Abstract
Aim: The aim of the present clinical trial was to test the hypothesis that different dental implant connections have the same result of maintaining crestal bone. The implants analyzed have internal conical connections and platform switching and this has a positive impact on crestal bone-level changes after 3 years. Two different dental implants with different connections are compared.
Material and Methods: Forty implants with two implant connection designs were placed in 38 patients: one with a hexagonal bacteria free conical connection (Cea Medical ONE) and one with a bacteria free tapered connection as well as with a hexagonal index (Cea Medical H2O). Twenty-one patients received implant ONE and 19 received implant H2O. All the implants which were inserted follow producer indications, in particular ONE at crestal level and H2O 1 mm below the crestal tissue. Patients were followed up at 1-year intervals in order to monitor the crestal bone reabsorption.
Results: All implants were completely osseo-integrated. Bone levels between the two groups are different, despite the fact that both implants have bacteria free connections. At year 3, the mean radiographic peri-implant bone loss was -0,41 ± 0.22 mm (ONE Implant) and +0.37 ± 0.19 mm (H2O implant).
Conclusion: The dimension of the conical bacteria free connection influences the marginal crest, superior results have been achieved with a larger melted surface.
Keywords: Bone Reabsorption; Follow- Up Studies; Implant Connection; Implant Platform; Platform Switching
Introduction
At the beginning of the 21st century the theory of platform switching had been introduced to implant dentistry based on clinical observations to minimize the crestal bone reabsorption [1,2]. Several randomized controlled clinical trials highlight that the amount of marginal bone reabsorption was inversely proportional to the range of the implant–abutment mismatch [3]. Recent studies analyze the existence of a micro-gap between the implant and the abutment. This micro-gap represents a contamination area for bacteria. On the contrary, in the bacteria-free implants there was a contact of greater length and width with the connective tissue, therefore a shorter epithelial downgrowth. The presence of a micro-gap in the bacteria free system may justify the histologic mild inflammation in the connective tissue [4]. The presence of bacteria is a consequence of the melting of the two connecting surfaces. If the space is inferior to the dimension of the bacteria, the connection will be a bacteria free connection. In these Metallographic section images, it is possible to observe the two different implants with bacteria free connections. The marginal connection of both surfaces is melted together with the implant body. The melted surface with a hexagonal connection is smaller than the conical connection (Figure 1).
Figure 1: Metallographic section images of two different implants. In the upper image an implant with a hexagonal connection, in the lower one an implant with a conical connection.
Visio-fit® abutments (cea medical SA, Geneva Swiss) thanks to a cold-welded connection with the implant, practically remove micromovement, tipping and the effects of vibration. When the abutment is seated into the implant with the right torque, the abutment hex frictionally engages the walls of the implant’s internal hex. Gaps between the implant and abutment leave space for bacterial colonization. Chewing loads can generate a small displacement between components, which create a pumping effect. The resulting distribution of endotoxins in the tissue at the implant-abutment interface causes an inflammatory reaction. Until the correct biological width is established, the bone continues to be reabsorbed below the implant-abutment connection [5]. Furthermore, only a bacteria-free connection prevents bone reabsorption, stabilizing the soft tissues. The platform-switching concept is designed to increase the soft tissue volume, which contributes to long-term esthetic outcomes [6,7]. Additionally, with the platform-switching the transition area between implant and abutment is in a more central position, creating a medialized implant/abutment junction that dissipate the loads internally. In this way the peri-implant tissues are free from mechanical and microbial impacts [8,9]. Therefore, the platform switching associated with a stable and bacteria-free connection allows to achieve the stability of the peri-implant tissues [10.11].
