Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Voranush Chongsrisawat1*, Kantida Ongasivachai1, Chidchanok Tangjade1, Netsiri Dumrongpisutikul2 and Jiraphorn Amornfa3
Received: January 27, 2018; Published: February 06, 2018
Corresponding author: Voranush Chongsrisawat, Department of Pediatrics, Faculty of Medicine, Chulalongkorn University, Bangkok 10330, Thailand
DOI: 10.26717/BJSTR.2018.02.000732
We report a 6-year-old girl who presented with intractable hiccups and epigastric pain. Gastroesophageal reflux disease (GERD) was confirmed by esophageal pH monitoring and EGD revealed an esophageal ulcer and erosion at distal esophagus. Treatment with high dose PPI failed to reduce hiccups. MRI of brain demonstrated enhancing infiltrative lesion involved floor of forth ventricle, posterior aspect of lower pons, entire medulla, cervicomedullary junction and extended down to dorsal portion of C7 cord. This report emphasizes brain tumor as the etiology of intractable hiccups leading to severe GERD. When encountering a patient with intractable hiccups, appropriate CNS imaging studies should be included in the evaluation protocol.
Keywords: Intractable hiccups; Gastroesophageal reflux disease; Esophagitis; Esophageal ulcer; Brainstem tumor
Abbreviations: GERD: Gastroesophageal Reflux Disease; CNS: Central Nervous System
Hiccup or singultus is a reflex inspiratory movement consisting of involuntary, repeated, spasmodic contraction of the diaphragm and intercostal muscles followed by abrupt closure of the glottis [1]. Hiccup is usually a self-limited disorder without any clinical significance [2], most commonly caused by gastric distension (ie. food, air), alcohol ingestion, tobacco use, or sudden changes of gastrointestinal temperatures [2,3]. Episodes lasting longer than 48 hours are defined as persistent, and those lasting longer than two months are labeled as intractable [1]. Intractable hiccups have various etiologies including vagus or phrenic nerve irritation, toxic- metabolic disorders, central nervous system (CNS) disorders, and psychogenic causes. We reported a child with intractable hiccups and severe gastroesophageal reflux disease resulting from desmoid tumor at brainstem and cervical spinal cord.
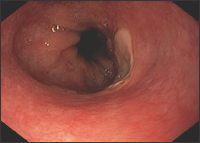
A 6-year-old girl presented with hiccups, snoring, and anemia for 2 months. Hiccups persisted throughout day and night. She also had epigastric pain, nausea, and loss of appetite. Her BW was 19.6kg (50th percentile) and height was 109cm (25th percentile). Her general medical examination revealed pallor and unremarkable otherwise. There was no papilledema. Motor, sensory, and cerebellar function were intact. Her hemoglobin was 8.6 g/dL, with normal leukocyte and platelet count. Gastroesophageal reflux disease was assumed as the cause of her symptoms, therefore she was put on 20 mg of omeprazole daily. One month later, she had hematemesis. EGD revealed an esophageal ulcer and erosion at distal esophagus (Figure 1). Her symptoms continued even she was on 60 mg of lansoprazole and iron supplement. Esophageal pH monitoring revealed a reflux index of 59% and impedance study demonstrated 65 episodes of acid reflux.
Figure 1: EGD revealed an oesophageal ulcer and erosion at distal oesophagus.
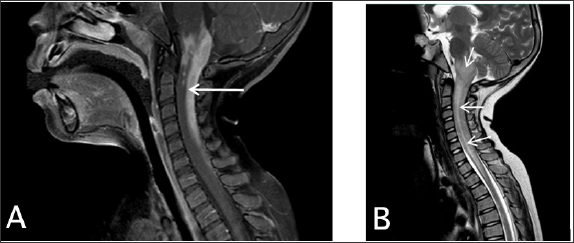
Upper GI series was unremarkable. Because of unremitting hiccups, brain imaging was conducted, and magnetic resonance imaging demonstrated enhancing infiltrative lesion involved floor of forth ventricle, posterior aspect of lower pons, entire medulla, cervicomedullary junction and extended down to dorsal portion of C7 cord (Figure 2). Biopsy revealed reactive gliosis. Her symptoms improved with radiotherapy. Subsequently she underwent complete tumor resection which revealed desmoid tumor. After 5 years, the patient is in good clinical condition without hiccup.
Figure 2: MRI showed enhancing infiltrative lesion involved floor of 4th ventricle, posterior aspect of lower pons, entire medulla, cervicomedullary junction and extended down to dorsal portion of C7 cord without leptomeningeal seeding (A: Gd-enhanced T1WI, B: T2WI).
Intractable hiccups can be caused by a disease or lesion along the hiccups reflex arc [4]. Gastrointestinal disease is the most frequent cause; about two thirds of these patients have a gastroesophageal reflux [3,5]. Atypical or extraesophageal presentations of GERD are increasingly documented and consist mainly of pulmonary and otolaryngologic symptoms. Yi, et al. reported hiccup symptoms in 55% of patients with GERD [6]. The mechanisms have been postulated as to how reflux occurs during hiccups is negative intraesophageal pressure and a reduction in LES pressure during hiccups result in movement of acid from the stomach into the esophagus resulting in esophagitis. Another mechanism is the repetitive diaphragmatic contractions that occur with hiccups resulting in increased gastric pressure, thus facilitating acid reflux. Complications of reflux such as strictures, esophagitis, and esophageal ulcer may stimulate vagal nerves that may result in intractable hiccups [7].
Intractable hiccups may result from serious pathological processes due to central nervous system disorders mostly caused by brainstem lesions such as trauma, ischemic stroke, infection, neuromyelitis optical and particularly brainstem tumor [1,3,4,8]. Hiccups have been implicated as a cause of severe reflux esophagitis [7,9]. However there has been no report of esophageal ulcer caused by intractable hiccups as our case. Therapy with potent PPI can differentiate hiccups caused by esophagitis and hiccups-induced esophagitis [3,5,10]. Brain MRI is indicated in patients whose hiccups fail to respond to high dose PPI as in our case.
Brain tumor presenting with hiccups is a rare condition in children. There have been a few case reports of brain tumor causing intractable hiccups in children. All reported patients had abnormality of neurological examination such as brisk deep tendon reflex, tongue fasciculation, and horizontal nystagmus [11,12]. This reported case had no neurological signs and symptoms and thus underwent multiple investigations for GERD. This report emphasizes brain tumor as the etiology of intractable hiccups. When encountering a patient with intractable hiccups even if the patients do not reveal any neurological manifestations, appropriate CNS imaging studies should be included in the evaluation protocol.


