Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
María del Carmen Díaz-Galindo1, Gabriela Careaga-Cárdenas, Ricardo E Ramírez-Orozco3 Flavia Josefina Lugo-Balderas2, Denisse Calderón-Vallejo1,4 and J Luis Quintanar1*
Received: July 28, 2022; Published: August 25, 2022
*Corresponding author: J Luis Quintanar, Laboratorio de Neurofisiología, Depto. de Fisiología y Farmacología Centro de Ciencias Básicas, Universidad Autónoma de Aguascalientes Av. Universidad 940 C.P. 20100 Ciudad Universitaria, Aguascalientes AGS., México
DOI: 10.26717/BJSTR.2022.45.007266
Patients with spinal cord injury (SCI) have central and peripheral nervous system damage and they exhibited an abnormal electromyography (EMG) response. Leuprolide acetate (LA) has been reported to induce neural regeneration after SCI in animal models and humans. The aim of this work was to analyze whether electromyography and clinical variables improved with treatment of LA in a patient with SCI. A 38-yearold woman had a car accident and a complete spinal cord section at C6 level was diagnosed. One year after the car accident, EMG and initial clinical evaluations were performed. Six months after these initial evaluations, treatment with LA started and consisted of an intramuscular injection (7.5 mg) each month during six months. At the end of this time, the electromyography and clinical signs were reevaluated. The patient treated with LA showed an increase nerve conduction velocity, encourage of muscle activity and higher muscle strength respect to initial evaluation. In conclusion, LA stimulate the recovery of muscle strength. These results are important because they offer an accessible pharmacological strategy that can improve the quality of life of patients with SCI.
Keywords: Neuroregeneration; Chronic Spinal Cord Injury; Leuprolide Acetate; Rehabilitation
Every year, worldwide, between 250,000 and 500,000 people suffer from a spinal cord injury (SCI), as shown by the World Health Organization [1]. SCI causes motor, autonomic and sensory dysfunction, this being the loss of communication between the central and peripheral nervous systems, which determines this clinical condition. It has been shown in clinical reports that SCI not only affects the central nervous system, but also affects the peripheral nervous system. In patients with SCI, the abnormal response of the needle electromyography (EMG) manifests positive acute waves and potential fibrillation, indicating peripheral alteration as reported by Tankisi et al [2]. In patients a complete clinical examination (muscle strength score, sensitivity level, and reflexes) could determine central, peripheral, or mixed injuries. All these patients present significant weakness or paralysis below the lesion, but also present some simple clinical differences such as the flaccid or spastic limb. On the other hand, leuprolide acetate (LA), a gonadotropin-releasing hormone agonist (GnRH), has been reported to have neurotrophic properties, improving sensory and motor functions in patients with chronic SCI [3]. Among the advantages of LA administration is that it can be systemic, it can cross the blood-spinal cord barrier and present few side effects [4]. The aim of this study was to analyze whether electromyography and clinical variables improved with treatment with LA in a patient with SCI.
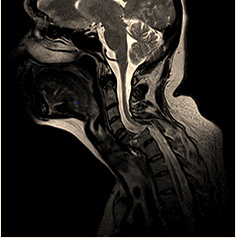
A 38-year-old woman had a car accident and the MRI findings showed loss of bone continuity with severe compression of the spinal cord at C5, dislocation from C4 to C7 and section of the C6- C7 spinal cord. With neurosurgical treatment, an anterior plate and an autologous hip graft were immediately placed to reconstruct the damaged vertebral body (Figure 1), tracheotomy and reconstruction of the left arm were also necessary. After the operation, she was transferred to the intensive care unit, the complete section of the spinal cord at level C6 was diagnosed and two months after hospital clinical care, rehabilitation therapy began.
Figure 1: MRI image from patient, 38-year-old woman a year later after suffering a car accident. Sagittal T2 weighted shows injury site and frontal plate from C5-T1 position.
The subject was invited to voluntarily participate in this study. Before the initial evaluation, she signed an informed consent letter, and all of her questions or concerns about the study were clarified. This research was approved by the Bioethics Committee of the Autonomous University of Aguascalientes.
One year after the car accident, EMG and initial clinical evaluations were performed. Six months after these initial evaluations, when no changes were observed due to rehabilitation, treatment with LA started and consisted of an intramuscular injection (7.5 mg) each month during six months. At the end of this time, the EMG and clinical signs were reevaluated (final evaluation). All evaluations were performed by a blinding rehabilitation doctor, which persists in all studies.
Clinical evaluation showed a complete spinal cord injury in C6. The muscles of the upper extremities obtained 1 or 2 points, including the hands, the rhomboids and the biceps possess a force of 3/5 (Table 1). There was no functional movement of the arms. She was completely dependent on all activities of daily life (drinking water through a straw). Surprisingly, the abdominal muscles contracted 1/5 of the scoring force, the lower extremities were flabby, normal sensory perception was present at the T4 level, and all extremities were hyporeflexic. Initially, EMG demonstrated multiple C4 to S4 radiculopathies bilaterally. Needle electromyography shows abnormal spontaneous activities (denervation data) at C7, C8, T1, L5, S1 to S4. A reduced amplitude was observed in sensory and motor action potentials. The EMG findings correspond to an incomplete mixed lesion of the spinal cord, denoting a segmental peripheral demyelinating polyneuropathy that affects sensitive and motor function.
