Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
David J John O Regan*
Received: September 20, 2017; Published: September 26, 2017
Corresponding author: David J John O Regan, National Health Service, Leeds, Yorkshire Heart Centre, England
DOI: 10.26717/BJSTR.2017.01.000393
The consent process is a complex relationship between rational cognitive thinking and emotional processes [1] (page 62) that can alter the choices that are being made and can shape probabilities of outcomes [2]. The patient or “lay person” is presented to the cardiac surgeon “expert” by means of a referral letter from a cardiologist who in turn saw the patient following referral from a General Practitioner. Both the patient and the surgeon have a general understanding of the need to act [3]. There is an expectation of surgery but the objectives and goals of surgery have not been defined. The consent process involves clarification of those objectives, exploration of alternatives and the addition of some structure to the decision process. This, however, is subject to natural biases or “heuristics” and especially subject to framing. I hope to explore these biases from the perspective of the patient ‘lay’ customer and the consultant surgeon or ‘expert’ and examine the consultation process using prospect theories. I hope to look beyond these heuristics and offer prescriptive alternatives that may go some way towards an ideal consent.
Abbreviations : CABG: Coronary artery bypass grafts; AHA: American Heart Association; MRSA: Methicillin Resistant Staph Aureus – “fleshing eating bug”
The Ideal consent can be prescribed in normative theory that is dependent on four major criteria
a. Decidability: All the outcomes of CABG can not always be defined, especially in patients over the age of 70 and all alternatives may not be known. Both parties are assumed to be perfectly informed.
b. Transitivity: Assumes that the alternatives can be placed in order and assigned the highest expected utility. These are different for the patient and surgeon. Indeed the “connectedness” and idealisation of the state of health could be thought of in terms of “bitterness”, but it also assumes that this order of “bitterness” is stable and not subject to inter-individual preference.
c. Invariance: Assumes that the decision would be the same no matter how the options are worded. In the context of consent it is extremely easy to “put a patient off” a procedure by introducing “fright factors” such as stroke or headline grabbing infections such as MRSA. Furthermore Kahneman theorised that invariance could be satisfied if there was no difference between mortality and survival. This cannot be said of medical problems [4] especially CABG.
d. Independence: Normative theory stipulates the importance of events should not influence the judgement of the patient or the doctor on the likely outcome of cardiac surgery. Indeed the utility and probability of surgery is not independent but as I will argue are very much interdependent on both the patient and surgeon.
Furthermore this decision process must be reproduced time and again for each and every patient with the application of logic, maths and statistics. As a practising clinician however, it is extremely difficult to translate “cold maths and statistics” to the individual sitting in front of you especially in a potentially emotionally charged atmosphere. It is, therefore, difficult to see how normative theory could apply to the consent process and a more Descriptive theory is required. I would therefore like to explore this from the perspective of each party and examine how the information that is presented influences the choices.
Health as a utility is relative to a previous state of health, experience, family and occupations [5] (page 322). It is difficult to define but is reflected in activities such as leisure, socialisation,business and family affairs. This should all be taken into account in a medical history of lifestyle. The patient’s beliefs about the next periods and state of health will affect perception of utility and function. It may also induce anxiety and even avoidance [6]. Images marked by positive or negative feelings will also guide judgement and decision making [7]. The prospect of having heart surgery is frightening and the limited time afforded in NHS clinics may induce affective choices whilst at the same time reducing analytical deliberation [7]. There will be a period of fear of the unknown and therefore the attractiveness and affected responses are also going to be very subjective [8]. There is certain inevitability about this process that is associated with the desire for certainly “I will be alright won’t I doctor?” and an over confidence in one’s surgical ability “I have every trust in your doctor”.