Material and Methods
The clinical study was based on a total of 38 patients (19 females and 19 males, range 30-75). Inclusion criteria were residual bone volume sufficient to receive implants; sufficient keratinized tissue; absence of systematic diseases and therefore all the conditions for which it is not possible to perform surgery and good oral hygiene. Exclusion criteria were: previous radiotherapy in the head and neck area; bruxism and/or clenching; smoking habits; immunocompromising diseases; partial/full dental prosthesis in occlusion with implants; local inflammation and oral mucosal diseases; need for bone grafting / guided tissue regeneration (GTR) prior to implant placement. The patients received 21 implants with a tapered hexagonal connection (Cea Medical ONE) and 19 received implants with a tapered conical connection (Cea Medical H2O). All surgeries were performed by an oral surgeon and a prosthetist, the interventions carried out under local anesthesia, were executed following the manufacturer’s guidelines. In the mandible the single crowns were placed after 10 weeks, while in the maxilla after 20 weeks. The post-surgical therapy prescribed was as follows: 400 mg ibuprofen 4-times a day for 2 days, 500 mg amoxicillin 3-times a day for 7 days and oral rinsing with 0.12% chlorhexidine gluconate (1 min) 2-times a day for 7 days. To evaluate the marginal bone levels, standardized intraoral paralleled x-rays (Kodak E DF; Eastman, Kodak Co, Rochester, NY) were taken at the time of the placement of the final restoration and in the subsequent annual follow-up appointments. Standardized scans were realized by individualizing x-ray templates with poly vinyl siloxane (Express; 3M ESPE, Seefeld, Germany).For both mesial and distal surfaces of each implant site, the mean of the coronal and apical measurements were calculated using a digital ruler.
Results
At the end of the study, none of the implants were lost. After the healing period, in fact, all the implant screws were firmly in place in the jaws. The radiographic control also showed no sign of a continuous peri-implant radiolucency. The 38 implants placed have Osseo-integrated to perfection, having a direct contact with the bone. At 36 months the mean x-ray peri-implant bone loss was -0,41 ± 0.22 mm (ONE Implant) and +0.37 ± 0.19 mm (H2O implants). A substantial difference was noted between the two different implant line connections.
Discussion
Most of the bone resorption takes place during the first year of prosthesis placement, then decreases with occlusal load. The favorable results of mismatched abutments/ implant platforms are also evident in several studies conducted on animals, thanks to radiographic analysis [12]. Platform switching was essential to reduce crestal bone reabsorption compared with matched diameter restorations, regardless of the position of the implant on the crestal bone. Subsequently, histological samples taken from the same experiment were studied and confirmed the reduced bone loss [13]. In this study the implants that were inserted differ in in the macro- and micro-design components of their fixtures, but the absence of a micro-gap could explain the health of the connective tissue and the reduced peri-implant reabsorption. Probably the different volume of bone loss around the ONE and H2O implants is due to the different connection designs. Despite the results obtained, it is necessary to carry out more systematic long-term studies, investigating the factors that contribute to bone resorption around the implants, after having standardized several variables such as: bone quality, bone quantity, micro / macro design, type of restoration, etc.
Conclusion
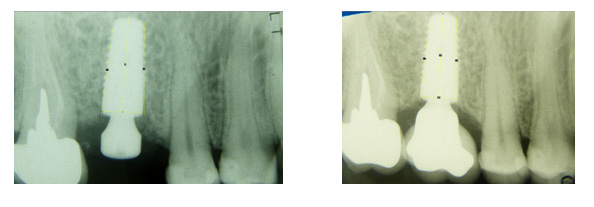
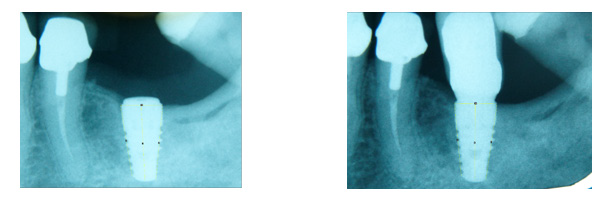
The outcomes of this investigation indicated that the major dimension surface of bacteria free conical connections defines a better crestal preservation. The dimension of melted surface affects the bacteria permeability. The hexagonal connection slightly conical seem not enough to preserve the crestal bone.The ONE implants displayed a small amount of bone reabsorption but on the other side the H2O implants have a small amount of bone increasing (Figures 2 & 3).
