Impact Factor : 0.548
- NLM ID: 101723284
- OCoLC: 999826537
- LCCN: 2017202541
*Muringani BN
Received: May 07, 2017 Published: May 23, 2017
Corresponding author: Muringani BN, Department of Medical Microbiology, Faculty of Health Sciences, National University of science and technology, Zimbabwe
DOI: 10.26717/BJSTR.2017.01.000105
Necrotising fasciitis are uncommon and remain a devastating disease, with an overall incidence of 0.24-0.4 per 100,000 adults [1]. Delays in instigation of appropriate treatment are associated with significant long-term morbidity with mortality ranging from 9% to more than 25% [2]. Early and repeated debridement of affected planes in combination with use of broad-spectrum antibiotics improves overall outcome [3]. This case study looked at a sudden incidence of a superbug which had consumed 17-20cm wide and 4-5cm deep of flesh within two days of presentation of illness in a 43 year old female.
Necrotising fasciitis are uncommon and remain a devastating disease, with an overall incidence of 0.24-0.4 per 100,000 adults [1]. Delays in instigation of appropriate treatment are associated with significant long-term morbidity with mortality ranging from 9% to more than 25% [2]. Early and repeated debridement of affected planes in combination with use of broad-spectrum antibiotics improves overall outcome [3]. However, early Necrotizing fasciitis can be difficult to distinguish from non-necrotising soft tissue infections in the absence of severe sepsis, multiorgan failure or pain. Significant risk factors for mortality have been predicted as age over 50 years, raised serum creatinine, delayed surgical intervention, multiorgan failure and elevated blood lactate. Clinical features typical of a diagnosis of Necrotizing fasciitis include agonising pain as the cutaneous nerve supply to overlying skin is destroyed, tenderness beyond erythematous areas, blister or bullae formation, swelling of muscle compartments which may give rise to a compartment syndrome and rapid progression of invading microorganisms through tissue planes [3].
This type of NF is a polymicrobial, often bowel flora derived and synergistic infection; tissue culture will show a mixed growth of anaerobes and aerobes. It is common type of NF; frequently occurs in patients with diabetes mellitus. Type 1 NF common to occur in perineum and trunk of the body.
A 43-year old female with no history of diabetics and no hypertension history reported to a physician with a problem which appeared to be heamorroid of the anal sphincter. The physician prescribed antibiotics and suppository and pain killers and discharged the patient for review after 48 hours. Within 24hours, the patient had come back presenting with severe pain in the periunum area which was swollen and very tender. Temperature was 38ºc, patient was confused with tachycardia. On examination of the swollen area, foul smelling pus started oozing out and about 1-2 litres of pus was removed.
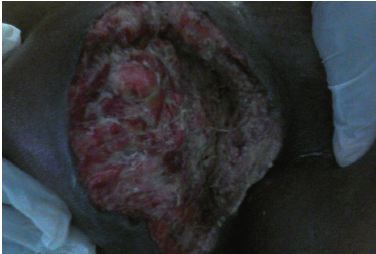
Figure 1: The difference between collimated light (laser) and uncollimated light.
Immediately the patient was put on IV metronidazole, ceftriazone and ciprofloxacin and transferred to hospital for an emergency dibrediment of the necrotized tissue. Pus and pus swabs were collected for microbiological analysis. Blood for full blood count and blood sugar was taken before the surgery. Pseudomonas aeruginosa and E.coli were isolated and these were multidrug resistant only sensitive to ceftriazone metronidazole and ciprofloxacin. Blood glucose was high and the full blood count showed an increase in white cell count. VAC therapy was then done for tissue granulation for 4 weeks See picture below for wound (Figures 1-3).
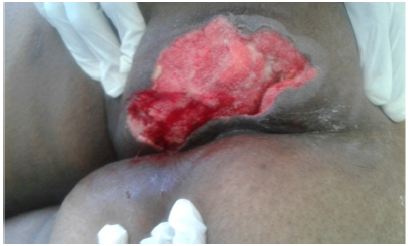
Figure 2: First week of VAC therapy.
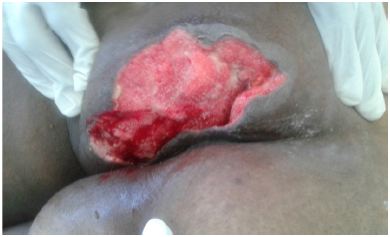
Figure 3: Third week of VAC therapy.
Necrotising fasciitis has a very high mortality and it quickly spreads before intervention can be done leading to loss of life. The situation with the patient in question was worsened by the fact that the wound was in a very difficult spot to bandage and clean which meant that ordinary method of managing the wound were not going to be effective. Introduction of VAC therapy improved the wound greatly leading to the conclusion that VAC therapy has become the latest method in managing wounds and preventing further contamination from general wound handling and bandaging [4].


