay: Tested cell lines were seeded in 96-well flat bottom microplates (Ref. 020036, Dutscher) into their medium containing 2% fetal bovine serum and incubated for 8 h at 37 °C. The wells were divided into three groups as follows:
Group I (n= 6): Control mock cell line microplates were treated with distilled water (DW)
Group II (n= 45): Cell line microplates were treated with metformin (Sigma-Aldrich, co) at multiple concentrations derived from 0.0008 mg/ml (0.8 μg/ml) [31].
Group III (n= 45): Cell line microplates were treated with misoprostol (Sigma-Aldrich, co) at multiple concentrations derived from 0.00004 mg/ml (0.04 μg/ml) [32,33].
Assessment of Half Maximal Cytotoxic Concentration (CC50):
To assess the half maximal cytotoxic concentration (CC50), stock solutions
of the test compounds were prepared and diluted in DMEM. The
cytotoxic activity of the extracts was tested in Vero-E6 cells by using
the 3-(4, 5-dimethylthiazol -2-yl)-2, 5-diphenyltetrazolium bromide
(MTT) method. Briefly, the cells were seeded in 96 well-plates (100
μl/well at a density of 3×105 cells/ml) and incubated for 24 h at 37 °C
in 5%CO2. As a pre-treatment, cells were subjected to our tested drug
compounds at various concentrations, then cell line was subjected to
SARS-CoV-2 infection in serum-free medium (SFM) in the presence
of the respective compound. Media supernatant was collected and
subjected to measuring viral titres. Measuring infectious viral titres
was done using MTT assay to compare mock and studied cell line results.
24-h later, the supernatant was discarded, and cell monolayers
were washed with sterile 1x phosphate buffer saline (PBS) 3 times,
and MTT solution (20 μl of 5 mg/ml stock solution) was added to
each well and incubated at 37 °C for 4 h followed by medium aspiration.
In each well, the formed formazan crystals were dissolved with
200 μL of acidified isopropanol (0.04 M HCl in absolute isopropanol
= 0.073 mL HCL in 50 mL isopropanol). Absorbance of formazan
solutions was measured at λmax 540 nm with 620 nm as a reference
wavelength using a multi-well plate reader. The plot of % cytotoxicity
versus sample concentration was used to calculate the concentration
which exhibited 50% cytotoxicity (CC50) and to our interest, select the
concentrations that achieved ≥ 80% cell viability. The percentage of
cytotoxicity compared to the untreated cells was determined with the
following
equation:
Assessment of Viral Inhibitory Concentration (IC): The viral inhibitory concentration (IC) of the compound is the concentration required to reduce the virus-induced cytopathic effect (CPE) relative to the virus control assessed using crystal violet assay which relies on washing away the detached dead cells from cell culture plates and the staining of the remainder live cells with crystal violet dye that is solubilized and measured by absorbance at 570 nm. In 96-well tissue culture plates, 2.4×104 Vero-E6 cells were distributed in each well and incubated overnight at a humidified 37°C incubator with 5% CO2. The cell monolayers were then washed once with 1x PBS and subjected to virus adsorption (hCoV-19/Egypt/NRC-03/2020 (Accession Number on GSAID: EPI_ISL_430820)) for 1 h at room temperature (RT). The cell monolayers were further overlaid with 50 μl of DMEM containing the selected concentrations of the test sample. Following incubation at 37°C in 5% CO2 incubator for 72 h, the cells were fixed with 100 μl of 4% paraformaldehyde for 20 min and stained with 0.1% crystal violet in distilled water for 15 min at 37° C. The crystal violet dye was then dissolved using 100 μl absolute methanol per well and the optical density of the color was measured at 570 nm using Anthos Zenyth 200rt plate reader (Anthos Labtec Instruments, Heerhugowaard, Netherlands) [35].
Statistical Analysis
Statistical analysis was done using SPSS v.28.0.1.0. Data were presented as mean ± SD. Regression analysis for viral inhibition was done. p value <0.05 was considered statistically significant.
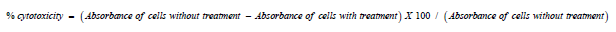
Metformin Cytotoxicity
Cell viability (%) achieved by metformin at a concentration ranging 0.0001-4.5 mg/ml. Cytotoxicity was diminishing in a dose-dependent manner. The half maximal cytotoxic concentration (CC50) of metformin cytotoxicity was 0.94 mg/ml. 90% cytotoxicity manifested at a concentration of 4.5 mg/ml, while 80% cytotoxicity was associated with 3.2 mg/ml. Acceptable cell viability ≥ 80% was attained with 0.01, 0.02 & 0.05 mg/ml (Figures 1 & 2).
