Abstract
Although several therapeutic agents have been evaluated for the treatment of coronavirus disease 2019 or Covid-19, no antiviral agents have yet been shown to be efficacious. Many more anti-viral medicines, antibiotics, minerals, vitamins and flavonoids are being worked upon to attain beneficial after effects. Diligent efforts for the development of vaccines are in their developing stages. Till then most important is to take the preventive measures and to rely on the available alternates. This update deals with the review of the available medicines, which are being used right now to combat Covid-19.
Keywords:Corona; Virus; Treatment; Vaccine; Regimen; Medicine
Mini Review
Coronaviruses are viruses that cause illness in humans and animals. Coronaviruses can infect people and then spread between people, as seen with MERS and SARS [1]. The outbreak of Novel coronavirus disease or COVID19 was initially noticed in Wuhan city of China in mid-December, 2019, has now travelled to several countries worldwide [2]. WHO has declared this as a “Public Health Emergency of International Concern” on 30thJanuary 2020? WHO later on declared COVID-19 a pandemic on 11th March, 2020 [3]? Front-line clinicians have promoted a multi-disciplinary approach to care for patients with COVID-19, including those with mild, moderate, severe, and critical disease as depending on severity of infection, with government concern [4]. The aspects of COVID-19 care as treatment of acute and chronic infections, ethical principles, and reporting of death are wider areas of concern [5]. Patients with a mild clinical symptom may not require hospitalization, and many will be able to manage their illness at home. The decision to monitor a patient should be made on a case-by-case basis [6]. The symptoms of coronavirus disease are as follows:
A. Fever
B. Cough
C. Fatigue
D. Shortness of breath
E. Expectoration
F. Myalgia
G. Rhinorrhea, sore throat, diarrhea [7]
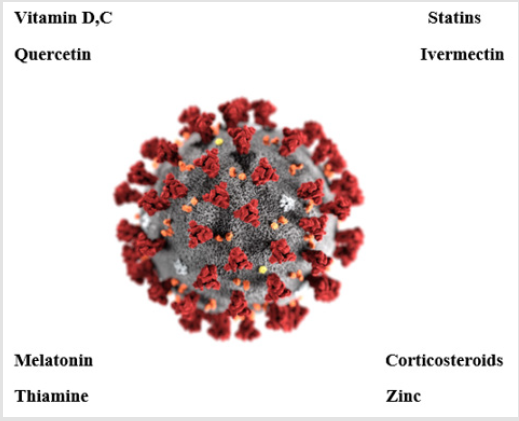
The present article is based on the different treatment regimen as in Figure 1 based on the severity of infection.
Testing for Infection
Diagnosis of COVID-19 is essential in order to detect SARSCoV-
2 RNA by Antigen test and by RT-PCR. Detection of SARS-CoV-2
viral RNA is better in nasopharynx samples compared with throat
samples. Lower respiratory samples may have better viral yield
than upper respiratory samples.SARS-CoV-2 antigen tests can also
be used in a variety of testing strategies. SARS-CoV-2 RNA has also
been detected in stool and blood. Detection of SARS-CoV-2 RNA in
blood may be a marker of severe illness [8].
Prophylaxis: While there is extremely limited data, the
mentioned combination may have a role in the prevention of
COVID-19 disease. A recent publication suggests that melatonin
may reduce the risk of COVID-19 infection, [9] Melatonin, a wellknown
anti-inflammatory and anti-oxidative molecule, is protective
against virus and other pathogens. Melatonin is effective in critical
care by reducing vessel permeability, anxiety and improving
sleeping quality, which might also be beneficial for better results
for COVID-19 patients. Notably, melatonin has a high safety profile.
Even when melatonin was given at dose of 1 gm. /day for a month
in humans, there were no adverse effects of the treatment [10,11].
Many papers suggest that Vitamin D deficiency increases the risk of
infection and is associated with a significantly worse result. Vitamin
D favorably corrects host responses to severe acute respiratory
syndrome coronavirus 2 or SARS-CoV-2, both in the early viraemic
and later phases of COVID-19. Vitamin D metabolites have been
known to promote innate antiviral mechanisms [12-14]. Lower
circulating 25(OH) D concentrations have also been reported to
relate to SARS-CoV-2 infection. Possibility persists that vitamin
D deficiency might arise as a result of pulmonary inflammation.
