Abstract
The result of polymer advances is Polyetheretherketone (PEEK), which is one of the well-known thermoplastic polymers. The PEEK biomaterials deliver high performance with remarkable mechanical strength, chemical resistance and high thermal stability. The usage of PEEK progressed from the aviation industry to biomedical sciences due to its exceptional physical and biological properties. This review aims to present a comprehensive overview of applications of PEEK in various aspects of dentistry highlighting clinical prospects in restorative materials, as veneers, fixed and removable prosthesis, endocrown, framework for implant supported prostheses, and as dental biomaterial for implants. Owing to their bio-inertness, these materials have to be modified by a several methods to improve their bioactivity amplifying its application in clinical dentistry. These are constantly evolving materials with limited publications in literature. Therefore, long term evaluations are required to assess the performance of PEEK and PEEK blends in order to generate a robust opinion regarding intraoral use of these materials.
Abbreviations: PEEK: Polyetheretherketone; MFI: Melt Flow Index; MN: Molecular Weight; STEAM: Sterilization Methods Including Autoclave; PIII: Plasma Ion Immersion Implantation; CFR: Carbon Reinforced; SEP: Super-Engineering-Plastics; CAD: Design Software CAM: Design Milling; PES: Polyethylene Sulfone; PVDF: Polyvinyl Difluoride; AKP: Aryl-Ketone Polymer
Introduction
Polymeric advances in biomedicine have led to the development of thermoplastic materials including PEEK (Polyetheretherketone), which was developed originally by the USA aerospace industry (1970s) [1]. It gained popularity due to its stable structure at high temperatures and potential for high load-bearing similar to titanium [2]. Commercialized in 1980s and initially used in orthopedics, PEEK was proposed for biomedical application in 1988 by Invibio Ltd. (Thornton-Cleveleys, UK) [2]. PEEK-OPTIMA was launched by Victrex PEEK business (Imperial Chemical Industry, London UK) for long-term implantable applications [1,3]. PEEK is a synthetic, tooth-colored, semi-crystalline, thermoplastic polymer [1]. The monomer ether-ether-ketone undergoes polymerization via step-growth dialkylation reaction of bis-phenolates, forming polyetheretherketone [4]. Commonly reaction between 4,4’-difluorobenzophenone and disodium salt of hydroquinone in a polar solvent (diphenyl-sulphone at 300 oC) is conducted to form PEEK [5]. These materials are composed of 80% straight and 20% kinked structure with durable physical properties.
Advantages of Peek
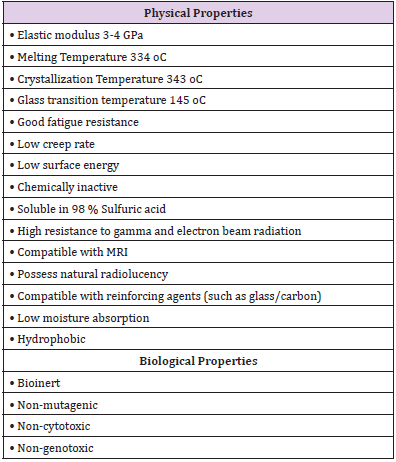
PEEK serves a remarkable alternative material in medicine and surgery owing to physical and biological properties (Table 1) with the following advantages:
a. Modulus of Elasticity: PEEK offers a modulus of elasticity similar to the human cortical bone. This allows it to bear load, unlike conventional stainless steel or titanium [6].
b. Strength and Stiffness: PEEK has an elastic modulus of 3.6 GPa, but can be further modified to 18 GPa, which is closer to that of bone, by addition of carbon fibers [6].
c. Radiolucency: This material is resistant to radiation, and is radiolucent. This makes complications easier to spot. Barium is suggested to enhance the radiopacity for PEEK, without altering its properties.
d. Biocompatibility/ Bio-inertness: Upon undergoing extensive animal testing, PEEK displayed no cytotoxicity, genotoxicity or immunogenetic (allergic) concerns [7].
e. Sterilization: PEEK has shown compatibility and retained integrity with conventional sterilization methods including autoclave (steam), ETOX and radiation without degradation. (even after repeated cycles) [8].
f. Customizable Design: PEEK and PEEK blends can be easily customized compared to conventional metal which is not yet open for design modification to a greater extent [9].
g. Mass Production: Components using high-performance polymers can be machined from stock shapes, or if high volumes are needed, they can be injection molded as well. Injection molding is particularly useful for single use instruments, as it provides a cost-effective option [10].
h. Lightweight: High performing plastics offer better ergonometric and control for the surgeon to avoid repetitive stress injuries and prevent fatigue during lengthy procedures[10].
i. Dimensional Stability: It is insoluble in solvents in mouth and at room temperature, stable over 300oC [11].
j. Flexibility: The versatility of PEEK allows its form to be modified into tubings, spacers, seals, or compression screws [12].
k. Plaque Affinity: Low plaque affinity [13].
l. Esthetic: Allows superior polishibility [13].
