Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Takele Achalu Dengela*
Received: July 17, 2023; Published: July 26, 2023
*Corresponding author: Takele Achalu Dengelam, Lecturer at Africa medical , St Lidat Health Science, Addis Ababa medical and business college, Addis Ababa, Ethiopia
DOI: 10.26717/BJSTR.2023.51.008161
Background: Hypertension is a serious global health issue that is linked to morbidity and mortality. It is a prevalent risk factor for cardiovascular disease. One serious cardiovascular illness that frequently affects people with high blood pressure is diabetes mellitus. Cardiovascular problems are four times more common when both of those chronic illnesses are present.
Objective: the Jimma University Medical Center in South-West Ethiopia to look into the prevalence of blood pressure control among hypertension and diabetic hypertensive patients
Methodology: Adult patients with hypertension and diabetic hypertension at Jimma University Medical Center who meet the inclusion criteria were the subjects of a comparative cross-sectional study design. The Statistical Package for Social Science (SPSS) version 22.1 was used to clean, code, and enter the data for analysis. All variables underwent descriptive statistics using frequency distribution.
Results: 100 people were enrolled in the study, and when the data were analyzed, 56% of the hypertension patients were female and 61% of the diabetic hypertensive patients were male, with SDs of +13.87 and +11.4, respectively. Compared to hypertension patients alone, diabetic hypertensive patients had a higher prevalence of blood pressure management. Among diabetic hypertensive patients, 60% of respondents had controlled blood pressure; additionally, 53% of participants had controlled blood pressure among hypertensive patients alone.
Conclusion: Compared to diabetic hypertensive patients, uncontrolled blood pressure was considerably higher in hypertensive patients. Promoting medication compliance and using two antihypertensive medications helped to lessen the effects of insufficient blood pressure management.
Keywords: Hypertension; Blood Pressure Control; Diabetes Mellitus; Jimma University
Abbreviations: DM: Diabetes Mellitus; BP: Blood Pressure; HOT: Hypertension Optimal Treatment; CVD: Cardiovascular Diseases; CD: Chronic Diseases; NHANES: National Health and Nutrition Examination Survey
One of the most important risk factors for cardiovascular illnesses is hypertension (CVDs). It is expected to become the major cause of morbidity and mortality among non-communicable illnesses by 2025, with a projected increase from roughly 1.0 billion in 2000 to 1.5 billion by that time. It accounts for 13% of all fatalities worldwide and is the third cause of disability-adjusted life-years [1]. Significant numbers of people in Sub-Saharan Africa are affected with hypertension, which has demonstrated a rapid rise in prevalence there (SSA). SSA affects between 25.4% and 41.1% of males and between 27.2% and 38.7% of women [2]. Because of the epidemiological shift brought on by the adoption of Western lifestyles, the prevalence of hypertension in SSA has reached epidemic levels. By 2025, 125.5 million adults in SSA are expected to have hypertension, a fourfold rise from 2005 to 2008 in the anticipated prevalence of the disease [3]. The reported prevalence of hypertension in various Ethiopian regions varied significantly. According to estimates, the prevalence in the nation is from 20% to 30% [4]. As the sixth greatest cause of death in Ethiopia for the year, hypertension was responsible for 1.4 percent of all fatalities [1].
More than 70% of diabetic people have hypertension generally, and high blood pressure considerably raises the risk of diabetes complications. Numerous studies have shown the advantages of keeping BP in check in diabetes patients. In the Hypertension Optimal Treatment (HOT) experiment, the impact of reduced diastolic blood pressure on significant cardiovascular events was examined. Despite the well-known advantages of decreasing blood pressure, new statistics show that only 25% of people with diabetes and hypertension have their blood pressure under control [5]. About 70% of all deaths in people with diabetes mellitus (DM) are related to CVD, making DM an independent risk factor for CVD. When DM is newly diagnosed, it is crucial to reevaluate CVD risk factors and regulate blood pressure (BP). Patients who have both hypertension and diabetes mellitus are four times more likely to have CVD than those who don’t have either of these conditions [6]. Hyperinsulinemia, extracellular fluid volume expansion, and increased arterial stiffness have also been suggested as contributory causes for the development of hypertension in diabetics [2], in addition to renal impairment brought on by diabetes. Current guidelines advise that patients with cardiovascular disease and its equivalents should lower their blood pressure to less than 140/90 mmHg in all patients and, provided the treatment is well tolerated, should aim to lower their blood pressure to 130/80 mmHg or less in the majority of patients [7]. Worldwide, hypertension is a significant cause of disease and a common risk factor for CVD. Furthermore, it is the single biggest factor in premature mortality [8]. Despite the availability of numerous potent antihypertensive drugs that have been shown to reduce cardiovascular morbidity and death, hypertension control is still inadequate. Less than 27% and 10%, respectively, of hypertension patients in high- and low-income nations have reached their goal blood pressure. Only 24.6% of patients with hypertension who were receiving therapy had their blood pressure under control in a recent population-based survey in Cameroon [9].
