Introduction
Skin metastases (SM) are infrequent secondary locations of deep neoplasia that can sometimes be indicative of primary cancer. They represent 0.2 to 10% of metastases from solid tumors[1]. The most frequent primary tumors in men were carcinoma of the lung (24%), carcinoma of the large intestine (19%), melanoma (13%), and squamous cell carcinoma of the oral cavity (12%). The most common primary tumors in women were carcinoma of the breast (69%), carcinoma of the large intestine (9%), melanoma (5%), and carcinoma of the ovary (4%)[2].The incidence of cutaneous involvement by all urological malignancies is 1.1% to 2.5% [3]. The kidney is the most common organ to serve as a source of metastasis to the skin[4]. Bladder cancers are less likely to metastasize to the skin. We report a new case of skin metastases presenting as a large tumor in the thoracic level in a patient followed for a urothelial carcinoma of the bladder.
Case Report
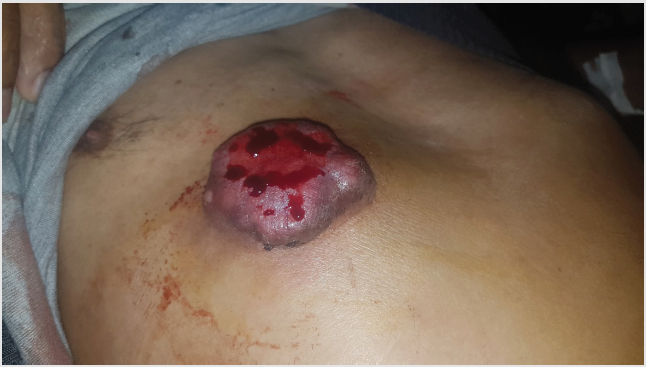
Figure 1: Pigmented tumor of 5/6 cm of large,an ulcerated and bleeding surface in anterior surface of the thorax.
We report the case of a 66-year-old patient, followed for a high-grade urothelial carcinoma for 2 years, initially mesa static at the level of the prostate. The patient was then put on neoadjuvant chemotherapy, but he was lost to follow-up and presented himself after 5 months, with extension of the tumor to the gallbladder, and the urethral masses , the internal obturator muscle and bilateral external iliac lymphadenopathy, as well as adrenal metastasis, with an examination of oncologists the presence of a skin tumor in the right thoracic level, hence a dermatological opinion was requested. A dermatological examination on an objectified presence of a pigmented tumor of 5/6 cm of large, an ulcerated and bleeding surface, sitting at the level of the anterior surface of the thorax, on the right side (Figure 1). At the dermoscopy we had pigmented areas without structures, with the presence of a polymorphic vascularization made of arborising vessels as well as tortuous vessels (Figure 2), in front of this aspect associated with the clinical context we first thought to a skin metastasis bladder tumor, and a skin biopsy was performed confirming this diagnosis. The patient was then kept on palliative chemotherapy based on cisplatin + gemcitabine and died 2 months later.
Discussion
Only 5.3% of all malignancies lead to cutaneous metastasis. Out
of these, 1.34% are linked to underlying genitourinary malignancy;
bladder cancer accounts for 0.84% of these [5] with a limited number
of published cases, It usually metastasizes to regional lymph nodes,
liver, lungs and bones [1] Large 20-year retrospective Taiwanese
study found only 2 cases of skin metastases among 911 patients
with bladder and ureter cancer [6] and Kishi, et al. [7] reported that
66.7% of patients with T3 and T4 tumors had metastatic disease.
Cutaneous involvement from bladder cancer is achieved by direct
tumor invasion, hematogenous routes, lymphatic spread, and direct
seeding due to iatrogenic implantation [8].Iatrogenic implantation
is the most common cause of seeding outside of the urinary tract
[9]and its due to surgical treatment of these tumors, including
cystectomy, partial cystectomy, TURBT, and other procedures [8].
The clinical appearance of these lesions varies and may mimic other
dermatologic diseases. The lesions can be solitary or multiple, and
can have a nodular, fibrotic, and inflammatory appearance[8].