Figure 1 : Graphic representative of a patient’s state of health. The state of health as perceived by the patient is represented on the Y axis. The X axis represents the time - this could be the duration of illness or life span from youth to old age. There is a slow deterioration over time that is tolerated. Patients describe themselves as “not too bad” for long periods of time. There is a point where a patient becomes ill. This is usually related to some family, social or other event. Following this, a degree of “loss or deterioration” is steeper and more significant than the health gain. The patient’s reference point regarding their health can be anywhere along this line and not too infrequently they remember their fitter years associated with being young.
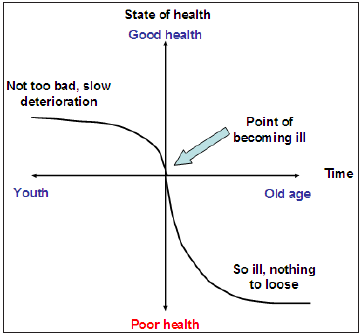
The decision to have surgery is not without uncertainty. The prospect of an operation is difficult to imagine. Often the availability of information is diminished unless they have recent knowledge of another person who has had the operation. Patients are therefore very likely to be risk averse and neglect the probability of adverse outcomes. In the first instance the patient quite frequently does not want to know, does not ask, does not see the relevance of knowing adverse outcomes and sometimes may not actually understand. On many occasion there may be an overriding emotions. On the other hand the patient may over value the treatment options and present in clinic expecting surgery to cure everything. They may not understand that other treatment options are perhaps available and demonstrate a ‘preference reversal’ [1] (page 247). During the consultation the context of possible outcomes will be described. This may affect the patient’s perspective of utilities constituting a form of Allias paradox [1] pg 248. These biases mean that patients ‘over weight’ small probabilities and underweight large probabilities [2] and neglect to consider long term outcomes [9]. On making the decision the patient is anticipating a hypothetical state [2] that is going to be evaluated as a change from a reference point. The reference point however is dependent on their state of health (Figure 1).
Patients often tolerate a slow deterioration of health over prolonged periods of time, until such stage they suddenly become ill. They feel a sense of loss to the extent that they may have nothing to lose. Losses are treated more seriously depending and as shown in the Tversky and Kahneman “Asian flu experiments” they are more likely to take a chance if they perceive their life is actually at risk. Utility decisions in medicine often assume that the total utility of the same condition over time compared to death is constant. In other words the utility per year can be considered in duration in years i.e. Quality Adjusted Life Years. The variation of the perception of utility is seen when people are asked about choosing how long they would tolerate ill health [10]. When the expected life span is short, many people give priority to living as long as possible and would take the risk [11]. Conditional framing ensues as patients disregard that they may not be operable and vote for possible survival against a background of reduced longevity [9].
Death as an event and outcome option does help force explicit decisions. Technology and advancement of medical science means quite often we can, but the question remains, should we? [12,13]. The subject of death has to be discussed openly as a possible risk of cardiac surgery if it is to retain the humanities of medicine that could be threatened by technology [13,14], particularly as the age of our patients is increasing and we are questioning the value of life [15]. The increasing age of the patient again provides another problem related to the comprehension of the complexities of procedures and the increasing inconsistency and likelihood of preferences [16]. A diminished mental capacity of patients that may hinder decision making is frequently missed [16].
Surprisingly the extent to which patients are involved in decision making does not influence a choice in hypothetical scenarios. The most important factors from a patient’s perspective are
a) being able to talk themselves
b) understanding the explanation, whatever it is
c) the quantity of information transferred
d) waiting time [17]
The status of the consultant surgeon is to date achieved following an “apprenticeship period” observing other “experts” at work duplicating and working to “rules of thumb” [18]. In keeping with other experts surgeons rely on intuition and gut feelings through the application of knowledge, experience and observation of patterns of trends and extrapolating from what is to what could be [19]. The consultant surgeon will continue to be influenced by an informal network of information exchange and socialisation with professional colleagues highlighting the importance of organisational and group culture that is also dependent on local opinions and educational directives [20]. Much of the thinking and decision processes are private and often hidden [18] and often learnt by storing and retrieving examples of similar conditions. These exemplar-based models can be enriched or calibrated, but in general this is poor in medicine and may be difficult to achieve because of retrieval limitations [21].
