Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Jian Song1, Yulin Zhan2*, Yaqian Wang3 and Jiaqi Li1
Received: August 26, 2022; Published: September 07, 2022
*Corresponding author: Yulin Zhan, Orthopedics Department, Shanghai Sixth People’s Hospital East Affiliated to Shanghai University of Medicine Health Science, Shanghai, 201306, China
DOI: 10.26717/BJSTR.2022.46.007284
Background: Simultaneous fracture of bilateral femoral necks is a rare case. The femoral neck is a key position of stress on the upper and lower limbs. The femoral head necrosis may be caused by the injury, which is often paid close attention to by trauma surgeon. Fractures due to trauma are categorized as fatigue fractures, and fractures due to pathological factors such as vitamin D deficiency, hyperparathyroidism and chronic renal failure are categorized as dysfunctional fractures
Case Presentation: This case described a 30-year-old young male patient with bilateral femoral neck fractures after a short jog. MRI be diagnosed as Garden I type; CT showed mild hip osteoporosis; Laboratory index showed vitamin D deficiency and other performance are normal. He had a history of chronic ankle instability due to the right ankle sprain. Under the guidance and advice of doctors, the fracture achieved recovery after conservative treatment.
Conclusion: The young adult caused by low-energy occult bilateral femoral neck fracture in the early diagnosis is not obvious. Femoral neck fracture in the early X-ray slice is difficult to determine and easy to be misdiagnosed as synovitis of the hip or traumatic arthritis, so that the clinical intervention time was delayed. To avoid fracture displacement and femoral head necrosis, the patient of femoral neck mild fracture requires complete non-weight bearing for 8-12 weeks and part weight bearing for 4-6 weeks; In order to prevent osteomalacia, more severe osteoporosis and abnormal bone metabolism causing convulsions or epilepsy, punctual vitamin D supplementation and reasonable exposure to sunlight is considerable. Timely and effective surgical intervention is necessary for the complete and displaced fractures. CT, MRI, laboratory examination and comprehensive inquiry are helpful to diagnose and eliminate misdiagnosis. Diseases that affect metabolic processes, such as smoking, long-term stay up and severe fatty liver, can be also result in to bilateral femoral neck fractures.
Keywords: Fracture of Femoral Neck; Vitamin D Deficiency: Chronic Ankle Instability; Conservative Treatment; Case Report
Abbreviations:: CT: Computed Tomography; MRI: Magnetic Resonance Imaging; SLRT: Straight Legs Raising Test; CAI: Chronic Ankle Instability; CRIF: Closed Reduction and Internal Fixation; THR: Total Hip Hemiarthroplasty; THA: Total Hip Arthroplasty; AVN: Avascular Necrosis; NWB: Non-Weight Bear; PWB: Part- Weight Bear
Cases of unilateral femoral neck fracture are often encountered clinically. Studies have confirmed that femoral neck fracture on one side often leads to secondary fractures on the other side due to increased compensatory force on the undamaged side [1]. However, Simultaneous bilateral femoral neck fracture is very rare, which is more difficult to detect in the young patient population. It usually occurs in traumatic situation, such as accidental electric shock [2- 5]. traffic accident [6-8], The recruit training [9,10], high or sudden fall [11,12], weight lifting [13], etc. There are also secondary to pathological condition, The etiology due to hyperparathyroidism or osteomalacia caused by vitamin D deficiency [14-22], epileptic seizure [16-25], chronic renal insufficiency [25,26], secondary metabolic disorder of malnutrition [26-30], postoperative joint replacement [31], drugs of Allen phosphonic acid or sugar cortical hormone [32], narcotic drug abuse [33], abnormal bone metabolism and bone resorption on account of metastatic tumor [34], etc. The etiology of this kind of fracture is complex and the condition of a patient is occult. Early X-ray examination is difficult to diagnose and is often misdiagnosed as hip arthritis or synovitis, which delays the treatment and leads to irreversible damage such as delayed or nonunion of bone, even avascular necrosis of femoral head. Timely MRI and comprehensive inquiring are helpful for early diagnosis and clinical intervention. This article describes a 30-year-old patient with habitual falls due to chronic ankle sprains、osteoporosis due to vitamin D deficiency and bone metabolic disorders due to fatty liver, who is diagnosed as bilateral femoral neck fractures(Garden I type). He was taken conservative remedial measures with no weight bear 2 months and part weight bear for 1 month, in addition to non-highlight insolation and nutritional supplements. Ultimately the fracture was completely healed, Except for fatty liver, other index was normal, and the patient returned to daily work and life after 1 year follow-up visit. The article was written and published with the informed consent of patients.
