Editorial
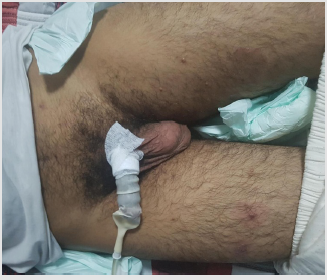
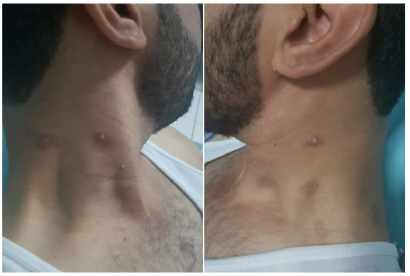
A 29-year-old man followed in neurology for multiple sclerosis for 5 years, put under several treatments without improvement, with installation of a paraplegia where the change of the treatment, and the patient was then put on fingolimod at the dose of 0.5 mg/ mg, 2 months after the start of treatment, the patient has developed multiple asymptomatic papules, located everywhere on the body, such at the trunk, neck, back, 4 limbs and at the genital area, the patient has then consulted in dermatology 5 months after the appearance of these skin lesions. Physical examination revealed multiple waxy lesions, which were skin-colored domeshaped papules with diameters of 2 to 10mm some of which showed central umblication (Figures 1-3). Serologic tests for HIV-1, hepatitis C and B, and Syphilis tests returned negative. CD4+ T-cells count was obtained and was significantly low - 350 cells/mm. Skin biopsy confirmed the clinical diagnosis of molluscum contagiosum. Due to the patient’s economic status, the majority of lesions were individually removed mechanically However, it was necessary to repeat the procedure several times to remove all lesions. In addition, the patient was also put on potassium hydroxide solution 5% for local application, with regression of all lesions after 3 months of treatment.
Molluscum contagiosum is commonly a self-limiting condition
occurring in children [1] it is a benign viral skin disease caused by
the molluscum contagiosum virus of the Poxviridae family, which
is transmitted by direct contact [2]. In the case of typical lesions
the diagnosis is straightforward [3], widespread infection can be
encountered occasionally in patients with impaired cell-mediated
immunity [1] its frequently occurs as an opportunistic infection in
immunocompromised patients, and there seems to be a correlation
between the extent and severity of molluscum contagiosum and
lower CD4-positive T-lymphocyte counts [4]. This has been shown
by some previous reports of widespread molluscum contagiosum
infection in patients treated with immunosuppressive drugs
[2] such as topical calcipotriol / betamethasone (C/B) in an
immunocompetent adult [5] in this patient this was explained by
the fact that the patient continued the application of C/B ointment
on normal skin long after the complete resolution of his skin
prsoriasis thus inducing a shift of the immune response in the Th2
direction, as in AD patients.
Also in patients on systemic therapy such as methrotrexate
[1,2] after alemtuzumab in a patient with chronic lymphocytic
leukaemia [4] Ruxolitinib which is a Janus kinase 1 and 2 inhibitor
in a patient with polycythemia vera [6] and in patients receiving
tumor necrosis factor alpha inhibitors [7]. It has also been reported
in HIV-positive patients with Severe immune suppression, and CD4
+ T-cells <100 cells/mm3 [3]. In the mid-1980s, atypical molluscum
contagiosum was recognized as a feature of HIV infection but with
widespread use of HAART, lesions are now less frequently observed
in Western countries [8]. But high burden of lesions such as our
patient had is uncommon. Our patient was on fingolimod which is
a new pharmacological agent used as a background treatment for
multiple sclerosis (MS), an autoimmune demyelinating disease of
the central nervous system, with lymphopenic properties and this
by reversibly sequestering lymphocytes at the level of secondary
lymphoid organs by inhibiting their exit by an antagonistic action
on the sphingosine1-phosphate receptors, and would thus prevent
the passage in the central nervous system of the lymphocytes
involved in the autoimmune response, This results in an overall
decrease the number of circulating lymphocytes [9]. This explains
this significant desiccation of lesions in our patient who has a
low blood lymphocyte level. Treatment options for disseminated molluscum contagiosum developing with immunosuppressive
therapy include discontinuing the immunosuppressive therapy
followed by manual extraction, chemical cauterization, or
cryotherapy [1]. Here, we report the first case of Disseminated MC
caused by fingolimod. Notably, the severity of MC was much higher
than that of conventional MC.
References
- Relhan V, Roy E, Garg V, Khurana N, Bansal S(2014) Disseminated molluscum contagiosum in a patient on methotrexatetherapy for psoriasis. Indian Journal of Dermatology, Venereology, and Leprology [Internet]. Medknow80(2):179.
- Lim KS, CCI Foo (2007) Disseminated Molluscum Contagiosum in a Patient withChronic Plaque Psoriasis TakingMethotrexate. Clinical and ExperimentalDermatology 32(5): 591-593.
- Filo-Rogulska M, Pindycka-Piaszczyńska M, Januszewski K, Jarząb J(2013) Disseminatedatypical molluscum contagiosum as a presentingsymptom of HIV infection. Advances in Dermatology and Allergology. TermediaSp. z.o.o30(1): 56-58.
- Pitini V, Arrigo C, Barresi G (2003) Disseminated molluscum contagiosum in a patient withchroniclymphocyticleukaemiaafteralemtuzumab. British Journal of Haematology. Wiley 123(4): 565-565.
- Bae JY, Lee JI, Jang DH, Jung HJ, Park MY, et al. (2020) A case of disseminated molluscum contagiosumcaused by topicalcalcipotriol/betamethasone in an immunocompetentadult. JDDG: Journal der DeutschenDermatologischen Gesellschaft. Wiley 18(1): 44-46.
- Kinoshita M, Ogawa Y, Kawamura T, Kirito K, Shimada S (2016) Case of disseminated molluscum contagiosumcaused by ruxolitinib, a Janus kinase 1 and 2 inhibitor. The Journal of Dermatology. Wiley 43(11): 1387-1388.
- Gur I (2008) The epidemiology of Molluscum contagiosum in HIV-seropositivepatients: a unique entity or insignificantfinding? Int J STD AIDS 19(8): 503-506.
- Azevedo T, Catarino A, Ferreira L, Borges F, Mansinho K (2017) Disseminated molluscum contagiosumlesions in an HIV patient. Cleveland Clinic Journal of Medicine. Cleveland Clinic Journal of Medicine84(3): 186-187.
- A Chardain, B Stankoff (2012) Mécanisme d’action et applications thérapeutiques du fingolimodMechanism of action and therapeutic applications of fingolimodLa Lettre du Pharmacologue- juillet-août-septembre 26(3).

 Research Article
Research Article