Abstract
Nutritional Psychiatry is a term used to describe a field of research, and a way of approaching the prevention and treatment of mental illness, which focuses on diet and nutrition. Among the complexity of the determinants of Mental Health problems, the emerging evidence from Nutrition shows relevant factors in the high prevalence of mental disorders, suggesting that diet is as important for Psychiatry as for Cardiology, Endocrinology and Gastroenterology. Studies of the relationship between diet quality (and potential nutritional deficiencies) and mental health disorders, as well as the use of nutrients to treat deficiencies, are increasing. Nutritional psychiatry has been promoting the interaction between the cardiologist-nutricionist-neurocientist, which has been recommended in the nutritional care of patients with chronic diseases, among them: heart failure. Certainly, this new area of nutritional psychiatry will allow us to broaden our look under the conception of future research that evaluates intervention in psychiatrynutrition- cardiology a multidisciplinary and interdisciplinary approach.
Keywords: Nutritional Psychiatry; Depression, Heart failure; Nutrition
What’s the Evidence?
Nutritional psychiatry is a new area for the study of the correlation
of mental disorders, metabolic abnormalities, nutrition in chronic
diseases [1]. The term “Nutritional Psychiatry” emerged in 2013
after a consensus statement that advocated as a new field of research
focused on the comprehensive development of evidence, cohesive
and scientifically rigorous to support a shift in thinking around the
role of diet and nutrition in health [2]. Nutritional psychiatry has
been promoting the interaction between cardiologist-nutricionistpsychiatrist-
neurocientist, which has been recommended in the
nutritional care of patients with chronic diseases, among them:
heart failure [1-3]. HF is a complex clinical syndrome, often chronic
in nature, which is associated with metabolic, inflammatory,
nutritional abnormalities and has a high prevalence of depression
[1,4]. HF promotes metabolic and nutritional abnormalities
that are associated with different multimorbidities, among
them depression. Current evidence shows that better food quality,
i.e. fruits, vegetables, fish and whole grains are associated with
lower risk for depressive symptoms, but not all available results
are consistent with the hypothesis that diet influences the risk
to develop depression [3,5,6]. Depression when associated with
heart conditions causes inflammatory, metabolic and nutritional
disorders. Lifestyle and particularly nutrition seem to be able to
influence the development and course of depressive morbidity.
Different nutrients or different dietary patterns can influence the
aggravation of depressive symptoms, but are not yet explored in HF
[1,2,7].
Nutritional aspects are so important in mental health that they
have inspired researchers to a new field of multidisciplinary research
called nutritional psychiatry. The inter and multidisciplinary
approach involving nutritionists, nutrologists, psychiatrists, psychologists, neuroscientists and cardiologists specializing in HF
has allowed a transdisciplinary look at the relationship in mind/
brain and metabolism, lifestyle and nutrition in chronic diseases
[7]. The changes in the dietary pattern have been reported with
the worsening of depressive symptoms and depression, resulting
in increased inflammation and oxidative stress, consequently
in nutritional deficiencies and depletion of essential fatty acids.
Nutrients form the substrate of essential biological processes in
the body and brain, thus ensuring that nutrient levels are adequate
in patients suffering from serious diseases is important [1,8]. In
the study conducted by Sarris et al., [3] in the area of nutritional
psychiatry showed that patients who consumed foods rich in
omega 3 or eicosapentaenoic acid (EPA) showed strong association
in significantly reducing depressive symptoms. In addition, other
studies alone showed that the benefits of creatine supplementation
by adding zinc, vitamin C, the amino acid tryptophan and folic acid
produced mixed results in depressed patients, however, considered
all these supplements relatively safe.
Although, it is not the focus of nutritional psychiatry to support
the use of nutritional supplements. Jacka et al. 2017 have speculated
that the use of these supplements can increase the effectiveness
of antidepressants in various ways, perhaps directly altering the
activity of neurotransmitters or indirectly, reducing inflammation,
known to contribute to depression. However, research in this area
is gradually uncovering potential facts based on their specific
nutritional deficiencies, brain conditions and genetic profiles,
seeking to understand the basic factors that can influence nutrient
metabolism, including intestinal health [1-5].
What Is the Connection?