Declarations
Ethics approval and consent to participate: Certified systems available on the market were used. Patients received informed consent. The evaluation was of a clinical radiographic type and therefore not gruesome for the patient. Consequently, it was deemed unnecessary to request an etic committee as it was a noninvasive intervention.
Consent for Publication
Consent to publication was obtained from all participants included in the study.
Availability of Data and Materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
Competing Interests
The authors declare no competing financial interests.
Funding
No funding.
Authors’ Contributions
Each author have made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data; has approved the submitted version (and version substantially edited by journal staff that involves the author’s contribution to the study); agrees to be personally accountable for the author’s own contributions and for ensuring that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and documented in the literature. All authors have read and agreed to the published version of the manuscript.
Acknowledgement
Not applicable.
References
- Lazzara RJ, Porter SS (2006) Platform switching: a new concept in implant dentistry for controlling postrestorative crestal bone levels. Int J Periodontics Restorative Dent 26(1): 9-17.
- Gupta S, Sabharwal R, Nazeer J, Taneja L, Choudhury BK, et al. (2019) Platform switching technique and crestal bone loss around the dental implants: A systematic review. Ann Afr Med 18(1): 1-6.
- Canullo L, Fedele GR, Iannello G, Jepsen S (2010) Platform switching and marginal bone-level alterations: the results of a randomized-controlled trial. Clin Oral Implants Res 21(1): 115-121.
- Tenenbaum H, Schaaf JF, Cuisinier FJ (2003) Histological analysis of the Ankylos peri-implant soft tissues in a dog model. Implant Dent 12(3): 259-265.
- Zheng Z, Ao X, Xie P, Jiang F, Chen W (2021) The biological width around implant. J Prosthodont Res 65(1): 11-18.
- Atieh MA, Ibrahim HM, Atieh AH (2010) Platform switching for marginal bone preservation around dental implants: a systematic review and meta-analysis. J Periodontol 81(10): 1350-1366.
- Abou-Ayash S, Schimmel M, Kraus D, Mericske-Stern R, Albrecht D, et al. (2020) Platform switching in two-implant bar-retained mandibular overdentures: 1-year results from a split-mouth randomized controlled clinical trial. Clin Oral Implants Res 31(10): 968-979.
- Aslam A, Hassan SH, Aslam HM, Khan DA (2019) Effect of platform switching on peri-implant bone: A 3D finite element analysis. J Prosthet Dent 121(6): 935-940.
- Soliman G, Guazzato M, Klineberg I, Chang MC, Ellakwa A (2021) Influence of Platform Switching, Abutment Design and Connection Protocols on the Stability of Peri-Implant Tissues. A Systematic Review. Eur J Prosthodont Restor Dent 29(4): 194-207.
- Romanos GE, Javed F (2014) Platform switching minimises crestal bone loss around dental implants: truth or myth?. J Oral Rehabil 41(9): 700-708.
- King GN, Hermann JS, Schoolfield JD, Buser D, Cochran DL (2002) Influence of the size of the microgap on crestal bone levels in non-submerged dental implants: a radiographic study in the canine mandible. J Periodontol 73(10): 1111-1117.
- Ronald E Jung, Archie A Jones, Frank L Higginbottom, Thomas G Wilson, John Schoolfield, et al. (2008) The influence of non-matching implant and abutment diameters on radiographic crestal bone levels in dogs. J Periodontol 79(2): 260-270.
- David L Cochran, Dieter D Bosshardt, Leticia Grize, Frank L Higginbottom, Archie A Jones, et al. (2009) Bone response to loaded implants with non-matching implant-abutment diameters in the canine mandible. J Periodontol 80(4): 609-617.

 Research Article
Research Article