The consultant surgeon relies on two contrasting approaches to decision making, namely a clinical or example based decision or actuarial approach founded empirical data [22]. It is assumed the clinician uses both but if the clinical and actuarial facts do not agree a choice must be made. Research has shown that clinical choices are not as accurate as actuarial evaluation of outcome [22]. It must be noted that individual patients, rare events and interpretation of patient utility function are not included in statistical methods. Clinicians, therefore, often find exception to actuarial conclusions [22] that cannot compensate for “pattern recognition” focussed by specialisation which in itself constrains cognition [23]. The problem with medical decisions is that the consultant rarely gets immediate feedback about the criteria he or she used in making the judgements. The process therefore can often end up as self fulfilling. The judgement is shaped and probability assigned to fit that outcome. There is also a desire for certainty especially in difficult situations where the risk benefit equation is equivocal. This is translated into an over confidence, and over estimation of probability.
Figure 2 : Adaption of Atkinson’s model of experience utility as applied to a surgeon. The expected utility of success is going to be higher if the surgeon has successfully operated on a high risk case. Conversely the expected utility of failure will be similarly reduced if not more if a low risk case has died following surgery. This equates to the affective emotional rollercoaster often described by Cardiac Surgeons.
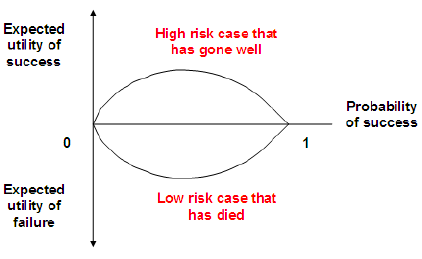
The ordering of information is going to be affected by fatigue and recent experience 22. Indeed as a surgeon one experiences a real “high” following the successful outcome of difficult surgery and a corresponding “low” if a more straightforward operation has not gone as well. For the surgeon, therefore the expected utility of success and expected utility of failure are dependent upon one another. This will certainly influence the level of confidence (Figure 2). Actuarial decision making by doctors is rather alarming. Kahneman and Tversky and work by Gigerenzo highlight the common errors and cognitive short cuts taken by physicians in interpreting data [24]. These fall into three broad categories,Representativeness: sample size, prior probability and frequency are ignored. There is also an expectation of an ordered outcome to random processes and a failure to recognise regression to a mean. Evidence therefore will be open to misinterpretation. Furthermore the relationship between correlation and causality is ignored.
i. Availability: the ease with which the surgeon can retrieve information whether it is vivid or imagined will also affect the decision process. Frequently the decision to operate or not operate starts in the form of a generic template and subjective estimate of probability and utilities [25].
ii. Anchoring and adjustment: Probability is used as an initial anchor and then adjusted accordingly up and down in light of the surgeon’s own knowledge and experience [26]. Validity and correlation is questioned. Hindsight, elusions, base rate fallacy and conjunction with fallacy (i.e. the probability of conjunctions being higher than constituent events) are other sources of error.
Figure 3 : Complications following cardiac surgery represented in a matrix of “fright factors”. Stroke is most feared. This carries a high dread and high unknown factors and if introduced into conversation can easily be risk aversive. Similarly MRSA achieves a high dread factor in view of the fact that this “flesh eating bug” is repeatedly reaching the headlines. Other complications following surgery including infection and bleeding will fall into the low dread, low unknown category and are largely accepted by the patient.