Types of Peek
According to the Melt Flow Index (MFi) and molecular weight (Mn), PEEK-optima materials are divided into three grades:
a. LT1-standard grade (MFi-3.4; Mn = 115.000)
b. LT2-optimized grade for melt strength and viscosity (MFi- 4.5; Mn = 108.000) and
c. LT3- high-flow grade for injection molding thin-walled parts [1]
PEEK composites applied in biomedical fields are based on the PEK LT1 materials which are considered biologically inert [1,14].
Modifications of Peek: PEEK materials are biologically inert and can be modified by the addition of functional monomers prepolymerization or post-polymerization [15] Surfaces modifications of PEEK materials can broadly be classified as (Table 2) [16]
a. Physical treatment
b. Chemical treatment
c. Surface coating
d. Composite preparation [16]
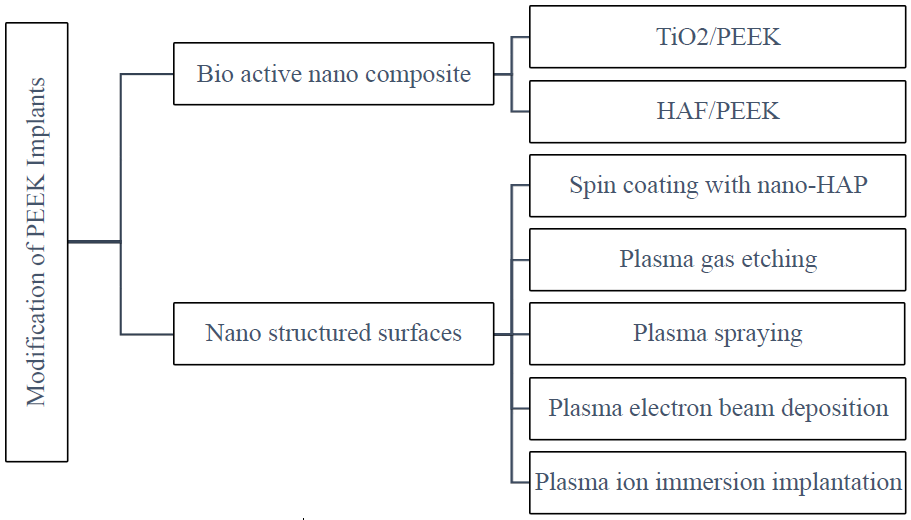
Incorporation of bioactive composites in PEEK substrate and introduction of reinforcement agents to produce nanosized composites are commonly used in surface modification of PEEK implants [16,17]. In addition, by blending with fine filler particles to synthesize PEEK composites, bioactive implants with good osseointegration can be produced [18]. Nano-modification includes spin-coating, gas plasma etching, electron beam deposition, plasma ion immersion implantation (PIII) [19-22] (Figure 1).
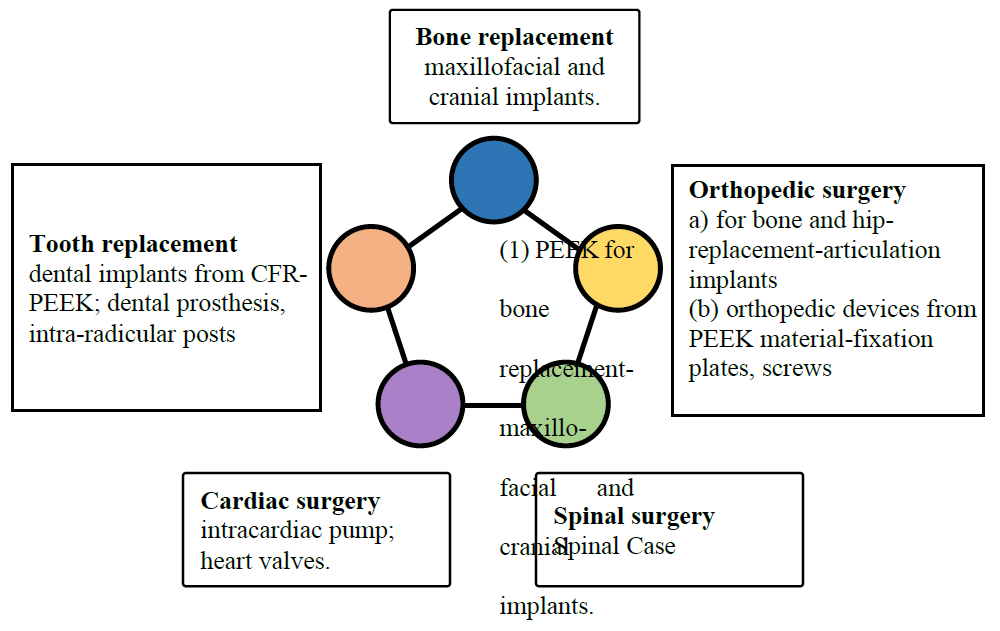
Applications of Peek in Surgery : On the basis of Clinical Classification of PEEK (Figures 2 & 3) following applications of PEEK have been elaborated
a. PEEK for bone replacement
b. PEEK for spine surgery
c. PEEK for orthopedic surgery
d. PEEK for tooth replacement
e. PEEK for cardiac surgery
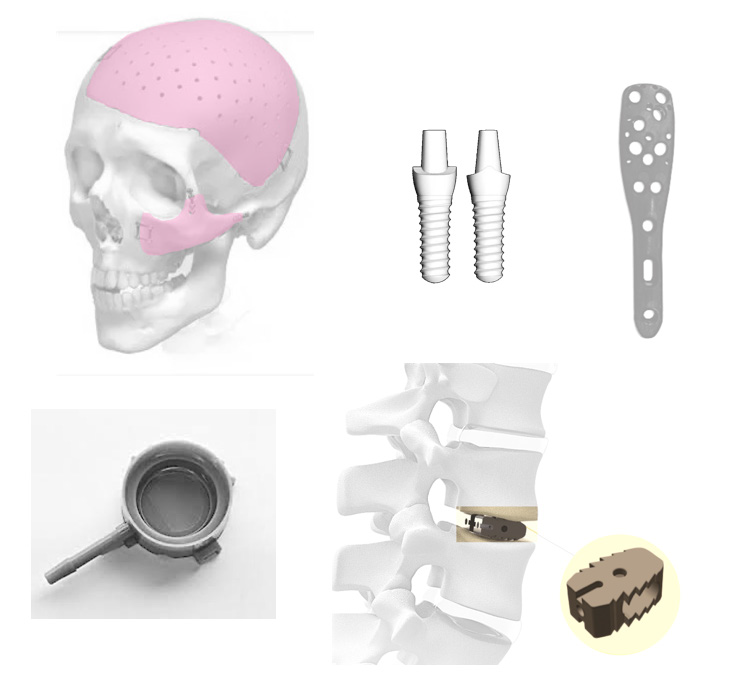
Figure 3: Biomedical applications of PEEK
a. Osteosynthesis plates
b. Dental implant
c. Bone fixation plate
d. Cardiac valve
e. Interbody fusion cages.
PEEK has been adapted for surgical field for fracture fixation, including the use of Carbon Reinforced (CFR) PEEK material (Figure 3c) [23]. CFR-PEEK, provides elite load-to-failure strength and degrades over years, hence, providing ample time for healing to promote osteoconductivity to avoid complications [24]. It increases patient comfort by being lightweight, which allows joint manipulation with less effort [25]. Shuai et al. incorporated Hydroxyapatite into polyetheretherketone/ polyglycolic acid (PEEK/GPA) hybrid to improve upon its properties and concluded that PEEK/PGA scaffolds with HAP were more attractive for bone and tissue regeneration [26]. Owing to its remarkable variations, PEEK has found its place in replacement for bone and cartilage, cardiac, spinal and maxillofacial operations [27,28]. Craniofacial applications include customizable osteosynthesis plates, repair of cranial vault defects (Figure3a), replacement of nasal, maxilla and mandible bones with an allowance of easier revisions [27,28] (Table 1). PEEK and PEEK blends match metal in most, and exceed effectiveness in other areas highlighting their use as an equivalent or superior alternative to metal instruments including drug delivery, dental abutments, catheters, blood management and surgical instruments [27,29].