Table 1: Upper limb muscles evaluation obtained by motor score in the evaluations. Remarkable improvement in most muscles were present comparing initial and final evaluation.
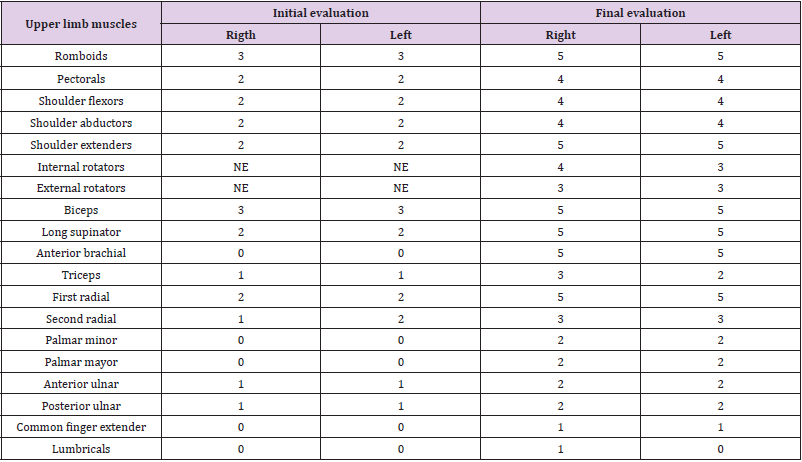
Note: * NE: No Evaluable (unassessable)
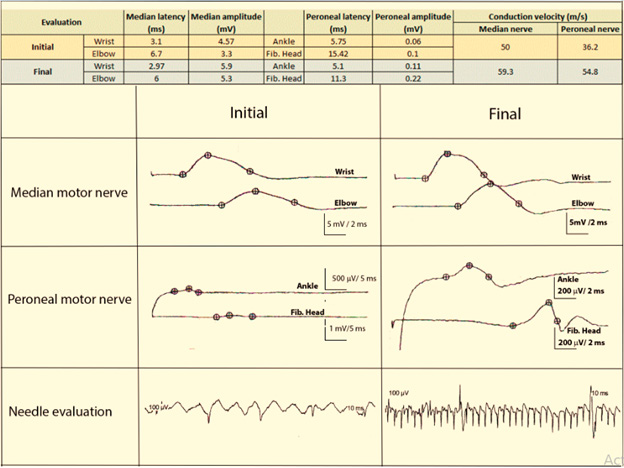
After six months of LA treatment, a new clinical and electromyographic evaluation was performed. The results indicate that the muscles of the upper extremities had greater strength and another different muscle showed contraction (Table 1). The abdominal muscles obtained a force of 2/5, the lumbar square and the iliac psoas obtained a noticeable contraction. The sensitive level persists in T4, the hyporeflexia in four extremities was maintained as in the beginning. The improvement in strength gradually increased after the second administration of LA. Functionally, the patient could eat with a spoon, drink a glass of water and was able to sit straight in bed. The EMG results show a greater amplitude and latency, while the values of both sensory and motor action potential decrease. The denervation activity was intensified for all the muscles evaluated (Figure 2). The perception of pain was significantly intensified with the electrical stimulus, triggering an exacerbated response in the patient.
Figure 2: Representative action potential comparing results observed at initial and final EMG. A representative figure was placed because changes were present in almost all the muscle analyzed. Notably, amplitude increase comparing initial and final action potential, latency decrease, and velocity conduction is greater in sensitive and motor nerves. Needle evaluation exhibits the presence of more positive waves with an increased muscle activation.
In this study, it was found that the patient with SCI treated with LA showed a clinical improvement directly associated with EMG changes. An increase in the velocity of nerve conduction and the amplitude of the action potential was observed. It is probably due to the fact that a greater number of activated axons responded to the stimulus and, therefore, to a greater activation of the motor units with a consequent greater force muscle contraction. Therefore, it was found that intramuscular injection of LA increases the contraction force of the upper limb muscles in the patient with SCI. It has been reported that the systemic injection of LA every month for 6 months in patients with SCI, induces a significant improvement in motor, sensory and functional independence [3], being that LA is able to cross the blood-brain barrier [4]. In vitro experiments with culture of rat embryonic spinal cord neurons, it has been observed that incubation with GnRH induces a significant neuritic growth, as well as an increase in the expression of neurofilaments presenting a neurotrophic effect [5]. Likewise, the administration of LA improves the neurogenic bowel conditions caused by spinal cord injury in rats, indicating an effect on the peripheral nerve [6]. According to this background, it is possible that the treatment with LA induces a recovery in the peripheral nerves through the trophic effect on the neurofilaments, since these determine the axonal diameter and thus increase its conduction velocity. There are few treatment options for patients with chronic SCI. The application of trophic factors alone or together with other factors provides some improvement. Although, with significant side effects after administration or high risks related to the procedure and the site of application since most of them cannot cross the bloodbrain barrier if administered systemically [7,8]. In conclusion, LA administration in a patient with SCI improved muscle strength in the lower extremities, as well as action potentials generated in involved muscles and nerves. These results are important because they offer an accessible pharmacological strategy that can improve the quality of life of patients with SCI.


