Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Sumayah Askandarani¹, Khadija M. Alshehabi²*, Ali Alshaqaq¹, Tofol Al-Nashmi¹, Khalid Bel’eed- Akkari¹, Meteb Al-Bugami¹, Abdulaziz S. Alghamdi1, Muna Alshehabi3
Received: May 09, 2023; Published: May 16, 2023
*Corresponding author: Khadija M Alshehabi, Nephrology, Salmaniya Medical Complex, Government Hospitals, Manama, Bahrain
DOI: 10.26717/BJSTR.2023.50.007952
Chronic kidney disease (CKD) has grown to be a global and public health concern due to the increasing number of patients receiving renal services and its economic burden on the healthcare system in terms of increased healthcare costs. CKD also is associated with unfavorable outcomes and raised morbidity and mortality rates. Worldwide, the prevalence of CKD is high due to the increased prevalence of chronic non-communicable diseases such as diabetes and hypertension. Unfortunately, the CKD prevalence is not well studied in Arab countries due to a lack of epidemiological databases. Based on the available data, multiple organizations recommended starting CKD screening programs for high-risk group populations in countries with a high burden of CKD and End Stage Kidney Disease (ESKD). However, challenges may stand against the effective implementation of CKD screening programs in certain countries, especially with low-middle income, which are related to the limitations of the resources including the costs and manpower. Nonetheless, outweighing the costs of these screening programs over the costs of the management of advanced CKD including the different modalities of Renal Replacement Therapy (RRT) is very essential. The Ministry of Health in the Kingdom of Saudi Arabia has recently transformed the healthcare system to provide an integrated network of healthcare services covering all the regions of the kingdom. Therefore, we are proposing a pathway to integrate primary healthcare in CKD screening and management of the early stages of the disease in order to improve patient care and quality of renal services and enhance the smooth transition to secondary hospitals with the ultimate goal of reducing the costs, decreasing morbidity and mortality rate and obtaining favorable results in the long-term.
Chronic kidney disease (CKD) is one of the worldwide major health problems that is rapidly approaching epidemic proportions. At least 2.4 million deaths per year are caused by CKD and around 850 million people worldwide have chronic kidney disease (World health organization, 2017) [1]. The prevalence of chronic diseases is rising in most countries due to human longevity which is negatively affecting the healthcare systems in the form of increased demands and costs. The estimated prevalence of CKD worldwide is 11-13% (Hill N 2016 [2]). Unfortunately, the CKD prevalence is unknown in Arabic counties including Saudi Arabia due to a lack of epidemiological data (Faraj Y [3]). However, according to a pilot study done by (SEEK-Saudi Investigators), the prevalence of CKD in the young Saudi population was around 5.7% (Alsuwaida [4]). In addition, a recent study by Mousa, et al. [5] assessed 5177 relatives from 4500 dialysis patients to determine the prevalence of undiagnosed CKD among first-degree relatives of Saudi hemodialysis patients and it showed a prevalence of 13.8% (Mousa, et al. [5]). Chronic kidney disease is not only associated with high prevalence and economic burden, but it is also a leading cause of morbidity and mortality worldwide. Based on researchers’ reports, the mortality due to CKD increased 41.5% from 1990 to 2017, rising from the 17th leading cause of death to the 12th.. In 2017, 1.2 million individuals died from CKD. An additional 1.4 million deaths from cardiovascular disease were attributed to impaired kidney function. Together, CKD and related cardiovascular disease deaths accounted for 4.6% of total mortality (Persaud N, [6]).
Unfortunately, CKD awareness is low among the general population, especially since the early stages of renal diseases are often asymptomatic (Alsuwaida, [4]). Epidemiological data showed that 96% of the patients with mild CKD and 48% of the patients with severe CKD are unaware of their disease (Ring A [7]). Therefore, early detection and prevention of CKD by screening programs at primary healthcare centers may have an impact on slowing the progression of CKD, reducing cardiovascular mortality, and reducing the cost of healthcare systems (James, et al. [8,9]) (Table 1). Furthermore, such programs may also promote public health awareness and education. Also, CKD commonly occurs alongside other conditions such as diabetes mellitus, hypertension and obesity and this is an additional reason to make the primary clinicians have a key role in coordinating the care of patients in a centered approach and providing the continuity of care (Fraser, [10]).
Table 1. Relative reduction in ESKD progression and all-cause of mortality in the screening group (Komenda P [9]).