COVID-19 in populations where vitamin D deficiency is prevalent;
has to be worked upon its consequences [15,16].
Vitamin C: Low dose (0.5–2 g/d) of it may have benefits when
used early in severe acute respiratory syndrome coronavirus 2
infections. 500 mg twice daily is extremely helpful. Vitamin C
especially at high doses can reduce mediators such as interleukin-6
and endothelin-1. Thus, vitamin C also helps with severe late-stage
coronavirus disease 2019. Vitamin C, as an essential micronutrient
for humans and as free radical scavenger, is beneficial for severe
viral respiratory tract infections [17]. It is known to support
various cellular functions of both innate and adaptive immune
systems, including adapting vulnerability to various viral infections
[18,19]. In chick embryo tracheal organ cultures, vitamin C, was
found to increase resistance to infection by a coronavirus [20-22].
As an anti-oxidant, the vitamin might help to protect cells from free
radicals damage. Vitamin C supplements on regular usage shortens
the common cold duration [23]. It is likely that this antiviral effect is
why vitamin C is a possible treatment of COVID-19 [24].
Quercetin: 3,3′,4′5,7-pentahydroxyflavone, is a widely
distributed plant flavonoid, found in several vegetables, leaves,
seeds, and grains, where it combines with sugars to form quercetin
glycosides. Studies suggest that quercetin supplementation
promotes antioxidant, anti-inflammatory, antiviral, and immunoprotective consequences [25]. Quercetin has been
studied in various types and models of viral infection due to its
antiviral properties in inhibiting polymerases, proteases, reverse
transcriptase and binding viral capsid proteins [26,27].
Symptomatic Patients Care at Home
Famotidine: H2 receptor blocker FAMOTIDINE came to limelight due to its role in reducing the symptoms of COVID-19 patients. A lower peak ferritin value among users of famotidine, supported the hypothesis that its use may decrease cytokine release in the setting of SARS-CoV-2 infection. A randomized controlled trial is currently is under process to prove whether famotidine can improve clinical aspects in hospitalized patients with COVID-19 [28]. Famotidine is one of the highest-ranked matches for drugs predicted to bind 3CLpro,3 receptor, a SARS-CoV-2 protease that generates non structure proteins critical to viral replication as per molecular modeling concepts [28]. Famotidine is known to inhibit human immunodeficiency virus replication without affecting lymphocyte viability [29,30].
Ivermectin: Is a drug of wide range bioactivity and has been in use for treatment of parasitic infections in humans .It can act as a possible target drug for SARS CoV-2 and is under extensive research? It is used in a dose of 0.15 mg/kg–0.2 mg/kg body weight for most of the parasitic infestations as oral tablet [31]. The antiviral properties of ivermectin have been tested against human virus as several RNA viruses, such as Zika virus, Influenza A virus, Newcastle disease virus, Chikungunya virus, Yellow fever virus, Dengue virus and DNA virus such as Equine herpes virus type 1 [32,33].
Mildly Symptomatic Patients
Zinc: Possesses a variety of direct and indirect antiviral properties, which are realized by different contrivances. Zinc supplement has a potential to enhance antiviral immunity, both innate and humoral, to restore depleted immune cell function and to improve normal immune cell function. It acts in a synergistic manner when co-administered with the standard antiviral therapy, as in patients with hepatitis C, HIV, and SARS-CoV-1. Zinc is effective to act by physical processes, such as virus attachment, infection, and uncoating [34-36]. Anti- apoptotic effects could result in an increase in the number of T helpers. It also induces inhibition of trans capillary movement of plasma proteins and reduce local edema, inflammation. Finally, Zinc may also stabilize the cell membrane which governs inhibition of the entry of the virus into the cell [37,38].
Respiratory complications
Corticosteroids: Although corticosteroid therapy improves viral pneumonia in some cases, there is no confirmed evidence till now of corticosteroid therapy reducing the mortality of COVID-19 patients. Higher concentration of cytokines and chemokines were detected in patients with severe disease. When the virus invades airway epithelial cells and alveolar epithelial cells, it causes stimulation of specific immune cells are stimulated to produce massive amounts of cytokines and chemokines rapidly, such as tumour necrosis factor-α, interleukin-1or IL-1, IL-6, IL-12 and IL-8 [39-42].