Peek in Dentistry
PEEK has widespread use as dental implants, orthodontic appliances, dental prostheses and utilization in threedimensional printing [27,28,30]. Its well-established use is due to its mechanical, physical, and biological properties combined with ease of customizable fabrication. Following are the proven uses of PEEK in dentistry with positive patient outcomes
Peek in Implants: Biologically inert PEEK materials are modifiable for their application as implants [18]. The CFR-PEEK implants present a higher load concentration in the cervical area and at the cortical bone than the titanium implants [31]. Finite element analysis suggests less stress shielding effect of CFR-PEEK as compared to titanium implants, which reduces the amount of bone resorption occurring around the implant [32]. PEEK has limited osteoconductive properties and absence of inflammation around the implant, however, few studies suggest increased protein turnover in cells in contact with PEEK and CFR-PEEK [33]. Similarity of elastic moduli between bone and PEEK surface, reduces the stress shielding effects and encourage bone remodeling [2]. A study by Sarot et al. reports similar stress distribution between titanium and PEEK implants [31]. Koch et al. reports comparable osseointegration of titanium, zirconia and PEEK implants, also no evidence of difference in bio-inertness among these three materials exist [34].
PEEK dental implants have not been used widespread clinically, so there is lack of evidence supporting their longterm use and bone remodelling. Osteogenic coatings (such as spin-coating) of PEEK implants, improve the mechanical and biological properties [19]. Animal studies resulted in higher bone to implant contact in case of coated PEEK implant [35]. Plasma gas-etching has also shown improved proliferation of human mesenchymal cells on modified PEEK in in-vitro studies [20]. CFR-PEEK prosthesis, plasma sprayed with titanium dioxide and hydroxyapatite, reportedly showed superior biocompatibility. Similarly, electron beam coating, improves hydrophilicity of the implant, as does titanium (+/- BMP-2) coating [21]. Plasma immersion ion implantation (PIII) with titanium has been shown to have antimicrobial effect against Staphylococcus aureus and Escherichia coli, but no reports regarding periodontal pathogens exist [36]. Nano-sized particles of hydroxyapatite are anti-microbial against Streptococcus mutans, and increased bioactivity was evident in animal studies [37]. Bioactive inorganic particles incorporated via melt-blending and compression blending have been employed to produce bioactive PEEK [18]. PEEK has been presented as a viable alternative to titanium in constructing implant abutments.
