Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Reem Dimachkie1*, Zakaria Alameddine1, Ahmad Mustafa1, Fouad Sakr1, Lina Dimachkie2 and Suzanne El Sayegh1
Received: July 06, 2023; Published: July 17, 2023
*Corresponding author: Reem Dimachkie, Internal medicine department, Staten Island University Hospital, Staten Island, 475 Seaview avenue, 10305 New York, USA
DOI: 10.26717/BJSTR.2023.51.008120
Introduction: Liver cirrhosis is associated with higher mortality and morbidity due to the resulting portal hypertension and hepatocellular insufficiency. However, it is also well known that patients with liver cirrhosis are at increased risk for serious infections. Febrile neutropenia is defined as fever in a patient with an absolute neutrophil count <1500 cells/microliter. The impact of liver cirrhosis on febrile neutropenia in not well studied. The aim of this study is to highlight the outcome of febrile neutropenia in cirrhotic patients.
Methods: National Inpatient Sample (NIS) Database 2016-2018 was used to sample individuals presenting with febrile neutropenia, and baseline demographics and comorbidities were collected using ICD-10-DM codes. Patients with missing data were excluded. Individuals were stratified into two cohorts based on the presence or absence of liver cirrhosis. Logistic regression analysis was performed to analyze the outcomes between the two groups.
Results: Out of 116,142 patients admitted with febrile neutropenia, 1418 had cirrhosis. On logistic regression analysis, cirrhotic patients had higher mortality (adjusted OR: 1.3 [1.1-1.6]; p=0.013), gastrointestinal bleed (adjusted OR: 3.8 [3.2-4.6]; p<0.001), sepsis (adjusted OR: 1.2 [1.02-1.40]; p=0.02) and acute renal failure (adjusted OR: 1.4 [1.2-1.6]; p<0.001).
Discussion: This study highlights that the presence of liver cirrhosis in patients with febrile neutropenia was associated with higher mortality, gastrointestinal bleed, sepsis, and renal failure. Thus, special care should be taken when managing patients with febrile neutropenia with an underlying diagnosis of cirrhosis. Further studies are needed to establish management strategies for this vulnerable population.
Abbreviations: AKI: Acute Kidney Injury; SBP: Spontaneous Bacterial Peritonitis; HVPG: Hepatic Venous Pressure Gradient; ANC: Absolute Neutrophilic Count; NIS: National Inpatient Sample; OR: Odds Ratio; HI: Hematologic Indices; SIRS: Systemic Inflammatory Response Syndrome; CI: Confidence Intervals
Infections, specifically bacterial infections, are diagnosed in 30% to 50% of all hospital admissions in cirrhotic patients [1]. The culprit for most bacterial infections in cirrhosis is an interplay of gut microbiota, intestinal permeability, and bacterial translocation [2]. Along with increasing morbidity, bacterial infections can also precipitate cirrhosis decompensation (hepatic encephalopathy, ascites, variceal bleeding, and/or jaundice) and can cause acute kidney injury (AKI). Clinical factors associated with an increased risk of infection are poor liver function, variceal bleeding, low ascitic fluid protein levels, prior spontaneous bacterial peritonitis (SBP), and hospitalization [2,3]. On the other hand, leukocytopenia, especially neutropenia, is often found in advanced chronic liver disease [4]. The main mechanisms of leukocytopenia are splenic sequestration of leukocytes due to hypersplenism, presence of serum hematopoietic progenitor inhibitory factors, and a shortened neutrophil lifespan caused by increased apoptosis [5]. Moreover, studies found that baseline thrombocytopenia and leukopenia were predictors of death or transplant, after adjusting for baseline hepatic venous pressure gradient (HVPG), and Child-Pugh scores [6]. Interestingly, febrile neutropenia which is defined as a single oral temperature greater than or equal to 101 F (38.3 C) or a temperature greater than or equal to 100.4 F (38 C) for at least an hour, with an absolute neutrophilic count (ANC) of less than 1500 cells/microliter has not been studied previously in cirrhotic patients. Neutropenic fever is the most common and serious complication associated with hematopoietic cancers or with patients receiving chemotherapeutic regimens for cancer [7]. Thus we conducted this study to better understand the outcomes of febrile neutropenia in patients with underlying liver cirrhosis versus patients without cirrhosis.