Methylprednisolone: Application of glucocorticoid for COVID-19 pneumonia has been controversial, considering the clinical evidence and their possible adverse effects. However, it is well known that glucocorticoids are useful for inhibiting the inflammatory storm via suppression of cytokine levels and proinflammatory gene expression. Glucocorticoids thus can diminish the serous exudate at the site of inflammation, reduce tissue edema and injury, and relieve symptoms of inflammation, may prove vital to combat symptoms of Covid-19 [43,44].
Additional Treatment Components
Thiamine: As antibodies, and mainly T-cells, are required to fight SARS-CoV-2 virus, thiamine deficiency can result in insufficient antibody responses, and subsequently more severe symptoms. Hence, adequate thiamine levels are likely to support proper immune responses during SARS-CoV-2 infection [45].
Magnesium: Magnesium supplementation has been shown to act against variety of disorders or diseases related to respiratory system, reproductive system, nervous system, digestive system, and cardiovascular system, diabetes and cancer. Serum magnesium level in COVID-19 patients need to be monitored. Mg supplementation reduces CRP levels in individuals with inflammation of CRP levels > 3 mg/dL. In a recent study, it has been shown that Mg supplementation diminishes disease severity and accelerates speedy recovery [46-48].
Atorvastatin: Statins are well known for their antiinflammatory effects, and some recovery centers included them in the COVID-19 treatment protocol. In addition, studies in vitro suggested that statins exert anti-viral activity and may hamper the activity of enveloped viruses”. Statins possess anti-inflammatory and immunomodulatory properties. On the other hand, statins increase the cellular expression of ACE2, the primary receptor for SARS-CoV-2. Hence, the outcome of statins on COVID-19 upshots deserves examination [49,50].
Future Prospects
A vaccine for the coronavirus will likely be ready by early 2021 but rolling it out safely across India’s 1.3 billion people will be the country’s biggest challenge in fighting its surging epidemic. India’s indigenous vaccine developers Bharat Biotech International Ltd. are at the second-phase human trial stage and Zydus Cadila is in the process to receive approvals for conducting third-phase clinical trials. Till then the preventive steps have to be followed fully, in order to get protected from Covid-19.
Conclusion
Although SARS-CoV-2 can be deadly, it has mild-mannered cousins called seasonal coronaviruses that are among the causes of the common cold. Some scientists have suggested that people might be shielded from SARS-CoV-2 infection if they have recently been infected by a seasonal coronavirus. Till the vaccine development as well as its availability, it is most important is to take the necessary precautions and to use the available alternates.
References
- Ye ZW, Yuan S, Yuen KS, Fung SY, Chan CP, et al. (2020) Zoonotic origins of human coronaviruses. Int J Biol Sci 16(10): 1686-1697.
- Mackenzie JS, Smith DW (2020) COVID-19: a novel zoonotic disease caused by a coronavirus from China: what we know and what we don't . Microbiol Aust, MA20013.
- Sohrabi C, Alsafi Z, O Neill N, Mehdi K, Ahmed K, et al. (2020) World Health Organization declares global emergency: A review of the 2019 novel coronavirus (COVID-19). Int J Surg 76: 71-76.
- Wei M, Yuan J, Liu Y, Fu T, Yu X, et al. (2020) Novel Coronavirus Infection in Hospitalized Infants Under 1 Year of Age in China. JAMA 2020.
- Chan JF, Yuan S, Kok KH, Kelvin KW, Hin C, et al. (2020) A familial cluster of pneumonia associated with the 2019 novel coronavirus indicating person-to-person transmission: a study of a family cluster. Lancet 395: 514-523.
- Hu Z, Song C, Xu C, Jin G, Chen Y, et al.(2020) Clinical characteristics of 24 asymptomatic infections with COVID-19 screened among close contacts in Nanjing, China. Sci China Life Sci 63: 706-711.
- Wang Y, Liu Y, Liu L, Wang X, Luo N, et al. (2020) Clinical outcome of 55 asymptomatic cases at the time of hospital admission infected with SARS-Coronavirus-2 in Shenzhen, China. J Infect Dis 221(11): 1770-1774.
- Reiter RJ, Ma Q, Sharma R (2020) Treatment of Ebola and other infectious diseases: melatonin “goes viral” Melatonin Res 3: 43-57.