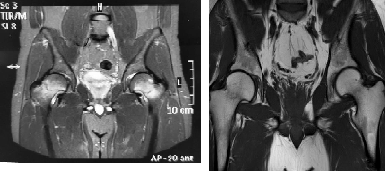
This case describes a 30-year-old male patient with bilateral femoral neck fracture after a short jog, he was labeled as an office worker、smoker、nightbird and fatty liver. One month before, because of his overweight(The body mass index = 25.68 kg/m2) the patient undergoes consecutive jogging about two kilometers per time. After the warm-up exercise on the fourth day, it was happened to the symptom of severe bilateral groin pain and swelling, which is aggravated by high knees lifting、stomping, and sneezing , meanwhile, it is eased by sit rest and hot compress. Physical examination is showed a positive result of Straight legs raising test(SLRT)、Heel strike test and Patrick ‘s test, The myodynamia the of bilateral lower limbs are V level. No abnormalities were found in the X-ray plates at the local hospital, it was considered as the hip arthritis. The resident prescribed Diphen (Diclofenac sodium Double Release Enteric capsule) and Huoxuezhitong capsule (Chinese patent medicine) for anti-inflammatory and analgesic with symptomatic treatment, however, no improvement was found, so he was transferred to our hospital. Computed tomography (CT) showed bilateral femoral neck incomplete fracture (Garden I type) and double hip mild osteoporosis; Magnetic resonance imaging(MRI) include TI-weight, T2-weight, and short-time inversion recovery(STIR) saw the fracture line and the surrounding callus, no tumor space-occupying lesions, bilateral bone structures are normal (Figure 1).
Figure 1: MRI of the patient was compared before and after the treatment
(A) The first MRI of STIR after injury which reveals a bilateral femoral neck fracture and diffuse edema at the fracture site.
(B) The 6 months MRI after injury which shows the bilateral healed fracture line.
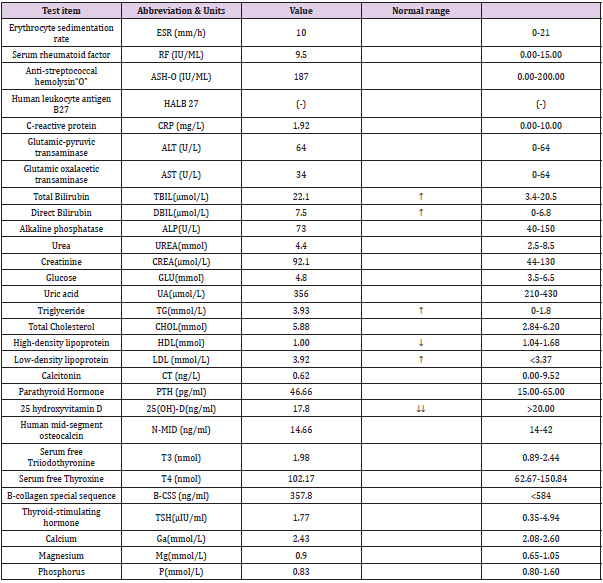
Laboratory tests showed: abnormal vitamin D:17.8 ng/ml (normal 30-100ng/ml), Previous high blood lipids including triglyceride、low density lipoprotein、high-density lipoprotein、total bilirubin、direct bilirubin, other blood indicators were normal, including blood cells, ESR, CRP, RF, HLA B27, ALP, Ca, P etc. (Table 1). A detailed inquiry revealed that the patient had a history of chronic ankle sprains, and the sequelae were chronic ankle instability(CAI), The clinical manifestations are easy to have a fall when walking and climbing stairs, For the past 2 months, The patient had fallen 6-8 times during walking up and down stairs, which may be the direct traumatic factors of fatigue fracture. The patient’s parents have various degrees of hypertension and diabetes, and no other related genetic diseases have been found. Final diagnosis determination: Bilateral femoral neck fatigue fracture (Garden I type); Vitamin D deficiency; Severe nonalcoholic fatty liver disease; Chronic ankle instability. To avoid the fracture displacement and return to normal activities as soon as possible, He was taken conservative remedial measures with no weight bear for 2 months and part weight bear for 1 month, to improve the vitamin D deficiency ,in addition to non-highlight insolation and nutritional supplements. the fracture was completely healed after 6 months, no complications including necrosis of the femoral head and secondary osteomalacia etc. Except for fatty liver, keeping the Vitamin D level close to normal and other index were within normal range, the patient returned to normal work and life during extra 1 year follow-up visit.