A trial by Koutouzis et al. suggested that there is no significant difference in the bone resorption and soft tissue inflammation around PEEK and titanium abutments [38]. Oral microbial flora attachment to PEEK abutments is comparable to those made of titanium, zirconia and polymethylmethacrylate [39]. There are several physicochemical methods to modify PEEK abutment surfaces; plasma, ultraviolet/ozone, airborne particle abrasion (grit blasting), acidic etching, and radiationinduced (plasma gas, laser, electron and ion-beam) treatment [40]. The conditioning of PEEK surface with Piranha solution (solution of sulfuric acid (H2SO4) and hydrogen peroxide (H2O2)) results in increased functional groups on the surface for bonding [41]. Rea et al., evaluated soft and hard tissue healing using different forms of PEEK healing screws [42]. The authors concluded that PEEK may be used as a healing screw material, since no statistical difference was observed between PEEK forms and titanium [42].
Peek Fixed Crown and Bridges: With the rise in nonmetallic restorative materials, use of PEEK for fabrication of FDP is gaining importance. Superior mechanical properties and compressive strength that is comparable to bone, enamel and dentin. Incorporation of inorganic components further improve compressive and tensile strength of material fabricated using vacuum pressing and milling. PEEK has low solubility and water sorption with absence of monomer which makes it suitable for intraoral use [43]. PEEK is white-grey and requires veneering for application in aesthetic areas [44]. Veneering using digital method improves the fracture load than conventional veneering [44]. Studies suggest that sulphuric acid, sand blasting, and microwave supported coating improves surface energy for veneering [45,46]. The material has also been used for framework fabrication on short or long span all-on 4 implant restorations, providing a cushioning effect as a distinct advantage over harder materials, resulting in less screw loosening [47].
The use of modified PEEK for single crown frameworks veneered with light polymerized composite resin has been suggested in case of metal allergies and weak abutments for patients with parafunctional habits [48,49]. These materials have been used to veneer PEEK endo-crown frameworks with predictable results [48]. Wagner et al. studied the retention between PEEK telescopic crowns and cobalt chrome copings of different taper and manufacturing methods [50]. Milled crowns with 0° taper showed the lowest retention, while tapers did not significantly affect the retention of PEEK crowns manufactured by injection molding [50]. The use of modified PEEK has also been proposed for fabricating Maryland bridges for in cases of abutment teeth with different mobility patterns [51]. The dampening of occlusal forces by the PEEK framework may contribute to decreased debonding rates and increased survival rates [51].
Peek in Restorations: In addition to wide application of temporary crowns, PEEK materials can easily be modified with dental burs and adhesives [52]. A study by Schmidlin et al. reports that etching with sulfuric acid resulted in a complex fiber network, while sandblasting with a particle size of 50 μm led to an irregular surface which was similar to surface with silica coating [53]. Although air-abrasion with or without silicon dioxide coating leaves the surface of PEEK more prone to moisture, etching with phosphoric acid creates a rough and chemically modified surface that allows a stronger bond of the material with the hydrophobic composites (shear bond strength: 19.0±3.4 MPa) [34,53]. Etching with phosphoric acid for 60 to 90 secs may result to shear bond strength with composite resin cements up to 15.3±7.2MPa after storage in water 37oC for 27 days [34]. A bond of 23.4±9.9MPa with the composites has been achieved in aged PEEK samples by combining etching with piranha acid and the use of adhesive agent [34]. A systematic review by Gama et al. concluded that bond strength of PEEK and veneering resin was significantly increased when surface pre-treatments were administered with adhesive systemsp [54].
Peek in Removable Prosthesis: Conventional use of Chrome denture frameworks has been a cost effective and predictable option for rehabilitation of missing dentition with great success [55]. These dentures are not esthetic considering the display of metal clasp at smile, bulkier weight of the prosthesis, metallic taste and allergy to the metal component, which led to the use of polymers for denture bases [56,57]. The use of PEEK in other disciplines since its inception has been successfully reported in literature [58]. A modification of PEEK with 20% ceramic fillers as high performance Bio-HPP presents these stable thermoplastics with mechanical, chemical and biological properties combined with high temperature resistance, as an option to be used intraoral [58]. Additional Advantages offered by PEEK materials include elimination of allergic reactions and metallic taste, high polishablitiy, good wear resistance combined with low plaque affinity enabling the patient to maintain their periodontal health as reported by Maryod et al. [59,60].
Furthermore, the esthetics are aided by the color of Bio-HPP making it an ideal intraoral material of choice for the removable prosthesis [60]. According to Mayinger et al., PEEK milled performed better then PEEK pressed materials while both materials exhibited sufficient retention for clinical usage compared with Co-Cr [61]. Costa-Palau et al. mentioned in their clinical report regarding the fabrication of maxillary obturator using PEEK as an alternative to conventional materials and methods [62]. They claimed that the PEEK obturator is weightless, biocompatible, with good retention and ease of polishing [62]. Hahnel et al. used PEEK framework with double retained crown for management of a patient with extensive loss of vertical dimension [63].
