Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Recep Öztürk*1, Ömer Faruk Ateş2, İsmail Burak Atalay1, Yaman Karakoç1, Güray Toğral1, Mesut Mısırlıoğlu1, Emin Kürşat Bulut1, Mehmet Akif Şimşek1 and Yusuf İkbal1
Received: January 08, 2019; Published: January 17, 2019
*Corresponding author: Recep Öztürk, Department of Orthopedics And Traumatology, Turkey
DOI: 10.26717/BJSTR.2019.13.002367
Musculoskeletal tumors are rare, but orthopedic surgeons should always consider tumors in differential diagnosis in patients with suspicious or persistent symptoms. Because survival in malignant tumors depends on the stage at the time of diagnosis. Although a malignant mass can be resected in the early period, amputation may be the only option in the late period. If the algorithm is always considered respectively history, physical examination, radiology, malignancy, it should be in the form of staging and histopathological diagnosis.
The first stage of the evaluation is the history of the patient and physical examination. The most common forms of complaint are pain, swelling, limitation of movement, pathological fracture, muscle atrophy and deformity. Patients may apply with complains such as pain (usually in the form of bone lesions), palpable mass (usually in soft tissue lesions) or other lesions that are found incidentally. The history of pain or soft tissue mass and the history of trauma or severe exercise should be questioned. The character of pain should be examined. A mechanical pain increases with trauma and decreases with resting, whereas tumoral pain is usually blunt and continuous. Resting pain and night pain, palpation or increased pain with mild exercise may suggest the malignancy. A malignant tumor may initially have increased pain with activity, with progression of resting / night pain may begin. Also, if a benign lesion has damaged the cortex, it may be painful with activity. Infection may also have a high degree of pain proportional to its severity. Although painless soft tissue mass may suggest a benign lesion, malignancy cannot be excluded [1].
How long the soft tissue mass has existed and trauma history should be questioned. Lesion myocytestarting with acute with a history of rapidly progressing trauma considers ossification. A patient with a history of trauma may have a painless soft tissue mass that was previously present. A rapidly growing painful soft tissue mass may consider malignancy, but may also exhibit similar clinical manifestations of infection, inflammation and bleeding. When patients with malignancy-related fractures are questioned in detail, they often indicate that they have mild to moderate pain in the area before the fracture. In the evaluation of soft tissue masses, even if the lesion is small and painless, when specific diagnosis cannot be made, potential malignancy should be considered and should not be observed only. One of the most important information acquired in the history is age because most tumors occur at a certain age range and at a particular location.
Primary bone tumors are usually seen at a young age and often involve the appendicular skeleton, especially around the knee. Over 50 years of age, metastases and multiple myeloma are common and frequently involve the axial skeleton. Lytic lesions seen in 20-30 years of age are usually benign.
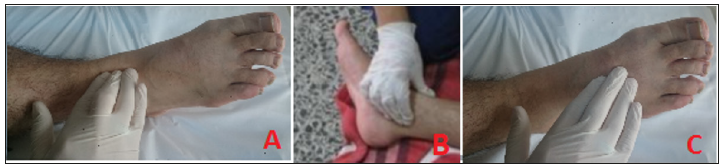
In physical examination, the size of the mass should be measured, and also localization, shape, consistency, mobility (presence of adherence to deep tissues), presence of sensitivity, presence of local heat increase, circulatory examination and presence of neurological field should be examined in detail (Figure 1). In soft tissue masses, which are considered as malignancy, the potential localization of lymph node metastases should be evaluated. In addition, general physical examination should be performed, for example, in the case of neurofibromatosis, cafe-aulait stains, neurofibromas or mafucci syndrome may help in the diagnosis of skin hemangiomas [2]. Benign soft tissue masses are often superficial, whereas malignant soft tissue masses are often located in deep tissue. Although the rapid growth of a lesion is suspicious in the direction of malignancy, malignancy cannot be excluded in a long-standing, slow-growing soft tissue mass. Family history can be helpful in multiple hereditary exocytosis, multiple hereditary enchondroma, neurofibromatosis.
Figure 1: Examination of tibialis anterior artery(a), tibialis posterior artery(b) and dorsalis pedis artery(c).
In musculoskeletal lesions, age and radiography often provide important information because many tumors have a tendency to appear in certain age ranges and in certain places. The most obvious example; in an incomplete patient with a skeletal maturation, the epiphysis lesion is most likely chondroblastoma, while the completed patient is probably a giant cell tumor. Osteomyelitis, round cell tumors (ewing sarcoma, leukemia, lymphoma, myeloma) are usually located in the diaphysis and intramedullary, while other malignant tumors are often metaphyses. In all suspected bone and soft tissue lesions, a direct radiography should be performed. It is a easy, inexpensive, fast examination. Although it is not definitively diagnosed, X-rays may give serious clues in evaluating the benign / malignant distinction of bone lesion and determining its aggression. In addition, some lesions such as bone infarction and intraosseous ganglion can be diagnosed by direct radiography, and no biopsy is required. Early bone lesions with direct radiography can be demonstrated by MR, CT, TVKS.