However, it can be challenging to diagnose, treat, and successfully control hypertension, particularly in elderly hypertensive patients. Demographic heterogeneity and the rising prevalence of hypertension by age make this condition one of the main health policy challenges, adding yet another layer of complexity to the public health issue [8]. High rates of hypertension and inadequate hypertension management are significant contributors to the pandemic growth of cardiovascular illnesses in developing nations. Uncontrolled blood pressure is caused by nutritional, genetic, or behavioral factors [1]. However, it is well known that the clinical management of chronic diseases (CD) like hypertension faces a number of challenges, including structural issues like restricted access to appointments, tests, and medications and issues relating to the professionals themselves because, in addition to a shortage of skilled workers, many are also unmotivated and unhappy at work. In addition to these elements, patient-specific problems such low socioeconomic circumstances, cultural influences, and behavioral challenges all hinder the process of adhering to the treatment of CDs. This fact threatens the quality of the care and the aimed, clinical outcome (Blood Pressure control) [10].
The demographic factors linked to uncontrolled BP in DM patients are not well understood. Uncontrolled blood pressure at follow-up was linked to a number of risk factors, including baseline uncontrolled blood pressure, use of oral hypoglycemic medications (as opposed to insulin or diet and exercise), use of three or more antihypertensive medications, and older age, in a retrospective cohort of 1231 patients with diabetes and isolated systolic hypertension. BP control was best among those with diabetes who were examined between 1988 and 1994 as part of the National Health and Nutrition Examination Survey (NHANES III), and it declined with age. Men had better control than women among those 65 and older (46% vs. 28% using 140/90 mmHg as the threshold) [6]. There are a limited number of researches on the BP control status of hypertensive and diabetic hypertensive in Ethiopia. The lack of adequate studies on hypertension significantly affects hypertension management and care of hypertensive patients in the country. Thus, this study aimed to fill such information gaps by assessing BP control status among adult hypertensive and diabetic hypertensive patients at Jimma University medical center (JUMC).
Study Area and Study Period
In JUMC’s ambulatory clinic, the study was carried out between December 1 and December 30, 2020. Over 10 million residents of southwest Ethiopia are served by JUMC, a teaching and tertiary level hospital, for both inpatient and outpatient care. The hospital is located in Jimma City, southwest Ethiopia, 352 kilometers from Addis Ababa, the nation’s capital. The hospital offers inpatient care in six clinical divisions, including internal medicine, surgery, gynecology and obstetrics, pediatrics, psychiatry, and ophthalmology, as well as outpatient care in the chronic illness follow-up clinics, including those for diabetes, hypertension, cardiovascular disease, asthma, epilepsy, tuberculosis, HIV, and psychiatry, as well as other outpatient services like dermatology and dentistry.
Study Design
A comparative cross-sectional study was conducted among hypertensive and diabetic hypertensive patients in JUMC.
Population
Source Population: All adult patients with hypertension and diabetic hypertension attending JUMC
Study Population: All adult hypertensive and diabetic hypertensive patients who has followed up at JUMC during the study period and who fulfill the inclusion criteria.
Sample Size and Sampling Technique
The sample size was estimated by using two proportion formula of Zα/2 is confidence level of 95%, α is 0.05 and the critical value is 1.96, Zβ is a power of 80%, β is 0.2 and the critical value is 0.84 and p1 and p2 are the expected sample proportions of the two groups. So, p1 is 50.3%, according to a study done in Jimma University specialized hospital [1] and p2 is 43.51%, according to a study done in JUMC [2]. The sample size for the study was determined by using the following formula
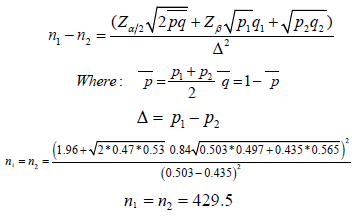
Therefore, the sample size based on the above formula results is 430subjects in each group and convenience sampling technique was used for data collection.
