Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
*Sushila B Ladumor
Received: August 12, 2017; Published: August 17, 2017
Corresponding author: Sushila B Ladumor, Consultant Body Imaging, Clinical Imaging Department, Hamad Medical Corporation, HGH, Doha, Qatar
DOI: 10.26717/BJSTR.2017.01.000281
Papillary carcinoma (PC) is the second most common type of renal cell carcinoma (RCC). PC has specific imaging and clinical features that may help in differentiation from clear cell RCC. At contrast material–enhanced CT and MRI, PC enhances less than other RCC in all phases of contrast-enhanced imaging.
Keywords: Kidney; Papillary Renal Cell Carcinoma; Renal Cancer; CT; MRI
Abbreviations: PC: Papillary Carcinoma; RCC: Renal Cell Carcinoma; CC: Clear Cell Carcinoma; CT: Computed Tomography; MRI: Magnetic Resonance Imaging; PACS: Picture Archiving and Communication System
The classification of renal cell carcinoma into subtypes is important as it has association with outcome of disease. Results have shown that renal cell carcinoma is not a single disease but, rather, a group of several disease entities [1]. According to the First International Workshop on Renal Cell Carcinoma held by the World Health Organization, renal cell carcinoma can be classified into conventional (i.e., clear cell) renal carcinoma, papillary renal carcinoma, chromophobe renal carcinoma, collecting duct renal carcinoma, and unclassified renal carcinoma [1].
Current findings reported in the literature suggest that the tumor is often hypo vascular on computed tomography (CT) and MRI [1,2], and is hypo intense on T2 weighted imaging [2]. Papillary renal cell carcinoma (RCC) is the second most common form of RCC, after clear cell RCC, accounting for 10-15% of cases [3]. In comparison with clear cell RCCs, papillary RCCs in general have less aggressive features, including being both smaller in size and lower in stage at presentation [3].
a. Morphology: The T2 weighted tumor signal was homogeneous in 57% of cases, slightly heterogeneous in 9% and heterogeneous in 34%. Eighty-nine percent of tumors were hypo intense compared to the normal renal parenchyma on T2 weighted images, 9% were hyper intense and 2% were intense. For masses imaged with MRI, the presence or absence of hemosider in was determined, defined as the subjective identification of loss of signal intensity on longer-TE in-phase images relative to opposed-phase T1-weighted dual-echo gradient-recalled echo images. Relative signal intensity in comparison with the normal renal parenchyma (i.e., hypo intense, is intense, hyper intense) was also recorded on unenhanced T1- weighted, unenhanced T2-weighted, and contrast-enhanced T1-weighted images. In addition, the presence or absence of enhancement was determined subjectively on subtraction images [3]. Diffusion restriction plays a key role in diagnosis of PC as it demonstrates remarkable restriction and shows low ADC value. Different apparent diffusion coefficients of RCC subtypes may be potentially helpful for differentiating RCC subtypes before choosing appropriate molecularly targeted drugs for patients with metastatic RCCs [4].
b. CT: The majority of papillary RCC demonstrates heterogeneous in appearance with minimal or no enhancement on nephrographic or excretory phase images, defined as an increase in attenuation of 20 HU or more between unenhanced and any series of contrast-enhanced images [3].
For the differentiation of the subtypes of renal cell carcinoma, degree of enhancement is the most valuable parameter; enhancement pattern, the presence or absence of calcification, and tumor-spreading patterns can serve supplemental roles in the identification of the subtype of renal cell carcinoma.
Clinical Indication for CT: Intermittent hematuria of 5 months duration. Patient has history of smoking and cardiac stent before 3years.
a. Indication: CT scan showed suspicious left renal parapelvic complex mass, for evaluation.
b. Histopathology:> Post left nephrou reterectomy Noninvasive high-grade papillary urothelial carcinoma of the renal pelvis and upper ureter (pTa) with free surgical resection margins.
Figure 1 Ill-defined mass is showing contrast enhancement. Left renal vessels are splayed around the mass lesion, however no renal vein thrombosis or abrupt cut-off seen. Left renal vein is retro-aortic. Few tiny lymph nodes are noted at renal hilum area. No perinephric extension seen. Right kidney is within normal limit.