Viral Inhibitory Activity of Metformin
The least concentration of 0.0001 mg/mL was not effective. The metformin concentrations that were associated with ≥ 80% cell viability were chosen to proceed with viral inhibition. The safest effective concentrations of 0.05, 0.02 and 0.01 mg/ml caused 22, 18 and 12% viral inhibition, respectively (Figures 3 & 4).
Misoprostol Cytotoxicity
Cell viability (%) achieved by misoprostol at a concentration ranging 0.02-2.4 mg/mL Cytotoxicity was diminishing in a dose-dependent manner. Concentration of 0.1 mg/ml caused 100% cellular cytotoxicity that was discarded and replaced by 1/10th this concentration. The half maximal cytotoxic concentration (CC50) of misoprostol cytotoxicity was achieved at 0.44 mg/ml. 90% cytotoxicity was attained at 2.2 mg/ml. Acceptable cell viability ≥ 80% was attained with 0.08, 0.13 & 0.16 mg/ml (Figures 5 & 2).
Viral inhibitory Activity of Misoprostol
The least concentration of 0.02 mg/mL was not effective. The misoprostol concentrations that were associated with ≥ 80% cell viability were chosen to proceed with viral inhibition. There was a dosedependent viral inhibition. The safest effective concentrations of 0.16, 0.13 and 0.08 mg/ml caused 2.9, 2.5 and 1% viral inhibition, respectively (Figures 6 & 4).
The pandemic of COVID-19 and its complications mandated an urgent need for proper treatment that is effective and safe. One strategy of addressing COVID-19 was the re-purposing of available medications. In the present study, metformin, an oral euglycemic medication and misoprostol, a prostaglandin E1 (PGE1) analog and anti-peptic ulcer medication, were tested to detect their safety and antiviral activity in SARS-Cov2-infecetd VERO-E6 cell line. Metformin use in the present study showed a dose-dependent SARS-CoV-2 inhibition reaching up to 80% inhibition with a concentration of 4.5 mg/ mL. Such antiviral therapeutic potential was emphasized in the work of Postler et al. [36] who noticed the efficacy of metformin against lipopolysaccharide- induced lung injury in mice inoculated with SARSCoV- 2. In hospitalized cases of COVID-19, patients with T2DM maintained on metformin showed an improved outcome and increased survival [37,38]. Likewise, metformin was associated with reduced COVID-19-related mortality [39]. Metformin was reported to lower cardiovascular risk, insulin resistance, systemic inflammation, and hypercoagulability in diabetic patients during COVID infection [40]. As the hyper-inflammatory state (cytokine storm) is one major contributor to COVID-19 morbidity and mortality, perhaps the therapeutic utility of metformin is mediated via the activation of 5’-adenosine monophosphate (AMP)-activated protein kinase (AMPK) [41], being an anti-inflammatory mediator as was demonstrated in a mouse model of autoimmune arthritis [42]. Parthasarathy et al. [43] emphasized that AMPK activation mediated by metformin supports the immune system at multiple levels. AMPK also regulates mitochondrial homeostasis, autophagy and apoptosis [44].
Dynamic decrease of serum inflammatory factors, including C-reactive protein (CRP), interleukin-6 (IL-6), interleukin-2 (IL-2) and tumor necrosis factor-alpha (TNF-α) was detected in the hospitalized COVID19 patients with metformin treatment than the non-metformin group [45]. Metformin also decreases circulating lipids which decreases viral load. RNA viruses need lipid droplets for proper virus backing and release. This suggests that the anti-viral effect of metformin may result from altered lipid metabolism [46]. AMPK enhances ACE2 phosphorylation, reducing SARS-CoV-2 binding. However, phosphorylation of ACE2 may slow the degradation of ACE2, theoretically increasing its concentration that means more virus entry. Nonetheless, potential benefits override the potential harms [47]. Thus, we can extend the use of metformin from specific treatment in diabetics to a more generalized scope, even in absence of DM. On opposite side, Bramante et al. [48] detected that metformin didn’t prevented the occurrence of hypoxemia, an emergency department visit, hospitalization, in COVID patients. These results may be due to high percent number of included patients were overweight or obese, different races in United States that included in the study. Also, use of hypoxemia as an end point as use of oximetry may be not accurate and carry incidence of measurement error caused by cold hands or improper fit [49]. Nevertheless, in our work, the dose-dependent viral inhibition of metformin was limited by its cytotoxicity, so that the safe effective concentration of 0.05 mg/mL achieved 22% viral inhibition. This concentration was 1/100th the concentration achieving 80% viral inhibition which caused 90% cellular cytotoxicity. Likewise, the cytotoxic activity of metformin was obvious in vitro cancer studies, enhancing the cytotoxic activity of cis-platin in esophageal squamous cell carcinoma cell line (ECA109) at 6.1 mM [50].