Inclusion and Exclusion Criteria
Inclusion Criteria: All hypertensive and diabetic hypertensive patients age ≥18 years.
Exclusion Criteria:
a. Those patient having comorbidity other than either hypertension
or diabetes
b. Those patients refuse of participating on the study.
Study Variables
Dependent Variables: Blood pressure Control
Independent Variables:
a. Patient related factors: Age, Gender, Ethnicity, Educational
level, Marital status, Occupation, Religion
b. Diseases related factors: Duration of disease diagnosed,
Family history, Blood pressure level, Blood glucose level.
c. Behavioral related factors: Adherence, Physical activity,
Smoking habit, Khat chewing Drug/therapy related factors.
d. Drug related: Antihypertensive drug regimen, Antiglycemic
drug regimen, Concomitant drug therapy, Duration of drug therapy.
Data Collection Instrument and Procedure
Data Collection Instrument: Face-to-face interviews and chart reviews were used to collect data using a semi-structured questionnaire that was derived from several academic works. The questionnaire was pre-tested on 5% of the sample in JUMC and was developed based on the study goals. The survey asks questions about socio demographics, behavior, clinical conditions, and drug use. For the examination of the chart and the in-person interview, check lists were employed. Data on clinical and drug-related factors were gathered using a chart review checklist. To gather information on socio-demographic and behaviorally relevant characteristics, an interview checklist was used. For documenting laboratory data such as blood pressure and fasting blood glucose of the previous three consecutive tests, an observational checklist was used.
Data Collection Procedures: The patients were informed prior to data collection regarding the objective of the study. Interview and review of the patient’s chart was conducted by principal investigator using interview for demographic, behavioral factors and review for the patient’s clinical and drug related factors.
Data Quality Assurance
The following actions were made to ensure data quality: The data collection tools were pre-tested on 5% of the sample at JUMC, and adjustments were made as needed in light of the pre-findings. test’s The final report did not contain the pre-tested examples. Data was coded, cleaned, and verified before being entered into SPSS.
Data Analysis and Interpretation
The Statistical Package for Social Science (SPSS) version 22.1 was used to clean, code, and enter the data for analysis. For socio-demographic, behavioral, clinical, and drug-related variables, descriptive statistics based on frequency distribution were used.
Ethical Consideration
The Jimma University Ethics Review Committee gave its approval for the study’s ethical conduct. After receiving authorization from the hospital, data collection was initiated and a letter was sent to JUMC. Throughout the whole study period, participants gave their written, informed consent in the local language before being interviewed. Records were stored in a locked cabinet and data gathered during the study was handled as confidential information. The patients’ decision to decline the interview or not take part was respected.
A total of 200 study participants were included in data analysis; 100 study participants form hypertensive patients and 100 study participants from diabetic hypertensive patients.
Socio-Demographic Characteristics
Out of 100 study participants, 56% of the hypertension and diabetic hypertensive patients were female and 61% were male. Participants in the study who had hypertension or diabetes-related hypertension ranged in age from 46 to 61 years old in 47% of cases and between 46 and 60 years in 43% of cases. Nearly and more than half of the study subjects, or 56% and 63% of hypertension and diabetic hypertensive patients, respectively, were of Oromo ethnicity. Among the participants, 44% of the hypertension patients had no formal education, while 48% of the diabetic hypertensive patients had completed first grade (Table 1).
Table 1: Socio-demographic characteristic of study respondents among hypertensive and diabetic hypertensive patients in JUMC ambulatory clinic from December 01 to December 30, 2020.

Table 2: Behavioral characteristic of study participants among hypertensive and diabetic hypertensive patients in JUMC ambulatory clinic from December 01 to December 30, 2020.

Behavioral Characteristics of Study Participants
20% of the participants in the study had smoked cigarettes in the past, but none of them were now smoking cigarettes in the hypertension group, but in the diabetic hypertensive group, 30% had smoked cigarettes in the past and two (6.7%) were still smoking cigarettes today. 4 (10.8%) of the study participants who had previously chewed khat were currently doing so among hypertension groups, while 6 (13.6%) of the study participants who had previously chewed khat were currently doing so among the diabetic hypertensive group. Around 13% and 16% were had previous history of alcohol consumption between both groups respectively, of these 1(7.7%) and 2(12.5%) were currently drink alcohol respectively, with frequency of 1-2 days per week. More than half 67% and 80%, were physical inactive among both group respectively (Table 2). Most of the study participants 76% and 79% were having good adherence among hypertensive diabetic hypertensive groups respectively (Figure 1).
