Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
N Yu Klimov* and AV Andreychikov
Received: August 10,2018; Published: August 24,2018
*Corresponding author: S Nikolay Yu Klimov, Department of Urology, Andrology and Sexology, Krasnoyarsk State Medical University,KGBU "Krasnoyarsk Regional Clinical Oncology Clinic named after AI. Kryzhanovsky, Russia
DOI: 10.26717/BJSTR.2018.08.001637
One of the most common oncological diseases in men is prostate cancer (PC). According to the frequency of occurrence among the causes of cancer death in men, it ranks second to bronchogenic lung carcinoma [1]. During the last 30 years, the incidence of prostate cancer increased significantly worldwide. Moreover, a change of the existing paradigm takes place at the present moment, according to which prostate cancer is highly androgen-dependent disease [2].
Objective: To establish the most common somatotype of patients with prostate cancer (PC) according to the index of Tanner and Rees-Eysenck body index.
Tasks:
a. To carry out anthropometry;
b. To compare the incidence of somatotype identified by Tanner and Rees-Eysenck indices in the group of patients with PC and healthy men of the same age;
c. To determine the Quetelet index in patients with prostate cancer and healthy men.
42 patients with morphologically confirmed diagnosis of prostate cancer were examined in the urology departments of Krasnoyarsk hospitals. Age of the patients - 46-91 years (middle age 69,3 ± 2,6). Standard anthropometry was made for all of them in 27 parameters [3-5] with the calculation of osteometric indices of Rees-Eysenck [3-4] and Tanner according to the known formulas [3,4,6]. Anthropometric data taken from the healthy men of the same age were used as a comparison group [5]. Statistical data management was made using the Student's test and x2. Differences were considered significant by criteria t (Student's test) and x2 at p <0.05 [7,8].
Figure 1: Comparison of the incidence of somatotypes according to the Rees-Eysenck index among patients with prostate cancer and male population.
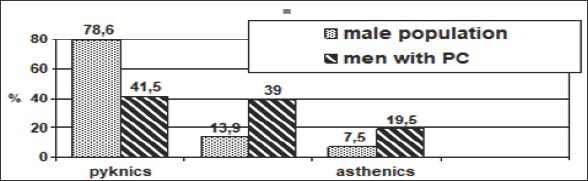
Determination of patient somatotype by Rees-Eysenck index showed that men of pyknic type suffering from PC made up 41.5%, normosthenic type -39%, asthenic type - 19.5%. When comparing the frequency of patient somatotypes and men of the population there is a significant difference. These comparisons are shown on (Figure 1). By distributing the patients into the somatotypes by index of Tanner - the index of sexual dimorphism - it was found out that gynaecomorphic males amount 65.6%, mesomorphic ones - 31.8% and andromorphic group made up 2.6%. Compared with the population norms - a striking contrast. Among the patients gynaecomorphic males prevail and andromorphic males are virtually absent (Figure 2).
Figure 2: Comparison of the incidence of somatotypes according to the Tanner body index among patients with prostate cancer and male population.
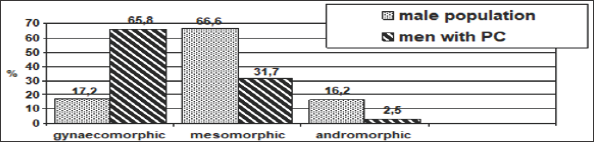
According to the foreign literature patients with PC, in comparison with male population are obese (Fontana S.L, et al.,2009; Moorthy K. et al. 2008). In our opinion, in recent times a wide spread attempt to explain that carcinogenesis is caused by food conditions in respect of prostate cancer is untenable because while comparing body mass index (BMI) of patients with prostate cancer we obtained the following results: patients with PC have BMI = 26, 51 ± 0, 62. When compared with the population data (BMI = 25,6 ± 0,23; P> 0.05) there are no differences! Conclusion: patients with pathology of the prostate and men population are equally overweight.
a. Among patients with prostate cancer gynaecomorphic and mesomorphic males are found predominantly but gynaecomorphic somatotype is the most frequently occurring. Mesomorphic type dominates among male population. Consequently, estrogens / androgens ratio is of direct relevance to the etiology of prostate cancer.
b. According to our findings: the more developed male characteristics (masculinity), the less prostate cancer probability.
c. According to the body mass index, patients with PC do not differ from the male population, and therefore, excess food and obesity have no relation to prostate cancer.