Peek in Orthodontic Appliance: Technological advances in materials, enabled the use of Super-Engineering-Plastics (SEPs) including PEEK for interceptive orthodontics by fabrication of space maintainers [64]. Acquisition of 3D images, using design software (CAD) and milling (CAM) for manufacturing PEEK devices allowed to show the space maintenance to favor the eruption of permanent teeth with little compliance [64]. In contrast to other available polymers, such as polyethylene sulfone (PES) and polyvinyl difluoride (PVDF), metalfree PEEK orthodontic wires offer higher orthodontic resistance compared to titanium-molybdenum (Ti- Mo) and nickel-titanium (Ni-Ti) [65]. Furthermore, PEEK can be used in combination with conventional wires as presented in a study by Shirakawa et al. which concludes that the new PEEK tube demonstrated a good combination of esthetic and functional properties for use in orthodontic appliances [66]. Retention is of utmost importance to prevent post-orthodontic relapse. Kadhum et al. reported the use of 0.8 mm round PEEK wire with comparable results and therefore suggested it as an alternate treatment option using 3D CAD CAM fabrication [67]. However, there is lack of studies to support their long-term claim [67]. PEEK does not have a shape memory but recent advances point PEEK modifications in that direction for future development [68].
Future Prospects
Alternative thermoplastic materials which have applications in medicine and dentistry include, PEKK, Bio HPP and Aryl-ketone polymer to name a few
Poly Ether Ketone Ketone (PEKK)
First introduced by Bonner, PEKK has applications in various industries [69] it is a derivative of PAEK, a family of ultra-high performance thermoplastic polymers, with a polyaromatic semicrystalline structure (–C6H4–O–C6H4–O– C6H4–CO–) n [1]. PEKK is a linear thermoplastic polymer with benzene ring, that has an additional ketone group, which enhances its compressive, flexural, tensile strength, polarity and rigidity [70] PEKK with 60% straight and 40% kinked segments melts at 305°C with amorphous and crystalline structure [71] Its shock absorbing ability, modulus of elasticity and fatigue limit, greater than zirconia and nickelchromium, raises the possibility of its use as restorative material [72]. The addition of titanium dioxide (TiO2) increases its hardness [73]. Their wide biomedical applications are promising due to the presence of second ketone group which allows for more surface modifications.
Bio HPP (Bio High-Performance Polymer)
Bio HPP (Bio high-performance polymer) is another material based on PEEK for applications in interim abutments, implantsupported bars, dental implants and fixed partial dentures [74]. It has superior physical properties, dental esthetics, low specific weight, low plaque affinity and biocompatibility [74]. The longevity of applications of this material is lacking research. Therefore, clinical evidence is required to imply widespread use in dentistry.
Aryl-Ketone Polymer (AKP)
Aryl-ketone polymer (Ultaire AKP), introduced by Solvay Dental 360 is indicated for removable dental prosthesis [75]. This material is provided as a milling blank to be processed by computer-aided design and computer-aided manufacturing (CAD-CAM) technology [76].
Conclusion
Applications of PEEK in dentistry include their use as dental implants, framework of implant supported prosthesis, endocrowns, fixed/removable partial dentures, orthodontic wires, and restorative materials. Furthermore, modifications can result in improved material properties resulting in wider applications in clinical dentistry. However, the use of PEEK in dentistry is a newer modality with a scarcity of clinical data, therefore longterm evaluations are needed to assess the performance of PEEK prostheses and generate a robust opinion regarding these materials for clinical use.
References
- Kurtz SM, Devine JN (2007) PEEK biomaterials in trauma, orthopedic, and spinal implants. Biomaterials 28(32): 4845-4869.
- Rahmitasari F, Ishida Y, Kurahashi K, Matsuda T, Watanabe M, et al. (2017) PEEK with Reinforced Materials and Modifications for Dental Implant Applications. Dent J (Basel) 5(4): 35.
- Green S, Schlegel J (2001) A polyaryletherketone biomaterial for use in medical implant applications. Polym for the Med Ind Proc, Brussels, p. 14-15.
- Tekin S, Cangül S, Adıgüzel Ö, Değer Y (2018) Areas for use of PEEK material in dentistry. International Dental Research 8(2): 84-92.
- T van De Grampe, Gary W (2012) Wheatley; Ernst-Ulrich Dorf; Edgar Ostlinning; Klaus Reinking. Polymers, High-Temperature. Ullmann's Encyclopedia of Industrial Chemistry.
- Schwitalla A, Müller WD (2013) PEEK dental implants: a review of the literature. Journal of Oral Implantology 39(6): 743-749.
- Rivard CH, Rhalmi S, Coillard C (2002) In vivo biocompatibility testing of peek polymer for a spinal implant system: a study in rabbits. Journal of Biomedical Materials Research 62(4): 488-498.
- Kumar A, Yap WT, Foo SL, Lee TK (2018) Effects of sterilization cycles on PEEK for medical device application. Bioengineering 5(1): 18.