Metformin at micromolar concentrations suppressed cell proliferation in mouse models and patients with DM, while higher concentrations of millimolar values were required to produce such effect in vitro cell lines [51]. A secondary effect of metformin in hypoxic states would be the increased production of lactic acidosis with tissue hypoxia, especially with respiratory diseases [52]. In this context, recommendation of discontinuing using metformin with severe COVID-19 as it induced respiratory complications, even with close monitoring of acidosis and renal functions [45]. COVID-19 Treatment Guidelines Panels recommended against the use of metformin as a treatment for COVID-19, though advised patients already on metformin regimen to continue their medication under the medical supervision [53]. Recently published as an expert opinion, metformin was suggested as a therapeutic modality for COVID-19, namely, outpatients and post-COVID [54], but in acute COVID settings, the dilemma remains unresolved. In terms of inflammatory storm during COVID-19, claims about the feasibility of NASIDs arise from their ability to inhibit the synthesis of inflammatory prostaglandins (PGs) such as prostaglandin E2 (PGE2) [55]. While existing literature converged on studying or discussing PGE2 [56,57], the role of PGE1 was overlooked, despite its anti-inflammatory role in rats and humans [58–60]. To our knowledge, our study was pioneer to test the efficacy and safety of misoprostol in SARS-CoV2-infected VERO-E6 cell line.
In the present study, misoprostol was much less effective than metformin, so that while a concentration of 0.02 mg/mL of metformin achieved 18% viral inhibition, it was ineffective for misoprostol. Similarly, misoprostol was much less safe than metformin, with 1 mg/mL of metformin causing 45% cell viability, versus 25% with misoprostol. In a previous study, a positive link was outlined between the use of potent antisecretory drugs that lower gastric pH such as proton pump inhibitors [61] or histamine-2 receptor (H2) [62] blockers and the susceptibility to COVID-19 infection, as the virus can invade the body through its gastrointestinal tract and has been recovered in the stool of patients [63], increasing the likelihood of lung invasion and injury [64]. Misoprostol can decrease acid secretion as well as showing an anti-inflammatory effect in experimental models of rheumatoid arthritis, systemic sclerosis, pulmonary hypertension, and glomerulonephritis [65]. Misoprostol has been reported to decrease pro-inflammatory cytokine as TNF α, IL6, and IL-8 as PGE1 activates cAMP. cAMP can decrease nuclear factor kappa-B (NFκB) transcriptional activity that decrease macrophage activation and TNF mRNA expression [66] that was claimed in the pathogenesis COVID-19 [67]. The failure of misoprostol to inhibit TNF expression in horses that detected by (Martin, et al. [27]) was limited by their use to single small dose only of oral misoprostol. Misoprostol caused mild dose-dependent reductions in cell number and size in a study performed by (Warkus et al. [68]) on in vitro morphogenesis model using pluripotent P19C5 mouse embryonic carcinoma stem cells. This was opposed by the work of (Pedrosa, et al. [69]) elaborating the safety of misoprostol on gelatin egg cells.
In SARS-CoV-2-infected VERO-E6 cell line, metformin showed a dose-dependent viral inhibition within a narrow therapeutic range due to cytotoxicity. While misoprostol showed little efficacy, that was also limited by the higher cellular cytotoxicity. Benefits of both metformin and misoprostol in SARS-CoV-2 could not be exempted, based on their dose-dependent viral inhibitory potentiality. However, the remarkable dose-dependent cytotoxic activities of both medications associated with enhanced antiviral effects could preclude their use. Further in vitro, employing cell lines, other than the VERO-E6, and in vivo experimental studies are required, especially to elucidate the mechanisms underlying such promising antiviral activity and the factors that caused their sound cytotoxicity in COVID-19, and to evaluate the safety and efficacy of other anti-diabetic and anti-peptic ulcer medications in cases of COVID-19.
We acknowledge Prof. Dr. Soha Aly Elmorsy, Professor of Medical Pharmacology, Faculty of Medicine, Kasr AlAiny, Cairo University, Cairo, Egypt, for performing the regression analysis. She was blinded during statistical analysis regarding the virus and medications we were testing.
The authors declare no conflict of interest.


