Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Tanveer Hussain1*, Anam Shakeel2, Javaria Zahid Khan3, Aqsa Naseer3, Anum Abbas3, Sadia Ahmed3, Misbah Noureen3 and Tayyab Saeed Akhter3
Received: November 10, 2022; Published: November 18, 2022
*Corresponding author: Tanveer Hussain, Associate Professor Gastroenterology (Rawalpindi Medical University), HOD, Gastroenterology, Holy Family Hospital, Rawalpindi, Pakistan
DOI: 10.26717/BJSTR.2022.47.007461
Background: Acute pancreatitis is a pancreatic inflammatory condition, with the involvement of underlying tissues and remote organ systems. Early diagnosis of severe acute pancreatitis is crucial to detect complications. The purpose of this study was to correlate the NLR values with the severity of acute pancreatitis.
Materials and Methods: This study was conducted at Department of Gastroenterology, Holy Family Hospital from 01 November 2020 to 30 April 2021. It was a cross sectional study. 95 patients with diagnosis of acute pancreatitis were included. Ranson’s score was calculated. Severity of acute pancreatitis was confirmed on completing ranson’s score. The NLR values were calculated on first day of admission and repeated after 72 hours of admission. Data were entered and analyzed using SPSS v25.0. Independent t-test was used to determine if mean score was significantly different between two categories of severe pancreatitis as per ranson’s scale.
Results: The mean age of the patients in our study was 64.66±5.84 year. Out of 95 patients, 40(42.1%) were males and 55(57.9%) were females. The frequency of severe acute pancreatitis was 22.1%. In patients with mild and moderate acute pancreatitis with Ranson’s score<3, the mean NLR at admission was 5.45 ±2.50. while in severe AP with Ranson’s score >3, the mean NLR was 14.90 ± 4.70. The results of NLR at admission and at 72 hours of admission were significantly different in patients regarding severity of acute pancreatitis.
Conclusion: NLR significantly correlated with severity of acute pancreatitis. NLR can be used as a prognostic biomarker in patients admitted to the emergency department with acute pancreatitis.
Keywords: Acute Pancreatitis; Ranson’s score; Neutrophil-Lymphocyte Ratio
Abbreviations: AST: Aspartate Aminotransferase; LDH: Level and Serum Lactate Dehydrogenase; HCT: Hematocrit; BUN: Blood Urea Nitrogen; NLR: Neutrophil-to-Lymphocyte Ratio; SIRS: Systemic Inflammatory Response Syndrome
Acute pancreatitis is an inflammatory condition, with the underlying tissue and remote organ systems involvement [1- 3]. Acute Pancreatitis is one of the most common diseases of the gastrointestinal system requiring hospitalization. Acute pancreatitis occurs in 80 to 90 percent of patients as an isolated condition and does not require any treatment; however, it occurs in its clinically serious form in 10 to 20 percent and may cause local or systemic complications [4,5]. Early diagnosis of severe acute pancreatitis is crucial if care is to continue treatment in due course, as early as possible to detect complications, and to refer patients to appropriate treatment centers [6]. To schedule care for patients at risk for serious diseases and the occurrence of complications, different guidelines are applied, and other serum markers may be used to determine the seriousness of the disease scoring systems. The neutrophil- lymphocyte ratio (NLR) may be one such measure [7]. The NLR is determined by dividing the peripheral blood neutrophil count by the lymphocyte count. The existing literature revealed NLR as a parameter representing the negative effects of high numbers of neutrophils and low numbers of lymphocytes that together demonstrate the worsening of the general health condition and physiological stress [7,8].
In benign and malignant clinical conditions, high NLRs have been associated with poor prognosis [9]. The NLR can be quickly and simply calculated using a complete blood count in the emergency department and studies have demonstrated that the NLR provides valuable information for critical hours interventions [10]. In a study, 19% patients had severe acute pancreatitis. Mean NLR in mild acute pancreatitis was 5.01±5.10 and 16±13.81 in severe acute pancreatitis [11]. In another study, mean NLR in mild acute pancreatitis was 8.56±9.68 and 16.36±11.96 in severe acute pancreatitis [12]. The rationale of the study was to document NLR as a predictor for acute pancreatitis severity assessment in local population. By determining the mean neutrophil-lymphocyte ratio, we may be able to determine the risk of complications in patients with severe acute pancreatitis. This may ultimately help in reducing the impact of long-term complications of acute pancreatitis.
Study Setting: The study was conducted at Gastroenterology Department, Holy Family Hospital, Rawalpindi.
