Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Trifon Valkov1, George Dimitrov2 and Radka Argirova3*
Received: July 05, 2023; Published: July 12, 2023
*Corresponding author: Argirova, Department of Clinical Laboratory, Acibadem City Clinic Tokuda Hospital, 1407 Sofia, Bulgaria
DOI: 10.26717/BJSTR.2023.51.008110
Objective: This retrospective study aimed to examine the outcomes of cohorts of patients who had
uncomplicated type II diabetes mellitus as their only documented chronic condition. We compared fully
vaccinated and non-vaccinated populations within different sex and age groups, considering their clinical
outcomes.
Design: From March 2020 to June 2022, an extensive retrospective analysis was carried out using national
patient data obtained from the database of the Ministry of Health of the Republic of Bulgaria, following a
formal written request. The study encompassed a total of 1,126,946 confirmed COVID-19 patients.
Results: Among the 1,126,946 confirmed COVID-19 patients included in this study, 0.33% (n=3,792) had
type II diabetes mellitus as their sole chronic condition. Statistical analysis revealed significant findings
in favor of the vaccinated cohorts, demonstrating reduced rates of hospitalizations [0.76 (95% CI 0.6550
to 0.9001); p=0.0011], ICU admissions [OR=0.38 (95% CI 0.2698 to 0.5282); p < 0.0001], in-hospital
mortality [0.20 (95% CI 0.1126 to 0.3552); p<0.0001], and ICU-related mortality [0.25 (95% CI 0.0789 to
0.7860; p=0.0178]. Furthermore, the vaccinated cohort exhibited lower hospitalization rates specifically
during the alpha wave of the pandemic. Statistically significant reductions in mortality rates were observed
in the vaccinated cohorts during the beta [OR=0.01 (95% CI 0.0008 to 0.2085); p=0.0022], delta [OR=0.42
(95% CI 0.2636 to 0.6842); p=0.0004], and omicron [OR=0.20 (95% CI 0.1321 to 0.3132); p < 0.0001]
waves. Additionally, within the vaccinated cohorts, those who received mRNA-based vaccines experienced
higher and more significant reduction rates compared to those who received viral-vector-based vaccines.
Conclusion: This retrospective analysis highlights a consistent pattern among patients with uncomplicated
type II diabetes mellitus as the sole chronic condition who have received COVID-19 vaccination. Notably,
vaccinated individuals hav
Keywords: COVID-19 Vaccination; Chronic Diseases; Type II Diabetes Mellitus Without Complications; Mortality Rates
Diabetes mellitus is a chronic metabolic disorder that arises from inadequate insulin production or utilization, leading to elevated blood glucose levels. Even before the emergence of the SARSCoV- 2 pandemic, the morbidity and mortality rates associated with chronic conditions like diabetes have presented significant challenges. Moreover, these chronic conditions have been found to heighten the susceptibility to severe cases of COVID-19 [1]. In light of these circumstances, it is of utmost importance to prioritize and enhance vaccination rates as a means of mitigating the potential for increased premature mortality associated with COVID-19. This is particularly critical for high-risk populations, including individuals with diabetes. By ensuring a higher proportion of the population receives vaccination, the aim is to minimize the adverse outcomes and protect vulnerable groups from the severe consequences of COVID-19. The effectiveness and safety of vaccines have been widely reported by numerous international and local sources. The most recent data consistently demonstrates the substantial advantages of vaccination, particularly among patients with chronic comorbidities [2,3]. Extensive research has established that individuals with type II diabetes mellitus (DM), particularly those with poorly controlled blood glucose levels, face an elevated risk of experiencing severe illness and increased mortality due to COVID-19. This heightened susceptibility is attributed to the higher prevalence of cardiovascular disease and compromised immune function associated with DM [4].
Previous studies have indeed highlighted the concern that patients with this chronic condition may experience a compromised immune response, leading to reduced effectiveness of SARS-CoV-2 vaccines [5,6]. Additionally, individuals with this condition have been found to have an elevated risk of developing opportunistic infections [7]. These factors further underscore the importance of addressing the specific challenges faced by patients with this chronic condition in the context of COVID-19 vaccination efforts. The existing body of research regarding the impact of COVID-19 vaccination on outcomes such as supplemental oxygen requirement, ICU admissions, and mortality in patient cohorts specifically characterized by uncomplicated type II diabetes mellitus (DM) as the sole chronic condition remains limited. Consequently, our study sought to explore the potential associations between these parameters and COVID-19 vaccination status in this particular patient population. By addressing this research gap, we aim to contribute to a better understanding of the effects of vaccination in individuals with uncomplicated type II diabetes mellitus and its potential implications for their clinical outcomes.
