Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Matar Khaled*1, Matar Mohammed2, Helal Ayman1, Abo Jazr Iyad1 and Al nahhal Mousa1
Received: March 19, 2018; Published: April 06, 2018
*Corresponding author: Khaled Matar, Gastroenterology department, European Gaza hospital, Khan Younis City-Alfukhari, Gaza Strip-Palestine, southern Gaza Strip
DOI: 10.26717/BJSTR.2018.03.000927
An endoscopic or radiologic percutaneous approach may be an initial minimally invasive method for treating biliary strictures after living donor liver transplantation. However, cannulation of biliary strictures is sometimes difficult due to the presence of a sharp or twisted angle within the stricture or a complete stricture. The rendezvous technique can be used to overcome this difficulty. Herein, we report a modified rendezvous technique in for a patient with duct-to-duct anastomotic complete stricture after liver transplantation.
Keywords: Liver Transplantion; Bilo Pleural Fistula; ERCP; PTBD
Abbreviations: LDLT: Living Donor Liver Transplantation; ERCP: Endoscopic Retrograde Cholangio Pancreatography; PTBD: Percutaneous Transhepatic Biliary Drainage
A 55-year-old male was referred to our unit with abdominal distention, jaundice, pancytopenia and fatigue for 2 months. He had been followed at the Gastroenterology clinic and had been worked thoroughly for pancytopenia, jaundice and splenomegaly [1] . Gastroscopy was carried out which showed grade 2 esophageal varices. Meanwhile he was diagnosed as having Hepatitis B related cirrhosis based on laboratory tests showing impaired hepatic synthetic and excretory functions along with positivity for hepatitis B surface antigen and detectable hepatitis DNA by quantitative PCR [2] . Then, upon further evaluation at the gastroenterology clinic he was found to have MELD scare of more than 15 which qualifies him for listing for orthotopic liver transplantation. Meanwhile, he started having more abdominal discomfort mainly postprandially, early satiety, progressive abdominal distension and pedal enema for which he was put on diuretics [3]. He did not complain of altered sensorium suggesting hepatic encephalopathy. On examination in our unit: He had pallor, mild citrus and mild pedal enema; his blood pressure was 124/ 80 mm Hg PR: 90 bpm. Abdominal examination showed shrunken small liver, splenomegaly (>4cm), and shifting dullness suggestive of Ascites. Investigations revealed haemoglobin of 9gm/dl, total leukocyte count of 3200, platelet count of 65-105/, INR: 2.1 Liver function tests revealed serum bilirubin of 5.4 mg/dl, aspartame aminotransferase of 81 IU/ml, alanine aminotransferase of 54 IU/ml, alkaline phosphatise of 164, and serum albumin levels of 2.5 g/dl with globulins of 3.5 g/dl. Ascitic fluid analysis was wide gradient and there was no SBP. Her hepatitis B surface antigen was positive while ant hepatitis C virus antibodies were negative [4].
An ultrasound Doppler revealed shrunken liver with coarsened echo texture (13.6cm) and all three hepatic veins were patent. Also, there was no CBD dilatation and no intrahepatic biliary radicals dilatation. He had splenomegaly and splenic vein was 14 mm in diameter. There was moderate ascites and multiple spleno-renal collaterals were present. The final diagnosis was Hepatitis B related advanced liver cirrhosis Gastroscopy was carried out and showed evidence of Grade II Esopahgeal varices, mild portal hypertensive Gastropathy but no Fundal varices. After full evaluation he was referred for orthotopic liver transplantation. He was listed for OLT in Egypt, where he underwent the OLT successfully in March 2017 [5].
He came back to Gaza Strip in august 2017, where he was evaluated upon arrival in the gastroenterology clinic. His lab studies showed a dramatic improvement in hepatic synthetic and excretory functions with the following parameters detected; WBC's:4.5, Hgb: 11, Platelets: 220, AST:45, ALT: 40,ALP:157, Albumin:3.9, T.Bilirubin: 1.2, Tacrolimus Blood level: 9.3. He was maintained on the following postransplant medications: Mycophenolate Mofetil, Tacrolimus, Deptrin DS tab and valgancyclovir. Upon re-evaluation at follow up visit one month later, he was found to be jaundiced with disturbed liver function tests and T. Bilirubin of 7 [6]. MRI with MRCP was carried out which raised a suspicion of prospective anastomotic stricture. He was admitted and kept on broad spectrum antibiotics, yet, he started having progressively deepening jaundice , intractable itching, fever and raising kidney function tests. Hence, the decision was to proceed to ERCP in order to avoid the fatal outcome of ascending cholangitis.
