Introduction
A handful of rare and newly reported dermatoses have come into light following COVID-19 infection. While most manifestations are benign are transient, there are also a handful of reports of COVID-19 triggering a chronic dermatosis [1]. Although there are reports of triggers and flares of various morphological variants of psoriasis following COVID-19 infection, there is no such report of trigger of napkin psoriasis following the viral infection [2,3].
Case Report
A 6 months old female child presented to our skin out patient
department with the parents complaining of development of
whitish pink macerated lesions in her groin since 3 weeks. On
examination there was presence of well-defined bilaterally
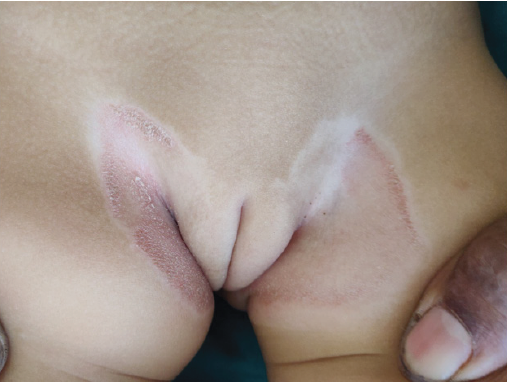
symmetrical fine scaly erythematous and slightly indurated plaques
in intertriginous areas of groin, buttocks and anogenital region
(Figure 1). The parents reported that the child had developed a lab
proven COVID-19 infection 2 months back, which she presumably
contracted from her infected mother. The onset of her cutaneous
lesions had begun 5 weeks following the infection, while she
experienced a respiratory flare in her symptoms. Current lab
investigations revealed the girl to be RTPCR negative for COVID-19.
Rest of the lab investigations were unremarkable. The child also
had an optimum weight, height and milestones for her age. The
KOH and fungal culture of lesional scraping and woods’ lamp was
negative. The child was diagnosed with inverse or flexural psoriasis
on the basis of striking clinical picture which further got confirmed
by histopathological analysis.
Biopsy findings included hyperkeratosis, fused rete ridged,
suprapapillary thinning, and dilated tortuous dermal blood vessels.
The child was prescribed hydrocortisone lotion and pemicrolimus
ointment, along with oral antihistaminincs.
Discussion
The only variant of psoriasis presumed to have a definitive correlation following a systemic infection is guttate psoriasis. It is triggered following a staphylococcal infection and seen predominantly in children and young adults [4]. Various other genetic, environmental and idiopathic factors have also been reported to be responsible for triggering psoriasis. In fact. Even respiratory viral triggers, including COVID-19, are being reported. A viral infection can lead to immune dysregulation which stimulated TLR-3 which can stimulate CXCL8 and IL-36 [5]. As the novel COVID-19 evolves and unfolds it is only obvious that its myriad manifestations and complications will unravel. Skin being the largest organ has a great potential of being perhaps the greatest target of various immune deregulatory sequalae of this infection, especially in long haulers. Although our patient had a favourable clinical course with rapid recovery, the potential long term complications of COVID-19 are still unpredictable.
Conclusion
To the best of our knowledge this is the first such case of napkin psoriasis triggered by COVID-19. A dermatologist must always be on the look out to differentiate such presentation from other similar looking spotters like candida intertrigo, tinea cruris, and acrodermatitis enteropathica to name a few.
References
- Mohta A, Mohta A, Nai RS, Arora A, Jain SK, et al. (2021) An Observational Study of Mucocutaneous Manifestations among SARS-CoV-2 Patients from Three COVID-19 Dedicated Tertiary Care Centers. Indian Dermatol Online J 12(5): 687-695.
- Ozaras R, Berk A, Ucar DH, Duman H, Kaya F, et al. (2020) Covid-19 and exacerbation of psoriasis. Dermatol Ther 33(4): e13632.
- Gananandan K, Sacks B, Ewing I (2020) Guttate psoriasis secondary to COVID-19. BMJ Case Rep 13(8): e237367.
- Telfer NR, Chalmers RJ, Whale K, Colman G (1992) The role of streptococcal infection in the initiation of guttate psoriasis. Arch Dermatol 128: 39-42.
- Sbidian E, Madrange M, Viguier M, Salmona M, Duchatelet S, et al. (2019) Respiratory virus infection triggers acute psoriasis flares across different clinical subtypes and genetic backgrounds. Br J Dermatol 181: 1304-1306.

 Case Report
Case Report