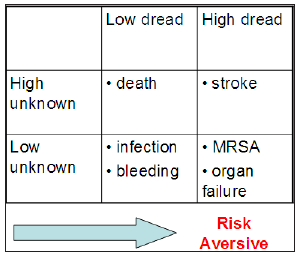
Complex decisions are being made in partial ignorance [27] using pieces of information that are clouded with uncertainty [28]. The way information is presented will affect how it is interpreted [29]. A doctor can increase or decrease a patient’s commitment to a course of action by a playing respective positive and negative heuristics for example emphasis on a complication can elicit fright response (Figure 3). Kahneman and his experiments used problems where lives would be saved or lost [9]. In a similar respect a surgeon is able to frame outcomes as severe gains or losses using positive and negative heuristics. This could be likened to the elusion of executive control in so far as the doctor knows best [3].
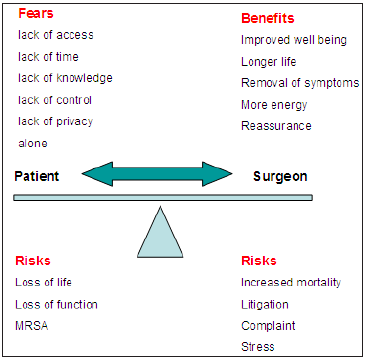
The consultation brings a lay patient and an expert surgeon together in time and place. Surgeon ‘expert’ brings science evidence and experience into the consulting room. The patient offers situation, family history, personal beliefs and more increasingly evidence [30]. The relevant influence of the doctor and the patient is summarised (Figure 4). It is dependent on perceived knowledge, assertiveness and loss of control and assessment of each other’s abilities [31]. Each party brings to the consultant natural heuristics as outlined above together with fears, expectation, benefits set against a background of risks as outlined (Figure 5).
Figure 4 : Relative influence of patient and doctor. The complex interaction between a physician and patient is a balance of powers, assertiveness and control represented in this diagram.
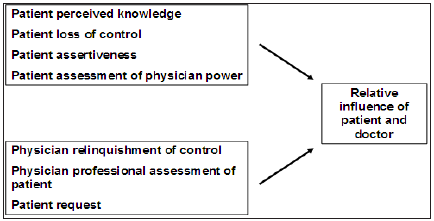
Figure 5 : The fears, benefits and risks for patient and surgeon. The fears and benefits of the patient and surgeon are shared. Their perceptions however are different as are their risks.
The consultation is dependent on open communication and the complex area of trust. It is not only dependent on the professionalism and reputation of the surgeon but also an expressed empathy and history of previous encounters as well as a willingness of the physician to relinquish “control” [31] (Figure 6). The decision making should be shared [32]. Options and outcomes should be clearly stated and patients helped to personalise information through a process of guidance and coaching. Many decisions are not clear because the probability of outcome and failure are scientifically uncertain or unknown to the surgeon and they are insensitive to the values of individual patients.
Figure 6 : Graphic representation relationship between patient and surgeon. This is a relationship that is built on trust and open communication. The surgeon brings to the relationship science, evidence, experience and knowledge of outcome which will help he or she determine probabilities. The patient likewise brings to the clinic situational family backgrounds and inherent beliefs. These can be regarded as utilities or values as determined by the patient. Increasing IT knowledge of disease processes are enabling patients to assimilate their own evidence.
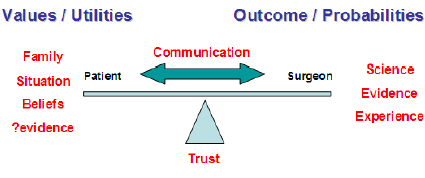
Figure 7 : Negotiation matrix. The negotiation between a patient and doctor can be represented as doctor and patient losses and gains. The ideal outcome from the consultation is a doctor gain, patient gain. Patient gain, doctor loss should indicate surgery but we are working in an increasingly litigious society. Likewise a doctor gain, patient loss should not occur. Ethical guidelines, professional conduct and clinical governance regulate this scenario.