Table 1: Laboratory data during patient’s visit ↑ suggests indicators are on the high side; ↓suggests indicators are on the low side; The amount of ↑ and ↓ reflects the severity.
Femoral neck fracture is a common orthopedic disease. Due to its occult location and weak blood circulation, its diagnosis and treatment are complicated. Improper treatment may cause fracture nonunion or even necrosis of the femoral head, which will bring lifelong pain and lameness to the patients. Simultaneous bilateral femoral neck fracture is rare in clinic, past the old case only 31 cases in young people (Table 2), the most common cause of accidental electric shock, seizures, recruits training, chronic renal failure, vitamin D deficiency cause osteomalacia and osteoporosis, hyperparathyroidism and other metabolic dysfunction disease. This article describes the case is a 30-year-old young people because of chronic ankle instability, lead to overall instability of lower limb lines of force [35], too much load to the femoral neck the maintaining of the key parts of the onset of coordination and balance, the burden of femoral neck becomes overweight, the constant bony destruction causes inflammatory factor invasion, leading to increased bone remodeling, eventually lead to local micro fracture. Other etiological factors is the osteoporosis caused by a lack of vitamin D [36], the reason comes down to the patient working all of the day night and less sun exposure[37], patients with abnormal liver function[38] is also an important reason resulting in abnormal bone metabolism index, Vitamin D is key molecules, in bone metabolism in liters of blood calcium effect of the parathyroid hormone and calcitonin balance effect between role in blood calcium.
Table 2: Literature review associated with Simultaneous bilateral femoral neck fractures in young patients.
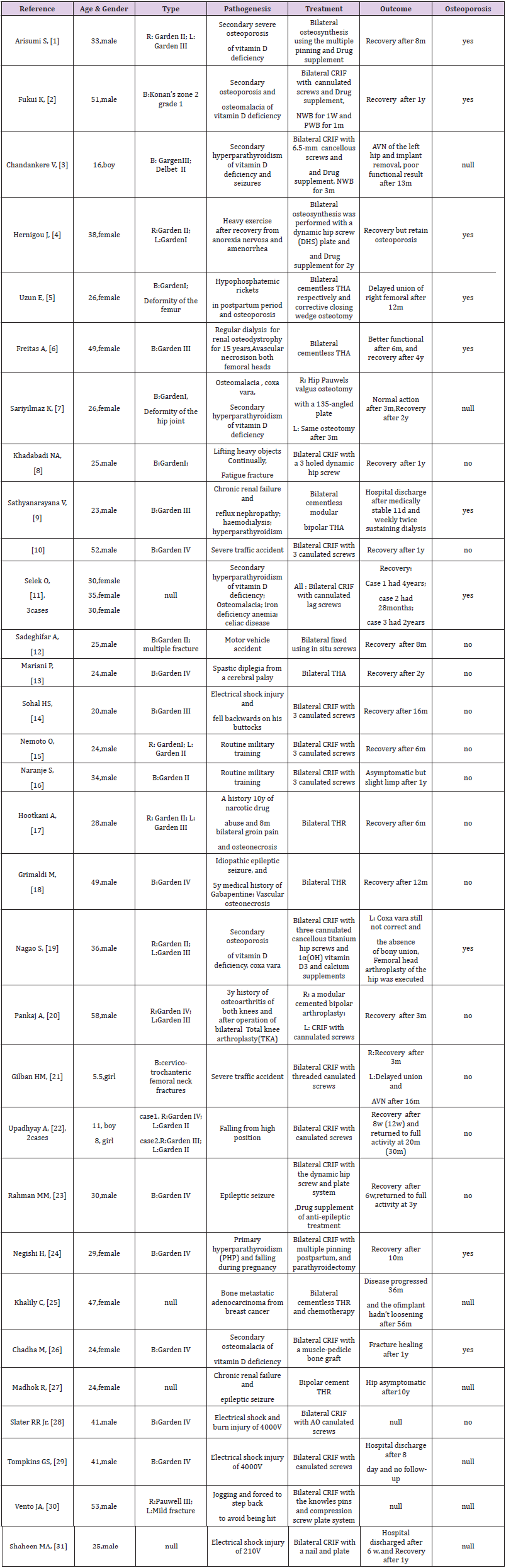
Note: B:Bilateral; L:Left; R:Right; CRIF:Closed reduction and internal fixation; THR:total hip hemiarthroplasty; THA:total hip arthroplasty; AVN:Avascular necrosis; NWB:non-weight bear; PWB:part-weight bear; y:year(s); m:month(s); w:week(s); d:day(s); V:voltage; null:not mentioned.
