Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
Juan Manuel Suárez Grau*1, Estrella Rodríguez Agea2, Luis Alfonso Carrasco Nestal3 and Carmen Forero Diaz4
Received: July 26, 2017; Published: August 14, 2017
Corresponding author: Juan Manuel Suárez Grau, Department of General and Digestive Surgeon, Hospital of Riotinto, Huelva, Clinic Quirón “Sagrado Corazón” Seville, Spain
DOI: 10.26717/BJSTR.2017.01.000268
Background: The presence of an intrauterine device migrated into the abdominal cavity can be detected incidentally or due to complications (the most frequent abdominal pain, obstructive 8complications or cause of acute abdomen). We report the case of a woman of 35 years, with an intrauterin device (Mirena®) misslocated in the abdominal cavity incidentally 18 months after puerperium (6 months after implantation). After the detection by abdominal conventional X-ray and transvaginal sonography, the management was a laparoscopic surgery in order to remove the device. It was firmly adhered to the major omentum in the right low quadrant. The surgery was performed with no problems and the discharged of the patient was at 12 hours uneventful. The follow up at first month was correct in vaginal and abdominal exploration.
Conclusion: When detecting the migration of the device incidentally both conservative management and surgical treatment are contemplated in the literature. [1] We opted for a laparoscopic surgical treatment due to the potential consequences of perforation viscera, instususcepción, obstruction or infection from abandoned in the abdominal cavity devices [2].
Keywords: Intrauterin Device; Misslocated; Laparoscopy; Omentum.
Intrauterine devices (IUDs) are not exempt from complications and can migrate to another region. This adverse event is primarily associated with iatrogenic perforation during insertion, uterine abnormalities or normal peristaltic activity of the uterus. [1] Uterine perforation is common among women with ‘lost’ IUDs and can cause severe morbidity and mortality and should be carefully managed. Perforations can occur during insertions or later, occurring at or following 1/350 to 1/2500 insertions [2,3].
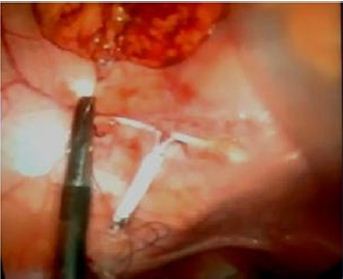
A 35-year-old woman, 18 months after second birth (6 months after implantations of IUD), was revised in the clinic detecting a miss located IUD. The patient presented an history of abdominal pain a week before treated in the Emergency Service; a normal vaginal ultrasound with the IUD in the uterus was detected, and no alterations in the abdominal explorations. In the revision (a week after the isolated abdominal pain episode) the IUD was not in the uterus, and an abdominal conventional X-ray detected the IUD in the low right quadrant into the abdominal cavity. The patient does not have any painful alteration in the review and vaginal and abdominal examination revealed no discomfort. Laparoscopic surgery scheduled for IUD removal was raised. Laparoscopic surgery was performed with three 5 mm trocars (navel = optical, left lower quadrant and hypogastric). The IUD was firmly adhered to the omentum in the right lower quadrant (over the cecum). (Figure 1) Was necessary dissection and resection of the affected? Part omentum to liberate the IUD. (Figure 2) Without consequence It was extracted through one of the trocars. There were no changes that suggested affectation of the uterus (rupture) or ovarian. The recovery was excellent, with discharge at 12 hours and without consequences in reviewing a month after the surgery.
52Uterine perforation is the most common cause of ‘lost’ IUDs [2,3]. Perforations can occur during 53insertions or later [1,3]. Misplacement of the IUD usually occurs at time of insertion and is recognized during the first year in 90% of women [1,2]. In our patients we cannot conclude the cause, but we thought it was probably due to a uterine rupture. If IUD strings are not visible during gynecologic examination, ultrasound should be tried to locate the IUD and pelvic X-ray used only when USG fails to locate the IUD. In our case transvaginal sonography was combined with abdominal X-ray to reach a definitive diagnosis. [3,4] There are two different recommendations about lost IUD treatment: This is the most accepted treatment for displaced IUDs because of the putative risk of adhesion formation or of damage to the intestine or urinary bladder [1,4] Conservative management. In asymptomatic patients, under exceptional circumstances (anesthesia risks, refused of the surgery, coagulations disorders) with a correct follow-up in order to avoid a possible complication by the misslocated IUD [3,5].
The World Heath Organizations recommend that any displaced IUD within the abdomen should be removed following IUDassociated uterine perforation. In contrast, Markovitch et al. suggest that removal of the perforated IUD may not be necessary due to the adhesion formation following uterine perforation by the IUD tends to occur in localized area [5]. However, the high success rate of laparoscopic removal in asymptomatic/symptomatic patients, make this technique such as the most viable option [1,2]. Currently conservative management is not without significant risks (19 cases of bowel perforation associated with IUDs have been documented in world literature) [1,3,6]. The laparoscopy offers a secure and easy surgical procedure to locate and remove the IUD. Recovery is often excellent and can perform the procedure in ambulatory surgery extremely safe [1,3]. For this reasons in cases of intra-abdominal IUD, laparoscopic removal of the IUD must be the first choice of therapy. Laparoscopy, even during pregnancy, has proven to be a safe and simple tool for managing a variety of surgical conditions (such as the IUd in volving in colon and ileum, ovarian migration, etc.) [2,3,6,7].
Figure 1: IUD involved in the omentum.
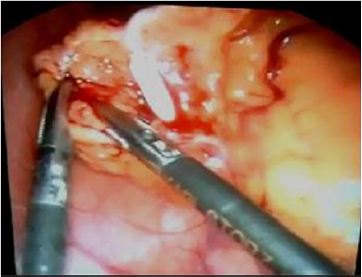
Figure 2: IUD before extraction thought the trocar.