Abstract
Revision of total hip arthroplasty (THA) is uncommon but is commonly indicated in the setting of component wear, osteolysis, dislocation, and infection. Here we report a case of catastrophic failure of the fiber metal mesh junction of the Zimmer VerSys Epoch femoral stem without precipitating trauma or infection. A 63-year-old woman, with morbid obesity and index primary total hip arthroplasty 13 years prior, was found to have osteolysis of the proximal femoral component with subsequent implant loosening and intraoperative findings suggestive of metallosis. After removal of the femoral component with trochanteric osteotomy, cerclage cables were used to secure a revision component.
Introduction
Since Dr. Austin T. Moore first introduced a metal prosthesis
for total hip arthroplasty (THA) in 1940, it has been a largely
successful surgery, with excellent clinical outcomes at 15-20 years
[1-3]. Beginning in the 1980s, advancements lead to cement-less
THA, which demonstrate decreased rates of revision and decreased
annual subsidence [4]. Studies have determined the most common
prosthetic component failures include polyethylene failure, modular
acetabular dissociations, femoral stem fractures, dissociation of the
femoral head and neck, and ceramic head fractures [5]. The cementless
Zimmer VerSys system has demonstrated more favorable pain
scores, increased range of motion, and lower rates of revision at
later follow-up [6,7]. The Zimmer VerSys Epoch system has been
designed for reduced stiffness and porous ingrowth. It utilizes a
cobalt-chromium-molybendenum core for strength of the femoral
component and a polyetheretherketone (PEEK) polymer matrix
for a lower modulus of elasticity. The outer layer of titanium fiber
metal mesh allows for porous bone ingrowth. Reduced stiffness
reduces stress shielding and thigh pain for patients postoperatively
with total hip arthroplasty.
Catastrophic failure of THA components is rare, with rates
reported at less than 0.5% [5,8]. There have been two reported
cases of the VerSys system femoral stem failure secondary to
chronic prosthetic infection [9]. The authors hypothesized that
the additional interface between the fiber metal mesh and cobalt
chrome core was susceptible to mechanical breakdown in the face
of chronic infection, causing the fiber mesh to de-bond from the
cobalt-chromium-molybendenum core. However, here we describe
a case report of the fiber metal mesh junction in a morbidly obese
patient with no signs of previous trauma, infection, or dislocation.
Case Report
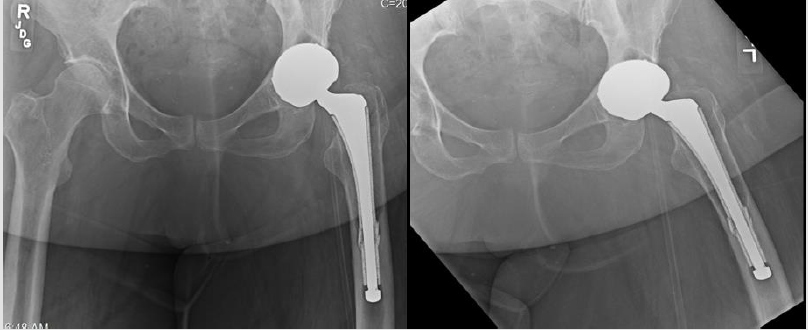
In July 2017, a 63-year-old female, with a past medical history of morbid obesity, presented 13 years after left THA with worsening, severe left hip and thigh pain over the past two months. She denied any traumatic episode. At presentation, she had been admitted to a rehabilitation unit due to an inability to ambulate. On physical examination, her BMI was calculated to 56.89. She described groin pain with rotation. There was no visible injury. Her incision was wellhealed with no erythema or sign of infection. Pelvic radiographs demonstrated osteolysis of the proximal femoral component with subsequent implant loosening (Figure 1). The patient was diagnosed with osteolysis, metallosis, and loosening of total hip arthroplasty femoral component with catastrophic implant failure. Due to her inability to ambulate and increasing pain, she elected to move forward with a revision total hip arthroplasty of the femoral component and bearing surface. Preoperative lab testing was not suspicious for any infection.
Figure 1: In-office (A) AP and (B) lateral radiographs of the left hip demonstrate loosening of the implant, osteolysis of the proximal aspect of the femoral compartment (black arrow), and catastrophic failure of the femoral stem fiber metal mesh junction (white arrow). Also noted was use of a metal-on-metal bearing surface. Implant was identified as a Zimmer VerSys Epoch femoral stem (Zimmer, Warsaw, IN).
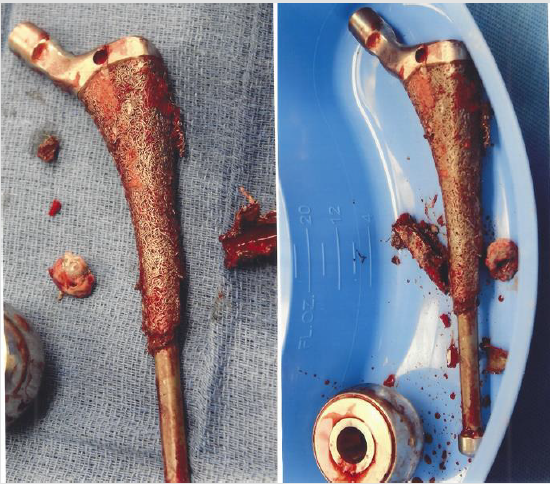
Figure 2: Intraoperative photo of explanted Zimmer VerSys Epoch stem. Failure of the femoral stem and the fiber metal mesh junction was noted.