- Kaleli N, Sarac D, Külünk S, Öztürk Ö (2018) Effect of different restorative crown and customized abutment materials on stress distribution in single implants and peripheral bone: A three-dimensional finite element analysis study. The Journal of prosthetic dentistry 119(3): 437-445.
- Haleem A, Javaid M (2019) Polyether ether ketone (PEEK) and its manufacturing of customised 3D printed dentistry parts using additive manufacturing. Clinical Epidemiology and Global Health 7(4): 654-660.
- Yang C, Tian X, Li D, Cao Y, Zhao F, et al. (2017) Influence of thermal processing conditions in 3D printing on the crystallinity and mechanical properties of PEEK material. Journal of Materials Processing Technology 248: 1-7.
- Peng TY, Ogawa Y, Akebono H, Iwaguro S, Sugeta A, et al. (2020) Finite-element analysis and optimization of the mechanical properties of polyetheretherketone (PEEK) clasps for removable partial dentures. Journal of prosthodontic research 64(3): 250-256.
- Perween AM, Gupta R (2021) PEEK: A Futuristic Dental Material in Pediatric Dentistry. J Pediatr 7(2): 724.
- Dennes TJ, Schwartz J (2009) A nanoscale adhesion layer to promote cell attachment on PEEK. Journal of the American Chemical Society 131(10): 3456-3457.
- Lee WT, Koak JY, Lim YJ, Kim SK, Kwon HB, et al. (2012) Stress shielding and fatigue limits of poly‐etherether‐ketone dental implants. Journal of Biomedical Materials Research Part B: Applied Biomaterials 100(4): 1044-1052.
- Ma R, Tang T (2014) Current strategies to improve the bioactivity of PEEK. International journal of molecular sciences 15(4): 5426-5445.
- Ortega Martínez J, Farré Lladós M, Cano Batalla J, Cabratosa Termes J (2017) Polyetheretherketone PEEK as a medical and dental material. A literature review. Medical Research Archives 5(4).
- Najeeb S, Khurshid Z, Matinlinna JP, Siddiqui F, Nassani MZ, et al. (2015) Nanomodified peek dental implants: Bioactive composites and surface modification—A review. International journal of dentistry 2015: 381759.
- Johansson P, Jimbo R, Kjellin P, Currie F, Chrcanovic BR, et al. (2015) Biomechanical evaluation and surface characterization of a nano-modified surface on PEEK implants: a study in the rabbit tibia. International journal of nanomedicine 9(1): 3903-3911.
- Wang H, Lu T, Meng F, Zhu H, Liu X (2014) Enhanced osteoblast responses to poly ether ether ketone surface modified by water plasma immersion ion implantation. Colloids and Surfaces B: Biointerfaces 117: 89-97.
- Randolph SJ, Fowlkes JD, Rack PD (2006) Focused, nanoscale electron-beam-induced deposition and etching. Critical reviews in solid state and materials sciences 31(3): 55-89.
- JV Mantese, IG Brown NW, Cheung GA (1996) Collins Plasma-immersion ion implantation,”MRS Bulletin 21(8): 52-56.
- Bradley JS, Hastings GW, Johnson Nurse C (1980) Carbon fibre reinforced epoxy as a high strength, low modulus material for internal fixation plates. Biomaterials 1(1): 38-40.
- Li CS, Vannabouathong C, Sprague S, Bhandari M (2015) The use of carbon-fiber-reinforced (CFR) PEEK material in orthopedic implants: a systematic review. Clinical Medicine Insights: Arthritis and Musculoskeletal Disorders, p. 33-45.
- Neugebauer J, Adler S, Kisttler F, Kistler S, Bayer G (2013) The use of plastics in fixed prosthetic implant restoration. Zwr-German Dent J 122: 242-245.
- Shuai C, Shuai C, Wu P, Yuan F, Pei Feng, et al. (2016) Characterization and bioactivity evaluation of (polyetheretherketone/polyglycolicacid)-hydroyapatite scaffolds for tissue regeneration. Materials 9(11): 934.
- Panayotov IV, Orti V, Cuisinier F, Yachouh J (2016) Polyetheretherketone (PEEK) for medical applications. Journal of Materials Science: Materials in Medicine 27(7): 118.
- Ferguson SJ, Visser JM, Polikeit A (2006) The long-term mechanical integrity of non-reinforced PEEK-OPTIMA polymer for demanding spinal applications: experimental and finite-element analysis. European spine journal 15(2): 149-156.
- Harting R, Barth M, Bührke T, Pfefferle RS, Petersen S (2017) Functionalization of polyethetherketone for application in dentistry and orthopedics. BioNanoMaterials 18(1-2).
- Tada Y, Hayakawa T, Nakamura Y (2017) Load-deflection and friction properties of PEEK wires as alternative orthodontic wires. Materials 10(8): 914.
- Sarot JR, Contar CM, Da Cruz AC, de Souza Magini R (2010) Evaluation of the stress distribution in CFR-PEEK dental implants by the three-dimensional finite element method. Journal of Materials Science: Materials in Medicine 21(7): 2079-2085.