- Wu X, Ji H, Wang Y, Gu C, Gu W, et al. (2019) Melatonin alleviates radiation-induced lung injury via regulation of miR-30e/NLRP3 axis. Oxidative Med Cell Longev 2019: 4087298.
- Zhang R, Wang X, Ni L, Di X, Ma B, et al. (2020) COVID-19: Melatonin as a potential adjuvant treatment. Life Sci 250: 117583.
- Hemila H (2017) Zinc lozenges and the common cold: a meta-analysis comparing zinc acetate and zinc gluconate, and the role of zinc dosage. J Royal Soc Med Open 8: 1-7.
- Singh M, Das RR (2013) Zinc for the common cold. Cochrane Database of Syst Rev 6: CD001364.
- Hoeger J, Simon TP, Beeker T, Marx G, Haase H (2017) Persistent low serum zinc is associated with recurrent sepsis in critically ill patients - A pilot study. PloS ONE 12(5): e0176069.
- Freedberg DE, Conigliaro J, Sobieszczyk ME, Markowitz DD, et al. (2020) Famotidine use is associated with impoved clinical outcomes in hospitalized COVID-19 patients: A propensity score matched retrospective cohort study. medRxiv.
- D Avolio A, Avataneo V, Manca A, Cusato J, Nicolo A, et al. (2020) 25-hydroxyvitamin D concentrations are lower in patients with positive PCR for SARS-CoV-2. Nutrients 12(5): 1359.
- Hastie CE, Mackay DF, Ho F, Morales C, Srinivasa V, et al. (2020) Vitamin D concentrations and COVID-19 infection in UK Biobank. Diabetes Metab Syndr 14(4): 561-565.
- Janowitz T, Baglenz E, Pattinson D, Wang TC, Conigliaro J, et al. (2020) Famotidine use and quantitative symptom tracking for COVID-19 in non-hospitalized patients: a case series. Gut 69(9):1592-1597.
- Mather JF, Seip RL, Mc Kay RG (2020) Impact of famotidine use on clinical outcomes of hospitalized COVID-19 patients. Am J Gastroenterol.
- Chroboczek T, Lacoste M, Wackenheim C, Challan Belval T, Amar B, et al. (2020) Beneficial effect of corticosteroids in severe COVID-19 pneumonia: a propensity scores matching analysis. medRxiv.
- Wu C, Chen X, Cai Y, Xia J, Zhou X, et al. (2020) Risk factors associated with acute respiratory distress syndrome and death in patients with Coronavirus disease 2019 pneumonia in Wuhan ,China. JAMA Intern Med.
- Cruz AF, Ruiz Antoran B, Gomez AM, Lopez AS (2020) Impact of glucocorticoid treatment in SARS-CoV-2 infection mortality: A retrospective controlled cohort study. medRxiv.
- Liu J, Zheng X, Huang Y, Shan H, Huang J (2020) Successful use of methylprednisolone for treating severe COVID-19. J Allergy Clin Immunol 146(2): 325-327.
- Meduri GU, Bridges L, Shih MC, Marik PE, Siemienluk RA, et al. (2016) Prolonged glucocorticoid treatment is associated with improved ARDS outomces: analysis of individual patients’ data from four randomized trials and trial-level meta-analysis of the updated literature. Intensive Care Med 42(9): 829-840.
- (2020) WHO Association between administration of systemic corticosteroids and mortality among critically ill patients with COVID-19. A meta-analysis. JAMA 2020 324(13): 1330-1341.
- Spedding G, Ratty A, Middleton E Jr (1989) Inhibition of reverse transcriptases by flavonoids. Antiviral Res 12: 99-110.
- Cushnie TP, Lamb AJ (2005) Antimicrobial activity of flavonoids. Int J Antimicrob Agents 26: 343-356.
- Debiaggi M, Tateo F, Pagani L, Luini M, Romero E (1990) Effects of propolis flavonoids on virus infectivity and replication. Microbiologica 13: 207-213.
- Freedberg DE, Conigliaro J, Wang TC, Tracy Kevin, Michael V, et al. (2020) Famotidine Use Is Associated with Improved Clinical Outcomes in Hospitalized COVID-19 Patients: A Propensity Score Matched Retrospective Cohort Study. Gastroenterology 59(3): 1129-1131.