Patient Cohort Criteria
This retrospective study utilized an initial cohort consisting of 1,126,946 individuals who were confirmed to have SARS-CoV-2 infection. The confirmation process involved real-time polymerase chain reaction (PCR) testing for 612,378 individuals, while antigen testing was employed for 436,196 individuals. Among the cohort, 47% (486,182) were male, and 53% (562,393) were female. Patient data was obtained from the Ministry of Health of the Republic of Bulgaria via the “United Information Portal” following a formal written request. The primary focus of our study was to analyze the outcomes of COVID-19 in two specific groups: fully vaccinated and non-vaccinated Bulgarian patients who had type II diabetes mellitus as their sole chronic condition. Notably, patients with documented macro/ microvascular or immunodeficient complications were excluded from the study. The process of patient selection and categorization by age groups is illustrated in Figure 1. In addition to the main analysis, we collected additional data by subgrouping the vaccinated cohort based on gender and the specific type of vaccine received, which included BNT162b2 (Comirnaty), CX-024414 (Spikevax), ChAdOx1- SARS-CoV-2 (Vaxzevria), and Ad26.COV2-S (Janssen COVID-19 vaccine), all of which are currently available in Bulgaria.
Note: ICU, Intensive care unit.
Statistical Analysis
The statistical analysis was performed using SPSS version 26.0 (SPSS, Chicago, IL, USA) and GraphPad Prism 6 (GraphPad, La Jolla, CA, USA). Associations between variables were assessed using the Pearson’s Chi-Square test. Correlations between variables were evaluated using the Pearson’s correlation coefficient. The Cox regression model was utilized to determine odds ratios (OR) between the vaccinated and non-vaccinated groups. Univariate logistic regression analyses were conducted to estimate the odds ratio of different events among patients with type II DM and identify potential risk factors associated with COVID-19-related mortality in this patient population. A p-value of ≤0.05 was considered statistically significant, a p-value of ≤0.01 was considered highly statistically significant, and a p-value of ≤0.001 was considered very highly statistically significant.
Patient and Public Involvement:
The research question and outcome measures of this study were formulated without patient involvement, and patients were not directly involved in the design or implementation of the study. The results of the research will not be disseminated directly to study participants or the relevant patient cohorts.
Among the 1,126,946 confirmed SARS-CoV-2 infected patients, 0.33% (n=3,792) had diabetes mellitus as the sole comorbidity, with a median age of 48. Out of the 247,441 hospitalized COVID-19 cases requiring supplemental oxygen therapy, 0.56% (n=1,382) had DM, with a median age of 64 years (Table 1). Within the hospitalized cohort, the majority of patients requiring supplemental oxygen were unvaccinated diabetic women aged between 60 and 69, totaling 240 patients. The highest mortality rates were observed in both unvaccinated diabetic men and women aged between 70 and 79, with 88 deaths in each group (Figure 2). The unadjusted univariate analysis showed statistically significant reductions in hospitalizations [0.76 (0.6550 to 0.9001); p=0.0011], ICU admissions [OR=0.38 (95% CI 0.2698 to 0.5282); p < 0.0001], in-hospital mortality [0.20 (0.1126 to 0.3552); p<0.0001], and ICU-related mortality [0.25 (0.0789 to 0.7860); p=0.0178] in favor of the vaccinated cohorts (Figure 3). For a more comprehensive analysis, we examined the mortality rates within the vaccinated cohorts based on the type of vaccine administered. Among the studied cohort, 75.4% (534 out of 708) received an mRNA- based vaccine (i.e., BNT162b2 or CX-024414), while the remaining 174 individuals were vaccinated with a viral vector-based vaccine (i.e., ChAdOx1-SARS-CoV-2 or Ad26.COV2-S). Only the mRNA-based vaccinated group showed a statistically significant reduction in hospital admissions [0.77 (0.6387 to 0.9270); p=0.005].