In urological cancer with cutaneous metastasis,several
aspects have been described in the literature,like , A cutaneous
erysipelas-like lesion [10] Zosteriform cutaneous metastases [11]
or Herpetiform cutaneous metastases [12], but the most common
clinical picture is an infiltrated plaque or nodule [10] Ulcerated
swelling, subcutaneous nodules, violaceous papules, and ulcerated
plaques have been reported [1] in our patient the appearance was
that of a large tumor with ulcerated surface. Dermoscopy of skin
metastases has been recently reported in the literature [13], the
most reported sign was a polymorphic vascularization made of
arborising vessels, as well as serpiginous, but these aspects were
not retained as specific, since they can be found even in front of a
primary skin tumor, such as melanoma or squamous cell carcinoma.
Local excision, radiotherapy, chemotherapy, immunological and
combination therapy have been reported in previous studies [14].
Due to the poor outcomes of these patients, the treatment options
are limited and primarily supportive in nature. The prognosis
of any cancer with cutaneous metastasis is poor; with regard to
bladder cancer with cutaneous metastasis, median survival time is
< 12 months [10].
Conclusion
We report a new case of skin metastasis of a bladder tumor, in the form of a pigmented tumor in a patient with multiple visceral metastases. Although cutaneous metastasis is a rare dermatological condition, cutaneous metastasis should be included in the differential diagnosis of tumoal lesion. Skin biopsy should be performed to prevent misdiagnosis. For the patients with urologic malignancies, we suggest that all urologists should increase attention to the physical examination of the skin because skin lesions can be the first sign of silent or recurrent urologic malignancies.
References
- Nashan D, Müller ML, BraunFalco M, Reichenberger S, Szeimies RM, et al. (2009) Cutaneous metastases of visceral tumours: A review. J Cancer Res Clin Oncol 135(1): 1-14.
- Brownstein MH (1972) Patterns of cutaneous metastasis. Archives of Dermatology105(6): 862-868.
- Block CA, Dahmoush L, Konety BR (2006) Cutaneous metastases from transitional cell carcinoma of the bladder. Urology 67: 846.e15-17.
- Mueller TJ, Wu H, Greenberg RE, Hudes G, Topham N, et al. (2004) Cutaneous metastases from genitourinary malignancies. Urology 63(6): 1021-1026.
- Weizer AZ, Shariat SF, Haddad JL, Escudier S, Lerner SP (2002) Metastatic transitional cell carcinoma of the urinary bladder to the shoulder girdle. Rev Urol 4: 97-99.
- Hu SC, Chen GS, Wu CS (2009) Rates of cutaneous metastases from different internal malignancies: experience from a Taiwanese medical center. J Am Acad Dermatol 60(3): 379-387.
- Saito S (1998) Solitary Cutaneous Metastasis of Superficial Bladder Cancer. Urologia Internationalis 61(2): 126-127.
- Narayana MA, Patnayak R, Rukmangadha N, Chowhan AK, Kottu R, et al. (2014) Cutaneous metastasis of transitional cell carcinoma of the urinary bladder: Cytological aspect. J Cytol 31: 50-52.
- Tal Cohen, Daniel Ricchiuti, Mark Memo (2017) Bladder cancer that metastasized to the skin: A unique presentation that signifies poor prognosis. Rev Urol 19(1): 67-71.
- Chang CP, Lee Y, Shih HJ (2013) Unusual presentation of cutaneous metastasis from bladder urothelial carcinoma. Chin J Cancer Res 25(3): 362-365.
- Thomaidou E, Armoni G, Klapholz L, Hadayer N, Maly A, et al. (2018) Zosteriform cutaneous metastases. Clinical and Experimental Dermatology 43(6): 734-736.
- Somani BK, Prita D, Grant S, Nabi G, N’Dow J (2006) Herpetiform cutaneous metastases from transitional cell carcinoma of the urinary bladder: Immunohistochemical analysis. Journal of Clinical Pathology. BMJ 59(12): 1331-1333.
- Deinlein T, Haenssle HA, Fink C, HofmannWellenhof R, Blum A (2018) Dermatoskopie von kutanenMetastasen 70(2): 142-144.
- Nashan D, Meiss F, BraunFalco M, Reichenberger S (2010) Cutaneous metastases from internal malignancies. Dermatol Ther 23(6): 567-580.

 Case Report
Case Report