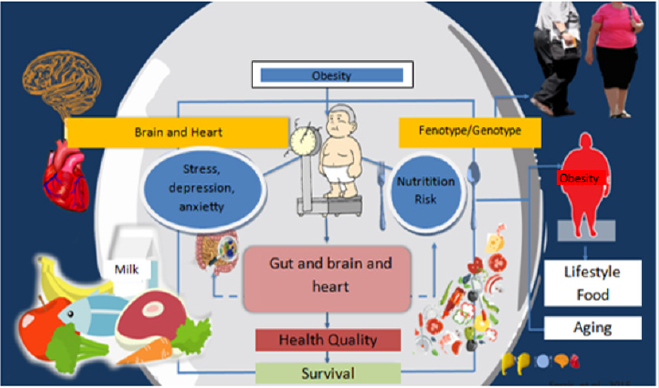
Another important aspect in this connection of the nutritional state - depression - CI is obesity. Obesity increases the chance by four times the risk of developing depression. In patients with HF, obesity is related to several alterations in cardiac structures, cardiac hypertrophy, increase in epicardial fat and infiltration of myocardial fat, enlargement of the right ventricle cavity and alteration in the left ventricle ejection fraction (LVEF). Despite this, obesity has also been identified as a protective factor for the risk of mortality from HF, a factor referred to in the literature as “reverse epidemiology”. A hypothesis for reverse epidemiology would be the fact that HF itself generates catabolic state in the individual. Thus, obese individuals with a higher metabolic reserve are resistant to catabolic condition [6-9]. However, there is little evidence of studies associated with depression and nutritional changes in patients with HF. In this sense, in figure 1 connecting the concepts of HF with the evidence of nutritional psychiatry - to generate knowledge about nutritional factors and design studies directed and personalized to depression and other psychiatric diseases in order to promote quality of life and survival in these patients [10]. Currently, we have started in Brazil the pioneering research in the line of nutritional psychiatry in patients with heart failure, which is an innovation in the field of research, because in this study we think about mental and brain health and the relationship with cardiology, the model focused on integrative physiology, nutritional aspects and the understanding of biomarkers.
Certainly, this new area of nutritional psychiatry will allow us to broaden our look under the design of future research that evaluates the intervention in mental health - nutrition - cardiology - facing a multi and interdisciplinary approach.
References
- FN Jacka (2017) Nutritional Psychiatry: Where to Next? EBioMedicine. 17: 24-29.
- W Marx, G Moseley, M Berk, Felice Jacka (2017) Nutritional psychiatry: The present state of the evidence. Proceedings of the Nutrition Society 76: 4: 427-436.
- Jacka FN, O Neil A, Opie R, Itsiopoulos C, Cotton S, et al. (2017) A randomised controlled trial of dietary improvement for adults with major depression (the ‘SMILES’ trial). BMC Med 15:23.
- Baxter AJ, Patton G, Scott KM, Degenhardt L, Whiteford HA, et al. (2013) Global epidemiology of mental disorders: what are we missing? PLoS One 8(6): e65514.
- (2018) Coordinating Committee for the Heart Failure Directive. Brazilian Guideline for Chronic and Acute Heart Failure. Arq Bras Cardiol. 111(3): 436-539.
- RB Othman, O Mziou, A Gamoudi, Amal Smida, Cyrin Souissi, et al. (2018) Nutritional Status of Depressive Patients. J Diabetes Metab 9: 2.
- JJ McMurray, S Adamopoulos, SD Anker (2016) The Task Force for the Diagnosis and Treatment of Acute and Chronic Heart Failure of the European Society of Cardiology. Eur Heart J 33(14): 1787-847.
- E Zamora, C Díez-López, J Lupón, Marta de Antonio, Mar Domingo, et al. (2016) Weight Loss in Obese Patients with Heart Failure. J Am Heart Assoc 24(3): 5.
- JMP RUIZ (2017) Impact of nutritional assessment in patients with heart failure. Nutr Hosp. 34(6): 1265-1266.
- Guerra B by R Thais (2018) The nutritional psychiatric paradigm associated with different methods of depression in patients with heart failure. PhD Thesis in Cardiovascular Sciences; Universidade Federal Fuminense).

 Mini Review
Mini Review