the first hydroxylated vitamin D3 in the liver forms 25-(OH)- vitamin D3,which promotes bone formation, the second hydroxylates in the kidney forms vitamin D, which promotes the calcium ion of original urinary being absorbed into the bloodstream. Vitamin D deficiency often leads to abnormal blood bone metabolismrelated indicators such as Ga, P and Mg, and eventually decreases femoral bone mineral density and increased susceptibility of microfractures. Furthermore, poor lifestyle habits such as smoking [39] and staying up late [40] can also lead to changes in bone mineral content and even fractures. Based on previous clinical practice, according to the severity of fracture (Garden I type) and the clinical cases reported in the literature, therefore we chose conservative treatment strategies, namely the weight 2 months, part weight bearing a month, and every day low-light sun exposure. eventurely we found the bilateral healed fracture line, regular follow-up showed that he had restored to the normal work and life. Previous treatment methods have focused on high-cost surgical therapy such as internal fixation or hip arthroplasty. This case provides clinicians with a new treatment idea.
Bilateral femoral neck fracture is very rare, early clinical feature is difficult to detecte. Garden type I is harder to come across. For common patients with femoral neck fractures, surgical operative treatment is the usual strategy. this patient had a satisfactory curative effect after conservative treatment. This case provided a reference for future clinicians.
Ethics Approval and Consent to Participate: Not applicable.
Written informed consent was obtained from the patient for publication of this case report, along with any accompanying images. A copy of the written consent is available for review by the Editor of this journal.
All data concerning the case are presented in the manuscript.
The authors declare that they have no competing interests.
Major Project of Shanghai Municipal Health and Family Planning Commission (201640004). The applicant and beneficiary of this Funding is Zhan Yulin ,who reviews and makes the determination of the final version of the manuscript; The fund will sustain all the expenses during the submission process of this research.
a. Conceptualization, Writing of manuscript, Literature review,Patient consultation and follow-up: SJ.
b. Diagnosis and treatment of patients,Reviewing and decidng the final version of the manuscript: ZYL.
c. Data collections and arrangements: WYQ; LJQ
d. All authors have read and approved the manuscript and ensured this is true.
We thank Du Jingyu (Shanghai University of Traditional Chinese Medicine, China) for providing professional English language editing of this article.
Between June 2014 and December 2016, 8 childhood or adolescents with tibial-sided ACL avulsion fractures were treated at our institution. And all patients had obviously clinical symptoms: pain, swelling, giving way and locking, and pivot-shift test positive and Lachman test positive. Radiographic examinations were used to evaluate the injury on admission. Seven patients had type III fractures and one patient had type IV fracture, which were defined according to the classification of Meyers and McKeever. All 8 patients have intact ACL, without osteoarthritis or tibial and femoral fracture. Besides, all patients have non-fusion epiphysis. All patients were followed-up at least 12 months. Clinical outcomes were assessed using IKDC and Lysholm scores at 1, 3, 6, and 12 months after the operation. CT scans were also performed in all cases at 1 day, 3, 6 and 12 months postoperatively.
Patients were in a standard supine position with the knee at 90 degrees of flexion. Diagnostic arthroscopy was performed through the standard anterolateral portal and anteromedial portal, and the hemarthrosis was evacuated from the joint. The fracture was visualized, and the fracture bed on the underlying tibial cancellous bone was cleaned with a shaver and slightly deepened (Figure 1A). A pilot hole for the anchor was created with a 15.0 mm suture anchor punch (Bio-Corkscrew, Arthrex, Naples, FL, USA) angled at 45°in the sagittal plane with respect to the tibial plateau. The hole was located 5mm posterior to the fracture rim at 2 o’clock (10 o’clock in the left knee) (Figure 1B). While maintaining reduction with a probe through the anterolateral portal, the inferomedial part of the ACL was pieced with a suture hood loaded with NO.2 polydioxanone (PDS) through the anteromedial portal (Figure 1C). The PDS was advanced out through the hook and retrieved out from the media portal with a grasper. and the suture was passed through the base of the ACL to the anteromedial portal by pulling the PDS (Figure 1D). “8” knot-type was performed with the use of a self-locking sliding knots at the tip of the anchor to achieve appropriate tissue tension. Then, a 19.5 mm lateral-row of anchor (Bio-Corkscrew, Arthrex, Naples, FL, USA) was inserted angled at 90° in the sagittal plane located 10 mm inferior to the lateral side tibial tubercle to fix the knot (Figure 1E). Usually total one bioabsorbable suture anchor and one lateral-row of the anchor were used (Figure 2).