The superiority of the computed tomography to the radiograph was as follows: higher resolution and axial cross-sectional anatomy images. Bone involvement and accompanying soft tissue mass, if present, are very useful in the evaluation of cortex continuity. Whole body bone scintigraphy (TVKS) shows the degree of osteoblastic activity. For example, in a benign blastic bone lesion, minimal activity increase is observed in the localization, while in metastatic involvement, warm involvement is obtained. The lesion cannot precisely determine its limits [3]. Although it is widely used to detect skeletal metastases and to evaluate the efficacy of chemotherapy, it can be used to assess the activity of a suspected lesion and to detect the presence of multiple lesions. As a general rule, its sensitivity is high and its specificity is considered low. Magnetic resonance imaging (MRI) is excellent in demonstrating the size and anatomical relationships of lesions in bone and soft tissue tumors. It replaced the angiography, myelography, and arthrography with the ability to demonstrate relationships with vascular nerve structures. MRI is the best examination of bony extravasation of bone tumors. It is also very successful in detecting skeletal metastases and in posttreatment follow-up. Its superiority against direct radiography and tomography is that it contains coronal, axial and sagittal series and does not contain radiation. However, without a direct radiograph, tumor interpretation with MRI is very risky (Figure 2).
Ultrasonography (USG) is non-invasive and inexpensive. it is generally used for the determination of the localization of a superficial soft tissue lesion, its size, its relationship with the surrounding structures and its separation of solid-cystic. USG cannot differentiate benign-malign. Doppler USG can be used to obtain information about the blood supply of the mass. Lesions that can be diagnosed frequently with USG are ganglion, abscess, bursitis, lipoma, hemangioma and synovial cyst.The diagnosis of Achilles xanthoma is usually done with USG. In deep-seated soft tissue masses, usg-guided biopsy can be performed. It is very valuable in the evaluation of the collections after wide resection. Angiography can be used to determine tumor vascularity and to differentiate benign malignancies, but some benign lesions such as hemangioma may also be hypervascular. Angiography is currently used in preoperative embolization of lesions with high vascularity (the most common aneurysmal bone cyst, renal cell carcinoma metastasis). PET-CT, detection of primary or metastatic disease, early evaluation of response to chemotherapy-radiotherapy, determination of soft tissue metastases as well as bones are their superiorities. PET-CT has been used frequently for screening because of its ability to catch metastasis and recurrence early [4].
Complete blood count can be helpful in diagnosing leukemia and infection. ESR is normal in high tumors of infection, but it can often be elevated in histiocytosis in metastases and small blue round cell tumors (ewing sarcoma, leukemia, lymphoma). Serum protein electrophoresis is also used in multiple myeloma. Prostatespecific antigen is examined in prostate carcinoma. Hypercalcemia can be seen in metastasis, hyperparathyroidism (Brown tumor) and multiple myeloma. Alkaline phosphatase may be elevated parallel to recurrence in previously diagnosed osteosarcoma. LDH is prognostic in Ewing’s sarcoma. Which lesions should be biopsied and what should be considered when performing a biopsy? No biopsy is indicated in most bone and soft tissue lesions. Lesions that are asymptomatic, do not damage the bone cortical integrity (without any significant fracture risk) and have benign characteristics in the radiological evaluation are followed. Certain tumors, such as osteochondroma, fibrous cortical defect and simple bone cyst, can be seen as long as there is no risk of pathological fractures and asymptomatic [5].
However, the clinical and radiological evaluation of the lesion may not be differential, even if it is asymptomatic and slowly growing, biopsy is indicated. Generally, subfacial, painful, fast-growing lesions require a biopsy diagnosis. Biopsy in musculoskeletal tumors is perceived by many patients, clinical doctors and surgeons as simple, easy and low risk. However, biopsy of the appropriate localization of the appropriate technique with a preoperative full planning of the patient significantly affects the prognosis. Biopsy should be taken by an orthopedic surgeon who deals with musculoskeletal tumors. The surgeon should be able to recognize a lesion occurring in the bone and soft tissues, to have a differential diagnosis about the etiology, to complete the history, examination, imaging and laboratory tests and to have the knowledge and experience to give biopsy / follow-up decision. Malignant tumors spread along the skin incision-lesion. The surgeon should be familiar with all standard and non-standard incisions of the extremity sparing surgery / amputation after biopsy diagnosis. The surgeon must plan an incisional biopsy with a final operation incision and resectable biopsy tract with wide borders.