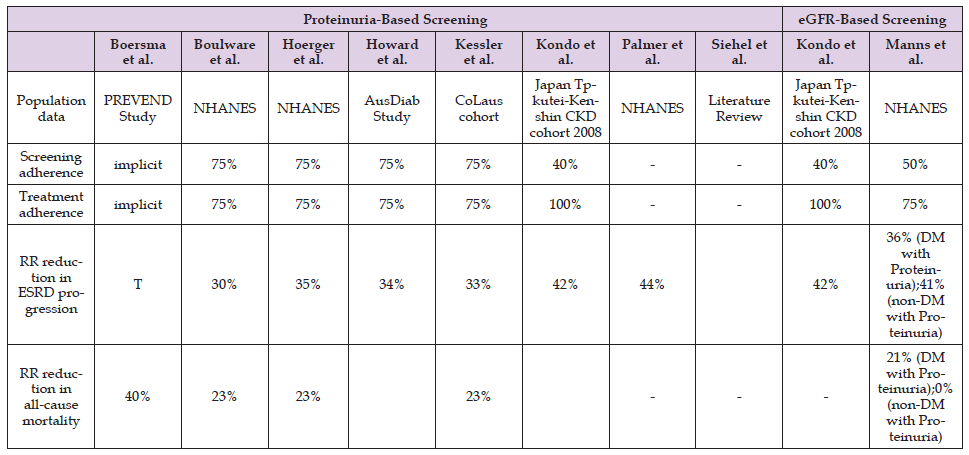
Note: Abbreviations: AusDiab: Australian Diabetes, Obesity and Life Style; CoLaus: Cohorte Lausannoise; CKD: Chronic Kidney Disease; DM: Diabetes mellitus; eGFR: Estimated Glomelluar Filtration Rate; ESRD: End Stage Renal Disease; NHANES: National Health and Nutrition Examination Survey; PREVEND: Prevention of Renal and Vascular Endstage Disease; RR: Relative Risk
So far, most of the local CKD care programs focus on the management of the advanced stages of CKD and their complications by offering the available options of renal replacement therapy (RRT) in the form of hemodialysis, peritoneal dialysis, or renal transplantation. According to the Saudi Center of Organ Transplant Registry, 19,522 patients were on hemodialysis in Saudi Arabia in 2019, with 1,546 patients on peritoneal dialysis, while 13,641 received kidney transplants (Saudi Center of Organ Transplant Report, 2019 [11]). The new healthcare system in Saudi Arabia like other many countries focuses on preventive medicine and screening programs, especially for silent diseases with drastic outcomes like CKD. Therefore, the Ministry of Health in the Kingdom of Saudi Arabia has recently transformed the healthcare system to provide an integrated network of healthcare services covering all the regions of the kingdom.
In healthcare systems, the cost-effectiveness is assessed using the incremental cost-effectiveness ratio (ICER) which is calculated as the incremental change in costs divided by the incremental change in health outcomes. This ratio provides an intuitive metric, which is the cost per life year gained, that helps the decision maker to judge the value of money of any new intervention relative to other technologies and interventions (Barnsbee L [12]). Screening for CKD is cost-effective for high-risk populations based on a systemic review of 9 studies evaluating the cost-effectiveness of primary screening for CKD, e.g., for proteinuria screening, the incremental cost-effectiveness ratios range from $14,063-$160,018/quality-adjusted life - year (QALY) in the general population, $5,298-54,943/QALY in the diabetic population, and $23,028 - $73,939/QALY in the hypertensive population. For eGFR screening, one study reported a cost of $ 23,680/QALY in the diabetic population and the range across two studies was $ 100,253 - $ 109,912/QALY for the general population (Komenda P [9]). Table 2 illustrates the cost-effectiveness of the CKD screening programs in the form of drug therapy compared to dialysis.
Note: All costs reported in 2011 Us dollars. Abbreviations: ACEi: Angiotensin-Converting Enzyme Inhibitor; ARB: Angiotensin Receptor Blocker: CKD: Chronic Kidney Disease; DM: Diabetes Mellitus; eGFR: Estimated Glomerular Filtration Rate; NA: Not Applicable
Most countries reported that nephrologists are primarily responsible for both CKD and Acute Kidney Injury (AKI) care or leaders to provide kidney disease care, but a lack of nephrologists may result in adverse consequences of policy and practice (Figure 1). This can be solved by focusing on the basic infrastructure at the level of primary healthcare for the prevention and early detection of kidney diseases (Crews D, [13]).
Understanding the situation concerning the previous arguments (lack of CKD screening programs in the community, disengagement of primary healthcare centers in the prevention and management of early CKD stages and the high prevalence of patients with end-stage kidney disease requiring renal replacement therapy leading to increased costs and poor patient outcome) has guided us to create a proposal by implementing CKD services within the Primary Health Care centers (PHCs) to be responsible for making all the needed procedures including CKD screening, diagnosing and risk stratifying the new cases based on the degree of kidney function. The CKD service within the PHCs will manage patients with early stages of CKD and refer the advanced cases to secondary hospitals as part of the integrated care. We have succeeded in implementing the CKD new service by using five main strategies:
1. Standardize the knowledge through a concise pathway that
defines the high-risk group patients (defined as individuals >
60 years, hypertension, diabetes mellitus, peripheral vascular
disease, cardiovascular disease, cerebral vascular disease,
autoimmune disease, renal stones, obesity (BMI > 35), previous
acute kidney injury (AKI), family history of stage 5 CKD
or hereditary kidney diseases in a first- or second-degree
relatives, recurrent urinary tract infections (UTIs), history of
kidney disease during childhood, chronic use of nephrotoxic
medications, chronic infection (HBV, HCV, HIV), malignancy
(active and inactive), sickle cell disease) for screening and
methods of screening.
2. Implement the knowledge into an action through the pathway
of screening and referral system based on the severity of
the disease (Figure 2).
3. Determine the required resources including manpower, investigations
and unified medical records.
4. Divide the responsibilities between PHCs, Mega clinics and
Secondary Hospitals (Figure 3).
5. Determine the Key Performance Indicators (KPIs) for monitoring.
Our proposal of implementing the new CKD service in PHCs for (screening the high-risk group for CKD, management of early stages of CKD and referral of advanced stages of CKD to secondary hospitals), has various advantages for the healthcare system that include:
1. Decrease the burden of CKD disease and eventually decrease
the high cost on the healthcare system.
2. Enhance a screening program in the community that will increase
awareness of the disease.
3. Standardizing CKD screening and caring programs in Saudi
Arabia will have a positive impact on patient care and will
enhance the knowledge of family physicians about CKD.
4. Improve local epidemiological data that will help in enhancing
CKD care in the future.
Based on the above benefits, we strongly recommended implementing the new CKD service in the Primary Health Care centers (PHCs) in Saudi Arabia to improve CKD patient care, reduce costs and enhance the quality of care.