Duration of Study: November 01, 2020, to April 30, 2021
Study Design: Cross sectional study
Sampling Technique: Non-probability consecutive sampling
Sample Size: The sample size of 95 cases was estimated by using 95% level of confidence with 8% margin of error and taking an expected percentage of severe acute pancreatitis as 19% in patients with acute pancreatitis [11].
After taking approval from hospital ethical committee, all patients with clinical diagnosis of acute pancreatitis diagnosed based on clinical findings and investigation from emergency and OPD were included after taking informed consent. Demographics including age, gender and address were recorded at day of admission. Ranson’s score was calculated for these patients by measuring age, white cell counts, blood glucose level, serum aspartate aminotransferase (AST) level and serum lactate dehydrogenase (LDH) level at the time of admission.
Severity was confirmed on second post-admission day completing ranson’s criteria by measuring decrease in hematocrit (HCT) level, Blood urea nitrogen (BUN) level, serum calcium level, arterial partial pressure of oxygen (PaO2), base deficit and fluid requirement. The NLR values were calculated by dividing the neutrophil number in the peripheral blood by the lymphocyte number. Sample for NLR was take on day of admission and was repeated after 72 hours of admission. All the data were collected through a pre-designed proforma (attached).
Data were entered and analyzed using SPSS v25.0. Mean and standard deviation were calculated for quantitative variables like age, BMI, ranson’s score and neutrophil lymphocyte count ratio at admission and 72 hours. Frequency and percentage were calculated for qualitative variables like gender and frequency of severe pancreatitis according to ranson’s score. Mean and standard deviation of NLR score was calculated for ranson’s score ≥3 and ranson’s score less than 3. Independent t-test was used to determine if mean score was significantly different between two categories of severe pancreatitis as per ranson’s scale.
Total 95 patients with clinical diagnosis of acute pancreatitis were included. Out of 95 patients, 40(42.1%) were males and 55(57.9%) were females. The mean age of the patients was 64.66±5.84 year. Most of the patients 62(65.3%) had ages >50 years, while 33(34.7%) had <50 years. The results of BMI showed that, 59(62.1%) patients had normal weight, while 32(33.7%) patients were overweight, and 4(4.2%) patients were obese. The mean value of Ranson’s score was 1.88±1.53. 74(77.9%) patients had mild to moderate acute pancreatitis with Ranson’s score (<3) and 21(22.1%) had severe acute pancreatitis with Ranson’s score (≥3). The frequency of severe acute pancreatitis in patients with acute pancreatitis was 22.1%.
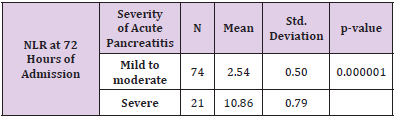
In patients of mild to moderate acute pancreatitis with Ranson’s (<3), the mean value of NLR at admission was 5.45±2.50 and in patients of severe acute pancreatitis with Ranson’s (≥3), the mean value of NLR at admission was 14.90±4.70. In patients of mild to moderate acute pancreatitis with Ranson’s (<3), the mean value of NLR at 72 hours of admission was 2.54±0.50 and in patients of severe acute pancreatitis with Ranson’s (≥3), the mean value of NLR at 72 hours of admission was 10.86±0.79. The mean value of Ranson’s score in mild to moderate acute pancreatitis patients was 1.19±0.72 and in severe acute pancreatitis patients was 4.33±1.02. The results of NLR at admission and at 72 hours of admission were significantly different in patients regarding severity of acute pancreatitis. The p-value was less than the level of significance (Tables 1-4).
Table 3: Comparison of NLR at 72 hours of admission between mild to moderate and severe acute pancreatitis.
Acute pancreatitis is an inflammatory disease of the pancreas that can involve the surrounding tissue and distant organ systems [13-15]. AP is one of the most common gastrointestinal system diseases that require hospitalization. More than 80% patients with acute pancreatitis recovered without any specific treatment or symptomatic treatment, but 10% to 20% patients with AP, have clinically severe disease that can cause local or systemic complications. Treatment goal for acute pancreatitis should be to predict about severe cases as early as possible to limit the complications. Acute pancreatitis severity diagnosis is important to start treatment, recognizing complications and shifting patients to relevant center. Treatment of acute pancreatitis, keeping in mind the severity of disease, many available severity scoring systems, different criteria, and few serum markers are in practice to find patients who will be potential candidates of severe pancreatitis and its complication The neutrophil-to-lymphocyte ratio (NLR) is one of these parameters that can assess severity of acute pancreatitis. NLR representing the negative effects of high numbers of neutrophils and low numbers of lymphocytes that together demonstrate the worsening of the general health condition and physiological stress [9].