- Ranaud M, Farkasdi S, Pons C, Panayotov I, Collart-Dutilleur PY, et al. (2015) A new rat model for translational research in bone regeneration. Tissue Eng C 22(2):125-131.
- Najeeb S, Bds ZK, Bds SZ, Bds MS (2016) Bioactivity and osseointegration of PEEK are inferior to those of titanium: a systematic review. Journal of Oral Implantology 42(6): 512-516.
- Koch FP, Weng D, Kramer S, Wagner W (2013) Soft tissue healing at one-piece zirconia implants compared to titanium and PEEK implants of identical design: a histomorphometric study in the dog. Int J Periodontics Restor ent 33(5): 669-677.
- Durham III JW, Montelongo SA, Ong JL, Guda T, Allen MJ, et al. (2016) Hydroxyapatite coating on PEEK implants: Biomechanical and histological study in a rabbit model. Materials Science and Engineering: C 68: 723-731.
- H Hu, W Zhang, Y Qiao, X Jiang, X Liu, et al. (2012) Antibacterial activity and increased bone marrow stem cell functions of Zn-incorporated TiO2 coatings on titanium. Acta Biomaterialia 8 (2): 904-915.
- Xu J, Ding G, Li J, Yang S, Fang B, et al. (2010) Zinc-ion implanted and deposited titanium surfaces reduce adhesion of Streptococccus mutans. Applied surface science 256(24): 7540-7544.
- Koutouziz T, Richardson J, Lundgren T (2011) Comparative soft and hard tissue responses to titanium and polymer healing abutments. J Oral Implantol 37: 174-182.
- Hahnel S, Wieser A, Lang R, Rosentritt M (2015) Biofilm formation on the surface of modern implant abutment materials. Clinical oral implants research 26(11): 1297-1301.
- Ratner BD (1995) Surface modification of polymers: chemical, biological and surface analytical challenges. Biosens Bioelectron 10(9-10): 797–804.
- Dos Santos FS, Vieira M, Da Silva HN, Tomás H, Fook MV (2021) Surface Bioactivation of Polyether Ether Ketone (PEEK) by Sulfuric Acid and Piranha Solution: Influence of the Modification Route in Capacity for Inducing Cell Growth. Biomolecules 11(9): 1260.
- Rea M, Ricci S, Ghensi P, Lang NP, Botticelli D, et al. (2017) Marginal healing using Polyetheretherketone as healing abutments: an experimental study in dogs. Clinical oral implants research 28(7): 46-50.
- Zoidis P (2018) The all-on-4 modified polyetheretherketone treatment approach: a clinical report. J Prosthet Dent 119(4): 516-521.
- Keul C, Liebermann A, Schmidlin PR, Malgorzata Roos, Beatrice Sener, et al. (2014) Influence of PEEK surface modification on surface properties and bond strength to veneering resin composites. J Adhes Dent 16: 383-392.
- Keul C, Liebermann A, Schmidlin PR, Roos M, Sener B, et al. (2014) Influence of PEEK surface modification on surface properties and bond strength to veneering resin composites. J Adhes Dent 16(4): 383-392.
- Ourahmoune R, Salvia M, Mathia TG, Mesrati N (2014) Surface morphology and wettability of sandblasted PEEK and its composites. Scanning 36(1): 64-75.
- Miguel de Araújo Nobre, Carlos Moura Guedes, Ricardo Almeida, António Silva, Nuno Sereno, et al. (2020) Hybrid Polyetheretherketone (PEEK)–Acrylic Resin Prostheses and the All-on-4 Concept: A Full-Arch Implant-Supported Fixed Solution with 3 Years of Follow-Up 9(7): 2187.
- Zoidis P, Bakiri E, Polyzois G (2017) Using modified polyetheretherketone (PEEK) as an alternative material for endocrown restorations: a short-term clinical report. J Prosthet Dent 117(3): 335-339.
- Zoidis P, Bakiri E, Papathanasiou I, Zappi A (2017) Modified PEEK as an alternative crown framework material for weak abutment teeth: a case report. Gen Dent 65(5): 37-40.
- Wagner C, Stock V, Merk S, Schmidlin PR, Roos M, et al. (2018) Retention Load of Telescopic Crowns with Different Taper Angles between Cobalt‐Chromium and Polyetheretherketone Made with Three Different Manufacturing Processes Examined by Pull‐Off Test. Journal of Prosthodontics 27(2): 162-168.
- Zoidis P, Papathanasiou I (2016) Modified PEEK resin-bonded fixed dental prosthesis as an interim restoration after implant placement. J Prosthet Dent 116(5): 637-641.
- Noiset O, Schneider YJ, Marchand-Brynaert J (2000) Adhesion and growth of CaCo2 cells on surface-modified PEEK substrata. J Biomater Sci Polym Ed 11(7): 767-786.
- Sproesser O, Schmidlin PR, Uhrenbacher J, Roos M, Gernet W, et al. (2014) Effect of sulfuric acid etching of polyetheretherketone on the shear bond strength to resin cements. J Adhes Dent 16(5): 465-472.