Clinical and Drug Related Characteristics Among Hypertensive Patients
18% of the study’s participants had a history of hypertension in their families. 44% of people had hypertension for at least five years. 70% of them had stage II hypertension when they were diagnosed. 54% of the participants, or more than half, had follow-up visits every month. 18% of them, or one-third of the group, were using a combination of the diuretic Thiazide and the calcium channel blocker Thiazide. 60% of people avoided taking a medication concurrently (Table 3).
Table 3: Clinical and drug related characteristic of study participants among hypertensive patients in JUMC ambulatory clinic from December01 to December 30, 2020.

Clinical and Drug Related Characteristics Among Diabetic Hypertensive Patients
20% of the individuals in the study had a history of diabetes, and 18% had a history of hypertension. The majority of them, 47% and 43%, respectively, had diabetes and hypertension for less than 5 years. A 67% glycemic control score was subpar. 64% of the participants, or more than half, had follow-up visits every month. The majority of them, 66% were using ACEIs alone from antihypertensive drugs, while 46% were receiving aspirin plus statins as a concomitant medication. 42% were taking metformin with glibenclamide, and 23% were taking metformin alone from antiglycemic medicines (Table 4).
Table 4: Clinical and drug related characteristic of study participants among diabetic hypertensive patients in JUMC ambulatory clinic from December 01 to December 30, 2020.

Prevalence of Blood Pressure Control
Compared to hypertension patients, diabetic hypertensive patients were more likely to have good blood pressure control. In the diabetic hypertensive groups, 60% of the study participants had controlled blood pressure, while 26% had increased SBP or DBP. In the hypertensive groups, 53% had controlled blood pressure, while 27% had increased SBP or DBP. In general, 40% of diabetic hypertensive patients and 47% of hypertension patients had insufficient blood pressure control (Figure 2).
Individuals with hypertension and diabetes mellitus have a four times higher risk of developing cardiovascular disease (CVD) than patients with either condition alone. Poor blood pressure management can raise the risk of stroke, myocardial infarction, and other cardiovascular diseases. Among diabetic hypertensive patients, blood pressure control was more common (60% vs. 53%, respectively) than among hypertensive patients alone. The prevalence of increased SBP or DBP was marginally greater (27% vs 26%, respectively) in hypertensive patients than in diabetic hypertensive patients. In patients with diabetes and hypertension, blood pressure control was 60% common. Our results were better than those of a research from Boston and Veterans Affairs, where patients with diabetes and hypertension were more likely to regulate their blood pressure at 40% and 59.5%, respectively [5,6]. The target achieved blood control was 27% vs 10% between high income vs low income correspondingly, which might be explained by the large difference in sample size (i.e., in our study the sample size is very low) and the change in study environment (i.e., high income vs low income) [9].
In our study, 47% of patients with hypertension had insufficient blood pressure control. Our results were higher than those of studies conducted in Brazil and Bahrain, where the prevalence of low blood pressure was found to be 44.89% and 33.7%, respectively [11,12]. This discrepancy may be caused by the study environment (i.e. variation of quality of health care providers). This result was consistent with an Azerbaijani study in which 55.1% of individuals had insufficient blood pressure control [8]. In our study, 53% of the hypertension individuals had blood pressure control. Our results were greater than those of a research from Cameroon, where 36.7% of respondents had their blood pressure under control. Different healthcare professionals could be the cause of the variation. This result was very similar to that of the JUSH trial, where blood pressure control was 50.3% prevalent [1]. We discovered that diabetic hypertensive and hypertension individuals had blood pressure control rates of 60% and 53%, respectively. This demonstrates that in our study, more than half (79% and 77%, respectively) of the individuals took their prescriptions as prescribed [13-19].
Our research indicates that people with hypertension who were not also diabetic had worse blood pressure control. 40% of hypertension patients and 47% of hypertensive alone had poor blood pressure control. According on our study’s findings, I would advise the Jimma University Medical Center to: Encourage patients to take their medications as directed to lower the likelihood of non-adherence, Implement the use of dual antihypertensive medications for individuals with comorbidities like diabetes to lower the risk of complications from CVD brought on by inadequate blood pressure management.