The National Inpatient Sample (NIS) database from the years 2016 to 2018 was utilized for this study. The study population consisted of individuals who presented with febrile neutropenia. Febrile neutropenia was identified using appropriate diagnostic codes (ICD- 10-DM codes) within the NIS database. Baseline demographic characteristics and comorbidities were collected for each patient using the respective ICD-10-DM codes. Patients with missing data regarding baseline demographics or comorbidities were excluded from the analysis. Based on the presence or absence of liver cirrhosis, patients were stratified into two cohorts: the liver cirrhosis cohort and the non-cirrhosis cohort. The presence of liver cirrhosis was determined using the relevant ICD-10-DM codes within the collected data. Logistic regression analysis was performed to compare the outcomes between the two cohorts. Descriptive statistics were used to summarize the baseline demographics and comorbidities of the study population. Logistic regression models were employed to calculate odds ratios (OR) and corresponding 95% confidence intervals (CI) for the outcomes of interest, comparing the liver cirrhosis cohort to the non-cirrhosis cohort. Adjustments for potential confounding factors, such as age, gender, and comorbidities, were considered in the regression models.
The study included a total of 116,142 patients who were admitted with febrile neutropenia. Among these patients, 1,418 individuals had a coexisting cirrhosis. The baseline characteristics and outcomes of the patients, and their findings are summarized in (Table 1). Based on the results provided, it was observed that cirrhotic patients had worse outcomes compared to non-cirrhotic patients. The adjusted odds ratio (OR) for mortality was 1.3, with a 95% confidence interval of 1.1 to 1.6 (p-value 0.013). Additionally, cirrhotic patients were found to have a higher risk of experiencing gastrointestinal bleed. The adjusted odds ratio for gastrointestinal bleed was 3.8, with a 95% confidence interval of 3.2 to 4.6 (p-value 0.001). Cirrhotic patients also had a higher likelihood of developing sepsis. The adjusted odds ratio for sepsis was 1.2, with a 95% confidence interval of 1.02 to 1.40 (p-value 0.02). Cirrhotic patients also had an increased risk of acute renal failure. The adjusted odds ratio for acute renal failure was 1.4, with a 95% confidence interval of 1.2 to 1.6 (p-value 0.001).
Table 1: Comparison of Clinical Characteristics and Outcomes of Febrile Neutropenia between Patients with and without Cirrhosis.
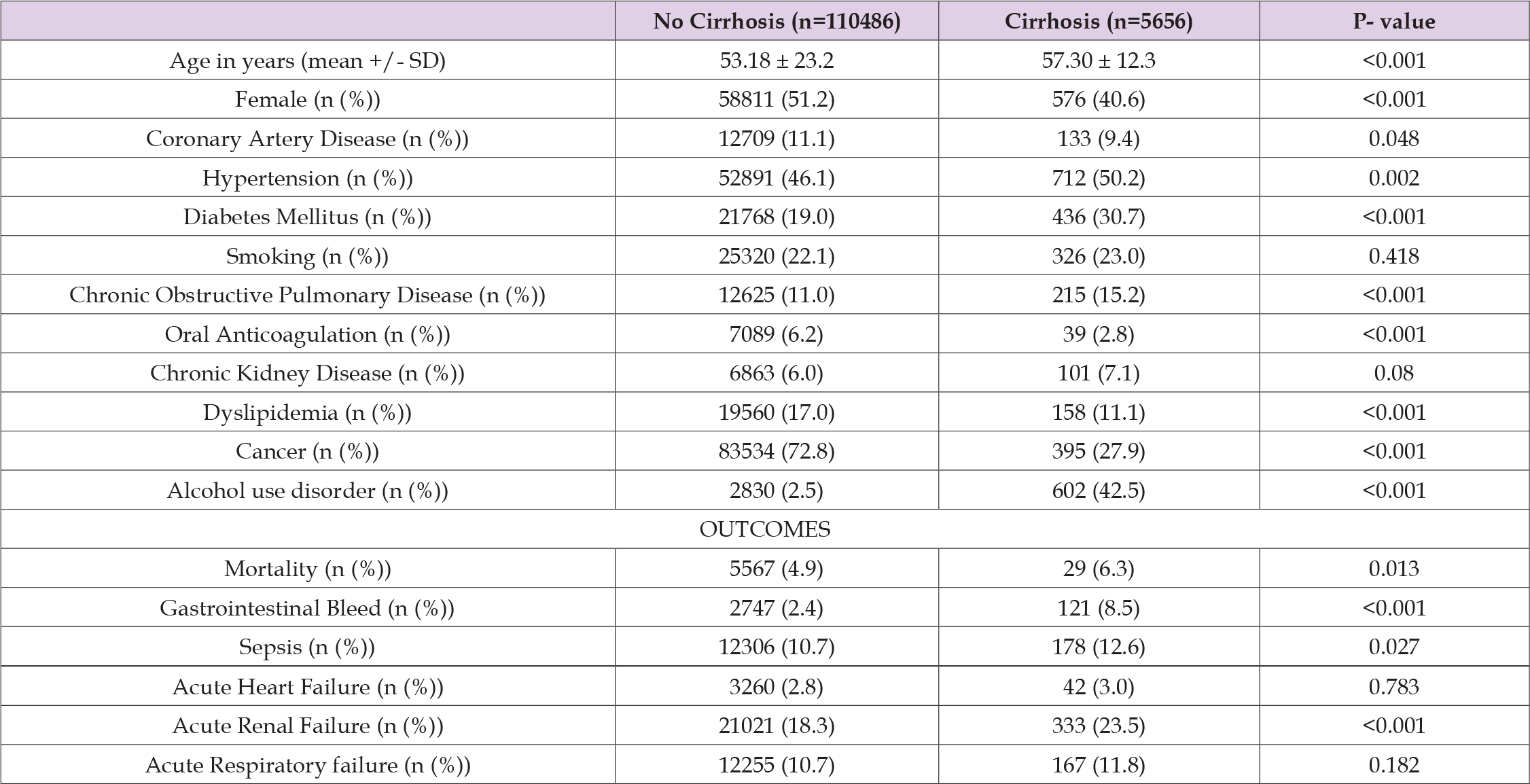
Note: SD: Standard Deviation, n: Number of Patients, %: Percentage
The findings of this study shed light on the association between liver cirrhosis and the outcomes of patients with febrile neutropenia. The study suggests that when patients with febrile neutropenia also have liver cirrhosis, they face a higher risk of mortality and complications such as gastrointestinal bleed, sepsis, and renal failure. The compromised immune response in patients with both febrile neutropenia and cirrhosis increases their susceptibility to sepsis, contributing to the higher mortality rates observed in this population. Abnormal hematologic indices (HI), defined as either