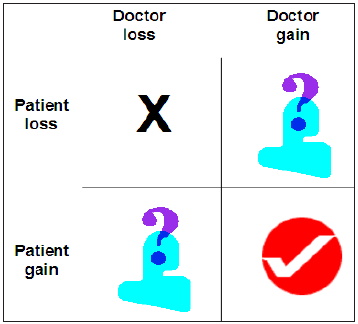
In the crudest sense the consent process could be considered as bargaining formulated as gains or losses [33]. If the decision falls within the domain of losses, it is risk aversive, where it is in the domain of gains, it is risk seeking (Figure 7). The surgeon can be seen as contributing to the Y axis of probabilities and the patient an authority of their own utilities represented on the X axis (Figure 8) i.e. the expert has a narrow quantitative view and the patient a wider view [34]. Prospect theory could thus be applied (Figure 9). Responses to losses or fear of losses would be more than in the equivalent or prospective health gains. This would be different for both the surgeon and the patient (Figure 10).
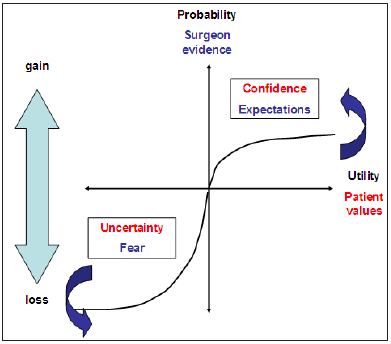
Figure 8 : Prospect theory applied to patient, surgeon relationship. The patient introduces utilities or values with a concomitant hopes, expectations, fears and losses. The surgeon introduces probabilities on the Y axis learn from experience enhanced by confidence and guarded against address outcome.
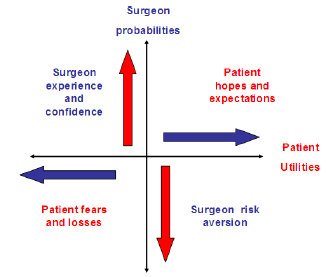
Figure 9 : Prospect theory applied to patient, surgeon relationship. Gains and losses are governed by confidence expectations, uncertainty and fear. Potential losses will be risk aversive, potential gains risk seeking.
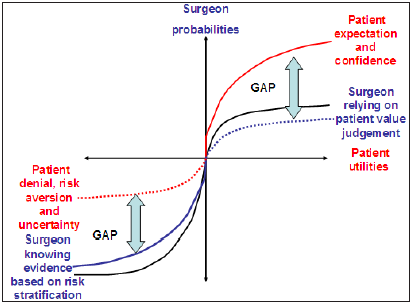
Risk aversive behaviour and positive heuristics of the patient would result in lesser expectations of loss and higher expectations of restoration of health. The surgeon will have a more realistic opinion of outcome based on risk stratification and would perceive a greater loss. The surgeon can only make a value judgement of patient’s interpretation of utilities. As seen in the diagram, interpretation of benefit and losses is similar, although on either side of the reference point is a potential gap between the patient and the surgeon. Over weighting of small probabilities and under weighting of larger probabilities does occur [2,9].
Figure 10 : Gaps between surgeon and patient as viewed with prospect theory. The natural heuristics of a patient and a surgeon mean that within prospect theory “likes” differ for the patient and surgeon their averse to risk, and uncertain and denies inherent risks. They usually have high expectation, confidence and trust in the surgeon. The surgeon conversely accepts the evidence based on risk stratification and can determine the accurate mortality and potential loss of intervention. He is however unable, especially in elderly patients, to make a value judgement of potential gains. The surgeon has to rely on the patient’s interpretation of their own utilities. These uncertainties for both the surgeon and the patient are represented by dotted lines. There is a potential gap between surgeon and patient, probabilities and utilities. The over confidence of the surgeon may not recognise the absolute potential loss of the procedure hence the blue line does not meet the black line.