- Gama LT, Duque TM, Özcan M, Philippi AG, Mezzomo LAM, et al. (2020) Adhesion to highperformance polymers applied in dentistry: a systematic review. Dent Mater 36: 93-108.
- Behr M, Zeman F, Passauer T, Michael Koller, Sebastian Hahnel, et al. (2012) Clinical performance of cast clasp-retained removable partial dentures: a retrospective study. Int J Prosthodont 25(2): 138-144.
- Fueki K, Ohkubo C, Yatabe M, Ichiro Arakawa , Masahiro Arita, et al. (2014) Clinical application of removable partial dentures using thermoplastic resin-part I: definition and indication of non-metal clasp dentures. J Prosthodont Res 58(1): 3-10.
- Arda T, Arikan A (2005) An in vitro comparison of retentive force and deformation of acetal resin and cobaltchromium clasps. J Prosthet Dent 94(3): 267- 274.
- Katzer A, Marquardt H, Westendorf J (2002) Polyetheretherketone–cytotoxicity and mutagenicity in vitro. Biomaterials 23(8): 1749- 1759.
- Adler S, Kistler S, Kistler F (2013) Compression-moulding rather than milling: a wealth of possible applications for high performance polymers. Quintessenz Zahntechnik 39: 376- 384.
- W Maryod, E Taha (2019) Impact of Milled Peek Versus Conventional Metallic Removable Partial Denture Frameworks on the Abutment Teeth in Distal Extension Bases. A Randomized Clinical TrialInter J Prost h Or H 5(3): 20-27.
- Mayinger F, Micovic D, Schleich A, Malgorzata Roos, Marlis Eichberger, et al. (2021) Retention force of polyetheretherketone and cobalt-chromemolybdenum removable dental prosthesis clasps after artificial aging. Clin Oral Invest, pp. 3141-3149.
- Costa Palau S, Torrents-Nicolas J, Brufau-de Barberà M, Cabratosa-Termes J (2014) Use of polyetheretherketone in the fabrication of a maxillary obturator prosthesis: a clinical report. J Prosthet Dent 112(3): 680-682.
- Hahnel S, Scherl C, Rosentritt M (2018) Interim rehabilitation of occlusal vertical dimension using a double-crownretained removable dental prosthesis with polyetheretherketone framework. The Journal of prosthetic dentistry 119(3): 315-318.
- Ierardo G, Luzzi V, Lesti M, Vozza I, Brugnoletti O, et al. (2007) Peek polymer in orthodontics: A pilot study on children. J Clin Exp Dent 9(10): 1271-1275.
- Maekawa M, Kanno Z, Wada T, Hongo T, Doi H, et al. (2015) Mechanical properties of orthodontic wires made of super engineering plastic. Dent Mater J 34: 114-119.
- Shirakawa N, Iwata T, Miyake S, Otuka T, Koizumi S, et al. (2018) Mechanical properties of orthodontic wires covered with a polyether ether ketone tube. The Angle Orthodontist 88(4): 442-449.
- Kadhum AS, Alhuwaizi AF (2021) The efficacy of polyether‐ether‐ketone wire as a retainer following orthodontic treatment. Clinical and experimental dental research 7(3): 302-312.
- Wu XL, Zheng H, Liu YJ, Leng JS (2010) THERMOMECHANICAL PROPERTY OF EPOXY SHAPE MEMORY POLYMERS. Int J Mod Phys B 24(16): 2386-2391.
- B Huang, J Qian, G Wang, M Cai (2014) Synthesis and properties of novel copolymers of poly (ether ketone diphenyl ketone ether ketone ketone) and poly (ether amide ether amide ether ketone ketone). Polym Eng Sci 54(8): 1757-1764.
- Fuhrmann G, Steiner M, Freitag-Wolf S, Kern M (2014) Resin bonding to three types of polyaryletherketones (PAEKs)—durability and influence of surface conditioning. Dental Materials 30(3): 357-363.
- Guo R, McGrath J (2012) Polymer science: a comprehensive reference. In: Matyjaszewski K, Möller M (Eds.)., Amsterdam: Elsevier, pp. 377-430.
- C Song J, Choi Y, Jeon C, Jeong S, Lee E, et al. (2018) Comparison of the microtensile bond strength of a polyetherketoneketone (PEKK) tooth post cemented with various surface treatments and various resin cements. Materials 11(6): 916.
- Lümkemann N, Eichberger M, Stawarczyk B (2017) Different PEEK qualities irradiated with light of different wavelengths: Impact on Martens hardness. Dent Mater, pp. 968-975.
- Bechir ES, Bechir AN, Gioga CH, Manu R, Burcea AL, et al. (2016) The advantages of BioHPP polymer as superstructure material in oral implantology. Materiale Plastice 53(3): 394-398.
- Campbell SD, Cooper L, Craddock H, Hyde TP, Nattress B, et al. (2017) Removable partial dentures. The clinical need for innovation. J Prosthet Dent 118: 273-280.
- Han X, Yang D, Yang C, Spintzyk S, Scheideler L, et al. (2019) Carbon fiber reinforced PEEK composites based on 3D-printing technology for orthopedic and dental applications. Journal of clinical medicine 8(2): 240.

 Review Article
Review Article