anemia, thrombocytopenia, leukopenia, or any combination, are frequently encountered in patients with liver cirrhosis, with thrombocytopenia being the most common [8]. Qamar, et al. [7] reported that hematologic abnormalities were found in 84 % of cirrhotic patients, with leukopenia accounting for 42% in these patients [6]. Even though leukopenia is not considered a normal response to infection, both leukopenia and leukocytosis are essential components of systemic inflammatory response syndrome (SIRS). In one study, Belok, et al. [8] found that leukopenia was associated with increased in-hospital mortality compared with leukocytosis [9]. In another cohort done by Qamar, et al. [7] evaluating 213 cirrhotic patients, baseline leukopenia was found to be significantly associated with mortality and liver transplantation [6]. Mortality was mostly infection-related; hence, leukopenia was suggested to be associated with a higher risk of infection.
Interestingly, although liver related mortality was increased, it did not reach statistical significance, but it is worth mentioning that the data related to some markers of morbidity such as gastrointestinal bleeding and spontaneous bacterial peritonitis, were not collected [6]. Cirrhotic patients are known to be at higher risk of infections due to their immunocompromised state. Infections in this subgroup of patients is associated with significantly increased mortality [10,11]. This could be explained by the fact that liver cirrhosis is a chronic dysregulated inflammatory state. Even though neutropenia and infections have been studied in cirrhotic patients, there have been scarce data regarding febrile neutropenia in this subgroup of patients. Febrile neutropenia is studied extensively in patients with hematologic malignancies and was found to be associated with higher morbidity and mortality [12]. Striki, et al. [12] analyzed data of 275 chronic hepatitis C patients with compensated liver disease who underwent treatment with PegIFNa and ribavirin where it was found that neutropenia was not associated with bacterial infections and that the presence of cirrhosis was associated with a higher risk of infection during antiviral treatment [13]. The limitations of this study stem from its reliance on the NIS population, which include potential sampling bias, data accuracy issues, missing data, inability to establish causality, and lack of detailed clinical information. Also, the reliance on ICD-10 codes for identifying patient diagnoses may lead to potential coding errors. Despite these limitations, our study has several strengths. We utilized a nationwide database that is representative of the general US population and matched for important covariates that may have confounded our results.
This study implies that the current understanding and approaches to managing febrile neutropenia may not be sufficient for patients with underlying liver cirrhosis. More studies are necessary to identify specific interventions, guidelines, and treatment modifications that can optimize the care and outcomes for these patients. It highlights the need for a multidisciplinary approach involving oncologists, hepatologists, infectious disease specialists, and other healthcare professionals to optimize the management and outcomes of these patients.