Malignant lesions should be referred to a specialist center. In this center, after the diagnostic tests and staging tests, appropriate localization and technique should be determined and then biopsy should be done.
Figure 3: In order to perform a biopsy from a lesion around proximal humerus, the incision must be made through deltoid muscle fibers but not via conventional deltopectoral clivage so that in the case of a malignancy we can sacrifice not both muscles but only the deltoid muscle.

The main reasons for preoperative imaging and staging are negative effects of MRI and bone scintigraphy due to surgical changes in tissues, determining the treatment to be applied by screening the whole body and determining the optimal localization and biopsy type for biopsy. A biopsy made without knowing the rules of biopsy may contaminate soft tissues. This procedure may cause wound closure difficulties after the final surgery due to the necessity of removing all contaminated tissues in the limb sparing surgery, large flap / graft requirement or single option amputation. And it may even endanger the patient’s life (Figure 3). Closed Biopsy; needle aspiration biopsy; or core needle (tru-cut or jamshidi). True-cut biopsy can be taken from palpable soft tissue masses. The best area of use is large soft tissue masses, away from major vascular structures.
The advantages compared to open biopsy are minimalinvasive, low risk of contamination, lack of wound healing and can be performed under local anesthesia without operating room conditions. Its diagnostic value is very close to open biopsies. The advantage of open biopsy over closed biopsy methods is that a greater amount of material can be taken, so that the diagnostic accuracy increases and the subtyping can be performed. it is the highest diagnostic value of biopsy. The general approach is to open and recommend open biopsies in all lesions. Its disadvantages are the necessity of anesthesia, prolonged duration compared to closed biopsy, risk of contamination, increased risk of pathological fractures in bone lesions of infection, hematoma and bone window. While biopsy from the bone lesion, a biopsy from the least differentiated area and the least mineralized area in radiological examination is recommended. The shortest possible length of biopsy can be used. The larger the incision track, the greater the tissue to be removed in contaminated tissue and final operation. The lesion should be reached by the shortest and most straight line possible, perpendicular to the tissue. The advantage of this is to allow as little tissue / compartment contaminants as possible.
The lesion should never be reached from inter-muscle / compartmental cleavage. The lesion should be reached by contaminating the single muscle / compartment while reaching the lesion directly. As a classic example, a lesion from a lesion in the proximal humerus should be reached from the lateral, deltoid fibers, not by deltopectoral incision frequently used in orthopedics. So that we sacrifice only the deltoid muscle, not the two muscles in the possible malignancy (Figure 4). Thus, the hematoma that may develop in and after the Biopsy remains in one compartment. Hemostasis should not be neglected throughout the case and at the end, it should be considered that tumor cells can be spread by hematoma. If there is a risk of hematoma, a drain must be placed. The tip of the drain should be removed from the immediate end of the long axis of the incision as close to the incision as possible and in the same direction as the incision. After the biopsy is taken, all floors should be planted tightly. this method prevents local spread as much as possible. Sutures with wide extension should not be used in the skin suture. When performing biopsy, significant vessels, nerves, tendons should not be seen at all. Before the biopsy, radiographs should be evaluated in this respect and incision should be made from the most guaranteed site. The contamination of these structures makes the final surgery extremely difficult. If the lesion is both soft tissue and bone mass, biopsy should be taken from soft tissue if possible.
Figure 4: Chondromixoid fibroma on proximal tibia, a. direct x-ray b. clivage towards the lesion after incision c. macroscopical view of the lesion d. the view of tumoral region after curettage.
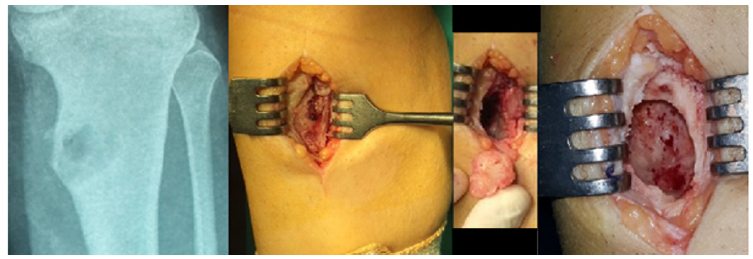
Treatment of bone and soft tissue tumors, particularly malignant tumors, requires a multidisciplinary approach involving the experienced orthopedic surgeon, pathologist, medical oncologist, radiologist and radiation oncologist.