The NLR can be calculated quickly and simply using a complete blood count in the emergency department, and studies have shown that the NLR provides valuable information for interventions during the critical hours [10]. In our study 95 patients with diagnosis of acute pancreatitis were included. The results of BMI showed that, 59(62.1%) patients had normal weight, while 32(33.7%) patients were overweight, and 4(4.2%) patients were obese. 74(77.9%) patients had mild to moderate acute pancreatitis with Ranson’s score (<3) and 21(22.1%) had severe acute pancreatitis with Ranson’s score (≥3). Mild to moderate AP group NLR value at admission and after 72 hours were 5.45 ±2.5 and 2.54 ±0.5 respectively. While severe AP group NLR value at admission and at 72 hours were 14.9 ±4.70 and 10.86 ± 0.79 respectively.
Patients with severe AP may suffer long-term intensive care admission, long-term hospitalization, and invasive interventions, and significant mortality rates may occur [16-20]. The scoring systems that have been used to determine the prognosis and severity of AP have various limitations. The search for new parameters besides these scoring systems is one of the active discussions at present. We examined NLR association with the severity of AP in the present study. According to the data obtained in our study, the NLR was significantly higher in the severe AP groups than in the mild AP groups, according to both Ranson’s scoring and revised Atlanta classification of AP (p<0.001).
Neutrophils provoke the inflammatory cytokine cascades (interleukin, IL-6, IL-8, and tumor necrosis factor alpha), proteolytic enzymes (myeloperoxidase, elastase, collagenase, and β-glucuronidase), and free oxygen radicals and stimulate inflammation and tissue destruction [21]. It has been observed that these inflammatory mediators have important effects on the systemic inflammatory response during AP [22]. An increase in the neutrophil count indicates the development of systemic inflammatory response syndrome (SIRS) and multiple organ failure syndrome, which are indicators of severe AP. Neutrophils provoke the inflammatory cascade and SIRS in AP, leading to a decrease in the lymphocyte count during severe sepsis, and this is associated with a poor prognosis [23-24]. SIRS, multiple organ failure, and severe sepsis are systemic complications of AP. Studies have also shown that there is an association between the low peripheral lymphocyte count and the severity of the disease in AP cases [25- 26].
Jones, et al. in his study conducted between 2007 and 2011 including 629 patients treated with the diagnosis of AP, examined the association between the severity of pancreatitis, disease prognosis, in-hospital mortality, and NLR. They reported that they detect a significant association between the NLR and the severity, prognosis, and in-hospital mortality of acute pancreatitis [27-28]. Azab, et al. in his study of 283 patients demonstrated that the NLR value is significantly higher in severe AP cases than in mildmoderate AP cases. Study showed that the NLR is superior to the WBC for predicting intensive care admission on their ROC curve for admission to the intensive care unit. They also reported the NLR cut-off value for predicting intensive care admission and duration of hospitalization as ≥4.7 [27]. Suppiah, et al. divided AP patients into groups of mild and severe AP according to the Atlanta criteria and compared the NLR values of these groups on admission, day 1, and day 2.
They reported admission NLR cut-off value as 10.6, day 1 NLR cut-off value as 8.1, and day 2 NLR cut-off value as 4.8 in their ROC analysis to predict patients with mild and severe AP 9.A retrospective study conducted in South Korea, the NLR on admission and day 2 was found to be significantly higher in the moderate to severe AP group than in the mild AP group (p=0.01 and p=0.001, respectively) [29].Additionally, the NLR on admission calculated according to the Ranson’s score was observed to be significantly higher in the severe AP group than in the mild AP group (median (IQR): 9.60 (13.68) vs. 4.56 (4.74), respectively; p<0.001) 11. The relationship between mortality and the NLR value in AP has been reported in several studies. Gülen, et al. published a retrospective study in 2015 that divided 332 patients with AP into two groups of alive and dead patients. They identified that the NLR is significantly higher (p=0.041) in the group that had expired than in the group that had survived patients [30].
This study has demonstrated association between NLR and severity of acute pancreatitis. Based on the available evidence, we believe that NLR as a single parameter can predict the systemic complications of AP. Emergency department physicians should also consider NLR in addition to the multifactorial scoring systems for predicting the prognosis of AP. NLR can be used as a prognostic biomarker in patients admitted to the emergency department with acute pancreatitis.