- Gupta D, Sahoo AK, Singh A (2020) Ivermectin: potential candidate for the treatment of Covid 19. Braz J Infect Dis 24: 369.
- Heidary F, Gharebaghi R (2020) Ivermectin: a systematic review from antiviral effects to COVID-19 complementary regimen. J Antibiot (Tokyo) 73: 593-602.
- Õmura S (2008) Ivermectin: 25 years and still going strong. Int J Antimicrob Agents 31: 91-98.
- Caly L, Druce JD, Catton MG, Jans DA, Wagstaff KM (2020) The FDA-approved drug ivermectin inhibits the replication of SARS-CoV-2 in vitro. Antivir Res 178: 104787.
- Momekov G, Momekova D (2020) Ivermectin as a potential COVID-19 treatment from the pharmacokinetic point of view: antiviral levels are not likely attainable with known dosing regimens. Biotechnol Biotechnol Equip 34: 469-474.
- Perry DK, Smyth MJ, Stennicke HR, Dureiz P, Poirier, et al. (1997) Zinc is a potent inhibitor of the apoptotic protease, caspase 3: a novel target for zinc in the inhibition of apoptosis. J Biol Chem 272: 18530-18533.
- Novick SG, Godfrey JC, Pollack RL, Wilder HR (1997) Zinc-induced suppression of inflammation in the respiratory tract, caused by infection with human rhinovirus and other irritants. Med Hypotheses 49: 347-357.
- Perry DK, Smyth MJ, Stennicke HR (1997) Zinc is a potent inhibitor of the apoptotic protease, caspase-3: a novel target for zinc in the inhibition of apoptosis. J Biol Chem 272: 18530-18533.
- Schoggins JW, Wilson SJ, Panis M (2011) A diverse range of gene products are effectors of the type I interferon antiviral response. Nature 472: 481-485.
- Himoto T, Masaki T (2018) Associations between zinc deficiency and metabolic abnormalities in patients with chronic liver disease. Nutrients 10: E88.
- Channappanavar R, Perlman S (2017) Pathogenic human coronavirus infections: causes and consequences of cytokine storm and immunopathology. Semin Immunopathol 39: 529-539.
- Wong CK, Lam CWK, Wu AKL, Ip WK, Lee NL, et al. (2004) Plasma inflammatory cytokines and chemokines in severe acute respiratory syndrome. Clin Exp Immunol 136: 95-103.
- Mahallawi WH, Khabour OF, Zhang Q, Makhdoum HM, Suliman BA (2018) MERS-CoV infection in humans is associated with a pro-inflammatory Th1 and Th17 cytokine profile. Cytokine 104: 8-13.
- Zhou P, Yang XL, Wang XG, Hu B, Zhang L, et al. (2020) pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature 579: 1-4.
- Darwish I, Mubareka S, Liles WC (2011) Immunomodulatory therapy for severe influenza. Expert Rev Anti-infect Ther 9: 807-822.
- Shang L, Zhao J, Hu Y, Du R, Cao B (2020) On the use of corticosteroids for 2019-nCoV pneumonia. Lancet (London, England) 395: 683.
- Chen RC, Tang XP, Tan SY, Liang BL, Wan ZY, et al. (2006) Treatment of severe acute respiratory syndrome with glucosteroids: the Guangzhou experience. Chest 129: 1441-1452.
- Marini JJ, Gattinoni L (2020) Management of COVID-19respiratory distress. JAMA.
- Baaij JH, Hoenderop JG, Bindels RJ (2015) Magne-sium in man: implications for health and disease. Physiol Rev 95: 1-46.
- Fulgoni VL, Keast DR, Bailey RL, Dwyer J (2011) Foods, fortificants, and supplements: where doAmericans get their nutrients? J Nutr 141: 1847-1854.
- Henriksbo BD, Lau TC, Cavallari JF, Denou E, Chi W, et al. (2014) Fluvastatin causes NLRP3 inflammasome-mediated adipose insulin resistance. Diabetes 63: 3742-3747.
- Pertzov B, Eliakim Raz N, Atamna H, Trestioreanu AZ, Yahav D, et al. (2019) Hydroxymethylglutaryl-CoA reductase inhibitors (statins) for the treatment of sepsis in adults - A systematic review and meta-analysis. Clin Microbiol Infect 25: 280-289.

 Mini Review
Mini Review