Figure 2: Schematic drawing of left knee in anterior view, illustrating non-transosseous 2-point suture fixation technique.

Patients received the standard rehabilitation protocol: immobilization of the knee with a brace in full extension for 6-8 weeks, after which mobilization was started, below 90°of flexion until the third month and then, increasing the flexion of the knee 15° every week. Full range of motion and progressing weight bearing with brace unlocked were allowed at 3 months after surgery. If anatomic fracture healing was confirmed completely via CT scan at several months, the brace was discontinued, and return to sports was allowed at more than 4 months.
Data were analyzed using STATA version 12.0 software (College Station, TX, USA). IKDC and Lysholm scores were compared using independent-sample t-tests between pre-operation and different follow-up points postoperatively. The P value for determining statistical significance was set at <0.05.
A total of 8 patients (5 males and 3 females) were included in the study, respectively. The right knee was affected in 4 patients and the left knee was affected in 4 patients. Mean age of patients at the time of trauma was 12.3 years (range, 9-14 years). Seven patients (87.5%) had type III fractures and one patient had type IV fracture (comminuted fracture). The mean operative time was 77.7 minutes (range, 62-90 minutes), and the mean bleeding volume was 9.3 ml (range, 5-15 ml). And four patients underwent injured meniscus suturing simultaneously. All patients underwent at least 12 months of follow-up, the mean follow-up period was 14.6 months (range, 12-18 months). The demographic data of selected patients was shown in (Table 1) There were no intraoperative or postoperative complications, such as infection, synovitis, or synarthrophysis in all patients. CT scan (Figure 3) showed that all 8 patients had an anatomical reduction of fracture at 1 week after the operation.
Table 2: Preoperative and follow-up outcome scores for all patients.

Note: *Knee clinical scores at 12 months follow-up compared with scores preoperatively
Figure 3:
a) Lateral CT scan showed ACL tibial avulsion fracture preoperatively.
b) Lateral CT scan showed anatomical reduction of fracture at 1 day after operation.
c) Lateral CT scan showed the fragment healing at 3 months follow-up.
d) At 12 months follow-up, lateral CT scan showed the fragment healed superiorly with persistent epiphysis.

Figure 4: A typical case of ACL tibial avulsion fracture (female, 12 years old).
a) Three mini-portals on left knee on gross view postoperatively.
b) Lateral CT scan showed ACL tibial avulsion fracture.
c) (C, D) Lateral CT scan showed an anatomical reduction of fracture 1 month and 1 year after the operation.
d) (E, F) MRI scan showed the fragment healing at 24 months follow-up.

And 3 months after the operation, CT showed fracture healing and at 12 months follow-up, the fragment healed superiorly with persistent epiphysis in all patients, and all patients had stable Lachman and negative pivot shift tests. IKDC score improved from 30.8±5.1 preoperatively to 87.6±3.4 at 12 months postoperatively (p<.001). The Lysholm scores also significantly increased from37.3±5.9 preoperatively to 91.5±2.6 at 12 months followup (p<.001). Subjective evaluation development over time by the described scores was shown in (Table 2). Statistical analyses of clinical scores were performed with regard to the different followup points. The IKDC and Lysholm score showed a significant increase comparing the different follow-up points (1, 3, 6 and 12 months) with the preoperative situation, especially at 6 months follow-up, the functional scores significantly were greatly improved (p<.001). A typical case of ACL tibial avulsion fracture was showed in figure 4. On the other head, the data on the height of all patients before and 1 year after operation (Table 3) was collected, and this technique did not affect growth based on the normal height scale.
Table 3: Height of all patients pre-operation and at final follow-up

Note: *Knee clinical scores at 12 months follow-up compared with scores preoperatively
This prospective study firstly described a novel technique of one-step arthroscopic “8” knotted fixation without bone tunnels in non-fusion-epiphysis patients who suffered tibial-sided ACL avulsion fractures using bioabsorbable suture anchors. The clinical efficacy was satisfactory at 12 months follow-up with fracture radiographically healing at 6 months follow-up. This operation had the advantages of promoting bone healing and moulding with no damage to the non-fusion epiphysis of patients. Thus we answered the following questions:
1. Is arthroscopic “8” knotted fixation without bone tunnels in tibial-sided anterior cruciate ligament (ACL) avulsion fracture suitable for non-fusion-epiphysis patients?