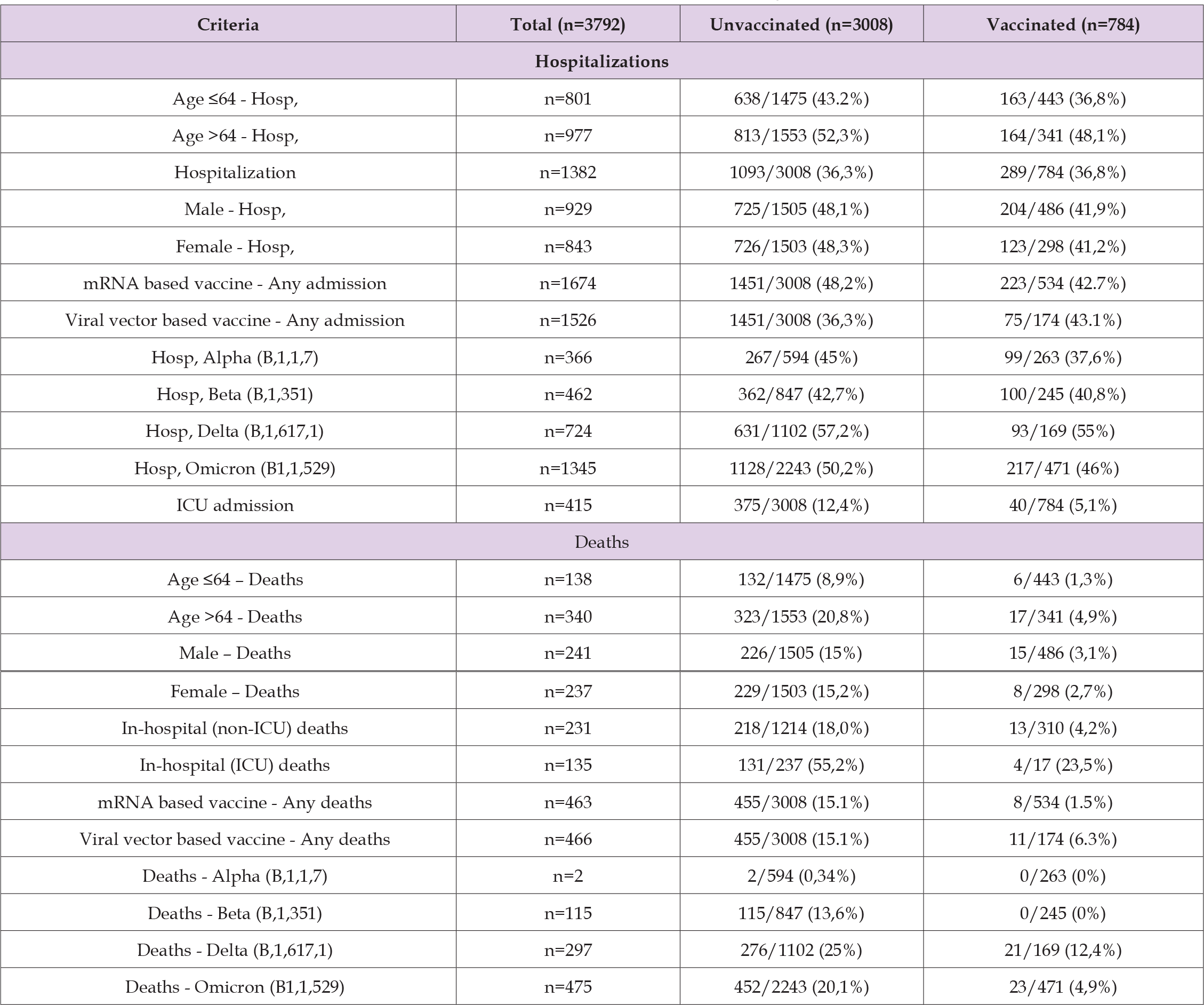
Table 1: Distribution of Patients with Type II Diabetes as their Sole Chronic Condition, categorized by Vaccination Status and Outcome.
Both the mRNA-based [0.08 (0.0422 to 0.1728); p<0.0001] and vector-based [0.38 (0.2040 to 0.7030); p=0.0021] cohorts demonstrated reduced mortality rates (Figure 3). To assess the impact of different SARS-CoV-2 variants of concern (VOC) on COVID-19 outcomes, we analyzed data during the corresponding time periods of each circulating VOC. The vaccinated cohort showed reduced hospitalization rates (non-ICU) specifically during the alpha wave of the pandemic [0.74 (0.5492 to 0.9952); p=0.0464] (Figure 3). Furthermore, statistically significant reductions in mortality rates were observed in the vaccinated cohorts during the beta [OR=0.01 (95%CI 0.0008 to 0.2085); p=0.0022], delta [OR=0.42 (95%CI 0.2636 to 0.6842); p=0.0004], and omicron [OR=0.20 (95%CI 0.1321 to 0.3132); p<0.0001] waves (Figure 3).
