Short Communication
We report the case of 59 years-old man with history of arterial hypertension, heavy smoking and obesity. The patient has presented effort angina two weeks before he had a cardiac arrest while effort (preceded by severe chest pain). The patient immediately received two defibrillations for ventricular tachycardia and cardiopulmonary resuscitation. Then, the prehospital thrombolysis was administrated. The low flow time was 30 min. The ECG post resuscitation showed a right bundle branch block with premature ventricular complexes. In coronary angiography, double simultaneous culprit occlusion of the proximal left anterior descending (LAD1) coronary artery and the distal left circumflex (LCX 3) associated to chronic total occlusion of the proximal right coronary artery (RCA) were found (Figures 1 & 2). A double angioplasty with stenting of LAD 1 and LCX 3 was performed. Transthoracic echocardiography showed left ventricule ejection fraction of 30% with extensive akinesia of anterior wall. The post resuscitation care was continued including a therapeutic hypothermia (36°) to optimize the neurological prognosis and hemodynamic optimization with inotropic and vaso-pressive agents. The evolution was unfavorable with anoxic encephalopathy and death at 9 days after admission. The simultaneous coronary occlusions resulting in acute myocardial infarction remain rare (1.3-2.5% in PCI vs 25-50% in autopsy). Many factors are thought to be behind the multiple coronary occlusion such inflammatory response, hyper-catecholaminergic secretion, arterial hypotension, hyper-coagulopathy, coronary embolism and coronary artery spasm. An urgent angiography within 2 hours with revascularization of all culprit coronary lesions should be considered in survivors of cardiac arrest, including unresponsive survivors, when there is a high index of suspicion of ongoing infarction such as the presence of chest pain before arrest, a history of established coronary artery disease, and abnormal or uncertain ECG results.
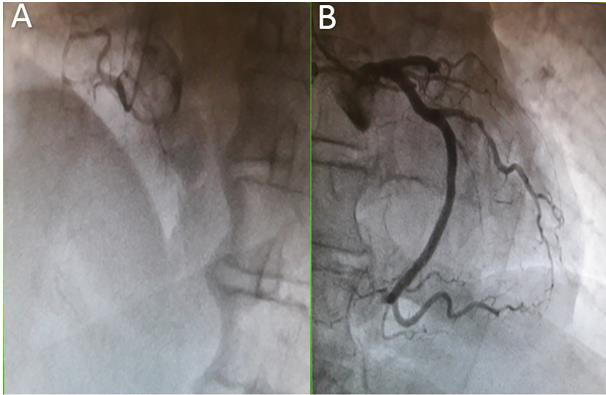
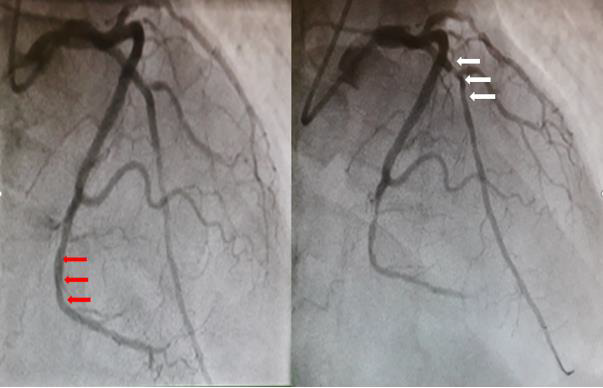
Figure 1: The coronary angiogram in left anterior oblique projection 30°(A) showing chronic total occlusion of the proximal right coronary artery (RCA) and right anterior oblique projection with caudal angulation (B) showing occlusion of the proximal left anterior descending (LAD1) coronary artery and the distal left circumflex (LCX 3).

 Review Article
Review Article