Evidence based medicine is altering the balance of power [35] by inter disciplinary intervention [36]. The establishment of multi disciplinary teams improves the ‘connectiveness’ of patient care pathway and there by improves decision making [37]. Group discussion increases information exchange between all parties and from a patient’s point of view, information assimilated from such multiple sources will be opened up to greater scrutiny [38]. Patients resent being left out of the decision process and provision of information is a simple way of including them [39]. Information technology can also be used to get the right information to the right patient at the right time [40]. It can also be used to facilitate the decision processes [41]. Giving people information and encouraging them to write personal mission statements expressing their utilities will also help tailor treatment to individual needs [42]. It is recognised that diabetics, knowing their disease process adjust their behaviour are more participatory in their treatment [43].
During the consultation process, writing down the decision process may help remove the respective biases [44] it would certainly be beneficial in a medico legal sense! Drawing such a causal map or cognitive mapping may overcome the framing biases and provide a period of increased reflection that enables the selection of alternative treatment options by highlighting certain and uncertain facts [5]. Such a decision tree is shown in (Figure 11). The decision to operate or not operate with the potential outcome of death in the right hand column may not be appropriate as this is an event rather than a utility. Perhaps the decision tree ought to be rephrased from a utility perspective of a patient, namely prognosis and symptoms as in (Figure 12). One drawback of this method is that it may increase bias by highlighting “fright factors” and increasing dread whilst waiting for surgery. Completing decision trees can still be subject to negative framing but is it significantly better [45] especially if both parties think of gains [46].
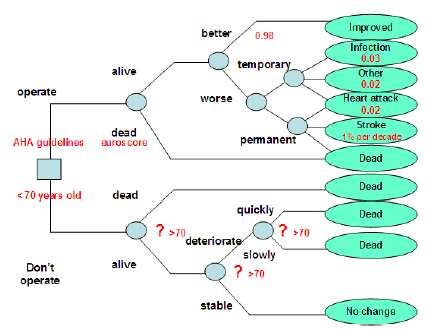
Figure 11 : To operate or not to operate decision tree. The decision to operate is outlined in the American Heart Association Guidelines. The evidence to date is pertinent to fewer than 70 year olds only and cannot be taken in an actuarial sense to apply to people over the age of 70. There is also a question mark over the long term survival of 70 year olds who do not have an operation. The decision to operate involves inherent risks. The Euro score risk stratification system is the best estimate and predictive score determining probability of death following surgery. Patients who survive surgery have a probability of improved survival and symptoms of 0.98. Permanent disability in the form of stroke following cardiac surgery is less than 1% and rises 1% per decade over the age of 70. Major morbidity in the form of heart attacks, infections, organ failure under the category of other is in general less than 3%. These obviously increase according to clinical condition and age.
The consent process needs to be more transparent [9]. Recent times have seen a change from blind trust in a doctor to a more informed and demanding patient requiring hard information and efficient quality performance [47]. Physician behaviour must change from paternalistic to more team work and participatory [47]. Multi disciplinary teams, ethics committees and inter disciplinary quality circles do accelerate and facilitate decision processes. They increase transparency, abolish power struggles, save time, remove embedded heuristics and at the same time reduce stress for both the patient and the surgeon.
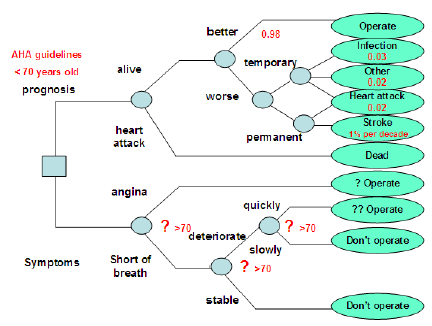
Figure 12 : Decision tree drawn according to indications for cardiac surgery. The main indications for cardiac surgery to prove prognosis as guided by the American Heart Association guidelines and to relieve intractable symptoms of chest pain. The improvement of prognosis and relief of symptoms is clear if American Heart Association guidelines are followed. This does not however apply to the age group over 70 at present and therefore the decision to operate or not to operate is problematic.
This a copy of a letter I sent to a GP after seeing a 73 year old female in clinic for consideration for cardiac surgery. She complained she felt tired and had no history of chest pain.