2. Dose this novel method improve functional and radiographical outcomes? Tibial-sided ACL avulsion fractures result in anterior knee instability and occasionally in loss of knee extension. Surgical treatment is recommended for all Meyer- McKeever classification except type I. A wide variety of fixation methods have been used to fix tibial-side ACL avulsion fractures including screw, steel wire, band wire, PDS suture and suture anchor. Fixation with screws with the advantage of direct reduction and compression of the fracture fragment was the most common method [8]. However, operation in the epiphyseal region would probably interfere with the growth of epiphysis, especially in childhood or adolescence. Besides, screw fixation destroyed the collagenous fibers of ACL attachment and was not appropriate for the small or comminuted fragment [9]. In addition, using steel wire or band wire was so complicated that needed two bony tunnels drilled from the proximal tibial cortex which may destroy the epiphysis even using 1.0 mm-sized K-wire [10]. By the way?, there may necessitate implant removal after fracture healing [9, 11, 12]. Besides, simply using PDS suture or suture anchors does not provide a direct reduction of the fracture fragment, although suture anchors could rely on a tension band effect from force applied to the ACL [13].
However, the limitations could be overcome using one-step arthroscopic “8” knotted fixation. First, “8” knotted fixation is not only suitable for large fracture fragments but also reliable for small or comminuted fragments. Second, previous researches have demonstrated that Wire suture is superior to single screw fixation in biomechanical testing [14,15]. In addition, Anderson et al [16] also showed that Wire suture tired over a suture button could improve fixation when compared with a single screw. In addition, the double-row suture technique in rotator cuff repair could provide a great contact area, as well as biomechanical advantages [17]. So this “8” knotted fixation technique achieved in one step with only one suture anchor may provide strong biomechanical strength for tibial-sided ACL avulsion fracture. Besides, this one-step technique further shortened the time of operation and decreased bleeding. Besides, there is no need to take out the suture anchors for their degradability. Based on the surgical benefits of this technique, we used one-step arthroscopic “8” knotted fixation without bone tunnels in non-fusion-epiphysis patients to fix the ACL avulsion fracture, and achieved good clinical results with anatomical reduction intraoperatively and radiographically healing postoperatively at 6 months after the operation. Consequently, this technique may be reliable for its biomechanical strength and simplification. In addition, there is no need to drill tibial tunnels through osteoepiphysis, and completely avoid damaging the epiphyseal plate during internal and external anchors insertion.
We collected the data on the height of all patients before and 1 year after operation, which indicated that this technique did not affect growth based on the normal height scale. The rehabilitation protocol tends to advocate a more conservative approach with longer periods of non-weight bearing, bracing and a delayed return to sport in comparison with more functional-based adult protocols [18, 19]. Furthermore, there seems to be a consensus on the use of a knee brace during sports activities, although no solid studies have been published on the area of bracing and ACL injuries in children [20]. In this study, the brace should be kept on being used until the fracture heals radiographically. As a result, the clinical scores at 1 and 3 months were not particularly satisfactory because of the conservative rehabilitation with the brace. Whileonce removed the brace at 4 months or more postoperatively, the patients underwent positive rehabilitation, consequently, the clinical scores were significantly improved than 1 and 3 months after the operation. The limitations of the present study are: first, we did not investigate the clinical scores and radiographical results at long-term follow-up, although this study showed satisfactory short-term results; second, this was a small initial case series without comparative studies, we cannot conclusively show the effectiveness of this technique. And further randomized controlled studies are desired to demonstrate the efficacy of this novel technique. Besides, it should be emphasized that no biomechanical study was conducted to determine fixation strength during this study.
The technique of one-step arthroscopic “8” knotted fixation without bone tunnels in ACL avulsion fracture was significantly effective in terms of CT scan and clinical outcomes in nonfusion- epiphysis patients. The use of arthroscopic fixation has an obvious advantage in that the osteoepiphysis could be protected during arthroscopy. This novel method with no need to remove the bioabsorbable anchors may be less invasive than traditional treatment. To conclusively show the effectiveness of this treatment requires comparative studies, especially with an established traditional arthroscopic procedure.
We thank all the authors for contributing to this study. This work was supported by the National Natural Science Foundation of China (82072398, 82002320, 81201395, 81171703) and Natural Science Foundation of Zhejiang Province (LQ21H060005).