Figure 1: Non-invasive high-grade papillary urothelial carcinoma of the renal pelvis and upper ureter (pTa) with free surgical resection margins.
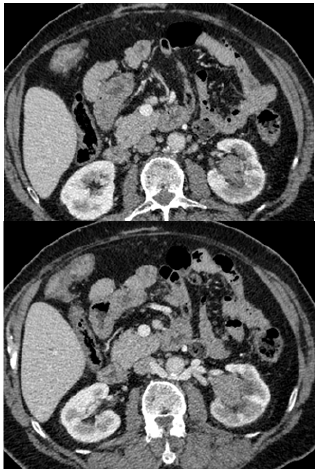
Figure 2 Mass is appears low density. Upper and lower pole calices are also prominent, more of upper calyx. Right kidney is normal in size with no hydro nephrosis. Heterogeneously intermediate low signal intensity mass lesion in T2 (c=coronal and d=axial) seen in left renal pelvicalyceal system extending till the pelvi-uretric junction; measures approximately 3.73 x 2.4 x 2.73 cm. Mass lesion is extending along the mucosal lining of dilated upper and lower pole calyceal system (Figure 3).
Figure 2: Axial post-contrast images.
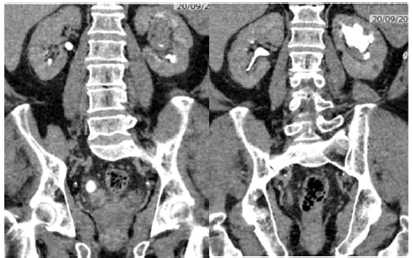
Figure 3: Coronal delayed post-contrast.
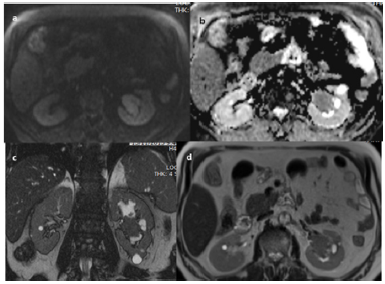
Figure 4 Mass is showing predominantly is intense signal to renal parenchyma in T1 (a) minimal to moderate contrast enhancement. Middle and lower pole calices are also prominent (trapped). Left renal vessels are splayed around the mass lesion, however no renal vein thrombosis or abrupt cut-off seen. Left renal vein is retro-aortic. Few tiny lymph nodes are noted at renal hilum area. No perinephric extension seen. Few simple cortical cysts noted in both kidneys. Right kidney is normal in size, as intensity and enhancement pattern.
Figure 4: Axial pre-contrast (a) and post-contrast images (b, c, and d).
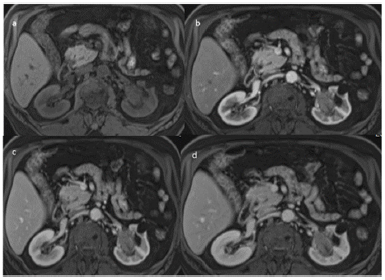
Figure 5: Coronal (a,b and c) and axial post-contrast (d).
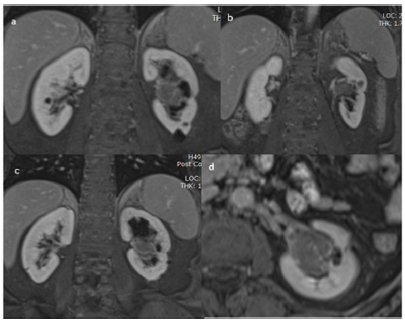
Figure 5 Mass is showing predominantly is intense signal to renal parenchyma in T1 (a) minimal to moderate contrast enhancement. Middle and lower pole calices are also prominent (trapped). Left renal vessels are splayed around the mass lesion, however no renal vein thrombosis or abrupt cut-off seen. Left renal vein is retro-aortic. Few tiny lymph nodes are noted at renal hilum area. No perinephric extension seen. Few simple cortical cysts noted in both kidneys. Right kidney is normal in size, as intensity and enhancement pattern.