Figure 1: A Guidewire passing through the ampulla was captured by a snare and then withdrawn through the endoscopic working channel.
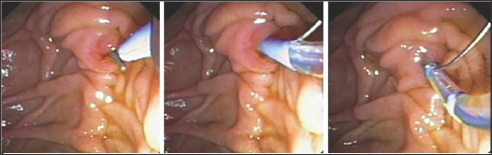
Figure 2: A tight Anastomotic stricture by percutaneous injection.

During ERCP cannulation was performed using standard method and accessories. The distal CBD was of a diameter of 0.8 cm and a tight stricture almost at the anastomosis where the guidewire could not be passed more proximally through the very tight stricture by any means [7]. So, the decision was to proceed with Rendezvous procedure with the aid of interventional radiologist. The percutaneous puncture was performed aided by ultrasound and access was gained into the mildly dilated right hepatic bile duct. The guidewire was introduced through the right intrahepatic duct through the anastomosis, where after few trials the wire had been passed through the stricture into CBD then out of the ampulla of vater. Then, using the duodenoscope the wire coming out the ampulla of vater was pulled into the scope channel and a sphincterotome was passed over the guidewire into CBD then across the stricture successfully. Finally a plastic stent of 7 F*7 cm was inserted successfully through the stricture with good bile drain. The percutaneous rendezvous procedure enabled placement of an internal-external drain [8]. One week after the procedure the patient reported having right sided chest pain along with progressive shortness of breath. The chest Xray showed a massive right sided pleural effusion. Paracenthesis revealed an exudative bilious fluid. The external drain was removed followed by replacement of a longer new internal plastic stent placement. The right pleural fluid reacumulation was diminished significantly and the patients shortness of breath improved dramatically (Figures 1-4).
Figure 3: External Drain and internal CBD stent in place.
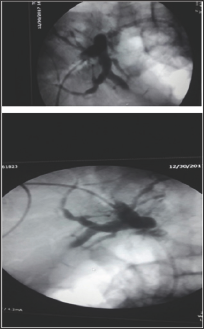
Figure 4: Post External and drain placement.

Biliary strictures are not uncommon after living donor liver transplantation (LDLT), and two-thirds of biliary strictures can be treated by endoscopic retrograde cholangiopancreatography (ERCP). If ERCP fails, percutaneous transhepatic biliary drainage (PTBD) is recommended. Although maintaining a PTBD catheter for a long period is beneficial for treating biliary strictures, it may be difficult for patients, especially in liver transplant patients, due to the development of PTBD catheter-related complications, such as leakage, pain, infection, and accidental removal of the PTBD catheter [9]. Therefore, replacing PTBD catheters with inside stents is recommended. Unexpected complications such as injury to the right pleural costophrenic reflection injury during PTBD placement resulting in a bile-pleural, can be managed either percutaneously or endoscopically.
Bile drainage can be achieved by means of a combined percutaneous transhepatic and endoscopic transpapillary approach (the rendezvous technique). Rendezvous procedure is when PTC is used to access the biliary tree in an anterograde fashion facilitating successful completion of a challenging ERCP. Randevue procedure is based upon liaison between the endoscopist and the interventional radiologist and it is a cornerstone step in achieving access into the biliary system and certain kinds of stricture when the transpapillary access or access through a tight stricture could not be achieved. Ile leak or fistula as a procedure complication can be managed in a timely manner endoscopically in a fashion similar to post cholecystectomy ile leak with sphincterotomy and stenting to facilitate bile drainage through natural route permitting healing of the leak site or the bilopleural fistula.
We would like to extend our sincere appreciation to Dr. Mohammed Matar the interventional radiologist for their assistance in the success of the randevues procedure and also creation of this manuscript.
This research did not receive any specific grant from funding agencies in the public, commercial, or non-for-profit sectors.