Note: OR , odds ratio; ICU, intensive care unit; Hosp, hospitalization.
Numerous studies have shed light on the significant association between COVID-19 and diabetes mellitus (DM), revealing the challenges faced by individuals managing diabetes during the pandemic. The impact of this correlation is multifaceted, encompassing an increased susceptibility to severe illness and the complexities of glycemic control. People with diabetes who contract COVID-19 face heightened vulnerability due to the virus’s utilization of the ACE2 receptor, which plays a crucial role in insulin signal transduction. Consequently, these individuals experience decreased insulin sensitivity and compromised glycemic control [8]. The heightened risk of developing diabetic ketoacidosis further amplifies the potential for severe illness, hospitalizations, and mortality [9,10]. Such adverse outcomes not only impose substantial burdens on healthcare systems but also incur elevated healthcare costs. Additionally, the elevated risk of severe illness has taken a toll on the mental well-being of individuals with DM and their families, leading to increased anxiety and stress. While individuals with diabetes who have additional comorbidities or poor glycemic control are known to be at a higher risk of severe illness and complications from COVID-19, even those with uncomplicated, controlled, diabetes may still face an elevated risk compared to individuals without the condition. The impact of COVID-19 on individuals with diabetes appears to vary across different waves of the pandemic. This variation likely stems from changes in the virulence and pathogenicity of SARS-CoV-2 variants over time, as well as fluctuations in healthcare resources and accessibility [11].
Furthermore, our data highlights that vaccination does not provide complete protection against hospitalization, as evidenced by the documented outcomes during periods of dominance by different variants of concern (VOC).
Despite vaccination efforts, a subset of vaccinated individuals still experienced hospitalization due to COVID-19. This finding underscores the need for continued vigilance and adherence to preventive measures, even among vaccinated individuals, in order to minimize the risk of severe illness and hospitalization. This study has several limitations that should be acknowledged. Firstly, the study design does not allow for a direct assessment of vaccine efficacy, as it is based on observed trends between vaccinated and non-vaccinated cohorts. Secondly, the study does not include an analysis of fasting glucose levels or HbA1c values, which could provide additional insights into the relationship between glycemic control and COVID-19 outcomes. Lastly, while efforts were made to account for relevant variables through statistical analysis, there is still a possibility of unmeasured or residual confounding that could have influenced the observed associations due to the lack of propensity score matching. Despite these limitations, the findings of this study provide valuable insights into the impact of COVID-19 on individuals with uncomplicated DM and emphasize the need for further research to better understand the relationship between the chronic condition, COVID-19 outcomes, and vaccination. The dynamic nature of the SARS-CoV-2 virus and the continuously evolving COVID-19 pandemic pose significant challenges in conducting prospective studies to comprehensively examine the impact of the disease on patients with cancer.
The constant viral evolution, emergence of new variants, and rapidly changing epidemiological situation make it difficult to design and implement studies in real time. The need to adapt research protocols and data collection strategies to address the evolving landscape adds complexity to the study design and implementation. The COVID-19 pandemic has significantly disrupted routine diabetes care, causing challenges in accessing regular check-ups, monitoring, and necessary medications and supplies. However, amidst these disruptions, there have been positive changes in diabetes management that emerged during the pandemic. One such change is the increased utilization of telehealth and virtual consultations, which have provided a valuable alternative for individuals with diabetes to receive medical advice and support remotely. These advancements in remote healthcare delivery have improved access to care, particularly for those who may face barriers in attending in-person appointments. The use of telehealth has allowed for ongoing monitoring, education, and medication management, empowering individuals with diabetes to stay connected with healthcare providers and maintain better control of their condition. These positive changes in diabetes management during the pandemic highlight the potential benefits of incorporating telehealth and virtual care into routine diabetes care beyond the pandemic period [12,13].
The COVID-19 pandemic highlights the importance of maintaining glycemic control, promoting vaccination, and ensuring healthcare access for individuals with diabetes. Vaccination plays a critical role in protecting such individuals from severe illness and complications caused by SARS-CoV-2.
Approval for this retrospective analysis was obtained from the Bulgarian Ministry of Health, under document number 94-4750 dated 09.11.2022.
All authors contributed equally in the production of this manuscript.
This research was carried out without external funding.
No conflict of interest to declare.