In October 2017, patient underwent surgical intervention. Significant scarring was noted on approach. Intraoperative gram stain and cultures were negative on final reads. Significant amounts of grayish, dense fibroconnective tissue consistent with metallosis were noted. The acetabular component was determined to be stable and in a good position. The femoral component was rotationally unstable. We were unable to extract the component due to the ingrowth of a small portion of the distal titanium fiber mesh (Figure 2). Attempted extraction with a Shukla extractor resulted in pistoning of the implant around the distal titanium fiber mesh. Extended trochanteric osteomy was performed with a high-speed bur, as well as an accudriver, to loosen the femoral component from bone. Following extraction, the trochanteric osteotomy was reduced and fixated with five cerclage cables (Figure 3). Biomet Arcos revision femoral stem was then prepared and trialed in standard fashion. Final components were placed, and surgical incision was closed in a layered fashion. Revision implants were a Biomet 19mm x 150mm Arcos STS stem size 70 high offset body, dual mobility with a 28mm x 44mm E1 head and 28mm standard ceramic head, and 5 Smith and Nephew Accord cables. Unfortunately for this patient her postoperative course was further complicated by repeated superficial infection and subsequent deep infection, requiring multiple courses of antibiotics and incision & drainage over the following 9 months.
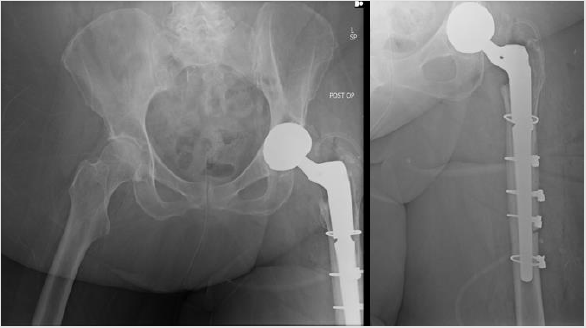
Figure 3: Postoperative AP radiographs of the (A) left pelvis and (B) left thigh demonstrate revision hip arthroplasty with Biomet Arcos STS stem and dual mobility E1 head with standard ceramic head. Five Smith & Nephew Accord cerclage cables were used to stabilize the femur and trochanteric osteotomy.
Discussion
Catastrophic failure of implants after THA is an infrequent cause of revision in patients in the United States, with aseptic failure of the fiber metal mesh junction rarely reported. More commonly, catastrophic failure is due to trunnionosis and subsequent metallosis with metal-on-polyethylene hip arthroplasty. This unique case of atraumatic and aseptic failure of the fiber metal mesh junction represents an important scenario that can be devastating for a patient. Osteolysis around the proximal prosthetic femoral stem decreased the overall implant stability and therefore caused fatigue failure at the fiber metal mesh juncture. This resulted in prosthetic loosening, subsidence, and catastrophic failure. While a similar breakdown in the setting of chronic infection has been noted, there have been no prior studies were found in the United States involving aseptic failure of the component at the fiber metal mesh junction of a Zimmer VerSys Epoch stem. The mechanisms of catastrophic failure of hip implants after THA are multifactorial, but this case with subsequent chronic infection can be considered to be partly attributable to fatigue loading due to morbid obesity. This female patient presented 13 years after initial THA and showed no evidence of deep infection by routine blood work, intraoperative examination, or staining and culture. To our knowledge, this is the first report of failure of the fiber metal mesh junction of a Zimmer VerSys Epoch system. We recommend further studies on the mechanical analysis to better understand the underlying causes of such a catastrophic failure to prevent such disastrous consequences for future patients
References
- Chillag KJ (2016) Giants of Orthopaedic Surgery: Austin T. Moore MD. Clin Orthop 474(12): 2606-2610.
- Morshed S, Bozic KJ, Ries MD, Malchau H, Colford JM (2007) Comparison of cemented and uncemented fixation in total hip replacement: a meta-analysis. Acta Orthop 78(3): 315-326.
- Athanaselis E, Komnos G, Karachalios T (2018) An Unusual Central Dislocation of a Total Hip Arthroplasty Due to Severe Wear of a Ceramic on Cross-linked Polyethylene Bearing Coupling - A Case Report. J Orthop Case Rep 8(6): 54-57.
- Kitamura S, Hasegawa Y, Iwasada S, Kenichi Yamauchi, Kouichi Kawamoto, et al. (1999) Catastrophic failure of cementless total hip arthroplasty using a femoral component without surface coating. J Arthroplasty 14(8): 918-924.
- Heck DA, Partridge CM, Reuben JD, Lanzer WL, Lewis CG, et al. (1995) Prosthetic component failures in hip arthroplasty surgery. J Arthroplasty 10(5): 575-580.
- Kawaji H, Uematsu T, Hoshikawa N, Watanabe H, Takai S (2016) Mid-Term Clinical Results of VerSys Hip System (Zimmer) Uncemented Total Hip Replacement Arthroplasty. J Nippon Med Sch 83(5): 184-187.
- White SP, Lee MB, Galpin J, Learmonth ID (2008) Ten-year results of a bone-preserving low-modulus composite total hip replacement stem. HIP Int 18(2): 81-87.
- Berry DJ, Barnes CL, Scott RD, Cabanela ME, Poss R (1994) Catastrophic failure of the polyethylene liner of uncemented acetabular components. J Bone Joint Surg Br 76(4): 575-578.
- Saltzman BM, Haughom B, Oni JK, Levine BR (2014) Chronic Infection Leading to Failure of a Composite Femoral Stem: A Report of Two Cases. HSS J ® 10(2): 180-185.

 Case Report
Case Report